Abstract
The objective of the present chapter is to present a time-line of the zygomatic implant technique. A literature review was performed to find relevant studies and to put them in chronological order to obtain a general perspective of the advances and evolution of the technique. The two major changes occurred from the development of the technique by professor P.I. Branemark in 1989 and its introduction to dental profession in 1998 were the surgical technique, itself, and the use of immediate loading protocols. In regard the surgical technique, a paradigm shift was developed changing the zigomatic implant insertion from an intrasinus to an extrasinus path, allowing an easier and less morbid procedure. The introduction of immediate loading entails a dramatic shortening of treatment time for the patiens in their seek of a functional prosthesis, getting the same or better results than the original two-step procedure.
Key words
zygomatic implants, zygomatic fixtures, history, time-line, surgical technique, immediate loading
Introduction
The edentulous patient still represents a challenge for the dental team. Masticatory and phonetic limitations are usually accompanied with aesthetics alterations that can, finally, affect the patient’s self-esteem. Also, the increase in life expectancy with the improvement of its quality (QoL) turns the treatment of this type of patients a priority with an increasing demand. Nevertheless, to increase patient acceptance to treatment, is mandatory to planned an affordable and predictable treatment protocol with low morbidity and a quickly recovery of function and aesthetics [1].
Dental implants are commonly used to replace missing teeth in various clinical situations. However, the possibility of placement of dental implants is limited by the presence of adequate bone volume, thus allowing their anchorage. In many clinical situations, particularly for edentulous patients with highly reabsorbed jaws and patients who have suffered traumatic bone loss or resective surgery for oral cancer, there is not enough bone to allow implant placement to support a fixed prosthesis.
It is known that the use of zygomatic bone as a support structure for implant fixation is indicated for cases of total or partial maxillary edentulism with extreme resorption. Zygomatic implants were documented as an alternative for atrophic posterior maxillary rehabilitation with the classic two-stage or immediate-loading protocol. The zygomatic implants avoid the procedures of grafting and elevation of the maxillary sinus and, therefore, contribute to a shorter, comfortable treatment and with lower morbidity.
Other indications for zygomatic implants include failure of conventional implants placement, failure of sinus augmentation or grafting procedures and rehabilitation after tumor resection and trauma. We illustrate this with two famous phrases about zygomatic implants taught by Professor Branemark: "How can we, in a simple, safe and highly predictable way, rehabilitate patients with highly reabsorbed jaws, where classical osseointegration techniques do not provide satisfactory results?". And: "Mother nature provided an area of dense and extensive bone, near the area of the jaw, which could provide good anchorage prognosis".
The purpose of this chapter was to put in a timeline the main events in the history of zygomatic implants to allow a better understanding of this important treatment alternative for total edentulous patients.
Methods
An electronic search was performed in the PubMed search engine, with articles until the year 2018 using the terms: zygomatic, zygomatic implants, intra-sinus technique, extra sinus and immediate loading, to identify follow-up studies, prospective and retrospective studies of placement of zygomatic implants. A total of 497 articles were found, of which 48 articles were selected for this review. We excluded articles with follow-up of less than five months, and articles that presented only a case report without proper follow-up. After inclusion of the articles, these were placed in chronological order for a better understanding of the evolution of zygomatic implants.
Eligibility criteria and study selection
Study characteristics
Selection criterio: Randomized, double-blind, placebo-controlled trials and others systematic reviews and meta-analysis in humans were selected and analyzed. Studies also needed to present the results of Number of zigomatic implants (ZI), Follow-up and ZI sucess rate.
Study selection and risk of bias in each study: Two independent reviewers performed research and study selection. The data extraction was performed by reviewer 1 and fully reviewed by reviewer 2. A third investigator decided some conflicting points and made the final decision to choose the articles. Only studies reported in Portuguese and English were evaluated. The Cochrane instrument was adopted to assess the quality of included studies [2].
Search strategy and information sources
In general, as an example, the search strategy in MEDLINE / Pubmed, Web of Science, ScienceDirect Journals (Elsevier), Scopus (Elsevier), OneFile (Gale) followed the following steps: - search for mesh terms (Zygomatic implants. Zygomatic fixtures. History. Time-line. Surgical technique. Immediate loading), - use of the booleans "and" between mesh terms and "or" among historical findings.
Statistical treatment of literary findings
The data found were written in an-Excel document and then transferred to statistical treatment in the Minitab 18 program. Descriptive analysis was performed with standard parameters of mean, standard deviation, maximum and minimum, amplitude and mode. Anderson-Darling normality test (α-level> 0.10 for a normal distribution) was also performed for continuous and categorical data, with consequent application of ANOVA variance analysis, accepting p-value greater than 0.05 for statistical significance (95.0 % CI). Linear regression analysis was also performed between the continuous predictors, with p> 0.05 with statistical difference (95.0% CI).
Risk of bias
Considering the Cochrane tool for risk of bias, the overall evaluation resulted in 19 studies with high risk of bias and 7 studies with uncertain risk. The domains that presented the highest risk of bias were related to ZI sucess rate (n = 20) and other sources of bias (n = 9). Also, absence of the source of financing of companies. Twenty-one studies mentioned the source of funding, and 15 did not disclose the conflict of interest statement.
Flow chart
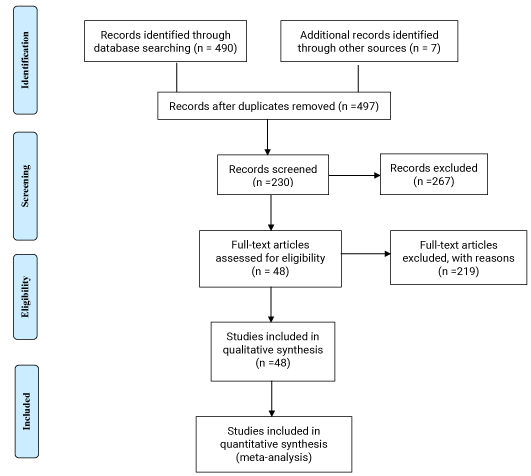
Figure 1.
Results
Zygomatic implants (ZI) were developed by Professor P. Branemark as an alternative to rehabilitate patients who underwent aggressive surgeries in the maxilla due to cancer or accidents. These people had very serious surgical sequelae, because as part of the palate were removed, they were unable to chew, swallow and even talk.
