Corneal disease is the fifth leading cause of blindness in the world. Corneal transplant surgery is the standard of care and a vision saving procedure. Visual outcome in these patients is mainly dependent on adherence to medication and attendance to follow up appointments. We aim to analyse factors responsible for poor adherence in corneal transplant patients via an interprofessional approach, such as to provide a theoretic perspective of integrating medical science, nursing science, behavioural sciences and information technology. This paper displays an in-depth analysis of factors responsible for poor compliance from a multidimensional perspective including socio-economic, cultural, medical, behavioural and cognitive, thus providing a holistic overview. We reviewed articles to consider medical, surgical nursing, technological and healthcare system related interventions. With this background, we have designed a concept map that displays various interventions to improve adherence to treatment. We recommend a patient centred approach along with close collaboration among healthcare organizations, ophthalmologists and ophthalmic care personnel to combat treatment failure in corneal transplants by emphasizing holism, embracing meaningful interactions, and utilizing continuous feedback. The concept of general systems theory can be applied to improve treatment outcomes of corneal transplant patients via a multidimensional approach beginning from behavioural changes at an individual level, healthcare reforms at an organizational level, and technological modifications at a global level.
corneal transplant, adherence, compliance, interprofessional, patient centered
Corneal transplant surgery was first described in 1951 by Ramon Castroviejo as a method for replacing a large area of diseased cornea with donor corneal tissue [1]. Corneal transplant is a vision-saving procedure and is the most common type of human transplant surgery [2]. Complimentary intensive medication is essential to avoid surgical treatment failure, which would lead to severe visual loss or even loss of the globe. Long-term use of oral and topical steroid eyedrops is crucial to prevent treatment failure. Therefore, the prognosis of successful corneal transplant surgery is mainly dependent on compliance to medication and adherence to frequent follow-up visits [3]. Apart from this corneal transplant patients must also conform to lifestyle changes such as wearing protective goggles, strict blood sugar control, and avoiding contact sports. Sometimes despite the surgical success, vision may not be restored due to other co-morbid eye conditions such cystoid macular edema, retinal detachment, glaucoma, and cataract [4]. This makes the management of corneal transplants highly capricious and complex.
Corneal disease is the fifth leading cause of blindness in the world. According to the WHO, about 39 million people worldwide are blind, of whom 12%, or about 5 million, have corneal blindness [5]. The most common indication for corneal transplant in developing countries is infectious keratitis and corneal scarring [6,7] whereas bullous keratopathy, Fuchs endothelial corneal dystrophy, and keratoconus attributes to the majority in developed countries [8]. Average corneal graft survival after best possible surgical outcomes and follow-up regimens is 74% at 5 years and 64% at 10 years. The corneal graft survival further reduces to 27% at 20 years and 2% at 30 years [9]. Maximizing the chance of graft survival is important, as the risk of graft failure increases with each subsequent transplant. Moreover, a global survey reported a considerable shortage of corneal graft tissue, with only one cornea available for 70 needed [10].
Recipients aged 60 years or more constitute an important subset of patients referred for corneal transplantation. The proportion of elderly recipients undergoing surgery has increased over 10 years [11]. It has been found that elderly graft recipients don’t fare well after corneal transplantation as compared to younger recipients. Poor adherence to treatment is one of the major causes of treatment failure in corneal transplant patients. Interestingly, the rate of non-compliance observed in corneal transplant recipients is considerably higher than the rates reported in other forms of organ transplantation [12]. It is commonly assumed that patients are solely responsible for their non-compliance. A corneal graft may fail because of several other reasons such as poor quality of the donor button, inadequate donor button storage and transport facilities, lack of infrastructure to preserve donor corneal buttons, poor surgical technique, and suboptimal healthcare delivery services. Unlike other organ transplants such as kidney, liver, or heart, corneal transplant is not a lifesaving procedure. It is not uncommon to notice laxity in compliance if the other eye of the patient has good vision. Missed appointments are an important cause of inefficiency in healthcare delivery and are associated with substantial monetary costs [13,14]. Poor attendance in office appointments correlates with failure to continue medication, a phenomenon known as "no show, no drops" [15]. This is of particular significance in a public health care system given the limited availability of both physical and human resources [16].
