This study describes for the first time a definition of Optimal Metabolism from the standpoint of cellular function. Very simply, cells require an optimal amount of T3, the main thyroid hormone for ideal performance. This paper describes specifically how to optimize a patient’s metabolism and the results. Optimal Metabolism is measureable and specifically defined by the FT3 (free T3) in the upper 20% of the normal range, the TT3/RT3 ratio (total T3/reverse T3) between 10-15, and the FT4 > 0.6. Being in the Optimal Range predictably coincides with substantial reductions in chronic diseases including Subclinical Hypothyroidism and other low T3 states. Being in the Optimal Range results in improved health spans and increased productivity. Substantial reductions in cost of health care also result because repetitive expensive hospitalizations, ER visits, ineffectual repetitive medical workups, and ineffective treatments are eliminated. Optimal Metabolism can improve public health at much lower cost.
To identify which chronic diseases benefit from Metabolic Optimization and the magnitude of the improvements. To prove the safety of Optimizing Metabolism and to increase awareness and use of this medical treatment.
This is a case controlled study with intervention of 165 patients measuring the reductions in chronic diseases by Optimizing Metabolism. Over the last 18 years participants were selected from my office ENT patients based on the following: A) one chronic ENT complaint with sub-optimal response to standard medical treatments, B) two or more general hypothyroid symptoms, and C) a sub-optimal thyroid profile.
(T3) liothyronine and (T4) levothyroxine were given in gradually increasing dosages until the Optimal Range was reached and maintained.
165 patients reached Optimal Metabolism. Percentage changes in symptomatology and any side effects were accurately recorded during each consultation after every blood test. This data was entered into an Excel spreadsheet. The average percent improvements (API) were calculated and side effects tallied.
The Immune system API was 63%. API for Neurology was 80%. API for Dermatology was 70%. Gastroenterology/Constipation - API of 74%.
Overweight - patients lost 7 lbs. average. *Decreased Medications - Allergy 34%; Prednisone and Psychotropics 4% each.
Side effects: Heart Palpitation - 16%, Heat Intolerance - 5%, Muscle Cramping - 4%.
Optimizing Metabolism is safe resulting in large multiple systemic improvements. Decreased disability, increased productivity, and increased human health spans result. Recurrent suppressive or more interventional therapies, hospitalizations, and medical costs can all be greatly reduced. This study is not double-blinded, placebo-controlled, and cannot prove causality. However, because of the large number of controlled trials and the magnitude and breadth of the improvements, those studies should be undertaken. Physicians could and should consider this readily available therapy perhaps beginning with their most difficult and refractory cases.
Low metabolism is extremely common. The most common cause is aging [4]. Metabolism will also slow in response to trauma, illness, inflammation or starvation as the body tries to preserve protein by causing RT3 to increase and FT3 to decrease [1,5,8]. RT3 makes the conversion of T4 to T3 less efficient [2] causing further slowing of metabolism. At some trigger point systemic dysfunction occurs.
Low metabolism is not generally recognized by doctors or patients as an underlying cause of chronic medical conditions. This is because:
1) Optimal Metabolism from the viewpoint of cellular function is not a current concept so,
2) Accurate blood testing reflecting the metabolic status at the cellular level is not ordered.
3) Symptoms of low metabolism are not considered during consultation when chronic illnesses are presented. Even if reported they are not linked because
4) Current evaluation and treatments are concerned only with T4 and TSH levels which do not accurately reflect cellular function which is predominantly controlled by T3 (four times stronger than T4).
So, conversely; if cellular metabolism were raised to an optimum level, its function should improve and those resultant pathologic states resolve.
This would happen when:
1) cells have an Optimal exposure to FT3 stimulation (upper 20% of normal range)
2) The normal ratio of TT3/RT3 is established (10:1); reflecting the total stimulatory and inhibitory cellular environments.
3) Keeping the T4 levels in the low normal or just below the low normal range to preserve normal T4 metabolism.
TSH is considered the least important variable since it plays no direct role in the conversion of T4 to T3 or RT3 – the metabolic on-off switch. TSH only controls the
manufacture and release of T4 and a little T3 from the thyroid gland. The main metabolic switch is located within the cell membranes where there are no TSH receptors.
Accurate measurements are necessary to obtain average FT3 levels.
To account for T3’s 6hr half-life theT3 dosages are halved, given twice a day, with repeat blood testing 6hrs after the last dose after allowing 3weeks for equilibration.