In 1998 Branemark published in the literature the possibility of using "zygomatic implants" to rehabilitate patients who did not have a bone structure [3]. Because the implants considered as conventional in the posterior region of the maxilla, could not be used for the minimum amount of bone due to the great pneumatization of the maxillary sinus and the great trauma caused by the use of total prosthesis. Then a new phase in implant dentistry was initiated, in which it would be possible to restore the total edentulous patients the possibility of chewing, smiling and living in society without the need for aggressive bone grafts, which would leave patients with sequelae and great morbidity.
The initial technique proposed by P.I. Branemark contemplated an initial vestibular incision, similar to a LeFort I incision, with periosteal detachment to the medial part of the zygomatic bone and zygomatic arch. After that, two windows (anthrotomy) were opened in the lateral wall of the maxillary sinus together with detachment of the Scheneider's membrane along the implant insertion path, regardless of the integrity of the membrane, for posterior placement of the intra-sinus zygomatic implants anchored in the medial portion of the zygomatic bone, which were totally internal to the maxillary sinus [4]. However, the major problem with the Branemark technique was the palatal exit of the implant that was in an unfavorable three-dimensional position on the palate, causing serious difficulties for phonetics, comfort, hygiene and adversely affected the configuration of the future prosthesis [4,5].
In view of these difficulties, Stella and Warner, in the year 2000 [5], altered the original technique, in which the implant remained totally inside the maxillary sinus, making slots in the external wall of the maxillary sinus, and thus improving in part the major problem that was the positioning of the implant head (prosthetic positioning), however 2/3 of the implant were still internally in the maxillary sinus and 1/3 being external to the maxillary sinus, closing the slot, and its insertion still in the medial wall of the zygomatic bone, improving the prosthetic position in relation to the technique presented by Branemark, leaving the implant less palatinate for future placement of the prosthesis.
In 2002, Bedrossian and co-workers [6] published a study in which a total of 44 zygomatic implants were placed by the original intra-sinus technique and 80 conventional implants were placed in 22 patients, followed up for 34 months, with a success rate of 100% for zygomatic implants and a success rate of 91.25% for premaxillary implants.
In 2003, two articles were published presenting new surgical protocols for placement of the zygomatic fixations. Beginning with Bothur and co-workers [7], in describing this modified technique, the authors proposed three possible positions for the placement of implants on one side, but in the authors' experience the placement of two zygomatic implants bilaterally is generally sufficient for reconstruction. Also in 2003, Boyes – Varley and collaborators [8] published an article with modification of the original protocol using implants that had an angulation in the head of 55 °, instead of the traditional 45 °, in this way, resulting in a reduced cantilever buccal in up to 20% in some patients. Both Bothur and collaborators and Boyes – Varley and collaborators used in their publications, surgical procedures in which the zygomatic implants were placed internally to the maxillary sinus.
Hirsch et al. [9] presented a publication in 2004, showing the results obtained after a one year of follow-up of 145 zygomatic implants in 16 different research centers. The total survival rate for zygomatic fixations was 97.9% after one year of follow-up. Eighty per cent of the patients were fully satisfied with the aesthetic and functional result at the time of insertion of the prosthesis after one-year follow-up. All data reported by the participating dentists rated that the aesthetic and functional outcomes of the treatment as acceptable.
Also in 2004, Malavez et al. [10] published their retrospective 48-month follow-up study of zygomatic implants using the intra-sinus technique. They reported no loss of implants in this period.
In 2005, Becktor et al. [11] carried out a follow-up study of 9 to 69 months of 31 zygomatic implants placed in 16 patients using the intra-sinus technique. The loss of three of these implants has been reported and sinusitis was the major problem in this follow-up.
In relation to the Sinus-Slot technique, published by Stella and Warner [5], Peñarrocha et al. [12] published an article in 2005 with the placement of 16 implants in an 18-month follow-up. No implant loss had been reported in this follow-up. Landes [13] reported the placement of 28 intra-sinus zygomatic implants in 12 patients, in which, were followed up for a period of four years. Reporting the loss of three of these implants.
Until the year 2005, all articles published in the literature described their cases using the original technique of Branemark [4] or by the use of the sinus slot technique proposed by Stella and Warner [5].
Working with the extrasinus technique since 2003, Migliorança et al. [14] in 2006, published for the first time in the literature, the use of the extra-sinus placement technique (Migliorança Technique). In this context, the externalized technique allowed a series of improvements related to the zygomatic fixations, among them: Better prosthetic positioning; less surgical invasiveness and better postoperative; shorter surgical time; absence of antrotomy and better surgical visualization. The proposal came to alter the technique previously suggested by Stella & Warner [5].
According to the authors, the possibility of placing the implant platform closer to the alveolar ridge without passing the implant through the maxillary sinus was possible. Soft tissue detachment and incision procedures remained the same as the original Branemark technique, however, the implant will be in the lateral (external) portion of the zygomatic bone next to the insertion of the masseter muscle where the largest bone volume is located, not needing to cross the bone, leaving space so, if necessary, it is possible to allocate a second zygomatic implant, changing the nomenclature of zygomatic fixation to zygomatic implant, because in the fixation the implant is anchored in the medial (internal) portion of the zygomatic bone. In the extrasinus technique the implants are in contact with the external wall of the maxillary sinus, the final positioning of the implant platform is completely close to the ridge crest, in the first molar region, resulting in greater support.
It has been described in the literature that the healing period after placement of dental implants is between three and six months [15]. In order to better serve the population in a more efficient and more comfortable way, it was developed the possibility of immediate loading of these implants without waiting for 3 to 6 months of the healing period previously recommended [16]. It is known today that since there is no macromotion and no micromovement greater than 100 μm, the concept of immediate loading of implants can allow osseointegration [17]. In addition, longer implants, better initial stability of the implant and the union of these implants with a prosthesis are considered important aspects to guarantee a predictable result [18].
The original zygomatic fixation protocol in two surgical stages also contemplated a waiting and healing period of six months [4]. Thus, some studies were developed to provide a better acceptance by the patient and to provide these patients a fixed provisional prosthesis with great stability, without requiring a second surgical stage [19-21].
Both published in 2006, Chow et al. [19], Bedrossian et al. [20] and Migliorança et al. [21] presented favorable results and conclusions regarding the immediate loading of zygomatic implants.