Poor compliance could lead to treatment failure on a long-term basis, despite initial surgical success. Several studies have demonstrated the importance of timely access to skilled ophthalmologists, adherence to the scheduled follow-up visits, and long-term compliance to steroid eye drops to avoid graft rejection [17]. The purpose of this paper is to analyse factors responsible for poor adherence in corneal transplant patients via an interprofessional approach. By interprofessional approach, we plan to provide a theoretic perspective of integrating medical science, nursing science, behavioral sciences, and information technology to improve adherence and enhance visual outcomes in corneal transplant patients.
Adherence or compliance refers to the extent to which a person’s behavior corresponds with the agreed recommendations of a health care provider [18]. Compliance is a complex healthcare concept comprising multiple patient factors [19]. The term adherence rather than compliance is preferred by many health professionals as it implies a therapeutic alliance between the patient and the physician as opposed to a paternalistic relationship [16]. A multitude of indirect measures of adherence exist in the literature, however, there is no “gold” standard for measuring adherence to medications. Triangulation of methods increases the validity and reliability of the adherence data collected [20].
The concept map (Figure 1) provides a comprehensive overview of various concepts and their relationship to each other regarding compliance in corneal transplant patients. According to WHO lack of adherence to treatment attributes to factors which are condition related, therapy- related, patient-related, socio-economic and healthcare team and system-related [18]. As poor compliance in corneal transplant is more common in elderly patients, the sub-concept, age, is further elaborated to describe how old age could contribute to transplant failure [11,21]. The second branch of the concept map is a flow chart on the consequences of poor compliance on corneal transplant patients. The flow chart depicts a cascade of events related to poor compliance leading to transplant failures and its economic drawbacks.
Figure 1. Factors Affecting Compliance in Corneal Transplant Patients
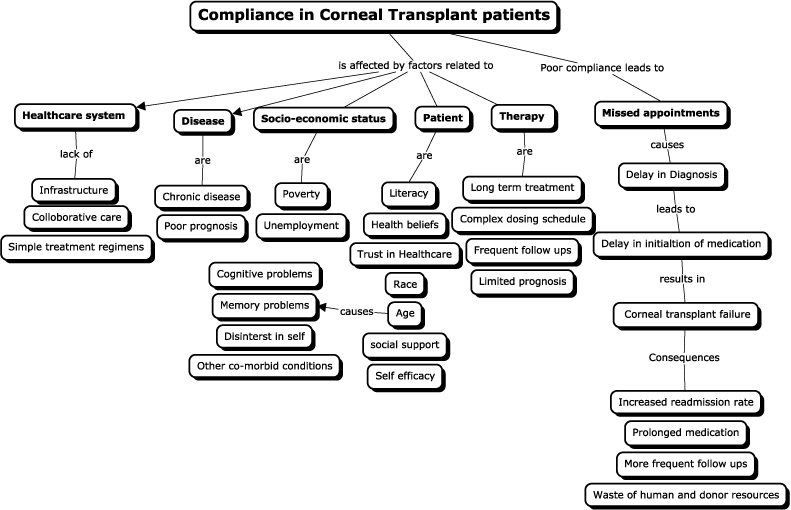
This concept map provides a comprehensive overview of various factors affecting compliance in corneal transplant patients and consequences of poor compliance.
1. Social and Economic factors
Factors known to have a significant effect on adherence include poor socio-economic status, poverty, illiteracy, low level of education, lack of effective social support network groups, unstable living conditions, high cost of transportation, high medication cost, culture and lay beliefs, and family dysfunction [18,22,23]. The lack of knowledge on the disease and understanding of long-term therapy would lead to poor acceptance of the condition which in turn would influence compliance. The cost of treatment is another important factor to be considered while the physician expects long-term compliance to treatment [24]. In developing countries, providing affordable care should be the goal to ensure good follow-up and long-term treatment. Race could influence treatment wherein certain cultural beliefs play a role in treatment acceptance [19]. Age is another important factor to be considered while ensuring adherence. Concerning corneal transplant, both extremities of age have demonstrated poor compliance due to various factors. Studies have suggested adolescents are less adherent than younger children [25]. In the elderly, the prevalence of cognitive and functional impairments increases the risk of poor adherence [26] (Figure 1). Moreover, elderly age group also present with multiple chronic diseases which require complex long- term treatment which further complicates adherence. Like in other chronic ocular conditions such as glaucoma, gender may play a detrimental role in families with a low socio-economic status where treatment of a male child gains priority over a female child [27,28]. Patients who became unemployed or retired after transplantation were also significantly less able in both visual functioning and socio-emotional status [29].
