Objectives: We aimed to analyze waiting list and liver transplantation trends for autoimmune liver disease in Argentina.
Methods: We designed a population-based analysis of waitlisted or liver transplanted patients for autoimmune hepatitis, primary biliary cholangitis or primary sclerosing cholangitis between 2006-2017 in Argentina. Cumulative incidence rates of waiting list registration and liver transplantation were standardized for age and sex using the 2000 WHO standard population. Joinpoint regression analysis was used to identify changes in waiting list and liver transplantation trends.
Results: Waiting list registrations for autoimmune hepatitis, primary biliary cholangitis and primary sclerosing cholangitis represented 9.66%, 5.07% and 0.85%. Wait-listing rates for autoimmune hepatitis and primary biliary cholangitis increased significantly between 2006 and 2017, with an annual percentage change of 4.9% (95% CI 0.8 to 9; p=0.01) and 5.5% (95% CI 1 to 10.2; p=0.01) respectively. Patients with autoimmune hepatitis and primary biliary cholangitis aged 40-59 years showed the highest increase in waiting list registration rates. Waiting list registration trends for primary sclerosing cholangitis remained stable: annual percentage change 1.4% (CI 95% -2.1 to 5; p=0.4). Liver transplantation for autoimmune hepatitis, primary biliary cholangitis and primary sclerosing cholangitis represented 10.69%, 5.99% and 3.64%. Liver transplantation trends remained stable in all autoimmune liver diseases.
Conclusion: Increasing trends of waiting list registration of autoimmune hepatitis and primary biliary cholangitis may respond to higher diagnosis and early referral rates to liver transplant units. Nevertheless, the growing waitlisting of patients with autoimmune end-stage liver disease underlines an unmet need for effective therapy.
autoimmune liver disease, waiting list registration, liver transplantation, trends
Autoimmune hepatitis (AH), primary biliary cholangitis (PBC) and primary sclerosing cholangitis (PSC) represent three major etiologies of chronic and progressive autoimmune liver disease [1]. The natural history of AH and PBC towards end-stage liver disease has been modified with the availability of effective therapy. Since the 1970s, treatment of AH with corticosteroids has proven to be successful in preventing cirrhosis and liver transplantation in a significant proportion of timely treated patients [2,3]. Similarly, since the 1990s, ursodeoxycholic acid therapy has managed to slow PBC progression to end-stage liver disease in approximately two-thirds of patients. Unfortunately, effective medical therapy for PSC is yet to be developed [4,5].
Prevalence studies of autoimmune liver disease are scarce. It has been proposed that the need of liver transplantation is a useful surrogate to estimate the burden of autoimmune liver disease and the impact of available treatment6. When analyzing liver transplantation etiology for end-stage liver disease in developed countries, listing for PBC decreased 50% in the last 20 years whereas AH has remained infrequent (~3% throughout the same study period) [6-8]. In the United States of America and the United Kingdom, PSC is currently the main indication for transplantation due to autoimmune liver disease 6. Similar observations have been made in other European countries [4,9].
Most of these studies addressing changes in waitlisting and liver transplantation for autoimmune liver disease were reported in developed countries; regions with a low prevalence of autoimmune liver disease [6] and high referral rates and access to effective medication. In Argentina, a developing country with mixed-ethnicity [10], the reported prevalence of autoimmune liver disease is quite different: AH is the fourth etiology of liver transplantation for end-stage liver disease [11,12]. Regarding cholestatic liver disease, PBC represented the 5th and PSC the 9th indication for liver transplantation for end-stage liver disease. Despite the high burden of autoimmune liver disease in Argentina, there is scant available information regarding current diagnosis timing and access to effective treatment.
Therefore, analyzing trends in liver transplantation due to autoimmune liver disease in Argentina may underline the access and effectiveness of current diagnostic and treatment strategies, as well as the impact that newly developed therapies (such as obeticholic acid) could have in our country in the future.
In this study we aimed to estimate waiting list registration and liver transplantation trends for autoimmune liver disease in Argentina, and to analyze the trend tendencies in the last decade.
We performed a population-based, time-series analysis of patients registered in the SINTRA database between January 1st, 2006 and December 31st, 2017. SINTRA is the Argentinian information system of the national procurement organization (INCUCAI) that contains the complete information of all liver transplantation activity nationwide. SINTRA information is routinely and prospectively collected since its creation in 2005. We included data from 2006 to 2017, publicly available at the SINTRA website [13]. The research was conducted according to the World Medical Association Declaration of Helsinki.
Case definition
We included all patients who were 1) registered on the waiting list for liver transplantation and 2) those who received a liver transplant in the above-mentioned period in Argentina. Only patients with a primary indication of autoimmune liver disease: AH, PBC or PSC were included. Patients were included considering the date of inscription on the waiting list for the first group; and the date of liver transplant graft perfusion for the second group. SINTRA classifies cases by etiology, using only one possible diagnosis without overlapping between categories. Patients in the emergency status were not included since the etiology of acute liver failure could not be individualized in the majority of cases. This is explained by the fact that SINTRA allows for several codes for inscription in emergency status such as fulminant hepatitis and sub-fulminant hepatitis without details as to underlying liver disease. Patients were also excluded if they received a combined transplant if they previously received a liver transplant or in case or living donor liver transplantation.