Still in 2006, Aparício and colleagues [22] published their five-year follow-up clinical study after placement of zygomatic implants using the original trans-sinus technique (intrasinus) and without immediate loading. A total of 131 zygomatic implants were placed, and there was no loss of these implants during follow-up, resulting in a high success rate.
In 2007, Kahnberg et al. [23] presented the results of a three-year follow-up of their preliminary multicenter study using the intra-sinus technique. In this follow-up the authors achieved a 96.3% success in zygomatic fixations.
Using the extrasinus technique, also in 2007, Migliorança et al. [24] published their four-year follow-up study between 2003 and 2007. One hundred and fifty-two zygomatic implants and 282 conventional implants were inserted using both immediate loading and late loading protocols after six months. During that time, two conventional implants failed, resulting in a cumulative success rate of 99.3%. Two zygomatic implants were removed, resulting in a cumulative success rate of 98.7%.
Davó and collaborators [25] published a retrospective study that included 18 patients treated between June 2004 and May 2006. The aim was to evaluate the survival rate of 36 zygomatic implants installed by the intrasinus technique and loaded immediately. No zygomatic implants were lost during the observation period and the survival rate was 100% over a 14-month observation period. All the provisional prostheses were stable and no relevant complications were observed.
Until then, few studies had been published in the literature that reported the level of patient satisfaction regarding the use of zygomatic fixation prostheses. For this purpose, Peñarrocha et al. [26] assessed 51 patients who underwent zygomatic implant placement surgery using the Stella Sinus-slot technique. The study presented a high level of satisfaction, being similar to patients who used prosthesis with conventional implants.
Duarte et al. [27] also investigated the use of immediate loading in zygomatic fixations published an article in 2007, in which 48 zygomatic implants were inserted by the intrasinus technique in 12 patients at a follow-up of 30 months. There was one zigomatic implant loss and all the prostheses were in good condition and with a high level of satisfaction on the part of the patients.
It is noteworthy that 2008 was the year of publication of the first articles by Aparício et al. [28] and Maló et al. [29] on the use of the extrasinus technique for zygomatic fixations. Also in the year 2008, Mozzati and colleagues [30] published in the literature their follow-up study of the insertion of zygomatic implants by the intra-sinus technique. Aparício et al. [31] have published in the literature their follow-up study of the insertion of zygomatic implants by the intrasinusal and extrasinusal technique. And Davó et al. [32] have published in the literature their intra-sinusal and Stella technique (Slot-Sinus) study. In all three publications the immediate loading of the provisional prostheses had been used. All of them presented favorable conclusions.
After demonstrating for the first time in the literature the use of the extra-sinus technique for the placement of zygomatic implants, Migliorança et al. [33] in 2009, published an article with the proposal of three-dimensional evaluation using the finite element method to dissipate tensions in peri-implant bone of zygomatic fixations installed internally and externally to the maxillary sinus, comparing quantitatively and qualitatively the tensions generated in both situations. This study concluded that the extrasinus technique presented a more homogeneous distribution of tensions in the peri-implant bone, both for zygomatic fixations and for conventional implants; the tensions peaks were 270% higher for the zygomatic fixtures in the original technique in relation to the exteriorized technique and the extrasinus technique provided greater area of bone/fixation contact.
Balshi et al. in 2009 [34], published an article from 9 months to 5 years of follow-up of 56 patients who received 110 zygomatic implants performed by the intra-sinus technique and with immediate loading. In this study, four zygomatic implants failed, with a success rate of 96.37%. The percentage of success related to prostheses was 100%.
Also in 2009, Davó et al. [35] presented a retrospective five-year follow-up study, in which 24 patients were rehabilitated with 45 zygomatic implants and 109 conventional implants using the two-stage intrasinus technique (without immediate loading). The prostheses success rate was 95.8%, with a survival rate of 97.4% for zygomatic implants and almost 90% for conventional implants in this study. Five patients presented sinusitis as a complication of the treatment.
In 2010, Stievenart and Malevez [36] published a cohort study of six to forty months of follow-up, in which ten patients underwent zygomatic implant placement using the intrasinus technique without immediate loading, and another 10 patients with immediate loading. Of these 10 patients, one patient underwent a computer guided surgery using a flapless technique. During the study, one patient lost three implants, with a success rate of 96.0%.
Chow et al. [37] presented a study in the year 2010 proposing a new surgical approach to eliminate the risk of maxillary sinusitis. The prospective study of this new approach was performed in 16 patients treated with 37 zygomatic implants and followed for a period of 6 to 24 months. There was no loss of any implant and no sinusitis had been reported.
In 2010, Bedrossian [38] published its seven-year follow-up study, in which 74 zygomatic fixations with immediate loading was performed (intra-sinus or extra-sinus). The study reported that two implants failed, and then replaced successfully. After that, all patients treated with the concept of immediate loading were restored with definitive prostheses, as planned.
Based on the zygomatic bone morphology and the subsequent location of the implant, Carlos Aparício published in the year 2011 a study presenting a new classification for zygomatic implants [39]. Aparicio named ZAGA his classification (zygoma anatomy guided approach), comprising five groups, ZAGA 0 to 4.
Also in 2011, Migliorança et al. [40] presented a retrospective study between 2003 and 2006 to report the clinical outcome of 150 extrasinus zygomatic implants combined with conventional implants for the implant-supported rehabilitation of the jaws with immediate and conventional loading. In this period it had been reported the loss of two zygomatic implants totaling 98.7% of success and all the prostheses were stable in function.
In 2012, Aparício et al. [41] published their 10-year follow-up clinical study, in which 41 zygomatic fixations were performed by the intrasinus technique and in two surgical stages (conventional loading). Two zygomatic implants were removed due to perimplant infection (95.12%) and all patients maintained functional prostheses.
Migliorança et al. [42] published in the literature in the year 2012 a prospective cohort study of eight years of follow-up. In which 40 extrasinus zygomatic implants and 74 conventional implants were evaluated together with the immediate loading of the provisional prosthesis. The success rate for extra-sinus zygomatic implants was 97.5% (one implant was removed) and 95.9% for conventional anterior implants (three implants failed during the study period), and the success rate of metal-reinforced prosthesis was 95.2%.