2. Health care team and system-related factors
Building a good doctor-patient relationship is vital to good adherence. Poorly developed health services, lack of knowledge or training of health care providers, overworked health care providers, inadequate counselling, and follow-up appointments would add to the burden of non-adherence. It is essential to provide health care services at the root level to improve patient adherence and follow-up. Additionally, this helps to bridge the gap between a primary and tertiary care center. Another study demonstrated that a more extensive transportation process correlated with significantly poor compliance [30]. Many times, eye care hospitals are stand-alone systems that are not integrated with other medical specialties. This becomes an additional burden to corneal transplant patients with other co-morbidities to find a single-stop care center to manage multiple coexisting disease conditions.
3. Disease Condition related factors
Disease condition-related factors relate to demands and factors such as the severity and level of disability that can significantly influence adherence. Patients who received bilateral corneal grafts were significantly less able socioemotionally than those with unilateral grafts. Corneal transplant failure could result in pain and loss of vision which could enhance patient’s dependence on caretakers. Thus, leading to a vicious cycle of poor compliance resulting in poor prognosis and so on. The need for long-term adherence in terms of months to years further affects their quality of life adding on to poor compliance. The association of depression with this ailment is another important modifier of adherence behavior. Depression could also influence a patient's self-perception of the burden of eye disease and treatment effectiveness. It is therefore important to identify corneal graft recipients who are at risk of developing depression given the availability of effective treatment for the condition. Corneal transplant recipients had a decreased vision-related quality of life as demonstrated by the National Eye Institute Visual Function Questionnaire-25 (NEI VFQ-25) [29].
4. Therapy-related factors
The cost and duration of treatment, the complexity of the medical regime, multiple drug prescribers’ previous treatment failures, delayed symptomatic improvements, drug side-effects adversely affect adherence [31].
5. Patient-related factors
This represents the knowledge, resources, attitudes, beliefs, perceptions, and expectations of the patient. A person's educational level (formal/informal/self-taught) is shown to have implications for health literacy such as following instructions prescribed by the provider and adhering to treatment protocols [32]. Factors like forgetfulness, psychosocial stress, inadequate knowledge about the disease and possible adverse effects, non-acceptance of the disease, hopelessness and negative feelings, frustration with health care providers adversely affect adherence. Older patients are more likely to have difficulties with eye drop administration due to problems with manual dexterity, difficulty in self-instillation wherein the patient has difficulty in tilting the head back, tremor of hands with various degrees of visual impairment. Furthermore, memory problems make it difficult for the elderly to follow a complex eye drop regimen. Lack of family or social support, disinterest in self-care, and associated comorbid conditions adversely affect adherence [21]. Most of the corneal transplant patients are either elderly or paediatric age group. Therefore, caretaker stress is another important factor to be considered as transplant patients are dependent on their caretakers for financial and cognitive support. Apart from bearing the financial burden of long-term follow-up, caretakers are challenged with frequent absenteeism from work due to long-term frequent follow-ups. Patients who prioritize health are expected to show higher levels of appointment compliance. Patients receiving treatment in the private sector may have chosen to emphasize health as a priority over other competing demands on their resources. Given the associated expense, patients who seek private health care could be considered to have greater financial security. Financial security facilitates attendance by allowing greater flexibility with time away from work, transport and parking issues, and childcare [33].