Cumulative incidence estimation
We estimated the crude cumulative incidence and the sex and age-stratified cumulative incidence of waiting list registrations and liver transplantation for each one of the 3 etiologies. Annual cumulative incidence rate was estimated between 2006 and 2017, starting the first day of January and ending the last day of December. We used the Argentinian population as denominator. The data were extracted from 2010 census and annual inter census estimates published by the National Institute of Statistics and Censuses Institute [14,15]. We estimated standardized cumulative incidence rates by direct standardization using the 2000 WHO standard population [16]. All rates are expressed by 1,000,000 people and presented with their respective 95% confidence intervals (CI).
Temporal trend analysis
We evaluated the standardized annual cumulative incidence of waiting list registration and liver transplantation using a join-point regression model analysis to identify significant changes over time throughout the selected 11-year period. We considered as “join-point” the significant changes in time-related trend tendencies [17]. We estimated the annual percentage change (APC) for each segment. The terms increase or decrease were used when the slope presented with an APC different than 0.5% and a significant p value; otherwise trends were considered stable [18,19]. If a significant trend was identified, further age group analysis was performed. To characterize age related differences, three age groups were created: younger patients (0-39 years old), middle-aged patients (40-59 years old) and older patients (equal or older than 60 years old) [20]. The JoinPoint Regression Program 4.4.0.0 software developed by the United States National Cancer Institute was used [17].
Liver transplant waiting list registration for autoimmune liver disease
A total of 7,604 patients were registered for first isolated liver transplantation in the Argentinian liver transplant waiting list during the study period. Considering the etiology, 736 patients were listed for AH (9.67%), 383 patients were listed for PBC (5.04%) and 119 patients for PSC (1.56%) during the entire study period.
Trends in liver transplant waiting list registrations according to the etiology of liver disease
Trends of standardized cumulative incidence rates for waitlist registrations were calculated for patients with AH, PBC and PSC during the 11-year study period (Figure 1). Using join-point analysis, we observed significant changes in AH and PBC patient`s registration rates (Table 1). The incidence of waiting list registration of patients with AH and PBC showed constant and significant increase, with an APC 4.85% (95% CI 0.8 to 9; p=0.01) and 5.50% (95% CI 1 to 10.2; p=0.01) respectively. However, PSC patient´s waiting list registration rates were stable throughout the study period with an APC of 1.42% (95% CI -2.1 to 5; p=0.4). No significant join-point was detected.
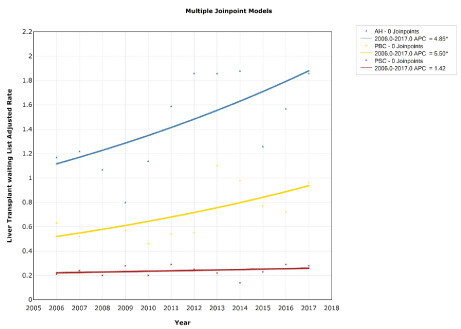
Figure 1. Trends in standardized cumulative incidence rates (per 1,000,000 persons) for liver transplant waiting list registrations according to autoimmune disease etiology in Argentina (2006 – 2017 period)
Note: Cumulative standardized incidence rates of waiting list registrations in Argentina stratified by disease etiology: autoimmune hepatitis (AH), primary biliary cholangitis (PBC) and primary sclerosing cholangitis (PSC). Dark blue curve: AH patients. The only segment during the 11-year study period had an annual percent change (APC) of 4.85%; CI 95% 0.8 to 9, p=0.01. Yellow curve: PBC patients. The only segment during the study period had an APC 5.5%; CI 95% 1 to 10.2; p=0.01. Red curve: PSC patients. The only segment had an APC 1.42%; CI 95% -2.1 to 5; p=0.4.
Table 1. Crude and standardized rates for liver transplant waiting list registrations according to autoimmune disease etiology in Argentina (2006 – 2017 period)
Year |
Total
Popul. |
AH |
PBC |
PSC |
WL pts |
Crude rate IC 95% |
Stand Rate IC 95% |
WL pts |
Crude rate
IC 95% |
Stand rate
IC 95% |
WL pts |
Crude rate
IC 95% |
Stand. Rate
IC 95% |
2006 |
39558883 |
47 |
1.18 (0.89-1.5) |
1.30 (0.99-1.7) |
28 |
0.70 (0.48-1) |
0.79 (0.56-1.1) |
9 |
0.22 (0.11-0.43) |