Current metabolic elevation goals treating with T4 (levothyroxine) often results in RT3 elevation and may not elevate FT3. Current treatment goals seek to keep the T4 level below the high normal and the TSH from being too suppressed which can be associated with hyperthyroidism (contributing to osteoporosis) and thus causes physicians to undertreat even with T4. The existing protocol does not address the cellular environment or cellular functional requirements. It places too much emphasis on pituitary gland’s TSH levels. Cellular low metabolism can occur with high, normal, or low TSH levels. “Subclinical Hypothyroidism” is often diagnosed but treatment with T4 fails to relieve symptoms (even though the TSH decreases) [14].
Patients suffering from chronic or recurrent ENT complaints were evaluated for evidence of low metabolism by reviewing their past medical history for chronic illnesses, medications, and questioning them for hypothyroid symptoms including: excessive tiredness, coldness, dry skin, brittle nails, hair loss (women), and constipation. If a patient had two or more hypothyroid symptoms, then Metabolic Optimization was recommended in addition to standard medications if needed. Liothyronine 5mcg po bid with empty stomach (morning and two hours after lunch) was prescribed and follow-up scheduled for 10 days after their next thyroid profile in three weeks. During the follow up accurate dosages and blood test timing are confirmed. Percentage improvements, thyroid levels, and any side effects are discussed and recorded. The main side effects - heart palpitations, muscle cramping, heat intolerance, or headaches (indicating generic intolerance) are asked about.
If the Optimal Range was not achieved and there were no side effects, then the liothyronine dose was raised by 2.5mcg. in the am and then by 2.5mcg. pm with subsequent blood testings and follow-ups. Levothyroxine was also given to keep the FT4’s at 0.6 or above.
Side effects were minimized by stopping caffeine or other stimulants to minimize jitteriness or heart palpitations; and by treating with magnesium 200mg as needed to prevent muscle cramping.
Most arrhythmias including atrial fibrillation were not caused or aggravated by Optimization. Sleep disturbance was rare but taking the afternoon dose earlier
helped. Some sleep disturbances were alleviated by Optimization by improving awake time and thereby improving sleep. Postmenopausal hot flashes can some times prevent achieving Optimal Metabolism. Sub-optimal dosing or other treatments to may be indicated.
Once Optimal Metabolism is reached, patients would continue that dosage if there were sufficient improvements with minimal side effects. The repeat blood testing would gradually decrease to once every five months. Dosages were changed as needed to keep the thyroid profiles in the optimal range.
Other categories were created later (*) - therefore under recorded because they were often reported. For example, Far Fewer Infections and Decreased Medication Use with subcategories - steroids, antihistamines/decongestants, and antidepressants. Overweight category was included because of its prevalence, its impact on slowing metabolism, and to characterize the possible weight loss benefits of Optimization. The data from the patient charts was entered into an Excel spreadsheet for analysis. Maximum percentage improvements were entered. Zero was entered if there was no improvement. The API for each category and system was then calculated (Graph 1).
Statistical analysis
There were 658 patients with diagnoses of hypothyroidism in my EHR. Of those, 370 were recommended for Metabolic Optimization. Their results were recorded in Excel where all the percentages and participations in the categories were summed and the average percentage improvements (API) calculated. The most important page was created analyzing the 165 patients who reached Optimal Metabolism. Their APIs, side effects, and additional information were recorded.
T test results
P values <0.05 were calculated for 23 of the 38 categories, proving that the treatment caused significant differences. P values were >0.05 for 3 categories, demonstrating insignificant differences.
I evaluated the results of raising metabolism in 370 patients, 165 reached Optimal Metabolism. Symptoms gradually improved with escalating doses with maximal improvements reported when reaching and remaining in the Optimal Range. In this group that reached Optimal Metabolism the
API for the Immune System was 63%. The specific categories are as follows: Allergic Rhinitis API - 56%. Allergy medicines decreased* – 34%. Allergy medications more effective* – 5.6%. Decreased prednisone use* – 5.6%.
Food Allergies API – 44%. Hives API -78%. Chronic Pharyngitis API - 35%.
Chronic Laryngitis API - 33.3%. Chronic Sinusitis API - 75%. Chronic Bronchitis API - 92.5%. Eustachian Tube Dysfunction API - 52.7%. Asthma API - 63.3%.