Treatment adherence after penetrating keratoplasty in a New Zealand population reported a considerably higher rate of nonattendance (10.5%) than that observed in other forms of organ transplantation. A ten-year follow-up study of 695 corneal transplant procedures reported good appointment compliance in 68.5%, moderate in 26.3%, and poor in 4.9% of the patients. The mean number of scheduled appointments was 14.6± 7.2 (range, 1-79) [33]. Lost to follow-up (LTFU) was associated with ethnicity and socioeconomic factors. Long-term follow-up is essential to ensure maximal corneal graft survival by early detection of potential post-operative complications such as graft rejection, traumatic dehiscence, increased intraocular pressure leading to glaucoma, infectious keratitis, and suture-related complications. [34] A recent study on 118 patients undergoing corneal transplants in Kenya, East Africa reported 33.9% of patients were lost to follow up at least one year postoperatively [22]. Specific reasons for LTFU in the study population from East Africa include financial barriers, confusion surrounding follow-up instructions, and not sensing the need to return. The odds of LTFU for patients age 60 and older were 3.78 times that of those who were age 18-59. Education level, employment status, distance from the hospital, and possession of a mobile contact number were marginally associated with follow-up status [22]. Patients who travelled more than four hours one way to and fro from the hospital are more likely to be LTFU. This is in contrast to the study by Crawford, et al. where higher rates of appointment adherence were inversely associated with proximity to treatment center [33]. This could be one major difference between the developing and developed nations wherein, the funding for post-operative visits is a responsibility of the district health boards, and travel expenses are covered if a patient is required to travel outside of their district to receive health services indicating that hospital and federal policies play a vital role in determining compliance to treatment.
A meta-analysis examining the rates of nonadherence in solid organ transplantation reported the following rates of nonattendance: all types 5.8%, kidney 4.7%, and heart 8.5% [12]. Among adult liver transplant patients, the rate of non-adherence to immunosuppressive drugs ranges from 15% to 40%, whereas the rate of nonadherence to clinical appointments ranges from 3% to 47% [35]. The prevalence of nonadherence to prescribed medications after lung or heart transplantation has been reported to vary between 1% and 43% [36]. To screen for medication adherence status, the four-item Morisky Medication Adherence Scale with dichotomous response options is used. This is a standard tool for assessing medication adherence with a reliability coefficient (Cronbach's α) value of 0.61 [37].
Clinical definition of successful corneal transplantation is often based on the postoperative anatomical outcome and visual acuity. However, these criteria do not necessarily correlate with the patient's performance of daily activities. Apart from anatomical success and visual acuity, ophthalmologists should also consider other aspects of visual outcomes. Compliance may be assessed with reference to medication compliance, conforming to lifestyle recommendations, and attending follow-up appointments. Therapeutic adherence has been extensively studied from pharmacological, behavioral, and economic perspectives. However, there is a lack of uniformity in the methods of analysis as each of these studies was conducted from a particular perspective, leading to significant lacunae in identifying and implementing strategies to tackle poor compliance in corneal transplant patients. This paper displays an in-depth analysis of factors responsible for poor compliance from a multidimensional perspective including socio-economic, cultural, medical, behavioral, and cognitive, thus providing a holistic overview.
One of the most current definitions of compliance is ‘the extent to which a person’s and/or caregiver’s behavior coincides with a health-promoting or therapeutic plan agreed upon by the person (and or family or community) and health care professionals [38]. This definition does not restrict interventions at the individual level, rather expands it to a multilevel, taking into account several invisible factors such as family, social and ecological circumstances. For instance, poor compliance to treatment should not be attributed to individual behaviors, beliefs, and lifestyle factors alone. Poor compliance should also be viewed from a broader perspective such as lack of family support, poor social and community networks, poor living and working conditions, hospital and federal healthcare policies. With this background, our research team has designed a concept map (Figure 2) that displays various interventions to improve treatment adherence. These include medical, surgical nursing, technological, and healthcare system-related interventions.