Also in 2012, Maló and colleagues [43] published their three-year retrospective cohort study, in which 92 zygomatic implants were placed by extra-sinus technique and 77 conventional implants, all of which were loaded immediately. No prosthesis or implant was lost, although one implant showed mobility within one year, but remained stable in subsequent follow-ups. Some complications occurred among them five cases of sinusitis in five patients who were diagnosed with sinusitis in the preoperative period and whose sinus membrane was ruptured during surgery.
In 2013, Aparício et al. [44] published an article comparing the classical intrasinus technique with extrasinus technique (ZAGA). Twenty-two consecutive patients were operated from 1998 to 2002 and 80 patients operated from 2004 to 2009 were selected. Aparício concluded that within the limits of this study, the results demonstrated that both procedures - the classic and ZAGA - presented similar positive clinical results in relation to implant survival.
It is important to report that in the year 2013, Davó and colleagues also published two prospective studies [45,46]. In their first study, Davó et al. [45] presented a prospective five-year study designed to analyze the results obtained from zygomatic implants using the intrasinus technique with immediate loading during a long follow-up period. A total of 81 zygomatic implants were inserted, 68 implants were reviewed in this period, and the loss of one implant occurred, with a success rate of 98.5%.
In the second study, Davó et al. [46] evaluated the clinical outcome of three years of prosthesis supported by four zygomatic implants by the intrasinus technique with immediate loading. In this study, no prosthesis or zygomatic implant failed, although an implant was not used to support the final prosthesis because it emerged in an unfavorable position. And there were some complications such as: penetration of the orbital cavity during the drilling procedure, without relevant consequences; infection followed by fistula in a zygomatic implant, resolved with antibiotic therapy and surgical drainage; and two patients developed sinusitis.
In 2014, Aparício et al. [47] published an article in the literature aiming to present an overview of the conventional technique of grafting, the current gold standard in the treatment of extremely reabsorbed jaws and to review the alternative treatment, the zygomatic implant. As well as, to establish specific criteria to evaluate and report the success of a rehabilitation anchored by zygomatic implants.
Also in 2014, Fernandez et al. [48] published a retrospective analysis of 244 zygomatic implants using the intrasinus technique, obtaining a high success rate.
Rodríguez-Chessa and colleagues [49] published a study in 2014, which aimed to retrospectively evaluate the zygomatic implants performed in 29 patients using the Stella Sinus-slot technique with immediate loading in 10 patients and conventional loading in 19 patients. Implant success rate was 79.1% and there was no statistical difference between immediate or conventional loading.
Yates and colleagues [50] published a retrospective observational cohort study in which 43 zygomatic implants placed by the Sinus-slot technique of Stella and Werner [5] were followed for a period of 5 to 10 years. In this study, the total success rate for zygomatic implants was 86.0%, with six of the implants failing to integrate or requiring removal due to persistent infection associated with the maxillary sinus.
Also in 2014, Maló and colleagues [51] published a study about extrasinus zygomatic implants placement technique. This article was a five years follow-up retrospective cohort study, with immediate loading. This study resulted in a 98.8% success rate in relation to zygomatic fixations.
Maló et al. [52] in the year 2015 published another extrasinus technique study with immediate loading of the prostheses. The objective of this study was to report the results of the rehabilitation of 352 patients with a complete edentulous atrophic maxilla using 747 zygomatic implants and 795 conventional implants at a follow-up from six months to seven years. The success rate for conventional implants was 97.9% and 94.4% for zygomatic implants.
Davó and Pons [53], also reported in the year 2015, the five-year follow-up of their previous study published in 2013 [46]. In this follow-up, Davo reported the loss of three implants, but still, achieving a high success rate.
Araújo and colleagues [54] published an article in 2016 that aimed to evaluate patients rehabilitated with zygomatic implants by the technique of Stella and Warner [5], considering the survival rate of conventional and zygomatic implants, and the health of the maxillary sinuses. The follow-up period varied from a minimum of 15 months to a maximum of 53 months after prosthetic rehabilitation, allowing a high survival rate of conventional and zygomatic implants (100.0%). The tomographic findings did not reveal characteristics of the sinus disease.
As we have seen previously, one of the topics related to the success of zygomatic fixations in the long term, besides the survival of the implant, is the presence or absence of sinus disease. D'Agostino et al. [55] published an important retrospective cohort study of patients submitted to zygomatic implants divided into two groups (Intrasinus technique and extrasinus technique) from January 2005 to May 2014. The results revealed a statistically significant increase in signs of sinus changes in patients who underwent zygomatic placement by intrasinus methods, but not in those who underwent extrasinus methods.
Agliardi et al. [56] published a prospective six-year follow-up study in 2017 in which extrasinus and intrasinus techniques were used with immediate loading of the provisional prostheses, and there was no loss of zygomatic implants, resulting in a rate of 100.0% success.
Neugarten et al. [57] also used both intra and extrasinus techniques with immediate loading in their retrospective 54-month follow-up study. One hundred five implants were placed, and there were four losses in only one patient, with a success rate of 96.0%.
Coppedê et al. [58] carried out a prospective clinical study of three years of follow-up, in which 94 zygomatic implants were performed by extrasinus technique and 179 conventional implants with immediate prosthetic loading. In this follow-up, one zygomatic implant (98.9%) and four conventional implants (97.7%) failed.
Still in 2017, Fortin [59] presented a 13 years follow-up clinical study, which aimed to evaluate the result of placement of zygomatic implants at an alternative fixation point (malar prominence). The author reported no loss of any zygomatic implants in this study.
Araújo et al. [60] published a retrospective study on patients who received zygomatic implants between 2007 and 2014. A total of 129 zygomatic implants were placed by the Stella and Warner [4] (sinus-slot) technique in two surgical times (without immediate loading). In this study, only two implants failed (98.4%) and maxillary sinusitis was the most common complication (21.6%).
De Rossi et al. [61] published an article that aimed to compare the electromyographic (EMG) activity of the masseter and temporal muscles in dentate patients and in individuals with implanted-supported total dentures anchored at the zygomatic bone. The authors concluded that the zygomatic implant promoted an active response of muscle fibers (hyperactivity) during mandibular posture and chewing conditions, probably due to the absence of periodontal receptors.
