Wave-MV™, a flowable composite resin, is used for fixed partial dentures (FPDs; referred to as WFPD). WFPD is a minimally invasive fixed prosthesis that is simpler and quicker and requires minimal treatment compared to conventional single-tooth replacement. In addition, conventional FPD requires significant drilling of the tooth surface. Recently, a dental implant has become the preferred alternative to single-tooth replacement. However, some patients are contraindicated for dental implants, and others may dislike the surgical aspects or long treatment period. In this study, we report the use of Wave-MV™ to bond an artificial tooth with an FPD and observe postoperative progress and patient satisfaction over a 12-year follow-up period. In this case, the patient has not experienced debonding or gum trouble and has good satisfaction with WFPD for over 10 years.
artificial tooth, flowable composite resin, fixed partial denture, minimal treatment, Wave-MV™
Use of Wave-MV™ (SDI Ltd., Melbourne, Australia) to bond an artificial tooth with a fixed partial denture (FPD; referred to as WFPD) is a new idea that minimizes the invasiveness of fixed prostheses. The prosthetic restoration of small edentulous spans poses a dilemma when the adjacent teeth do not require a crown and bridge, which makes it difficult to justify extensive reduction of the adjacent teeth to support a conventional FPD. Currently, a single-tooth oral implant is an alternative for patients with adequate bone dimensions and who are willing to undergo a minor surgical procedure. However, an oral implant is not the treatment of choice for many patients, and the FPD offers a possible solution. In 1977, Howe and Denehy [1] adapted the Rochette bonded cast-metal periodontal splint concept [2] to create the first FPD. A conventional FPD requires significant removal of tooth structure. This is especially true when there is either no or very conservative restoration in the abutment tooth. A dental implant may be the ideal alternative to single-tooth replacement.
Unfortunately, not all patients can receive implant restorations, and others may dislike the surgical aspects and long treatment times. In addition, medical conditions may result in surgical complications. In these situations, many clinicians focus on FPD. However, FPD may have some problems such as debonding, tooth darkening, and gum trouble during long-term retentions. The survival rates of conventional FPD reported in the literature widely vary, indicating restorations can be quite technique-sensitive [3,4]. More recently, use of resin-bonded with glass fiber-reinforced composites has been reported for FPD [5-7]. These restorations can be fabricated using direct or indirect techniques. Flowable resin is successfully bonded to the fibers and substructure bulk is added at the pontic region. Flowable resin is essential for the clinical success of these restorations [8,9].
From a patient’s perspective, important considerations are esthetics, tooth stability, and longevity of restoration. After taking these considerations into account, Wave-MV™ was chosen as the ideal product to use on this case. Here, we report the first use of Wave-MV™ to bind an artificial tooth to FPD. WFPD is simpler and quicker and requires minimal treatment compared to conventional methods. Furthermore, patient satisfaction with WFPD was also high, and WFPD has maintained good outcomes without debonding or gum trouble over 10 years.
A 32-year-old Japanese woman presented with small edentulous spans between lower lateral left and right incisor and canine teeth. The patient wished to decrease the gaps but did not want to receive treatment with a crown and bridge or dental implants. After extensive discussions, we decided to apply the WFPD in this case.
Images of the patient’s teeth were taken to create a working cast model (Figure 1). Artificial teeth (Endura anterio®; Shofu Co. Ltd., Kyoto, Japan) were selected (Figure 2a). Artificial teeth were prepared as follows. First, we fabricated an adhesion wing using Wave-MV™ (Figure 2b). Second, artificial teeth were fit onto the working cast before adhesion (Figures 2c and 2d). The artificial tooth position and biting height were confirmed to be suitable for the patient’s oral condition. Next, enamel etching and bonding of the tooth surface (Figure 3a) using 35% phosphoric acid (GC. Co. Ltd., Tokyo, Japan) and GC-Bond® (GC. Co. Ltd.) were performed (Figure 3b). Five milliliters of etching gel were applied on the targeted tooth surface, left for 30 s, washed, and then air dried. Then, 5 ml of bonding agent were applied to the targeted tooth surface, left for 10 s, air dried, and then light cured for 10 s. The artificial tooth was then adhered to the adjacent tooth using Wave-MV™ (1-mm thickness; Figure 3c) and light cured using SDI LED light (Figure 3d). Figure 3e shows the teeth after treatment.