Figure 2. Strategies to improve compliance in corneal transplant patients
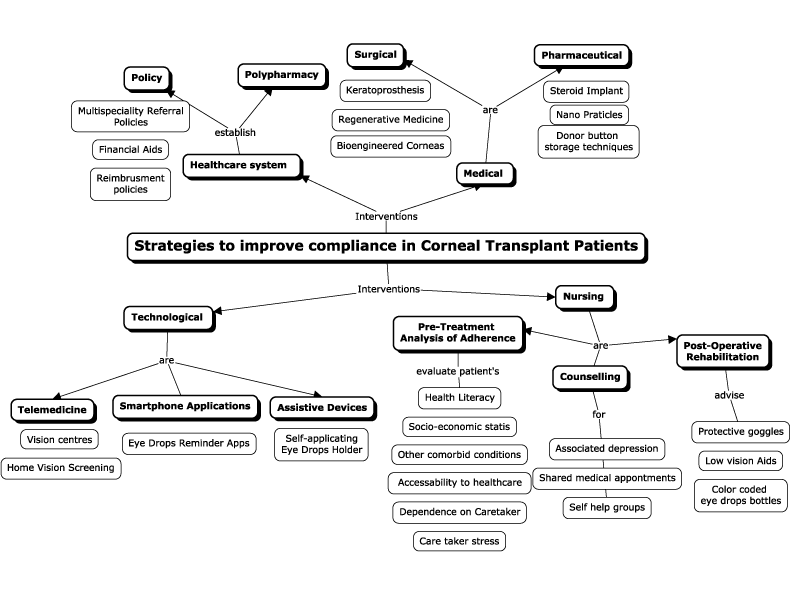
This concept map enlists multidisciplinary interventions to improve compliance in corneal transplant patients.
Ophthalmologists and other ophthalmic care providers must be able to view compliance from a cultural, social, and economic perspective without evaluating or rationalizing patient’s attitude to compliance. Such an approach refrains pitfalls such as coercion and paternalism and promotes patient-centered healthcare delivery. Ophthalmologists can promote engagement in care by being patient educators, advocates, and rehabilitators. To achieve this, ophthalmologists may have to expand their domain of interest from medical science to information science, social science, biological science, and behavioral sciences. The authors have attempted to enlist multidisciplinary interventions to improve compliance in Corneal transplant patients (Figure 2).
Medical Interventions
Recent advances in the medical management of corneal transplant patients include using intravitreal steroid implants instead of daily doses of steroids [39]. A combined approach would open doors to interprofessional collaboration in designing strategies to improve compliance and expand the horizon from medical science to social, behavioral, and economic sciences. Healthcare providers could spend more time with the patient enquiring about the patient's affordability to eye drops, family support, ease of self-application of eye drops, ease of commuting to the healthcare center for follow-up visits, patient's knowledge of medications, patient's level of health literacy, and willingness to take medication. By this approach, the healthcare provider understands both direct and indirect factors that influence compliance and design a treatment plan customized to that patient. This is particularly effective in elderly patients who are unable to self-administer eye drops regularly due to cognitive and memory deficits. Furthermore, the advent of nanoparticles can help reduce the frequency of steroids by prolonged retention in the eye [40].
One major concern of treatment failure in corneal transplant is the loss of donor tissue due to poor compliance [10]. The scarcity of donor corneal buttons often results in inequality in the distribution of the tissues. Surgical and basic science innovations such as bioengineered cornea and keratoprosthesis have been promising, yet inadequate to tackle the expanding need for corneal buttons.
Nursing Interventions
As corneal transplants mandate long-term follow-up and limited visual prognosis, corneal transplant patients are vulnerable to develop depression which can, in turn, contribute to poor compliance. It is important to integrate human behavior with the therapeutic milieu in the treatment plan. Nursing interventions such as education, counseling, and post-operative rehabilitation play a crucial role in boosting confidence and improving compliance. Healthcare provider-patient relationships should be the center of such a practice allowing abstract features like a patient's beliefs, culture, and socio-economic status. Such a patient-centric approach transforms healthcare providers' attitude towards patients from paternal authoritative advice to normative ethical advice. The clinician tries to decide prescriptions based on values, behaviors, and ways of being right or wrong. Group interventions such as shared medical appointments and self-help groups not only provide a healing touch but also delivers a feeling of well-being. Adding more to this approach is a simultaneous paradigm for nursing as a discipline-defining alternative discourse to healthcare. This approach gives equal importance to the patient's perspective and encourages patient participation, in addition to valuing the caregiver's knowledge production. So, both the patient and the caregiver must be flexible to adapt to the changing environmental conditions and adopt newer strategies to their treatment plan. Such an approach incorporates a person's inherent potential for self-organization, innovative patterning, and connection to the environment and allows transformation from conventional care to composite care where acceptable traditional methods could also be added. Eventually, facilitating a stronger patient-provider partnership, encouraging family participation and community involvement.