It was only in the year 2018 that the first two multicentre randomized controlled trials were published between the use of zygomatic implants with immediate loading compared with the use of conventional implants in patients who had augmented alveolar ridge [62,63]. Esposito and colleagues [62] evaluated 71 edentulous patients in a four-month follow-up. Eight patients lost 35 implants in the augmentation group, while one patient lost three implants of the zygomatic group, the difference being statistically significant. In total, 14 patients were affected by 20 complications in augmentation group while 26 zygomatic patients were affected by 35 complications, the difference being statistically significant. The authors concluded that even though, more complications were reported in zygomatic group, which were spontaneously resolved or could be easily treated, zygomatic implants proved to be a better modality of rehabilitation for severely atrophic jaws. And long-term data would be essential to confirm or challenge these preliminary results.
Davó and collaborators [63] published a one-year follow-up of this same study [62]. This time, eight patients lost 35 implants in the augmentation group while two patients lost four zygomatic implants, the difference being statistically significant. Overall, 14 patients were affected by 20 complications in the augmentation group while 26 zygomatic patients were affected by 35 complications (the same difference from the preliminary study of four months), and this difference was statistically significant. The authors concluded in this study that preliminary one-year post-loading data suggest that immediate loading zygomatic implants were associated with lower prosthetic failures, fewer implant failures, and less time required for functional load, compared to augmented alveolar ridge and conventionally loaded dental implants. And, zygomatic implants are a better rehabilitation modality for severely atrophic maxillaries and long-term data are essential to confirm or challenge these preliminary results.
Discussion
In this timeline, we can highlight some topics of great importance for the understanding of the history of zygomatic implants. The literature presents three different techniques for zygomatic fixations: The intrasinus technique, developed by P.I Branemark, a technique in which the implant body is totally inside the maxillary sinus [3]. The Sinus-slot technique, developed by Stella and Werner [5], in which a slot is created in the wall of the maxillary sinus, so that the implant body can be positioned lateral to the maxillary sinus. And the extrasinus technique developed by Migliorança [14], in which the implant body lies completely outside the maxillary sinus. Since, from a biomechanical point of view, the extrasinus technique presented a more homogeneous tension distribution in the perimplant bone [33].
Both Chrcanovic et al. [64] and Sharma and Rahul [65] presented conclusions favoring the use of zygomatic fixations, however, both suggest that multicenter, randomized controlled clinical trials and longer clinical trials should be implemented in this area before recommending the routine use of zygomatic implants for patients. And, Chrcanovic et al. [64] reported in their article that Migliorança and collaborators [14] were the first to publish in the literature the use of the extrasinusal technique.
Until 2006, all publications used the original technique described by Branemark or the use of the sinus-slot technique of Stella and Werner [4-6,9-13], and these techniques advocated the use of two surgical times, one for implant placement and other after six months, for placement of the abutments and the fabrication of the supported implant prosthesis. Miglorança et al. [21], Chow et al. [19] and Bedrossian et al. [20] were the first to publish the use of immediate loading for zygomatic implants, promoting better patient acceptance and simplifying the technique.
The increase in publications regarding the immediate loading of implant-supported dentures is also seen in the literature, and when possible the use of the immediate load seems to be the best choice [29-32,34,40,42,43,44,46,51-53,57,58,62,63]. And the reason for the good results reported, may be due to the concern with the primary stability in the act of the surgery.
Candel-Marti et al. [66] also concluded in a sistematic review that the most commonly used restoration was fixed prosthesis, with late loading after 3-6 months (89% -100% success) or immediate loading (96.37% -100% success rate) and the mean success rate was 97.05%.
It is worth mentioning that in a systematic review published in the year 2017, Tuminelli et al. [67] recommend the immediate loading and placement of zygomatic implants for the restoration of the severely atrophic maxilla with or without conventional anterior implants, and the complication rates are relatively few, rarely catastrophic, and easily managed.
We can analyze that the most frequent complication is maxillary sinusitis, and the onset of this complication is more related to the intrasinus technique and less to extrasinusal technique [37,55,68]. And the levels of satisfaction of the evaluated patients showed a high level of general satisfaction, with minimum hygiene problems and function [9,26].There are a number of published criteria to evaluate the success of zygomatic implants, but most authors considered mobility, pain or infection in the implants after prosthetic loading, absence of perimplant radiolucency and favorable positioning of the prosthesis as key factors to achieve the success. From these parameters the literature considers that the success percentage of zygomatic fixations is compatible with the success rate of conventional implants [68].
Chrcanovic et al. [68] updated their systematic review previously published in the year 2013 [64]. They concluded that zygomatic implants have a high clinical success rate of 12 years, with most failures occurring in the early postoperative stages and that the main complication observed was related to sinusitis, which may appear several years after the surgery.
The literature shows us a predominance of articles related to the intra-sinus technique (Table 1), but in recent years we can see a gradual increase in the number of publications related to extra-sinus fixations (Table 2), as well as articles comparing the two techniques mentioned above [47,55-57].