Chronic Oral Aphthae API - 75%. Far Fewer Infections* – 7.2%.
Raynauds Disease - API - 50%. Temporal Arteritis API - 100%.
Rheumatoid Arthritis API - 0%. Osteoarthritis API - 0%. Lupus API- 0%.
The API for Neurology was 80.36%. The specific catagories are as follows: Excessive Tiredness API - 81%. Excessive coldness API - 82%. Otoneurologic improvements including Vertigo reduction - 90% API. Dizziness API – 96%. Meniere’s Disease API - 89%. Migraine API – 90%. Headaches API – 77%. Trigeminal Neuralgia API - 100%. RSD (Reflex Sympathetic Dystrophy/Burning leg syndrome/Complex Regional Pain Syndrome) API - 100%. Neuropathies API of 92.5%. Depression API - 46%. Reduced antidepressant medications – 67%. Chronic Fatigue/Fibromyalgia API - 20%.
The API for Dermatology was 70%. Specific catagories: Dry Skin had an API - 71%. Hives API - 78%. Rashes API - 100%. Urticaria API - 80%. Eczema API - 53%. Blepharitis API - 94%. Excessive hair loss [women] API - 65%.
Brittle nails API - 83%.
In Gastroenterology Constipation (slow motility) API - 72%.
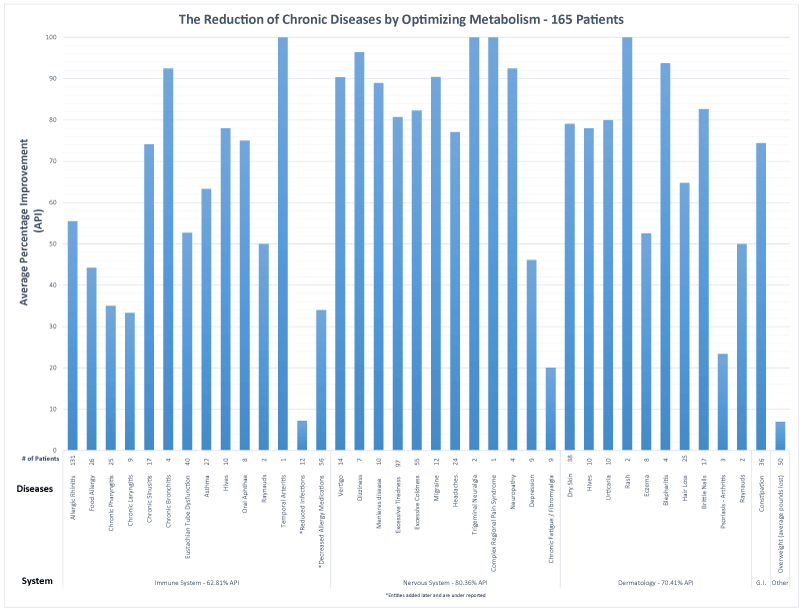
Figure 1. The reduction of chronic diseases by optimizing metabolism -165 patients.
Overweight
50 patients had a 7 lbs. average weight loss.
OBGYN
Positive effects include regulation of menstrual periods; reduction in menorrhagia; and help with fertility.
Resistance from endocrinologists and general medical doctors is significant because the TSH becomes suppressed both with Optimization and in hyperthyroidism. However, unlike Optimization, hyperthyroidism is a hypermetabolic state that can aggravate osteoporosis and arrhythmias. If the bones are experiencing a net loss, then treating that problem directly is necessary with vitamin D3, vitamin K2, Ca++, exercise, and/or bone-stimulating drugs. I have not seen accelerated deterioration of osteoporosis or osteopenia on serial bone density studies due to Optimization. Patient L.C. whose metabolism was Optimized over the last three years, reported an increase in bone density on serial bone densitometry despite her TSH continually suppressed (current – 0.022). TSH is a poor indicator of metabolic status. It can be high, normal or low in patients with low metabolism.
Here are three particularly interesting cases:
- R.C. is a 47 year-old male, S/P total thyroidectomy (papillary carcinoma), post RAI and on levothyroxine 150mcg/d. He presented with perennial allergies, recurrent sinusitis and bronchitis in spite of repeated antibiotics and steroids both IM and PO. He had many primary doctor visits and was frequently out of work. He was also excessively tired and depressed and on klonopin. I initially treated him with azelastine spray and ordered my thyroid profile: FT3 - 3.3 , TT3/RT3 - 3.7. I Optimized his metabolism on levothyroxine 75mcg plus liothyronine 12.5mcg am/10mcg pm. His thyroid profile on this dosage: FT3 - 4.1, TT3/RT3 - 10.4, TSH - 0.053 (continued suppression needed to repress any papillary thyroid cancer remnants).