0.26 (0.14-0.48) |
2007 |
39971084 |
50 |
1.25 (0.94-1.6) |
1.29 (0.98-1.69) |
25 |
0.62 (0.42-0.92) |
0.74 (0.51-1) |
10 |
0.25 (0.13-0.46) |
0.28 (0.16-0.5) |
2008 |
40382399 |
44 |
1.08 (0.81-1.4) |
1.12 (0.84-1.5) |
26 |
0.64 (0.43-0.94) |
0.72 (0.5-1) |
9 |
0.26 (0.11-0.42) |
0.25 (0.13-0.45) |
2009 |
40800290 |
33 |
0.80 (0.57-1.1) |
0.83 (0.59-1.16) |
27 |
0.66 (0.45-0.96) |
0.72 (0.5-1) |
11 |
0.22 (0.15-0.48) |
0.30 (0.17-0.52) |
2010 |
40778955 |
47 |
1.15 (0.86-1.5) |
1.24 (0.94-1.6) |
22 |
0.53 (0.35-0.81) |
0.61 (0.41-0.9) |
8 |
0.19 (0.09-0.3) |
0.21 (0.11-0.41) |
2011 |
41209048 |
69 |
1.67 (1.32-2.1) |
1.74 (1.38-2.1) |
24 |
0.58 (0.39-0.86) |
0.65 (0.44-0.95) |
12 |
0.29 (0.16-0.5) |
0.33 (0.2-0.56) |
2012 |
41658435 |
79 |
1.89 (1.52-2.3) |
1.96 (1.58-2.44) |
26 |
0.62 (0.42-0.91) |
0.68 (0.47-0.98) |
11 |
0.26 (0.14-0.47) |
0.26 (0.15-0.47) |
2013 |
42119370 |
80 |
1.89 (1.52-2.3) |
1.92 (1.55-2.39) |
49 |
1.16 (0.88-1.5) |
1.26 (0.97-1.6) |
15 |
0.35 (0.21-0.58) |
0.21 (0.11-0.41) |
2014 |
42576987 |
82 |
1.92 (1.55-2.3) |
1.96 (1.59-2.43) |
44 |
1.03 (0.76-1.38) |
1.17 (0.89-1.5) |
6 |
0.14 (0.06-0.3) |
0.16 (0.07-0.3) |
2015 |
43023042 |
55 |
1.27 (0.98-1.6) |
1.26 (0.97-1.64) |
34 |
0.79 (0.56-1.1) |
0.91 (0.66-1.2) |
10 |
0.23 (0.12-0.42) |
0.21 (0.11-0.4) |
2016 |
43478299 |
69 |
1.58 (1.25-2) |
1.57 (1.23-1.98) |
34 |
0.78 (0.55-1) |
0.82 (0.59-1.1) |
12 |
0.27 (0.15-0.48) |
0.28 (0.16-0.49) |
2017 |
44272125 |
81 |
1.82 (1.47-2.2) |
1.86 (1.5-2.31) |
44 |
0.99 (0.74-1.3) |
1.10 (0.83-1.4) |
12 |
0.27 (0.15-0.47) |
0.27 (0.15-0.48) |
Note: All rates were calculated per 1,000,000 persons. WL Pts: waitlisted patients; Stand: Standardized rate
Trends in liver transplant waiting list registrations for autoimmune hepatitis and primary biliary cholangitis stratified by age
When we stratified waiting list registration rates in patients with AH according to age (Figure 2A) younger patients (0-39 years old) and middle-aged patients (40-59 years old) had an increasing registration incidence. Both groups portrayed an upward slope, with an APC 5.58%; (95% CI 1.2 to 10.1; p=0.02) and an APC 7.23%; (95% CI 2.5 to 12.2; p=0.01) respectively. Older patients had stable trends of waitlist inscription (supplementary material). Regarding patients with PBC (Figure 2B) younger patients (0-39 years old) presented stable registration rates during the study period. However, middle-aged patients (40-59 years old) had an increasing incidence in their registration rates, with an APC of 13.61%; (95% CI 6 to 21.8; p=0.01). Older patients, aged 60 years old or higher, had significantly decreasing trend of waitlist inscription during the study period, with APC -5.71%; (95% CI -9.6 to -1,7 p=0.01) (supplementary material). No significant join-points were detected in either autoimmune condition in the age-stratified analysis.
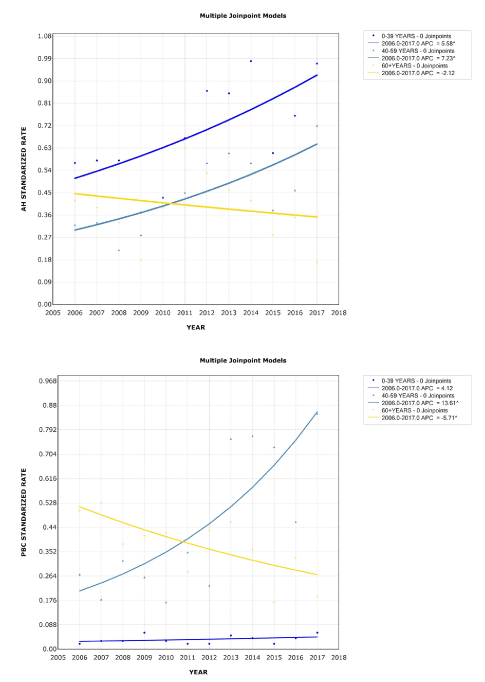
Figure 2. Trends insex-adjusted cumulative incidence rates stratified by age groups (per 1,000,000 persons) for liver transplant waiting list registrations according to autoimmune disease etiology: Autoimmune Hepatitis (A) and Primary Biliary Cholangitis (B) in Argentina (2006 – 2017 period)
A. Note: Cumulative incidence rates of waiting list registrations of autoimmune hepatitis patients in Argentina stratified by age. Dark blue curve: 0-39 years old patients. The only segment during the 11-year study period had an annual percent change (APC) of 5.58%; CI 95% 1.2 to 10.1 p=0.01. Yellow curve: 60 years or older patients. The only segment during the study period had an APC -2.1%; CI 95% -8.6 to 4.9; p=0.5. Light blue curve: 40-59 years old patients. The only segment had an APC 7.23%; CI 95% 2.5 to 12.2; p=0.01.
B. Note: Cumulative incidence rates of waiting list registrations of primary biliary cholangitis patients in Argentina stratified by age. Dark blue curve: 0-39 years old patients. The only segment during the 11-year study period had an annual percent change (APC) of 4.12%; CI 95% -3.7 to 12.6, p=0.3. Yellow curve: 60 years or older patients. The only segment during the study period had an APC -5.7%; CI 95% -9.6 to -1.7; p=0.01. Light blue curve: 40-59 years old patients. The only segment had an APC 13.61%; CI 95% 6 to 21.8; p=0.01.