Table 1. Studies performed the intrasinusal technique
Article |
Number of ZI |
Follow-up |
ZI sucess rate |
Branemark et al. [4] |
52 |
5 to 10 years |
94% |
Bedrossian et al. [6] |
44 |
34 months |
100% |
Hirsch et al. [9] |
145 |
1 year |
97,9% |
Malevez et al. [10] |
103 |
6 to 48 months |
100% |
Becktor et al. [11] |
31 |
9 to 69 months |
90,3% |
Peñarrocha et al. [12] |
10 |
12 to 18 months |
100% |
Landes [13] |
28 |
14 to 53 months |
82% |
Aparicio et al. [22] |
131 |
6 to 60 months |
100% |
Kahnberg et al. [23] |
145 |
3 years |
96,3% |
Davó et al. [25] |
36 |
6 to 29 months |
100% |
Duarte et al. [27] |
48 |
30 months |
97,9% |
Mozzati et al. [30] |
14 |
24 months |
100% |
Aparicio et al. [31] |
47 |
2 to 5 years |
100% |
Davó et al. [32] |
81 |
12 months |
100% |
Balshi et al. [34] |
110 |
9 to 60 months |
96,37% |
Davó et al. [35] |
45 |
60 months |
97,4% |
Stiévenart et al. [36] |
80 |
6 to 40 months |
96% |
Bedrossian [37] |
74 |
7 years |
97,3% |
Aparicio et al. [41] |
41 |
10 years |
95,12% |
Davó et al. [45] |
81 |
60 months |
98,5% |
Davó et al. [46] |
68 |
36 months |
100% |
Fernández et al. [48] |
244 |
6 to 48 months |
99,6% |
Rodríguez-Chessa et al. [49] |
67 |
10 to 40 months |
79,1% |
Yates et al. [50] |
43 |
5 to 10 years |
86% |
Davó et al. [53] |
68 |
60 months |
100% |
Araújo et al. [54] |
27 |
15 to 5 months |
100% |
Araújo et al. [60] |
129 |
12 months |
98,44% |
Results statistical analysis
p-value/R2 |
**** |
***** |
p=0.03<0.05
R2=87.0% |
Table 2. Studies performed the extrasinus technique
Article |
Number of ZI |
Follow-up |
ZI success rate |
Migliorança et al. [24] |
152 |
48 months |
98,68% |
Aparício et al. [28] |
36 |
36 to 48 months |
100% |
Maló et al. [29] |
67 |
6 to 18 months |
98,5% |
Migliorança et al. [40] |
150 |
12 months |
98,7% |
Migliorança et al. [42] |
40 |
8 years |
97,5% |
Maló et al. [43] |
92 |
36 months |
100% |
Maló et al. [51] |
92 |
60 months |
98,8% |
Maló et al. [52] |
747 |
6 months to 7 years |
98,2% |
Coppedê et al. [58] |
94 |
36 months |
98,9% |
Results statistical analysis
p-value/R2 |
**** |
***** |
p=0.01<0.05
R2=89.0% |
Aboul-Hosn et al. [69] published a systematic review that aimed to review and compare the survival rates of oral rehabilitations performed with two zygomatic implants combined with regular implants versus rehabilitations with fourth zygomatic implants. The results did not show statistical differences in either treatment, in terms of survival and implant failure rates.
It was only in 2018 that were published multicentre randomized controlled trials between the use of zygomatic implants with immediate loading compared with the use of conventional implants in patients who performed alveolar ridge augmentation, until then, comparative studies unpublished in the literature [62,63].
Conclusion
We can observe that during the last years, many studies have been carried out using zygomatic fixations, resulting in a significant number of clinical cases with efficiency and prosthetic function superior to 95.0%. Proving that zygomatic implants are a reliable alternative treatment for total edentulous patients, with a high percentage of success compatible with conventional implants.
References
- Adell R, Eriksson B, Lekholm U, Brånemark P, Jemt T (1990) A long-term follow-up study of osseointegrated implants in the treatment of totally edentulous jaws. Int J Oral Maxillofac Implants 5: 347-359. [Crossref]
- Higgins J, Green S (2011) Cochrane handbook for systematic reviews of interventions. Version 5.1.0 [updated March 2011]. The Cochrane Collaboration.
- Branemark PI (1998) The zygomatic fixture: Clinical procedures (ed 1). Gothenburg, Sweden, Nobel Biocare AB, pp: 1.
- Brånemark PI, Gröndahl K, Ohrnell LO, Nilsson P, Petruson B, et al. (2004) Zygoma fixture in the management of advanced atrophy of the maxilla: technique and long-term results. Scand J Plast Reconstr Surg Hand Surg 38: 70-85. [Crossref]
- Stella JP, Warner MR (2000) Sinus slot technique for simplification and improved orientation of zygomaticus dental implants: A technical note. Int J Oral Maxillofac Implants 15: 889-893.
- Bedrossian E, Stumpel L, Beckely ML, Indresano T (2002) The zygomatic implant: preliminary data on treatment of severely resorbed maxillae. A clinical report. Int J Oral Maxillofac Implants 17: 861-865.
- Bothur S, Jonsson G, Sandahl L (2003) Modified technique using multiple zygomatic implants in reconstruction of the atrophic maxilla: A technical note. Int J Oral Maxillofac Implants 18: 902-904.
- Boyes-Varley JG, Howes DG, Lownie JF, Blackbeard GA (2003) Surgical modifications to the Brånemark zygomaticus protocol in the treatment of the severely resorbed maxilla: A clinical report. Int J Oral Maxillofac Implants 18: 232-237. [Crossref]
- Hirsch JM, Ohrnell LO, Henry PJ, Andreasson L, Brånemark PI, et al. (2004) A clinical evaluation of the Zygoma fixture: One year of follow-up at 16 clinics. J Oral Maxillofac Surg 62: 22-29. [Crossref]
- Malevez C, Abarca M, Durdu F, Daelemans P (2004) Clinical outcome of 103 consecutive zygomatic implants: a 6-48 months follow-up study. Clin Oral Implants Res 15: 18-22. [Crossref]
- Becktor JP, Isaksson S, Abrahamsson P, Sennerby L (2005) Evaluation of 31 zygomatic implants and 74 regular dental implants used in 16 patients for prosthetic reconstruction of the atrophic maxilla with cross-arch fixed bridges. Clin Implant Dent Relat Res 7: 159-165. [Crossref]
- Peñarrocha M, Uribe R, García B, Martí E (2005) Zygomatic implants using the sinus slot technique: Clinical report of a patient series. Int J Oral Maxillofac Implants 20: 788-792. [Crossref]
- Landes CA (2005) Zygoma implant-supported midfacial prosthetic rehabilitation: A 4-year follow-up study including assessment of quality of life. Clin Oral Implants Res 16: 313-325.
- Migliorança R, Ilg JP, Serrano AS, Souza RP, Zamperlini MS. (2006) Sinus exteriorization of the zygoma fixtures: a new surgical protocol. Implant News 3: 30-35.
- Brånemark PI (1983) Osseointegration and its experimental background. J Prosthet Dent 50: 399-410. [Crossref]
- Tarnow DP, Emtiaz S, Classi A (1997) Immediate loading of threaded implants at stage 1 surgery in edentulous arches: ten consecutive case reports with 1- to 5-year data. Int J Oral Maxillofac Implants 12: 319-324.
- Brunski JB (1993) Avoid pitfalls of overloading and micromotion of intraosseous implants. Dent Implantol Update 4: 77-81. [Crossref]
- De Bruyn H, Raes S, Ostman PO, Cosyn J (2000) Immediate loading in partially and completely edentulous jaws: a review of the literature with clinical guidelines. Periodontol 66: 153-187.
