Abstract
This report describes a case of an infant of 5 months presenting with cephalohematoma since birth which was initially soft but later became hard and calcified after two months with the history of aspiration at one and half month of age. Surgical intervention using discard of the inner lamella and the cap radial craniectomy technique was used. The patient recovered uneventfully thereby. This report describes an infant presenting with a large calcified cephalohematoma leading to the surgical intervention using cap radial craniectomy. While the exact incidence is not known, large calcified cephalohematoma is rarely reported in the literature. We discuss here thoroughly the anatomy, classification, pathogenesis and different reconstructive surgeries of calcified cephalohematoma.
Key words
Cephalohematoma, calcification, reconstructive surgery, cap radial craniectomy
Introduction
Cephalohematoma is a collection of blood between the skull and the peri cranium confined within the borders of cranial sutures. These hematomas, also known as tumour crania sanguineous [1] are often caused by trauma associated with instrument assisted vaginal birth and are usually apparent within 24-72 hours after birth. The majority of cephalohematomas spontaneously resorb within one month of life [2].
Beyond this time, calcification of the hematoma occurs as bone is deposited under the lifted peri cranium [3]. While the exact incidence is not known, large calcified cephalohematoma is rarely reported in the literature [2,4,5]. This is reflected in the dearth of information on the surgical correction of this problem. Technique for cranioplasty was first described by Kaufman, et al. [6]. Subsequently, Chung, et al [7] reported three cases of surgically treated calcified cephalohematoma using technique similar to that described by Kaufman. To date, the indications for surgery and techniques for reconstruction have not been clearly elucidated.
Calcified cephalohematoma has inner and outer layers of bone. The inner layer consists of the foetal inner and outer table of intramembranous calvarial bone and the outer layer is made up of subpericranial bone formed after separation of the pericranium for the underlying calvarium. For the purpose of description and to avoid confusion, in this case report the former is referred to as the inner lamella and the latter as the outer lamella. We classified calcified cephalohematoma into two types; Types 1 and 2, with the distinguishing feature being the contour of the inner lamella in relation to the surrounding normal cranial vault. Type 1 calcified cephalohematoma has a nondepressed inner lamella with no encroachment into the cranial vault space while in Type 2, the inner
lamella is depressed into the cranial vault space [2,7].
This report describes an infant presenting with a large calcified cephalohematoma leading to the surgical intervention using cap radial craniectomy.
Case report
An infant of 5 months of age, presented with a hard-globular swelling over the right parietal region. The child was delivered via vaginal delivery using episiotomy with assisted vacuum suction at 40 weeks gestation. At birth, the cephalohematoma was noted. The swelling was initially soft but later became hard after 2 months. It was aspirated once by local doctor at one and half month of age. The child was otherwise healthy.
The CT scan demonstrated features consistent with type 2 calcified cephalohematoma of the skull (Figure 1 and 2). The cephalohematoma was excised with a high-speed drill, opened and its contents debrided and the inner lamella was discarded (Figure 3). Radial cuts were made on the outer lamella cap to collapse the elevated dome. These triangular fragments were trimmed as necessary to fit the defect. Irregular areas were burred away. The reconstructed calvarium was then secured back onto the skull (Figure 4). Care was taken to ensure complete coverage of the reconstructed calvarial bone graft with the pericranial flap. Meticulous haemostasis was ensured and the wounds were closed in layers. Drains were placed and the patient was given a firm compression head bandage for 24 hours after operation. Postoperative recovery was uneventful and she was discharged on the fifth postoperative day following a check skull roentgenogram (Figure 5).
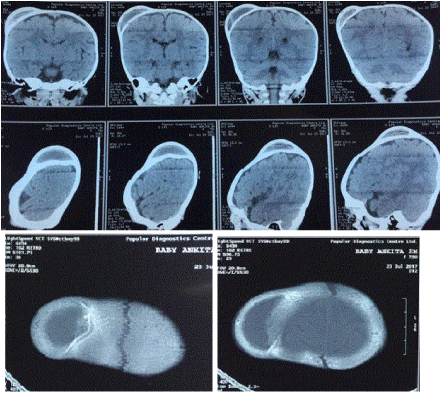
Figure 1. CT scan of brain (preoperative).
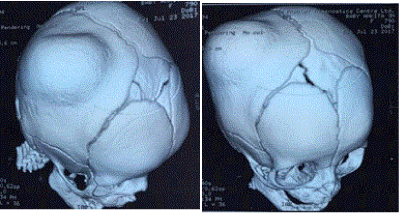
Figure 2. CT scan of head with 3D reconstruction (preoperative).