A total of 2,778 patients received an isolated deceased donor liver transplantation during the 11-year study period. AH, PBC and PSC were the etiology in 10.69%, 5.99% and 2.72% respectively.
Trends in liver transplant waiting list registrations based on etiology of liver disease
Trends in liver transplantation remained stable during the 11-year study period in all studied etiologies (Figure 3 and Table 2)
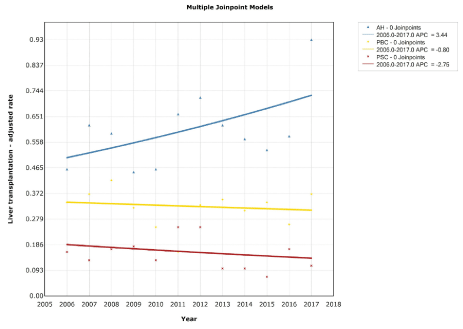
Figure 3. Trends in age and sex-adjusted cumulative incidence rates (per 1,000,000 persons) for liver transplantation according to autoimmune disease etiology in Argentina (2006 – 2017 period)
Note: Cumulative incidence rates of liver transplantation in Argentina stratified by disease etiology: autoimmune hepatitis (AH), primary biliary cholangitis (PBC) and primary sclerosing cholangitis (PSC). Dark blue curve: AH patients. The only segment during the 11-year study period had an annual percent change (APC) of 3.44%; CI 95% -0.2 to 7.2, p=0.1. Yellow curve: PBC patients. The only segment during the study period had an APC -0.8%; CI 95% -4.7 to 3.2; p=0.7. Red curve: PSC patients. The only segment had an APC -2.75%; CI 95% -9.6 to 4.6; p=0.4.
Table 2. Age and sex- standardized rates for liver transplantation according to autoimmune disease etiology in Argentina (2006 – 2017 period)
Year |
Total
Popul. |
AH |
PBC |
PSC |
LT pts |
Crude rate IC 95% |
Stand Rate IC 95% |
LT pts |
Crude rate
IC 95% |
Stand rate
IC 95% |
LT pts |
Crude rate
IC 95% |
Stand. Rate
IC 95% |
2006 |
39558883 |
18 |
0.45 (0.28-0.7) |
0.44 (0.28-0.7) |
13 |
0.32 (0.19-0.56) |
0.39 (0.24-0.64) |
6 |
0.15 (0.06-0.33) |
0.16 (0.07-0.34) |
2007 |
39971084 |
24 |
0.60 (0.4-0.89) |
0.65 (0.44-0.9) |
15 |
0.37 (0.22-0.61) |
0.42 (0.26-0.68) |
5 |
0.12 (0.05-0.29) |
0.13 (0.05-0.3) |
2008 |
40382399 |
24 |
0.59 (0.39-0.9) |
0.57 (0.38-0.8) |
17 |
0.42 (0.26-0.67) |
0.47 (0.3-0.74) |
7 |
0.17 (0.08-0.35) |
0.16 (0.07-0.34) |
2009 |
40800290 |
18 |
0.44 (0.27-0.7) |
0.41 (0.25-0.6) |
13 |
0.31 (0.18-0.54) |
0.37 (0.22-0.61) |
7 |
0.17 (0.08-0.35) |
0.17 (0.08-0.35) |
2010 |
40778955 |
18 |
0.44 (0.27-0.7) |
0.46 (0.29-0.7) |
11 |
0.26 (0.15-0.48) |
0.30 (0.17-0.52) |
5 |
0.12 (0.05-0.28) |
0.13 (0.05-0.3) |
2011 |
41209048 |
27 |
0.65 (0.45-0.9) |
0.64 (0.43-0.9) |
7 |
0.16 (0.08-0.3) |
0.18 (0.09-0.37) |
10 |
0.24 (0.13-0.44) |
0.27 (0.15-0.48) |
2012 |
41658435 |
30 |
0.72 (0.5-1) |
0.70 (0.49-1) |
14 |
0.33 (0.2-0.56) |
0.38 (0.23-0.62) |
11 |
0.26 (0.14-0.47) |
0.26 (0.14-0.46) |
2013 |
42119370 |
27 |
0.64 (0.44-0.9) |
0.63 (0.43-0.9) |
15 |
0.35 (0.21-0.58) |
0.38 (0.24-0.62) |
4 |
0.09 (0.03-0.24) |
0.08 (0.03-0.22) |
2014 |
42576987 |
24 |
0.56 (0.37-0.8) |
0.54 (0.36-0.8) |
13 |
0.30 (0.17-0.52) |
0.35 (0.21-0.58) |
4 |
0.09 (0.03-0.24) |
0.09 (0.03-0.23) |
2015 |
43023042 |
22 |
0.51 (0.33-0.7) |
0.51 (0.34-0.7) |
15 |
0.34 (0.21-0.57) |
0.39 (0.24-0.63) |
3 |
0.07 (0.02-0.2) |
0.07 (0.02-0.2) |
2016 |
43478299 |
25 |
0.57 (0.38-0.8) |
0.56 (0.37-0.8) |
12 |
0.27 (0.15-48) |
0.29 (0.17-0.51) |
7 |
0.16 (0.07-0.33) |
0.17 (0.09-0.35) |
2017 |
44272125 |
41 |
0.92 (0.68-1.2) |
0.95 (0.70-1.2) |
17 |
0.38 (0.23-0.61) |
0.43 (0.28-0.67) |
5 |
0.11 (0.04-0.26) |
0.11 (0.05-0.27) |
Note: All rates were calculated per 1,000,000 persons. LT Pts: liver transplant patients; Stand: Standardized rate
In this temporal trend analysis of waiting list registration and transplantation due to autoimmune liver disease in Argentina we observed that: 1. AH represented the most frequent indication for waiting list registration and liver transplantation due to autoimmune liver disease, followed by PBC and much less frequently by PSC during the entire study period; 2. waitlisting for AH and PBC showed increasing trends during the 11-year study period, whereas PSC trends remained stable; and 3. trends in liver transplantation remained stable in all studied autoimmune liver diseases.