His immune and nervo2021 Copyright OAT. All rights reservrgies are mostly gone -rarely using azelastine. He no longer gets sick and is back to work. His excessive tiredness is 100% gone. His depression is 100% gone. He is no longer on klonopin.
- S.S. is a 55 year-old female complaining of ear problems with tinnitus, fullness, and itching in the left ear; frequent vertigo treated with meclizine; seasonal allergies treated with Benadryl; She had frequent sinus headaches triggering migraine headaches. She also reported recurrent bronchial infections. She was on multiple psychotropic medications for anxiety, depression, and ADD. She was premenopausal with hot flashes. She was excessively cold and also suffered from dry skin and severe constipation. Audiometry confirmed mild Eustachian tube congestion in the left ear. Treatment with azelastine spray helped some but didn’t resolve the left aural fullness, dizziness, and headaches. Her baseline thyroid profile: FT3 - 3.2, TT3/RT3 - 6.18, TSH - 3.27, FT4 - 1.21. Metabolic Optimization after 3 years:
FT3 – 3.8, TT3/RT3 – 12.34, FT4 – 0.8, TSH – 0.012 taking liothyronine 10mcg am/7.5mcg pm and levothyroxine 75mcg am. Her migraines, headaches, vertigo, aural fullness, itching, bronchitis, and allergies have completely resolved (off azelastine).
- K.P. is a 71 year-old female who complained of headaches, vertigo (MRI --), dizziness (meclizine - no help), left aural fullness, pain and “thyroid issues” with dry skin, severe constipation, hair loss (treated with Rogaine) and brittle nails. +GERD with gas. She denied seasonal allergies. I treated her acute sinusitis and otitis media with clarithromycin, medrol dospak, and ordered my thyroid profile. On follow-up the patient reported only mild improvements. Her baseline profile was: FT3 -3.3, TT3/RT3 –5.1, FT4 –1.74, TSH –2.75, TT3 –101, RT3 –19.8. Note that the FT4 level was just below the high normal of 1.77. I then treated her with liothyronine 5mcg bid. Her profile quickly Optimized to FT3 -3.8, TT3/RT3 – 15.46, FT4 – 0.97, TSH – 1.49, TT3 – 150, RT3 – 9.7. Her dizziness was 100% gone; dry skin 100% gone; constipation 80% better, hair loss 90% better, brittle nails 100% better. She didn’t follow up and ran out of medication. Her internist refilled it instead with levothyroxine 50mcg. (reported to be equivalent)! When I saw her again she reported she couldn’t sleep for the last four months; her hair was falling out, her dizziness was returning; and despite stopping the levothyroxine she was only marginally better. I restarted liothyronine 5mcg bid. With her thyroid profile Optimized she became asymptomatic again.
Optimizing Metabolism is very different from the current system of raising metabolism. Optimizing Metabolism is a concept that is currently unknown, unpublished, and not currently in clinical consciousness or used in clinical practices. We are inundated with ads and supplements that claim to “boost metabolism,” yet they offer no measureable evidence to evaluate those claims besides a few patient testimonials. I present for the first time a measureable way to evaluate and treat this pervasive disorder. Knowing what the Optimal Range is and accurately obtaining measurements facilitates and tailors this treatment to each individual patient. I have found that every patient responds differently, with different sensitivities, tolerances, dosages, and trigger points where their systemic dysfunction ensues. Gradual symptomatic improvements are typical during the optimization process.
Previously a “large number of systemic diseases and other clinical situations have been associated with what is called low T3 syndrome” [1,10,11].
Low T3 levels were often accompanied by elevated levels RT3.” High MICU mortality associated with these levels [2,11].
The balance between the 5’deiodinase enzyme producing T3 and the 5 deiodinase enzyme producing RT3 determines the metabolic status of that cell plus the amount of T3 absorbed directly through its own cell membrane channels [3]. Reduced cellular metabolism results when T4 is converted to the inactive isomer RT3 by the 5 deiodinase enzyme. RT3 further slows metabolism by selectively inhibiting the 5’deiodinase enzymatic action on T4 [4,5]. Also, low intracellular reduced glutathione levels (inflammatory diseases and aging) further reduce the efficacy of the 5’deiodinase enzyme, further reducing intracellular T3 [6,12].