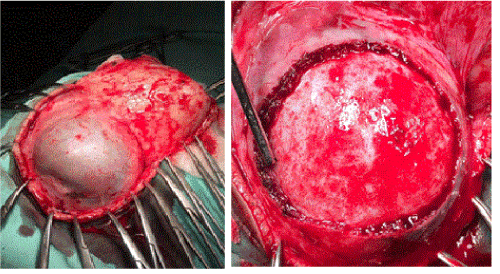
Figure 3. The calcified cephalohematoma is exposed and excised.
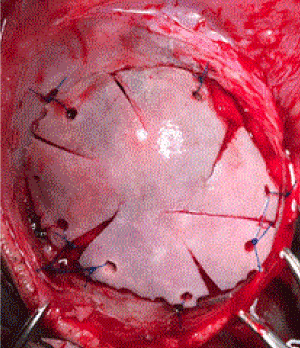
Figure 4. The reconstructed calvarium is secured back onto the skull (Cap Craniotomy).
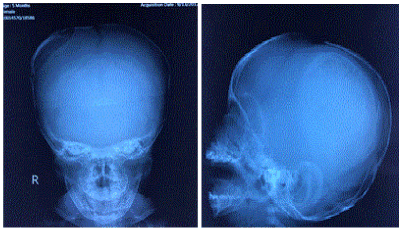
Figure 5. Postoperative skull roentgenogram.
Discussion
The authors recommended the cap radial craniectomy technique for irregularly shaped calcified cephalohematomas with a thinned-out inner lamella (type 2) as it allows total reshaping of the outer lamella to the desired contour.
In our case, the patient had a history of vaginal delivery with vacuum suction causing formation of the cephalohematoma which later became calcified with associated distortion of contour of the inner lamella. She was admitted to hospital at 5 months and a CT scan was done. Cap radial craniectomy technique was selected for the skull reconstruction.
As majority of cephalohematomas resorb within a month of birth, they should be expectantly observed during this period. Aspiration can be attempted for any significantly sized cephalohematoma when it failed to resolve after a month. Early authors such as Cushing have cautioned against aspiration for fear of infection and consequently osteomyelitis [2,3]. This fear is probably unfounded with proper technique and prophylactic antibiotics available today [1,8-12]. This should be done early (before 3-6 months of age) before a significant amount of bone has been laid down by the lifted pericranium. Firlik and Adelsen [13] reported a case of large chronic cephalohematoma that was observed for three months without any calcification and was successfully aspirated.
Calcification begins with the formation of a ridge around the edges of the hematoma and an eggshell-thin layer under the pericranium. At this stage, the cephalohematoma can be successfully treated by aspiration. Aspiration is performed with a large bore needle under aseptic conditions and prophylactic antibiotic coverage. The thin shell of calcification can be gently crushed and this would be incorporated back into the skull [2]. The ridge around the periphery of the hematoma may remain palpable but will resolve with time. A pressure bandage is applied after aspiration to prevent re-accumulation of the hematoma. In cases that present late (after 3-6 months), the cephalohematoma feels hard and on the CT scan, is completely encased by bone. Surgery is the only effective treatment for these calcified cephalohematoma.
2021 Copyright OAT. All rights reserv
The indications for surgery for calcified cephalohematoma have not been defined [6,7]. In the past, surgery for calcified cephalohematomas has been actively avoided for fear of complications associated with intracranial surgery [2-5]. While Tan [3] noted that as the skull grows, the swelling tends to become less conspicuous, many patients with this condition who were treated conservatively had a poor cosmetic outcome [2]. Today, an accepted indication is cosmesis, as this condition can cause significant skull asymmetry and is cosmetically unacceptable. Also, calcified cephalohematoma can potentially cause calvarial growth disturbances. Martinez-Lage, et al [14] reported a case of scaphocephaly secondary to a calcified cephalohematoma hindering the growth of the sagittal suture. While there are currently no reported cases of calcified cephalohematoma causing focal neurological deficits or disturbances in intracranial pressures, the long-term effects of a calcified mass encroaching into the cranial vault (in Type 2 calcified cephalohematoma) on brain development is unknown. Furthermore, while our experience with surgical correction of calcified cephalohematoma is limited, the safety and efficacy of intracranial surgery for correction of skull asymmetry in other conditions such as craniosynostosis in children have been well documented.