Technological interventions
Technological interventions such as 3-D printed self-applicating eye drops stand can address cognitive deficits in the elderly reducing their dependency on caretakers and family [41]. Patients with memory disorders and those having difficulty managing treatment regimens can be trained to use smartphone applications such as eye drops reminder applications. This will ensure correct and timely dosing of steroids which are crucial in the management of corneal transplant patients. Telemedicine facilities along with hospital system-related interventions such as polypharmacy could be used to reach those who are unable to reach the base hospital. Teleophthalmology is one of the hopes for improving access to care in corneal transplant patients via an information-sharing framework for human services. As a majority of transplant patients are elderly with other comorbid conditions, client and family-centered services Web page should result in healthcare systems having a greater number of inputs, outputs, and interactions facilitating timely access to care.
Healthcare system-related interventions
To strengthen the adherence, research and practice interventions should use a standardized definition of medication adherence and clearly describe the medication adherence methods used. Healthcare systems must be able to develop an infrastructure to support prescribing, procuring, dispensing, and administering medications. Healthcare organizations must see themselves within the context of learning health systems (LHS) and use big data analytics techniques such as process mining to develop better, integrated, and personalized pathways of care for patients. Every factor influencing compliance such as corneal biology, immune response, human behavior, and socio-economic influences must be meaningfully integrated to provide customized care for corneal transplant patients [42]. In particular, those who received bilateral grafts require more attention. Employment programs should be part of corneal transplantation rehabilitation planning.
A holistic understanding of different sciences components could facilitate compliance to treatment in corneal transplant patients by revealing unquestioned premises layer by layer [32]. Such an approach is grounded in the premise that the world is composed of systems that are interconnected and influenced by one another. General systems theory (GST) is one such approach that recognizes the importance of ‘‘wholeness,’’ that is, the whole being greater than the sum of the parts [43]. GST can be used as a guiding framework for influencing healthcare delivery to focus on the big picture rather than the incremental pieces that fail to generate substantive change [44]. The inclusive perspective of GST can facilitate open communication between multidisciplinary stakeholders working for a common goal of achieving optimal health. Such an approach transforms the attitude of healthcare providers from an authoritative approach to a participatory approach avoiding branding of patients as “non-compliant”. The focus of treatment expands from restoring vision alone to restoring vision without compromising the patient's financial and mental stability. Healthcare providers become aware of their dominance and try to understand patient’s perspectives before designing a treatment plan by being cognizant of paternalistic principles and institutional power enforced on patients to bring out compliant behaviors. This expands the role of healthcare providers to educators, rehabilitators, and patient advocates, thus promoting engagement in patients. It also encourages healthcare providers to be more innovative while planning their treatment regimen and follow-up. Ocular Steroid Depot Implants can be tried instead of steroid eye drops to combat cognitive issues in self-applying eye drops. Some follow-up visits could be scheduled in the nearest vision center instead of the main hospital if traveling far distance is a concern. The option of telemedical facilities could improve patients’ adherence to following up without compromising their day-to-day activities and reduce dependency and stress of caretakers.
The prognosis of successful corneal transplant surgery is mainly dependent on compliance to medication and adherence to frequent follow-ups visits. Compliance is affected by diverse factors ranging from individual factors to social, healthcare system, and disease condition-related factors. A patient-centered approach along with close collaboration among healthcare organizations, ophthalmologists, and ophthalmic care personnel is critical to address corneal blindness related to corneal graft failures. Such an approach paves way for interdisciplinary solutions to combat treatment failure in corneal transplants by emphasizing holism, embracing meaningful interactions, and utilizing continuous feedback. The concept of GST can be applied to improve treatment outcomes of corneal transplant patients via a multidimensional approach beginning from behavioral changes at an individual level, healthcare reforms at an organizational level, and technological modifications at a global level.
The authors declare no conflict of interest.
The authors have no proprietary or commercial interest in any materials discussed in the manuscript.
The authors received no financial support for the research, authorship, and/or publication of this article.