When T3 levels are increased inside the cell, they bind to receptors on the mitochondrial DNA, increasing the production of ATP. T3 also binds to peroxisomes increasing the breakdown of long chain fatty acids for continued energy production. T3 also binds to nuclear receptors stimulating transcription of proteins that are involved specifically with that cell’s activities. T3 also causes the increase in growth hormone and IGF-1 which also increases the conversion on T4 to T3 [7].
All these processes increase cellular function.
When obtaining Optimal Metabolism TSH becomes the least important variable measured because it controls only the manufacture and release of T4 (mostly) from the thyroid gland. There is no guarantee that the released T4 would be converted to T3 instead of RT3 – often it is not (eg. inflammation, insulin resistance). The vast majority of T3 is manufactured in the liver from T4 and within the cell membranes in the body. This is not directly under TSH control.
Low metabolism is a huge problem that includes Subclinical Hypothyroidism. Chronic diseases like allergies beginning or worsened as an adult suggests low metabolism as the underlying etiology. Allergy testing may be negative. Other illnesses or trauma cause metabolism to slow as well [5,11]. Obesity, insulin resistance, PCOS, and type II diabetes slow metabolism by preferentially converting T4 into RT3 instead of T3 [11]. This may be the mechanism underlying poor healing and immune systems associated with diabetics. Optimizing Metabolism may repair this immune dysfunction. In this study, 6.7% of the patients reported far fewer infections than they would normally get. Other chronic illnesses like osteoarthritis increase intracellular inflammation slowing metabolism [8]. Patients with multiple chronic diseases, on chemotherapy, in the ICUs [11] or in labor and delivery can all have lowered metabolism due to the significant traumas these conditions impact upon the body [12]. Resilience in these patients could improve by optimizing their metabolisms [13].
Obesity is a huge health problem. Optimizing Metabolism can help with weight loss by eliminating excessive tiredness that often prevents exercise and dieting. In this study 93 patients had an API 82.3% eliminating excessive tiredness. Now these patients have the mental energy to exercise and diet when they did not before. There were 48 patients who were overweight and “dieting” and had reached the Optimal Metabolism. They reported an average weight loss of 7 pounds without changing their current dieting habits. Some of these patients were not dieting too seriously where others had been stymied despite multiple diets with exercise. One particular patient - C. M. - lost 48 pounds [9]. Also her depression improved 100% and she stopped all her psychotropic medications. She was no longer excessively tired and her allergies improved by 60% as well.
Optimal Metabolism can be seen as both therapeutic and preventative. It is holistic in its scope benefitting general medicine and all of the specialties. It is at this inflection point that one can intervene and break the destructive cycle of metabolic syndrome, obesity and other inflammatory diseases and dysfunctions.
One can consider the thyroid to be the thermostat and the adrenals the furnace. Both systems should be considered for optimal function. Adrenal hormone testing, adrenal supplementation and HRT are also considered. Additional ways to improve cellular function include increasing intracellular glutathione levels. Glutathione is the cell’s premier antioxidant but declines 10% per decade after age 20 and it is greatly lowered by inflammation. There are supplements that increase intracellular glutathione levels, reducing intracellular inflammation thus facilitating energy production [7, 8,12].
There are many conditions that lead to low metabolism, the consequences of which cause increased dysfunction and disease. Low metabolism is very common because of aging and maladaptive hypothyroidism due to inflammation, obesity and illnesses. Low T3 states including Subclinical Hypothyroidism have been known for many decades but not accurately measured, diagnosed, nor successfully treated with T4 [14]. Understanding cellular requirements for optimal function is a valuable, powerful perspective. It takes into account all the thyroid hormones and in their order of importance impacting cell physiology. From a practical standpoint the Optimal Range serves as an accurate measure against which patient values can be compared and could serve as a treatment target considering their existing symptoms, diseases and medications. Obtaining Optimal Metabolism consistently correlates with the least amount of disease in that selected individual as long as they have one or two typical hypothyroid symptoms. This treatment is safe, powerful, readily available, reproducible, and should be a valuable treatment consideration. Optimal Metabolism improves patient health spans and productivity by eliminating chronic diseases. It can turn the most refractory and disabled patients into remarkable successes.