Waiting list registration and liver transplantation are considered proxies of the prevalence and burden of autoimmune liver disease in a particular country [6,21]. In developed regions such as the Netherlands, United States, United Kingdom, Sweden and other european countries there has been a decrease in waiting list registrations and/or liver transplantation rates for patients with PBC [1,6,21,22]. AH, however, remained as an infrequent cause of end-stage liver disease with need of liver transplantation [23]. It has been proposed that factors such as increased rates of early diagnosis and broad access to effective medical therapy, among other causes are possible explanations for these decreasing trends [1,21,22], especially considering that in some geographies up to 82% of PBC patients are being treated with ursodeoxycholic acid [22]. In concordance, the main etiology for liver transplantation in these regions is currently PSC, a disease without available effective therapy.
In contrast, we have observed a constant and increasing rate of patients with end-stage liver disease caused by AH and PBC being waitlisted for liver transplantation in Argentina. A unique explanation for these findings remains uncertain. A possible hypothesis is that there is an increasing proportion of AH and PBC patients in our country that requires early referral to liver transplantation units. This could be supported by the observed age groups of waitlisted patients: during the entire study period young and middle-aged AH patients had higher trends of inclusion in the waiting list. Similarly, middle-aged patients with PBC were the only age group with an increasing incidence on the waiting list. Including young and middle-aged patients could reflect poor response to treatment and a more aggressive course of both autoimmune liver diseases due to unknown reasons of cofactors (such as the concomitance of other liver diseases, like non-alcoholic fatty liver disease) [2,24].
However, if sicker patients with AH and PBC were listed for liver transplantation, we should have observed concordantly increasing liver transplantation rates and that was not the case: trends in liver transplantation for autoimmune liver disease remained stable throughout the studied period. It should be noted that Argentina has a MELD-based allocation policy since 2005. Access to liver transplantation was found to be notably higher in patients with MELD exceptions (predominantly for stage 2 hepatocellular carcinoma) compared with patients without MELD exceptions [12]. Since autoimmune patients rarely have hepatocellular carcinoma, this could explain the lack of concomitant increase in liver transplant rates in this subgroup. It is also worth mentioning that since this is a population-based analysis, we cannot exclude patients being listed for other causes different than end-stage liver disease (e.g pruritus).
Another proposed hypothesis is the growing detection of affected patients with PBC and AH in Argentina, and thus, an increase in referral rates. Hepatology has developed largely as a discipline within gastroenterology in the last decades in Argentina. Recently, in the year 2006, a specialist course in Hepatology became available in the capital city, and in 2012 in an online format for the rest of the country. Also in the year 2012, Hepatology achieved recognition as a distinct specialty by the Argentinian National Health Ministry [25]. Despite a shorter time of available formal training compared to other countries such as US [26], the Hepatology workforce in Argentina now reaches one specialist every 203.000 patients, a higher proportion than observed in the US, with approximately one hepatologist every 330.000 patients [27]. Thus, it is possible that with increasing education in this field, patients with autoimmune liver disease are more frequently diagnosed and thus timely referred.
An additional theory is related to the increased access to liver transplantation in Argentina. Since the performance of the first liver transplant in 1988 in our country, it has become the standard of care for end-stage liver disease and fulminant liver failure. In 2002, liver transplantation was included as part of the Obligatory Medical Plan for all citizens, independent to their type of health insurance [28]. This increase in waitlisting incidence rates of AH and PBC patients could express an easier access to liver transplant units, which may have affected physician behavior prompting an early referral of patients with decompensated cirrhosis to be treated while on the waiting list. This theory could explain the fact that liver transplantation trends remained unchanged.
This study has strengths and limitations. Only aggregate data was available for cumulative incidence rate calculation, thus limiting the analysis of individual confounding factors. However, observational studies that measure variables at group level have been proven to be adequate to describe changes in population trends and are appropriate for initial investigations of a causal hypothesis. On the other hand, this study provides novel information regarding the prevalence and trends of waiting list and liver transplantation due to autoimmune liver disease in a developing country.
Our study underlines that autoimmune hepatitis and primary biliary cholangitis are prevalent causes of end-stage liver disease in Argentina. The increasing trends of waitlisting for liver transplantation of patients with AH and PBC may respond to higher diagnosis rates and early referral to liver transplant units in our country. Regardless of the explanation, this increasing number of patients diagnosed with autoimmune end-stage liver disease in Argentina underlines a still unmet need of effective and accessible therapy in our region.
Melisa Dirchwolf and Andres Ruf were involved in the research design; acquisition, analysis, interpretation of data and drafting of the paper. Sebastian Marciano and Diego Giunta were involved in research design, interpretation of data, critical revision of the manuscript for important intellectual content and statistical analysis. All authors approved the final version of the manuscript.
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Researchers do not have any conflict of interest to disclose.