- CASTROVIEJO R (1951) Total penetrating keratoplasty; a preliminary report. Am J Ophthalmol 34: 1697-1706. [Crossref]
- Waldock A, Cook SD (2000) Corneal transplantation: how successful are we. Br J Ophthalmol 84: 813-815. [Crossref]
- Krysik K, Wroblewska-Czajka E, Lyssek-Boron A, Wylegala EA, Dobrowolski D (2018) Total Penetrating Keratoplasty: Indications, Therapeutic Approach, and Long-Term Follow-Up. J Ophthalmol 2018: 9580292. [Crossref]
- Tan DT, Dart JK, Holland EJ, Kinoshita S (2012) Corneal transplantation. Lancet 379: 1749-1761. [Crossref]
- Resnikoff S, Pascolini D, Etya'ale D, Kocur I, Pararajasegaram R, et al. (2004) Global data on visual impairment in the year 2002. Bull World Health Organ 82: 844-851. [Crossref]
- Tabin GC, Gurung R, Paudyal G, Reddy HS, Hobbs CL, et al. (2004) Penetrating keratoplasty in Nepal. Cornea 23: 589-596. [Crossref]
- Pan Q, Li X, Gu Y (2012) Apr. Indications and outcomes of penetrating keratoplasty in a tertiary hospital in the developing world. Clin Exp Ophthalmol 40: 232-238. [Crossref]
- Park, CY, Lee JK, Gore PK, Lim CY, et al (2015) Keratoplasty in the United States: A 10-Year Review from 2005 through 2014. Ophthalmology 122: 2432–2442. [Crossref]
- Borderie VM, Boëlle PY, Touzeau O, Allouch C, Boutboul S, et al. (2009) Predicted long-term outcome of corneal transplantation. Ophthalmology 116: 2354-2360. [Crossref]
- Gain P, Jullienne R, He Z, Aldossary M, Acquart S, et al. (2016) Global Survey of Corneal Transplantation and Eye Banking. JAMA Ophthalmol 134: 167-173. [Crossref]
- Williams KA, Muehlberg SM, Lewis RF, Coster DJ (1997) Influence of advanced recipient and donor age on the outcome of corneal transplantation. Australian Corneal Graft Registry. Br J Ophthalmol 81: 835-839. [Crossref]
- Dew MA, DiMartini AF, De Vito Dabbs A, Myaskovsky L, Steel J, et al. (2007) Rates and risk factors for nonadherence to the medical regimen after adult solid organ transplantation. Transplantation 83: 858-873. [Crossref]
- White P, Gunston J, Salmond C, Atkinson J, Crampton P (2008) Atlas of Socioeconomic Deprivation in New Zealand NZDep2006. [pdf] Wellington: Ministry of Health.
- Car J, Gurol‐Urganci I, de Jongh T, Vodopivec‐Jamsek V, Atun R (2008) Mobile phone messaging reminders for attendance at scheduled healthcare appointments. Cochrane Database Syst Rev 2013: CD007458. [Crossref]
- Schwartz GF, Quigley HA (2008) Adherence and persistence with glaucoma therapy. Surv Ophthalmol 53 Suppl1: S57-68. [Crossref]
- Osterberg L, Blaschke T (2005) Adherence to medication. N Engl J Med 353: 487-497. [Crossref]
- Smith GT, Taylor HR (1991) Epidemiology of corneal blindness in developing countries. Refract Corneal Surg 7: 436-439. [Crossref]
- Sabaté E, Sabaté E (2003) Adherence to long-term therapies: evidence for action. World Health Organization.
- Matossian C (2020) Noncompliance with Prescribed Eyedrop Regimens Among Patients Undergoing Cataract Surgery—Prevalence, Consequences, and Solutions. US Ophthalmic Review 13: 18-22.
- Lehmann A, Aslani P, Ahmed R, Celio J, Gauchet A, et al. (2014) Assessing medication adherence: options to consider. Int J Clin Pharm 36: 55-69. [Crossref]
- Dietlein TS, Jordan JF, Lüke C, Schild A, Dinslage S, et al. (2008) Self-application of single-use eyedrop containers in an elderly population: comparisons with standard eyedrop bottle and with younger patients. Acta Ophthalmol 86: 856-859. [Crossref]
- Ikpoh, BI, Kunselman, A, Stetter C, Chen M (2020) Lost to follow-up: reasons and characteristics of patients undergoing corneal transplantation at Tenwek Hospital in Kenya, East Africa. Pan Afr Med J 36: 95. [Crossref]
- Njenga LN (2018) Determinants of Non-adherence to Long Term Therapy with Prescription Medicines in Adult Patients Attending Medical Outpatient Clinic at Mbagathi Hospital. Doctoral dissertation, University of Nairobi.
