Abstract
Mucormycosis is a rare life-threatening opportunistic infection caused by mycetes of the order Mucoraceae. It appears mainly in immunocompromised patients (hematologic malignancies, anemia, AIDS) and in cases of advanced diabetes. A delayed diagnosis may imply a worse prognosis, so an early detection is mandatory for an adequate treatment. Herein we present a rare case of multi-organ mucormycosis with pulmonary, renal, pancreatic and spleen involvement detected and assessed by 18F-FDG PET/CT in a 24-years-old woman diagnosed of grey zone lymphoma (DLCBL/HL) who underwent an allogeneic stem cell transplantation. PET/CT with 18F-FDG was a key element in biopsy guide, final diagnosis and monitoring of response to therapy.
Keywords
mucormycosis, 18F-FDG PET/CT, allogeneic stem cell transplantation, lymphoma
Case Report
24-yr-old female, with history of diabetes and diagnosed of grey zone lymphoma (DLCBL/HL), underwent allogeneic stem cell transplantation (SCT) in October 2017. About the day +100 after SCT, she was admitted to our center with fever and complaints of pain in the left flank. Atypical consolidation area in right inferior lung lobe was seen in chest CT (Figure 1A), so the patient underwent to an 18F-FDG PET/CT to discard relapse of lymphoma. 18F-FDG PET/CT study showed peripheral 18F-FDG uptake in the pulmonary lesion (Figure 1B). In addition, an ametabolic area in the left kidney was seen on transverse fused PET/CT and MIP images (Figures 1C and 1D) which corresponded with the pain location referred by the patient and was informed as a probable renal infarction.
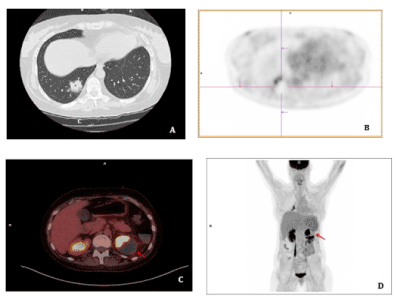
Figure 1. A: Atypical consolidation area in right inferior lung lobe was seen in chest CT. B: 18F-FDG PET/CT study showed peripheral 18F-FDG uptake in the pulmonary. C and D: An ametabolic area in the left kidney was seen on transverse fused PET/CT and MIP images
A month later, due to the progression of symptoms and an inconclusive lung function result, a new 18F-FDG PET-CT was performed and showed the above-described ametabolic kidney lesion increased in size, which now involved the whole left kidney (Figures 2A and 2B), as well as the pancreatic toe and spleen (Figure 3). A biopsy of perirenal hypermetabolic tissue, guided by PET/CT findings, was performed and histopathology showed abundant elongated structures in the form of thick, non-septate hyphae, with branches at right and obtuse angles, which with Grocott's silver stain showed thick contours (Figure 4). These findings lead to the final diagnosis of mucormycosis caused by Rhizopus oryzae. Due to involvement of such organs and the difficulty of its surgical debridement, the patient received medical treatment based on amphotericin B and Isavuconazole.
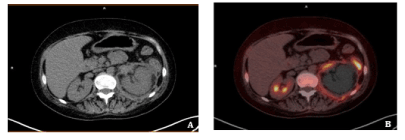
Figure 2. Second 18F-FDG PET-CT after SCT. The lesion previously informed as a probable renal infarction has increased and now affects the whole kidney, as seen in CT and PET/CT fusion images
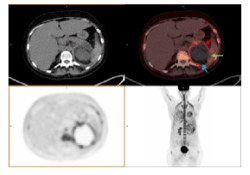
Figure 3. Second 18F-FDG PET-CT after SCT. An ametabolic lesion, with periferal uptake of 18F-FDG involves left kidney (blue arrow), spleen (Green arrow) and pancreatic toe (red arrow). These findings guided biopsy study, which lead to the final diagnosis of mucormycosis
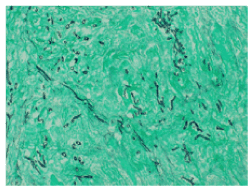
Figure 4. Histopathological images were studied using "Grocott stain", in which the microorganisms are seen as thick, elongated, cylindrical black structures and green background corresponds to necrotic perirenal fatty tissue
After 12 months of follow up, she remains stable in last 18F-FDG PET-CT study, with a mild clinical improvement (Figure 5).