- Chow J, Hui E, Lee PK, Li W (2006) Zygomatic implants--protocol for immediate occlusal loading: A preliminary report. J Oral Maxillofac Surg 64: 804-811.
- Bedrossian E, Rangert B, Stumpel L, Indresano T (2006) Immediate function with the zygomatic implant: a graftless solution for the patient with mild to advanced atrophy of the maxilla. Int J Oral Maxillofac Implants 21: 937-942.
- Migliorança RM, Ilg JP, Mayo TM, Serrano AS, Funis LP, et al. (2006) Função imediata em fixações zigomáticas: relato de dois casos com 18 e 30 meses de acompanhamento clínico. Implant News 3: 243-247.
- Aparicio C, Ouazzani W, Garcia R, Arevalo X, Muela R, et al. (2006) A prospective clinical study on titanium implants in the zygomatic arch for prosthetic rehabilitation of the atrophic edentulous maxilla with a follow-up of 6 months to 5 years. Clin Implant Dent Relat Res 8: 114-122.
- Kahnberg KE, Henry PJ, Hirsch JM, Ohrnell LO, Andreasson L, et al. (2007) Clinical evaluation of the zygoma implant: 3-year follow-up at 16 clinics. J Oral Maxillofac Surg 65: 2033-2038.
- Migliorança R, Coppedê A, Zamperlini M, Mayo T, Viterbo R, et al. (2007) Reabilitação da maxila atrófica sem enxertos ósseos: resultados de um novo protocolo utilizado em casos de edentulismo total. Rev Implant News 4: 557-564.
- Davo R, Malevez C, Rojas J (2007) Immediate function in the atrophic maxilla using zygoma implants: a preliminary study. J Prosthet Dent 97: S44-S51. [Crossref]
- Peñarrocha M, Carrillo C, Boronat A, Martí E (2007) Level of satisfaction in patients with maxillary full-arch fixed prostheses: zygomatic versus conventional implants. Int J Oral Maxillofac Implants 22: 769-773. [Crossref]
- Duarte LR, Filho HN, Francischone CE, Peredo LG, Brånemark PI (2007) The establishment of a protocol for the total rehabilitation of atrophic maxillae employing four zygomatic fixtures in an immediate loading system--a 30-month clinical and radiographic follow-up. Clin Implant Dent Relat Res 9: 186-196. [Crossref]
- Aparício C, Ouazzani W, Aparicio A, Fortes V, Muela R, et al. (2010) Extrasinus zygomatic implants: three-year experience from a new surgical approach for patients with pronounced buccal concavities in the edentulous maxilla. Clin Implant Dent Relat Res 12: 55-61.
- Maló P, Nobre Mde A, Lopes I (2008) A new approach to rehabilitate the severely atrophic maxilla using extramaxillary anchored implants in immediate function: A pilot study. J Prosthet Dent 100: 354-366. [Crossref]
- Mozzati M, Monfrin SB, Pedretti G, Schierano G, Bassi F (2008) Immediate loading of maxillary fixed prostheses retained by zygomatic and conventional implants: 24-month preliminary data for a series of clinical case reports. Int J Oral Maxillofac Implants 23: 308-314. [Crossref]
- Aparicio C, Ouazzani W, Aparicio A, Fortes V, Muela R, et al. (2010) Immediate/Early loading of zygomatic implants: clinical experiences after 2 to 5 years of follow-up. Clin Implant Dent Relat Res 12: e77-e82.
- Davo R, Malevez C, Rojas J, RodrÃguez J, Regolf J. (2008) Clinical outcome of 42 patients treated with 81 immediately loaded zygomatic implants: a 12- to 42-month retrospective study. Eur J Oral Implantol 9: 141-150.
- Migliorança RM, Vasco MAA, Coppedê AR, Mayo TM, Viterbo RBS (2009) Comparative study on the stress dissipation of zygomatic fixtures installed internal or external to the maxillary sinus: a 3D finite element method analysis. Implant News 6: 395-402.
- Balshi SF, Wolfinger GJ, Balshi TJ (2009) A retrospective analysis of 110 zygomatic implants in a single-stage immediate loading protocol. Int J Oral Maxillofac Implants 24: 335-341.
- Davó R (2009) Zygomatic implants placed with a two-stage procedure: a 5-year retrospective study. Eur J Oral Implantol 2: 115-124. [Crossref]
- Stiévenart M, Malevez C (2010) Rehabilitation of totally atrophied maxilla by means of four zygomatic implants and fixed prosthesis: a 6-40-month follow-up. Int J Oral Maxillofac Surg 39: 358-363.
- Chow J, Wat P, Hui E, Lee P, Li W (2010) A new method to eliminate the risk of maxillary sinusitis with zygomatic implants. Int J Oral Maxillofac Implants 25: 1233-1240. [Crossref]
- Bedrossian E (2010) Rehabilitation of the edentulous maxilla with the zygoma concept: a 7-year prospective study. Int J Oral Maxillofac Implants 25: 1213-1221. [Crossref]
- Aparicio C (2011) A proposed classification for zygomatic implant patient based on the zygoma anatomy guided approach (ZAGA): A cross-sectional survey. Eur J Oral Implantol 4: 269-275.
- Migliorança RM, Coppedê A, Dias Rezende RC, de Mayo T (2011) Restoration of the edentulous maxilla using extrasinus zygomatic implants combined with anterior conventional implants: A retrospective study. Int J Oral Maxillofac Implants 26: 665-672.
- Aparicio C, Manresa C, Francisco K, Ouazzani W, Claros P, et al. (2014) The long-term use of zygomatic implants: a 10-year clinical and radiographic report. Clin Implant Dent Relat Res 16: 447-459. [Crossref]
- Migliorança RM, Sotto-Maior BS, Senna PM, Francischone CE, Del Bel Cury AA (2012) Immediate occlusal loading of extrasinus zygomatic implants: a prospective cohort study with a follow-up period of 8 years. Int J Oral Maxillofac Surg 41: 1072-1076.
- Maló P, Nobre Md, Lopes A, Francischone C, Rigolizzo M (2012) Three-year outcome of a retrospective cohort study on the rehabilitation of completely edentulous atrophic maxillae with immediately loaded extra-maxillary zygomatic implants. Eur J Oral Implantol 5: 37-46.