Optimizing Metabolism can result in huge monetary and productivity gains for the patients and society as chronic and recurrent illnesses decrease. As life spans are increasing health spans must also increase. Today, cost estimates due to allergies alone are in the billions of dollars. If this treatment protocol can reduce inhalant allergies by 59% and food allergies by 44% the cost savings would be tremendous. Reductions in hospitalizations, repetitive expensive medical testing, and the numbers of disabled also would reduce insurance and medical costs substantially.
This retrospective review proves that Metabolic Optimization is safe but does not prove causality. As a Pragmatic Trial, this study could not be double-blinded nor placebo controlled and therefore cannot eliminate the biases of both the physician and the patients. However, it was objectively controlled by accurate blood testing and accurate medical chart documentation. A multicenter placebo-controlled trial should be undertaken given the magnitude and substantial implications of these improvements. Optimization should be a part of all medical, and specialty training. The public’s health and wealth depend upon it.
I would like to thank Alan McDaniel, MD whose insights and study groups were instrumental developing this concept; Kimberly Murphy for her Excel and statistical help; Michael Levine for his help with Excel and the Graph; and Steven Levine and Mary Levine for their editing expertise.
- Wartofsky L, Burman KD (1982) Alterations in thyroid function in patients with systemic illness: the “euthyroid sick syndrome. Endocr Rev 3: 164. [Crossref]
- Chopra IJ, Solomon DH, Chopra U, Wu SY, Fisher D, et al. (1978) Pathways of thyroid hormones. Rec Prog Horm Res 34: 521.
- Kohrle J, Brabant G, Hesch RD (1987) Metabolism of thyroid hormones. Horm Res 26: 58. [Crossref]
- FaberJ, Farancis Thomsen H, Lumholtz IB, Kirkegaard C, Siersback-Nielsen K, et al. (1981) Kinetic studies of thyroxine 3,5,3’-triiodothyronine, 3,3’,5’-triiodothyronine, 3’,5’-diiodothyronine, 3,3’-diiodothyronine, and 3’-monoiodothyronine in patients with liver cirrhosis. J Clin Endoinol Metab 53: 978.
- Vagenakis AG, Portnay GI, O'Brian JT, Rudolph M, Arky RA, et al. (1977) Effect of starvation on the production and metabolism of thyroxine and triiodothyronine in euthyroid obese patients. J Clin Endocrinol Metab 45: 1305. [Crossref]
- Chopra IJ, Huang TS, Beredo A, Solomon DH, Chua Teco GN, et al. (1985) Evidence for an inhibitor of extrathyroidal conversion of thyroxine to 3,5,3’-triiodothyronine in sera of patients with nonthyroidal illnesses. J Clin Endocrinol Metab 60: 666. [Crossref]
- Grunfeld C, Sherman BM, Cavalieri RR (1988) The acute effects of human growth hormone administration on the thyroid function in normal man. J Clin Endodrinol Metab 67: 1111. [Crossref]
- Tibaldi Jm. Surks MI (1985) Effects of nonthyroidal illness on thyroid function. Med Clin North Am 69: 899. [Crossref]
- On HCG Diet protocol.
- Wilson, E Dennis (1966) Wilson’s Syndrome The Miracle of Feeling Well, 3rd ed., Orlando, Fla: Cornerstone Publishing Company, 20-21.
- Moura Neto A, Zantut-Wittmann DE (2016) Abnormalities of Thyroid Hormone Metabolism during Systemic Illness: The Low T3 Syndrome in Different Cinical Settings. Int J Endocrinol.
- Vidart J, Wajner SE, Leite RS, Manica A, Schaan BD, et al. (2014) N-Acelylcysteine Administration Prevents Nonthyroidal Illness Syndrome in Patients with Acute Myocardial Infarction: A Randomized Clinical Trial. J Clin Endocrinol Metab 99: 4537-4545. [Crossref]
- Pingitore A, Galli E, Barison A, Iervase A, Scarlattini M, et al. (2008) Acute effects of Trioodothyronine (T3) replacement therapy in patients with chronic heart failure and low T3 syndrome: a randomized, placebo-controlled study. J Clin Endocrinol Metab 93: 1351-8. [Crossref]
- Stott DJ, Rodondi N, Bauer DC, TRUST Study Group (2017) Thyroid Hormone Therapy for Older Adults with Subclinical Hypothyroidism. NEJM. [Crossref]