- Carbone M, Neuberger JM (2014) Autoimmune liver disease, autoimmunity and liver transplantation. J Hepatol 60: 210-223. [Crossref]
- Montano Loza AJ, Czaja AJ (2007) Current therapy for autoimmune hepatitis. Nat Clin Pract Gastroenterol Hepatol 4: 202-214. [Crossref]
- Ichai P, Duclos-Vallée JC, Guettier C, Hamida SB, Antonini T, et al. Usefulness of corticosteroids for the treatment of severe and fulminant forms of autoimmune hepatitis. Liver Transpl 13: 996-1003. [Crossref]
- Andersen IM, Fosby B, Boberg KM, Clausen OPF, Jebsen P, et al. (2015) Indications and Outcomes in Liver Transplantation in Patients With Primary Sclerosing Cholangitis in Norway. Transplant Direct 1: e39. [Crossref]
- Sclair SN, Little E, Levy C (2015) Current Concepts in Primary Biliary Cirrhosis and Primary Sclerosing Cholangitis. Clin Transl Gastroenterol 6: e109. [Crossref]
- Webb GJ, Rana A, Hodson J, Akhtar MZ, Ferguson JW, et al (2018) Twenty-Year Comparative Analysis of Patients With Autoimmune Liver Diseases on Transplant Waitlists. Clin Gastroenterol Hepatol 16: 278-287.e7. [Crossref]
- Lu M, Zhou Y, Haller IV, Romanelli RJ, VanWormer JJ, et al. (2018) Increasing Prevalence of Primary Biliary Cholangitis and Reduced Mortality With Treatment. Clin Gastroenterol Hepatol 16: 1342-1350.e1. [Crossref]
- Carbone M, Mells GF, Pells G, Dawwas MF, Newton JL, et al. (2013) Sex and age are determinants of the clinical phenotype of primary biliary cirrhosis and response to ursodeoxycholic acid. Gastroenterology 144: 560-569.e7 [Crossref]
- Schöning W, Schmeding M, Ulmer F, Andert A, Neumann U (2015) Liver Transplantation for Patients with Cholestatic Liver Diseases. Viszeralmedizin 31: 194-198. [Crossref]
- Homburger JR, Moreno-Estrada A, Gignoux CR, Nelson D, Sanchez E, et al. (2015) Genomic Insights into the Ancestry and Demographic History of South America. PLoS Genet 11: e1005602. [Crossref]
- Mendizabal M, Marciano S, Videla MG, Anders M, Zerega A, et al. (2015) Fulminant presentation of autoimmune hepatitis. Eur J Gastroenterol Hepatol 27: 644-648. [Crossref]
- Cejas NG, Villamil FG, Lendoire JC, Tagliafichi V, Lopez A, et al. (2013) Improved waiting-list outcomes in Argentina after the adoption of a model for end-stage liver disease-based liver allocation policy. Liver Transpl 19: 711-720. [Crossref]
- https://cresi.incucai.gov.ar/Inicio.do
- https://datosmacro.expansion.com/demografia/poblacion/argentina
- https://www.indec.gob.ar/censos_total_pais.asp?id_tema_1=2&id_tema_2=41&id_tema_3=135&t=3&s=0&c=2010
- https://www.who.int/healthinfo/paper31.pdf
- https://surveillance.cancer.gov/joinpoint/
- https://progressreport.cancer.gov/methodology
- Fernandez E, González JR, Borràs JM, Moreno V, Sánchez V, et al. (2001) Recent decline in cancer mortality in Catalonia (Spain). A joinpoint regression analysis. Eur J Cancer 37: 2222-2228. [Crossref]
- Henson JB, Patel YA, Wilder JM, Zheng J, Chow S, et al. (2017) Differences in Phenotypes and Liver Transplantation Outcomes by Age Group in Patients with Primary Sclerosing Cholangitis. Dig Dis Sci 62: 3200-3209. [Crossref]
- Lee J, Belanger A, Doucette JT, Stanca C, Friedman S, et al. (2007) Transplantation trends in primary biliary cirrhosis. Clin Gastroenterol Hepatol 5: 1313-1315. [Crossref]
- Kuiper EMM, Hansen BE, Metselaar HJ, Man RA, Haagsma EB, et al. (2010) Trends in liver transplantation for primary biliary cirrhosis in the Netherlands 1988-2008. BMC Gastroenterol 10: 144. [Crossref]
- Adam R, Karam V, Delvart V, O'Grady J, Mirza D, et al. (2012) Evolution of indications and results of liver transplantation in Europe. A report from the European Liver Transplant Registry (ELTR). J Hepatol 57: 675-688. [Crossref]
- Poupon R (2010) Primary biliary cirrhosis: a 2010 update. J Hepatol 52: 745-758. [Crossref]
- de la Nación M de S (2012) Boletín Oficial de La República Argentina. Resolución 908/2012: Listado de Especialidades Medicas.