- Aparicio C, Manresa C, Francisco K, Claros P, Alández J, et al. (2014) Zygomatic implants: indications, techniques and outcomes, and the zygomatic success code. Periodontol 2000 66: 41-58.
- Davó R, Malevez C, Pons O (2013) Immediately loaded zygomatic implants: a 5-year prospective study. Eur J Oral Implantol 6: 39-47.
- Davó R, Pons O (2013) Prostheses supported by four immediately loaded zygomatic implants: a 3-year prospective study. Eur J Oral Implantol 6: 263-269.
- Aparicio C, Manresa C, Francisco K, Aparicio A, Nunes J, et al. (2014) Zygomatic implants placed using the zygomatic anatomy-guided approach versus the classical technique: A proposed system to report rhinosinusitis diagnosis. Clin Implant Dent Relat Res 16: 627-642.
- Fernández H, Gómez-Delgado A, Trujillo-Saldarriaga S, Varón-Cardona D, Castro-Núñez J (2014) Zygomatic implants for the management of the severely atrophied maxilla: A retrospective analysis of 244 implants. J Oral Maxillofac Surg 72: 887-891.
- Rodríguez-Chessa JG, Olate S, Netto HD, Shibli J, de Moraes M, et al. (2014) Treatment of atrophic maxilla with zygomatic implants in 29 consecutives patients. Int J Clin Exp Med 7: 426-430.
- Yates JM, Brook IM, Patel RR, Wragg PF, Atkins SA, et al. (2014) Treatment of the edentulous atrophic maxilla using zygomatic implants: evaluation of survival rates over 5-10 years. Int J Oral Maxillofac Surg 43: 237-242.
- Maló P, Nobre M de A, Lopes A, Ferro A, Moss S (2014) Five-year outcome of a retrospective cohort study on the rehabilitation of completely edentulous atrophic maxillae with immediately loaded zygomatic implants placed extra-maxillary. Eur J Oral Implantol 7: 267-281.
- Maló P, de Araújo Nobre M, Lopes A, Ferro A, Moss S (2015) Extramaxillary surgical technique: clinical outcome of 352 patients rehabilitated with 747 zygomatic implants with a follow-up between 6 months and 7 years. Clin Implant Dent Relat Res 17: e153-e162.
- Davó R, Pons O (2015) 5-year outcome of cross-arch prostheses supported by four immediately loaded zygomatic implants: A prospective case series. Eur J Oral Implantol 8: 169-174.
- Araújo PP, Sousa SA, Diniz VB, Gomes PP, da Silva JS, et al. (2016) Evaluation of patients undergoing placement of zygomatic implants using sinus slot technique. Int J Implant Dent 2: 2.
- D'Agostino A, Trevisiol L, Favero V, Pessina M, Procacci P, et al. (2016) Are Zygomatic Implants Associated with Maxillary Sinusitis? J Oral Maxillofac Surg 74: 1562-1573. [Crossref]
- Agliardi EL, Romeo D, Panigatti S, de Araújo Nobre M, Maló P. (2017) Immediate full-arch rehabilitation of the severely atrophic maxilla supported by zygomatic implants: A prospective clinical study with minimum follow-up of 6 years. Int J Oral Maxillofac Surg 46: 1592-1599.
- Neugarten J, Tuminelli FJ, Walter L (2017) Two bilateral zygomatic implants placed and immediately loaded: a retrospective chart review with up-to-54-month follow-up. Int J Oral Maxillofac Implants 32: 1399-1403.
- Coppedê A, de Mayo T, de Sá Zamperlini M, Amorin R, de Pádua APAT, et al. (2017) Three-year clinical prospective follow-up of extrasinus zygomatic implants for the rehabilitation of the atrophic maxilla. Clin Implant Dent Relat Res 19: 926-934.
- Fortin Y (2017) Placement of zygomatic implants into the malar prominence of the maxillary bone for apical fixation: A clinical report of 5 to 13 years. Int J Oral Maxillofac Implants 32: 633-641.
- Araújo RT, Sverzut AT, Trivellato AE, Sverzut CE (2017) Retrospective analysis of 129 consecutive zygomatic implants used to rehabilitate severely resorbed maxillae in a two-stage protocol. Int J Oral Maxillofac Implants 32: 377-384.
- De Rossi M, Palinkas M, de Lima-Lucas B, Santos CM, Semprini M, et al. (2017) Masticatory muscle activity evaluation by electromyography in subjects with zygomatic implants. Med Oral Patol Oral Cir Bucal 22: e392-e397.
- Esposito M, Davó R, Marti-Pages C, Ferrer-Fuertes A, Barausse C, et al. (2018) Immediately loaded zygomatic implants vs conventional dental implants in augmented atrophic maxillae: 4 months post-loading results from a multicentre randomised controlled trial. Eur J Oral Implantol 11: 11-28.
- Davó R, Felice P, Pistilli R, Barausse C, Marti-Pages C, et al. (2018) Immediately loaded zygomatic implants vs conventional dental implants in augmented atrophic maxillae: 1-year post-loading results from a multicenter randomised controlled trial. Eur J Oral Implantol 11: 145-161.
- Chrcanovic BR, Abreu MH (2013) Survival and complications of zygomatic implants: a systematic review. Oral Maxillofac Surg 17: 81-93. [Crossref]
- Sharma A, Rahul GR (2013) Zygomatic implants/fixture: a systematic review. J Oral Implantol 39: 215-224. [Crossref]
- Candel-Martí E, Carrillo-García C, Peñarrocha-Oltra D, Peñarrocha-Diago M (2012) Rehabilitation of atrophic posterior maxilla with zygomatic implants: review. J Oral Implantol 38: 653-657.
- Tuminelli FJ, Walter LR, Neugarten J, Bedrossian E (2017) Immediate loading of zygomatic implants: A systematic review of implant survival, prosthesis survival and potential complications. Eur J Oral Implantol 10: 79-87.
- Chrcanovic BR, Albrektsson T, Wennerberg A (2016) Survival and complications of zygomatic implants: An updated systematic review. J Oral Maxillofac Surg 74: 1949-1964.
- Aboul-Hosn Centenero S, Lázaro A, Giralt-Hernando M, Hernández-Alfaro F (2018) Zygoma quad compared with 2 zygomatic implants: A systematic review and meta-analysis. Implant Dent 27: 246-253.