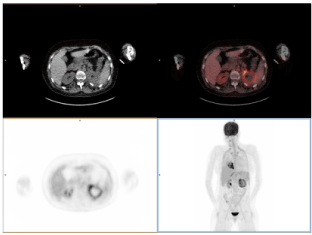
Figure 5. 18F-FDG PET-CT after 12 months of monitoring. After amphotericine B and isavuconazole therapy, the patient remains stable with mild clinical improvement
Discussion
Mucormycosis is an opportunistic infection caused by mycetes of the order Mucorales, that may have fatal consequences in absence of treatment [1]. It mainly affects patients with immunosupression (anemia, neutropenia, hematological malignancies, AIDS), Diabetes Mellitus and it has an incidence of 0.6% in patients who previously received allogenic STC [2]. Its diagnosis is usually difficult and late, mainly because of its clinical unspecific symptoms (fever, chest pain, congestion) and its relatively uncommon global incidence (10-50 less frequent than aspergillosis and candidiasis) and additionally it shows variable image patterns in CT and MRI studies [3]. Due to its ability to detect metabolically active tissue and differentiate it from necrosis, 18F-FDG PET/CT has emerged as a promising tool for the detection of fungal invasive disease. Although it has demonstrated its utility in a limited number of patients with lung, brain, hepatic and splenic candidiasis or mould infections [4,5], as well as cryptococcosis [6], there have been few publications concerning mucormycosis [1,7]. It usually presents as rhino-orbital-cerebral [1] or pulmonary [8] mucormycosis but is much less frequent in other locations as gastrointestinal, skin or other regions [9,10]. Its early diagnosis is mandatory, as a delay of treatment can significantly increase mortality [11]. Treatment usually consists of complete surgical debridement and antifungal therapy. Due to her renal, pancreatic and spleen involvement, surgical debridement was excluded, and she has received a combined therapy of Amphotericin B and Isavuconazole, a new triazole that has shown promising results even as a first line agent in anti-fungal therapy and profilaxis [12,13].
Conclusion
In conclusion, 18F-FDG PET-CT can differentiate between areas of metabolic active disease versus necrotic tissue and provides whole body images, so it can be very useful to confirm complete response to antifungal therapy. However, this case was particularly special because of the multi-organ involvement and the final diagnosis by perirenal fat biopsy, that was guided by 18F-FDG PET-CT. It allowed us to avoid necrotic tissue and therefore an inconclusive histological study, which would have meant a delay in initiation of treatment. We think it highlights the utility of this technique not only in diagnosis and therapy monitoring, but as a guide of biopsy studies [14].
Disclosure
The authors state no conflict of interests.
2021 Copyright OAT. All rights reserv
References
- Altini C, Asabella NA, Ferrari C, Rubini D, Dicuonzo F, et al. (2015) (18)F-FDG PET/CT contribution to diagnosis and treatment response of rhino-orbital-cerebral mucormycosis. Hell J Nucl Med 18: 68-70.
- Sakamoto H, Itonaga H, Sawayama Y, Taguchi J, Saijo T, et al. (2018) Primary oral mucormycosis due to rhizopus microsporus after allogeneic stem cell transplantation. Intern Med 57: 2567-2571.
- Herrera DA, Dublin AB, Ormsby EL, Aminpour S, Howell LP (2009) Imaging findings of rhinocerebral mucormycosis.Skull Base19: 117-125. [Crossref]
- Ho AY, Pagliuca A, Maisey MN, Mufti GJ (1998) Positron emission scanning with 18-FDG in the diagnosis of deep fungal infections.Br J Haematol101: 392-393. [Crossref]
- Chamilos G, Macapinlac HA, Kontoyiannis DP (2008) The use of 18F-fluorodeoxyglucose positron emission tomography for the diagnosis and management of invasive mould infections. Med Mycol J 46: 23-29.
- Igai H, Gotoh M, Yokomise H (2006) Computed tomography (CT) and positron emission tomography with [18F] fluoro-2-deoxy-D-glucose (FDG-PET) images of pulmonary cryptococcosis mimicking lung cancer. Eur J Cardiothorac Surg 30: 837-839.
- Hot A, Maunoury C, Poiree S, Lanternier F, Viard JP, et al. (2011) Diagnostic contribution of positron emission tomography with [18F]fluorodeoxyglucose for invasive fungal infections. Clin Microbiol Infect 17: 409-417.
- Marutsuka T, Masuda Y, Saishoji T (2013) Resected case of pulmonary Mucormycosis.Kyobu Geka66: 223-226. [Crossref]
- Prasad N, Manjunath R, Bhadauria D, Marak RSK, Sharma RK, et al. (2018) Mucormycosis of the thyroid gland: A cataclysmic event in renal allograft recipient.Indian J Nephrol28: 232-235. [Crossref]
- Asano-Mori Y (2017) Diagnosis and Treatment of Mucormycosis in Patients withHematological Malignancies [Translated Article].Med Mycol J58: E97-97E105. [Crossref]
- Vallverdú Vidal M, Iglesias Moles S, Palomera Fernandez M, Palomar Martinez M (2017) Isolated renal mucormycosis in a critically ill patient.Rev Iberoam Micol34: 57-58. [Crossref]
- Pilmis B, Alanio A, Lortholary O, Lanternier F (2018) Recent advances in the understanding and management of mucormycosis. F1000Res 7: 1429.
- Al-Obaidi M, Younes P, Ostrosky-Zeichner L (2018) Post-exposure prophylaxis with isavuconazole after occupational exposure to Rhizopus. Oxf Med Case Reports 2018: omy062.
- Liu Y, Wu H, Huang F, Fan Z, Xu B (2013) Utility of 18F-FDG PET/CT in diagnosis and management of mucormycosis.Clin Nucl Med38: e370-371. [Crossref]