- Luxon BA (2013) So You Want to Be a Hepatologist? Gastroenterology 145: 1182-1185. [Crossref]
- Russo MW, Koteish AA, Fuchs M, Gautham Reddy K, Fix OK (2016) Workforce in hepatology: Update and a critical need for more information. Hepatology 65: 336-340. [Crossref]
- https://www.sssalud.gob.ar/pmo/res_s_02_201.pdf
Editorial Information
Editor-in-Chief
Dr. Abdullah H. A. Almalki
Section Head of Nephrology, Department of Medicine, KAMC, Saudi Arabia
Article Type
Research Article
Publication history
Received date: March 05, 2021
Accepted date: March 31, 2021
Published date: April 05, 2021
Copyright
©2021 Dirchwolf M. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Citation
Dirchwolf M, Marciano S, Giunta DH, Ruf AE (2021) Waiting list registration and liver transplantation rates among patients with autoimmune liver disease: An 11-year trend analysis. Trends in Transplant 14(3): DOI: 10.15761/TiT.1000298

Figure 1. Trends in standardized cumulative incidence rates (per 1,000,000 persons) for liver transplant waiting list registrations according to autoimmune disease etiology in Argentina (2006 – 2017 period)
Note: Cumulative standardized incidence rates of waiting list registrations in Argentina stratified by disease etiology: autoimmune hepatitis (AH), primary biliary cholangitis (PBC) and primary sclerosing cholangitis (PSC). Dark blue curve: AH patients. The only segment during the 11-year study period had an annual percent change (APC) of 4.85%; CI 95% 0.8 to 9, p=0.01. Yellow curve: PBC patients. The only segment during the study period had an APC 5.5%; CI 95% 1 to 10.2; p=0.01. Red curve: PSC patients. The only segment had an APC 1.42%; CI 95% -2.1 to 5; p=0.4.

Figure 2. Trends insex-adjusted cumulative incidence rates stratified by age groups (per 1,000,000 persons) for liver transplant waiting list registrations according to autoimmune disease etiology: Autoimmune Hepatitis (A) and Primary Biliary Cholangitis (B) in Argentina (2006 – 2017 period)
A. Note: Cumulative incidence rates of waiting list registrations of autoimmune hepatitis patients in Argentina stratified by age. Dark blue curve: 0-39 years old patients. The only segment during the 11-year study period had an annual percent change (APC) of 5.58%; CI 95% 1.2 to 10.1 p=0.01. Yellow curve: 60 years or older patients. The only segment during the study period had an APC -2.1%; CI 95% -8.6 to 4.9; p=0.5. Light blue curve: 40-59 years old patients. The only segment had an APC 7.23%; CI 95% 2.5 to 12.2; p=0.01.
B. Note: Cumulative incidence rates of waiting list registrations of primary biliary cholangitis patients in Argentina stratified by age. Dark blue curve: 0-39 years old patients. The only segment during the 11-year study period had an annual percent change (APC) of 4.12%; CI 95% -3.7 to 12.6, p=0.3. Yellow curve: 60 years or older patients. The only segment during the study period had an APC -5.7%; CI 95% -9.6 to -1.7; p=0.01. Light blue curve: 40-59 years old patients. The only segment had an APC 13.61%; CI 95% 6 to 21.8; p=0.01.

Figure 3. Trends in age and sex-adjusted cumulative incidence rates (per 1,000,000 persons) for liver transplantation according to autoimmune disease etiology in Argentina (2006 – 2017 period)
Note: Cumulative incidence rates of liver transplantation in Argentina stratified by disease etiology: autoimmune hepatitis (AH), primary biliary cholangitis (PBC) and primary sclerosing cholangitis (PSC). Dark blue curve: AH patients. The only segment during the 11-year study period had an annual percent change (APC) of 3.44%; CI 95% -0.2 to 7.2, p=0.1. Yellow curve: PBC patients. The only segment during the study period had an APC -0.8%; CI 95% -4.7 to 3.2; p=0.7. Red curve: PSC patients. The only segment had an APC -2.75%; CI 95% -9.6 to 4.6; p=0.4.
Table 1. Crude and standardized rates for liver transplant waiting list registrations according to autoimmune disease etiology in Argentina (2006 – 2017 period)
Year |
Total
Popul. |
AH |
PBC |
PSC |
WL pts |
Crude rate IC 95% |
Stand Rate IC 95% |
WL pts |