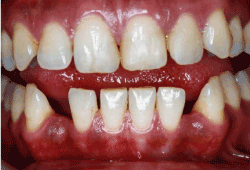
Figure 1a.Image before treatment
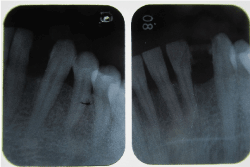
Figure 1b.tX-ray taken before (L) and just after (R) treatment
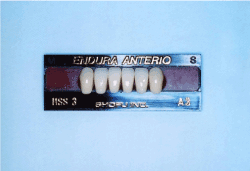
Figure 2a.Artificial Endura tooth from Shofu
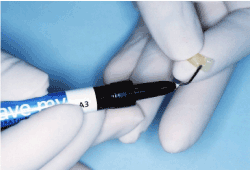
Figure 2b.Adhesion wing using Wave-MV™
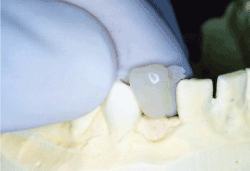
Figure 2c.Test fit for the working cast (front view)
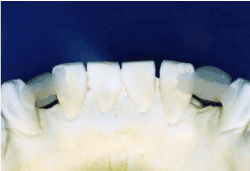
Figure 2d.Test fit for the working cast (back view)
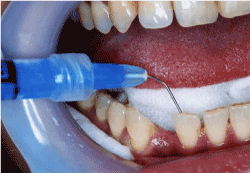
Figure 3a.Test fit for the working cast (back view)
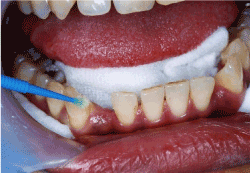
Figure 3b.Enamel bonding with GC-bond bonding agent
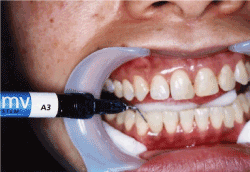
Figure 3c.Addition of Wave-MV™ for adhesion
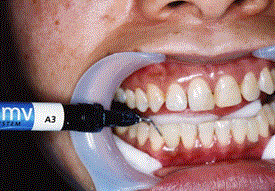
Figure 3d.Light curing using an SDI LED light
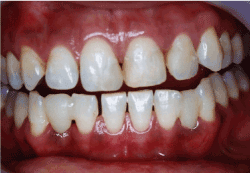
Figure 3e.Image taken immediately after treatment
Post-treatment photographs and X-rays were taken several times during the 12-year follow-up (Figures 4–9). The patient also received general cleaning by a dental hygienist at each follow-up visit. The postoperative course and patient satisfaction are shown in Table 1.
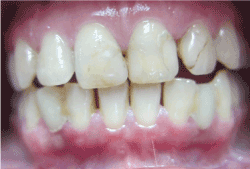
Figure 4.Image taken 1 year after treatment
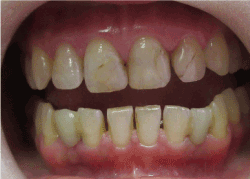
Figure 5.Image taken 3 years after treatment
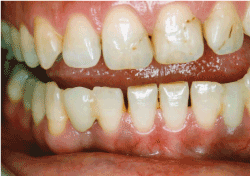
Figure 6.Image taken 5 years after treatment
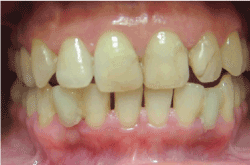
Figure 7.Image taken 7 years after treatment
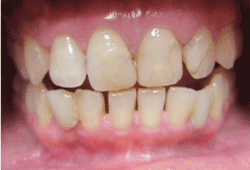
Figure 8a.Image taken 10 years after treatment
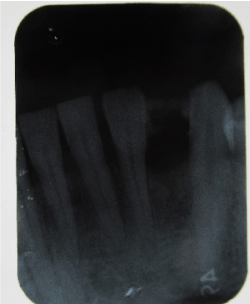
Figure 8b.X-ray image taken of the lower left side 10 years after treatment
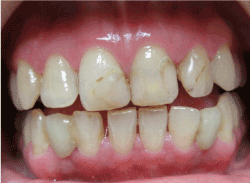
Figure 9.Image taken 12 years after treatment
Table 1. Patient satisfaction over the 12-year follow-up
|
JA |
1y |
3y |
5y |
7y |
10y |
12y |
Bonding |
3 |
3 |
3 |
3 |
3 |
3 |
3 |
Gum trouble |
3 |
3 |
2 |
3 |
3 |
2 |
3 |
Feeling |
2 |
2 |
3 |
3 |
3 |
3 |
3 |
Patient satisfaction was scored just after treatment (JA) and 1, 3, 5, 7, 10, and 12 years after treatment (1y, 3y, 5y, 7y, 10y, and 12y, respectively). 3: Excellent, 2: Good, 1: Not good
Dentists often question the use of FPD for reliable restoration of tooth-bound edentulous spaces. Initial attempts at bonding FPDs on teeth resulted in early failure due to debonding. In the 1980s and 1990s, improvements in preparation methods, metal alloys, and bonding techniques made the resin-bonded FPD a more predictable option [10,11]. The potential abutment teeth should be healthy, unrestored or minimally restored, free of caries and periodontal disease, and have an adequate crown height and width. Nonmobile teeth with adequate enamel provide an ideal abutment. Although young patients are more likely to have sound teeth, debonding rates are higher among people under 30 years of age [12].