When considering surgical correction, the appropriate technique depends on the type of calcified cephalohematoma as described above [7]. In general, Type 1 lesions tend to be smaller calcified lesions with minimal elevation above the skull [7,11,15]. Larger cephalohematomas, as those cases reported here, tend to protrude higher above the skull and at the same time push the pliable inner lamella into the cranial vault and are thus Type 2 lesions. For Type 1 calcified cephalohematoma, the pericranium is opened and the outer lamella is separated from the inner lamella either with a drill bit or an osteotome.
The organized hematoma within its core is removed. The inner lamella is smoothed with a burr and bleeding is stopped with bone wax. It is not necessary to enter the cranial cavity [7,11,15]. For Type 2 calcified cephalohematoma however, a craniectomy and cranioplasty is necessary to elevate the inner lamella to restore normal skull contour and intracranial volume [7]. Two techniques are available to achieve this and these were described above. The selection of surgical technique for calvarial reconstruction between the flip-over bull’s-eye technique and the cap radial craniectomy technique depends on the preoperative evaluation of CT scans and intraoperative findings. CT scan serves as a useful guide (Figure 6). The ultimate decision should be made intraoperatively after confirming the thickness, robustness and contour of the inner and outer lamellas. If the thickness and convexity of the inner lamella is satisfactory, the flip-over bull’s-eye technique is an excellent reconstructive option where the elevated, deformed outer lamella is discarded and the depressed inner lamella is cut around its edges, reversed (flipped-over) and plated onto the non-affected area of the calvarium, giving an impression of a ‘‘bull’s-eye.’’. The cap radial craniectomy technique can be used with excellent result in cases that do not fulfill these criteria [15,16].
After surveying the literature, we emphasize and recommend the use of reconstructive surgery of skull in appropriately selected cases of large calcified cephalhaematoma as observed in our case.
References
- Chorobski J, Davis L (1934) Cyst formations of the skull. Surg Gynecol Obstet 58: 12.
- Morgan JE (1944) Calcification in cephalhematomata of the newborn infant. Am J Obstet Gynecol 48: 702.
- Tan KL (1970) Cephalohematoma. Aust N Z J Obstet Gynaecol 10: 101.
- Kastendieck H (1939) Zur frage der verknochering von cephalhamatoma. Zentralbl F Gynak 2507: 35Y52.
- Ottow Von B (1937) Vollige ossification eines kephalohamatoma beim saugling mit dadurch bedingter bleibender schadelformation. Zentralbl F Gynak 1478: 18Y35.
- Kaufman HH, Hochberg J, Anderson RP, Schochet SS Jr, Simmons GM Jr (1993) Treatment of calcified cephalohematoma. Neurosurgery 32: 1037-1039. [Crossref]
- Chung HY, Chung JY, Lee DG, Yang JD, Baik BS, et al. (2004) Surgical treatment of ossified cephalhematoma. J Craniofac Surg 15: 774-779. [Crossref]
- INGRAM MD Jr, HAMILTON WM (1950) Cephalohematoma in the newborn. Radiology 55: 502-507. [Crossref]
- Silverman FN, Byrd CR, Fitz CR (1993) The Skull: Traumatic Lesions. (9th Edn) St. Louis, Mo: Mosby.
- Hartley JB, Burnett CWF (1944) An enquiry into the causation and characteristics of cephalohematomata. Br J radiol 17: 33Y41.
- Bruce DA (2000) Cephalohematoma and subgaleal hematoma. In: Wilkins RH, Rengachary SS (Eds) Neurosurgery.
- Negishi H, Lee Y, Itoh K, Suzuki J, Nishino M, et al. (1989) Nonsurgical management of epidural hematoma in neonates. Pediatr Neurol 5: 253-256. [Crossref]
- Firlik KS1, Adelson PD (1999) Large chronic cephalohematoma without calcification. Pediatr Neurosurg 30: 39-42. [Crossref]
- Martinez-Lage JF, Esteban JA, Martinez Perez M, Poza M (1984) Craniostenosis secondary to calcified subperiosteal hematoma: case report. Neurosurgery 15: 703-704. [Crossref]
- Cummings TJ, George TM, Fuchs HE, McLendon RE (2004) The pathology of extracranial scalp and skull masses in young children. Clin Neuropathol 23: 34-43. [Crossref]
- Petersen JD, Becker DB, Fundakowski CE, Marsh JL, Kane AA (2004) A novel management for calcifying cephalohematoma. Plast Reconstr Surg 113: 1404-1409. [Crossref]