Crude rate
IC 95% |
Stand rate
IC 95% |
WL pts |
Crude rate
IC 95% |
Stand. Rate
IC 95% |
2006 |
39558883 |
47 |
1.18 (0.89-1.5) |
1.30 (0.99-1.7) |
28 |
0.70 (0.48-1) |
0.79 (0.56-1.1) |
9 |
0.22 (0.11-0.43) |
0.26 (0.14-0.48) |
2007 |
39971084 |
50 |
1.25 (0.94-1.6) |
1.29 (0.98-1.69) |
25 |
0.62 (0.42-0.92) |
0.74 (0.51-1) |
10 |
0.25 (0.13-0.46) |
0.28 (0.16-0.5) |
2008 |
40382399 |
44 |
1.08 (0.81-1.4) |
1.12 (0.84-1.5) |
26 |
0.64 (0.43-0.94) |
0.72 (0.5-1) |
9 |
0.26 (0.11-0.42) |
0.25 (0.13-0.45) |
2009 |
40800290 |
33 |
0.80 (0.57-1.1) |
0.83 (0.59-1.16) |
27 |
0.66 (0.45-0.96) |
0.72 (0.5-1) |
11 |
0.22 (0.15-0.48) |
0.30 (0.17-0.52) |
2010 |
40778955 |
47 |
1.15 (0.86-1.5) |
1.24 (0.94-1.6) |
22 |
0.53 (0.35-0.81) |
0.61 (0.41-0.9) |
8 |
0.19 (0.09-0.3) |
0.21 (0.11-0.41) |
2011 |
41209048 |
69 |
1.67 (1.32-2.1) |
1.74 (1.38-2.1) |
24 |
0.58 (0.39-0.86) |
0.65 (0.44-0.95) |
12 |
0.29 (0.16-0.5) |
0.33 (0.2-0.56) |
2012 |
41658435 |
79 |
1.89 (1.52-2.3) |
1.96 (1.58-2.44) |
26 |
0.62 (0.42-0.91) |
0.68 (0.47-0.98) |
11 |
0.26 (0.14-0.47) |
0.26 (0.15-0.47) |
2013 |
42119370 |
80 |
1.89 (1.52-2.3) |
1.92 (1.55-2.39) |
49 |
1.16 (0.88-1.5) |
1.26 (0.97-1.6) |
15 |
0.35 (0.21-0.58) |
0.21 (0.11-0.41) |
2014 |
42576987 |
82 |
1.92 (1.55-2.3) |
1.96 (1.59-2.43) |
44 |
1.03 (0.76-1.38) |
1.17 (0.89-1.5) |
6 |
0.14 (0.06-0.3) |
0.16 (0.07-0.3) |
2015 |
43023042 |
55 |
1.27 (0.98-1.6) |
1.26 (0.97-1.64) |
34 |
0.79 (0.56-1.1) |
0.91 (0.66-1.2) |
10 |
0.23 (0.12-0.42) |
0.21 (0.11-0.4) |
2016 |
43478299 |
69 |
1.58 (1.25-2) |
1.57 (1.23-1.98) |
34 |
0.78 (0.55-1) |
0.82 (0.59-1.1) |
12 |
0.27 (0.15-0.48) |
0.28 (0.16-0.49) |
2017 |
44272125 |
81 |
1.82 (1.47-2.2) |
1.86 (1.5-2.31) |
44 |
0.99 (0.74-1.3) |
1.10 (0.83-1.4) |
12 |
0.27 (0.15-0.47) |
0.27 (0.15-0.48) |
Note: All rates were calculated per 1,000,000 persons. WL Pts: waitlisted patients; Stand: Standardized rate
Table 2. Age and sex- standardized rates for liver transplantation according to autoimmune disease etiology in Argentina (2006 – 2017 period)
Year |
Total
Popul. |
AH |
PBC |
PSC |
LT pts |
Crude rate IC 95% |
Stand Rate IC 95% |
LT pts |
Crude rate
IC 95% |
Stand rate
IC 95% |
LT pts |
Crude rate
IC 95% |
Stand. Rate
IC 95% |
2006 |
39558883 |
18 |
0.45 (0.28-0.7) |
0.44 (0.28-0.7) |
13 |
0.32 (0.19-0.56) |
0.39 (0.24-0.64) |
6 |
0.15 (0.06-0.33) |
0.16 (0.07-0.34) |
2007 |
39971084 |
24 |
0.60 (0.4-0.89) |
0.65 (0.44-0.9) |
15 |
0.37 (0.22-0.61) |
0.42 (0.26-0.68) |
5 |
0.12 (0.05-0.29) |
0.13 (0.05-0.3) |
2008 |
40382399 |
24 |
0.59 (0.39-0.9) |
0.57 (0.38-0.8) |
17 |
0.42 (0.26-0.67) |
0.47 (0.3-0.74) |
7 |
0.17 (0.08-0.35) |
0.16 (0.07-0.34) |
2009 |
40800290 |
18 |
0.44 (0.27-0.7) |
0.41 (0.25-0.6) |
13 |
0.31 (0.18-0.54) |
0.37 (0.22-0.61) |
7 |
0.17 (0.08-0.35) |
0.17 (0.08-0.35) |
2010 |
40778955 |
18 |
0.44 (0.27-0.7) |
0.46 (0.29-0.7) |
11 |
0.26 (0.15-0.48) |
0.30 (0.17-0.52) |
5 |
0.12 (0.05-0.28) |
0.13 (0.05-0.3) |
2011 |
41209048 |
27 |
0.65 (0.45-0.9) |
0.64 (0.43-0.9) |
7 |
0.16 (0.08-0.3) |
0.18 (0.09-0.37) |
10 |
0.24 (0.13-0.44) |
0.27 (0.15-0.48) |
2012 |
41658435 |
30 |
0.72 (0.5-1) |
0.70 (0.49-1) |
14 |
0.33 (0.2-0.56) |
0.38 (0.23-0.62) |
11 |
0.26 (0.14-0.47) |
0.26 (0.14-0.46) |
2013 |
42119370 |
27 |
0.64 (0.44-0.9) |
0.63 (0.43-0.9) |
15 |
0.35 (0.21-0.58) |
0.38 (0.24-0.62) |
4 |
0.09 (0.03-0.24) |
0.08 (0.03-0.22) |
2014 |
42576987 |
24 |
0.56 (0.37-0.8) |
0.54 (0.36-0.8) |
13 |
0.30 (0.17-0.52) |
0.35 (0.21-0.58) |
4 |
0.09 (0.03-0.24) |
0.09 (0.03-0.23) |
2015 |
43023042 |
22 |
0.51 (0.33-0.7) |
0.51 (0.34-0.7) |
15 |
0.34 (0.21-0.57) |
0.39 (0.24-0.63) |
3 |
0.07 (0.02-0.2) |
0.07 (0.02-0.2) |
2016 |
43478299 |
25 |
0.57 (0.38-0.8) |
0.56 (0.37-0.8) |
12 |
0.27 (0.15-48) |
0.29 (0.17-0.51) |
7 |
0.16 (0.07-0.33) |
0.17 (0.09-0.35) |
2017 |
44272125 |
41 |
0.92 (0.68-1.2) |
0.95 (0.70-1.2) |
17 |
0.38 (0.23-0.61) |
0.43 (0.28-0.67) |
5 |
0.11 (0.04-0.26) |
0.11 (0.05-0.27) |
Note: All rates were calculated per 1,000,000 persons. LT Pts: liver transplant patients; Stand: Standardized rate