- Di Zazzo A, Kheirkhah A, Abud TB, Goyal S, Dana R (2017) Management of high-risk corneal transplantation. Surv Ophthalmol 62: 816-827. [Crossref]
- FOTHERINGHAM MJ and SAWYER MG (1995) Adherence to recommended medical regimens in childhood and adolescence. Journal of Paediatrics and Child Health 31: 72-78.
- Johnson MJ, Williams M, Marshall ES (1999) Adherent and nonadherent medication-taking in elderly hypertensive patients. Clin Nurs Res 8: 318-335. [Crossref]
- Uddin MF, Molyneux S, Muraya K, et al. (2021) Gender-related influences on adherence to advice and treatment-seeking guidance for infants and young children post-hospital discharge in Bangladesh. Int J Equity Health 20: 64. [Crossref]
- Hossain MM, Glass RI (1988) Parental son preference in seeking medical care for children less than five years of age in a rural community in Bangladesh. Am J Public Health. ;78(10):1349-1350. doi:10.2105/ajph.78.10.1349. [Crossref]
- Mak ST, Wong AC (2012) Vision-related quality of life in corneal graft recipients. Eye (Lond) 26: 1249-1255. [Crossref]
- Tabin GC, Gurung R, Paudyal G, Reddy HS, Hobbs CL, et al. (2004) Penetrating keratoplasty in Nepal. Cornea 23: 589-596. [Crossref]
- Midão L, Giardini A, Menditto E, Kardas P, Costa E (2017) Adherence to Medication in Older Adults as a Way to Improve Health Outcomes and Reduce Healthcare System Spending. Gerontology.
- Butts JB, Rich KL (2013) Philosophies and Theories for Advanced Nursing Practice. (3rd Edn) Sudbury: Jones & Bartlett Learning.
- Crawford AZ, Krishnan T, Ormonde SE, McGhee CN, Patel DV (2015) Treatment adherence after penetrating corneal transplant in a New Zealand population from 2000 to 2009. Cornea 34: 18-22. [Crossref]
- Haidara MA, Jeng BH (2016) Early complications after penetrating keratoplasty. US Ophthalmic Review 9: 88-91.
- Burra P, Germani G, Gnoato F, Lazzaro S, Russo FP, et al. (2011) Adherence in liver transplant recipients. Liver Transpl 17: 760-770. [Crossref]
- Korb-Savoldelli V, Sabatier B, Gillaizeau F, Guillemain R, Prognon P, et al. (2010) Non-adherence with drug treatment after heart or lung transplantation in adults: a systematic review. Patient Educ Couns 81: 148-154. [Crossref]
- Morisky DE, Ang A, Krousel-Wood M, Ward HJ (2008) Predictive validity of a medication adherence measure in an outpatient setting. J Clin Hypertens (Greenwich) 10: 348-354. [Crossref]
- Murphy N & Canales M. (2001) A critical analysis of compliance. Nursing Inquiry 8: 173-181.
- Giannaccare G, Fresina M, Pazzaglia A, Versura P (2016) Long-lasting corneal endothelial graft rejection successfully reversed after dexamethasone intravitreal implant. Int Med Case Rep J 9: 187-191. [Crossref]
- Yuan XB, Yuan YB, Jiang W, Liu J, Tian EJ, et al. (2008) Preparation of rapamycin-loaded chitosan/PLA nanoparticles for immunosuppression in corneal transplantation. Int J Pharm 349: 241-248. [Crossref]
- Davies I, Williams AM, Muir KW (2017) Aids for eye drop administration. Surv Ophthalmol 62: 332-345. [Crossref]
- Johnson O (2019) General System Theory and the Use of Process Mining to Improve Care Pathways. Stud Health Technol Inform 263: 11–22. [Crossref]
- Bertalanffy L (1928) Modern theories of development—an introduction to theoretical biology. Translated from German by J H Woodger 1933: Oxford: Clarendon Press.
- Hronek C, Bleich MR (2002) The less-than-perfect medication system": a systems approach to improvement. J Nurs Care Qual 16: 17-22. [Crossref]