WFPD may be a definitive solution for single-unit edentulous spaces bounded by healthy teeth. However, the use of this procedure is currently considered a provisional treatment. As it is minimally invasive, WFPD can not only provide a temporary option for young patients who have suffered the early loss of an anterior tooth, but also a permanent option for older patients. In this case report, the entire WFPD procedure only took 2 days. Thus, it may be appropriate for patients who are apprehensive of dental treatment or unable to commit to multiple appointments.
However, the patient should still be dentally motivated and caries and periodontal disease should be controlled before placing fixed prosthodontics. In addition, managing expectations with regard to oral hygiene, esthetic outcome, and longevity should be considered an important part of treatment planning [13]. If expectations are unrealistic, then patient satisfaction with the final result is likely to be low.
The principal reason for FPD failure remains debonding of the framework from the abutment teeth, which is dependent on the physical bonding strength of resin to abutment teeth. In terms of this clinical issue, Wave-MV™ has high adhesion potential and physical strength. Furthermore, the preparation should be confined to the enamel as much as possible and the surface area maximized to enhance bonding of a rigid framework. Occlusive mechanical stress on the artificial tooth should be kept to a minimum and suitable-sized tooth should be avoided.
Two-day treatment using Wave-MV™ and an artificial tooth for WFPD can be highly effective in replacing missing teeth or decreasing a small edentulous space and restoring oral function and esthetics with high patient satisfaction. This case report demonstrated that WFPD is a minimally invasive, cost-effective, and long-lasting treatment alternative to conventional FPDs.
The authors wish to thank Dr. Hiromi Shimomura for helpful and critical discussions.
All authors contributed equally to this work and report no conflict of interest. S. Tsubura designed the study and interpreted the results. A. Suzuki and T. Tsubura collected test data and drafted the manuscript.
- Howe DF, Denehy GE (1977) Anterior fixed partial dentures utilizing the acid-etch technique and a cast metal framework. J Prosthet Dent 37: 28-31. [Crossref]
- Rochette AL (1973) Attachment of a splint to enamel of lower anterior teeth. J Prosthet Dent 30: 418-423. [Crossref]
- Ketabi AR, Kaus T, Herdach F, et al. (2004) Thirteen-year follow-up study of resin-bonded fixed partial dentures. Quintessence Int 35: 407-410.
- Zalkind M, Ever-Hadani P, Hochman N (2003) Resin-bonded fixed partial denture retention: a retrospective 13-year follow-up. J Oral Rehabil 30: 971-977. [Crossref]
- Jain P, Cobb D (2002) Evaluation of a glass-fiber-reinforced, bonded, inlay-supported fixed partial denture. 4-year results. Comped Contin Educ Dent 23: 779-788. [Crossref]
- Javaheri DS (2002) Provisionalization and definitive restoration of a missing premolar with an indirect fiber-reinforced resin fixed partial denture. Pract Proced Aesthet Dent 14: 387-391.
- Vallittu PK (2004) Survival rates of resin-bonded, glass fiber-reinforced composite fixed partial dentures with a mean follow-up of 42 months: A pilot study. J Prosthet Dent 91: 241-246.
- Freilich MA, Meiers JC (2004) Fiber-reinforced composite prostheses. Dent Clin North Am 48: viii-ix, 545-62. [Crossref]
- Freilich MA, Meiers JC, Duncan JP, Eckrote KA, Goldberg AJ (2002) Clinical evaluation of fiber-reinforced fixed bridges. J Am Dent Assoc 133: 1524-1534.
- Livaditis GJ, Tompson VP (1982) Etched castings: an improved retentive mechanism for resin-bonded retainers. J Prosthet Dent 47: 52-58.
- Creugers NH, Käyser AF, van 't Hof MA (1994) A meta-analysis of durability data on conventional fixed bridges. Community Dent Oral Epidemiol 22: 448-452. [Crossref]
- Goodacre CJ, Bernal G, Rungcharassaeng K, Kan JY (2003) Clinical complications in fixed prosthodontics. J Prosthet Dent 90: 31-41. [Crossref]
- Tredwin CJ, Setchell DJ, George GS, Weisbloom M (2007) Resin-retained bridges as predictable and successful restorations. Alpha Omegan 100: 89-96.


















