Objective: To evaluate the restorations microleakage in three materials with and without 2% chlorhexidine (CHX) pre-treatment and in two storage times.
Materials and methods: 120 class V cavities were prepared in healthy bovine incisors, divided according to restorative material: CCR (conventional composite resin); CBFR (composite bulk fill resin) and GIC (resin-reinforced glass ionomer cement) and subdivided according to storage time (7 and 60 days) and pretreatment (with or without CHX), with 10 wells for each subgroup. After the restorative procedure of each subgroup, the teeth were sealed and immersed in 0.5% basic fuchsin buffer for 24 hours. The teeth were sectioned and analyzed for the degree of microleakage.
Results: Data were submitted to Kruskall-Wallis analysis, which showed no statistically significant differences between the variables evaluated.
Conclusion: Based on the results found, the pre-treatment with chlorhexidine did not interfere in the marginal microleakage scores for the different storage times and in the different types of materials used.
chlorhexidine, microleakage, non-carious cervical lesions
Since the composite resins introduction in the market, improvements have been made in its composition and mechanical properties that have allowed great using versatility, and it can be indicated as restorative materials, for sealing of fossils and fissures, as cementing agents, temporary restorations, among others [1-10]. The basic composite resins composition are the organic matrix with different monomers, being the most used BisGMA, silane binding agents and photoinitiators (most present camphorquinone) and inorganic matrix composed of charge particles (vitreous or colloidal silica) [11].
Because BisGMA exhibits high viscosity and low polymerization conversion [16], the presence of thinner monomers such as TEGDMA and EGDMA is necessary to reduce the viscosity of the material, increase the stiffness and degree of monomers conversion [9].
During the polymer formation, the monomeric movement occurs towards the center of the material by means of the reduction of the weak forces of Van der Waals, converting these monomers into covalent bonds denominated polymers [17], which causes decrease of the volume of the material, known like polymerization contraction. This phenomenon is dependent on the amount of material, that is, the more monomers the greater the movement, consequently the more intense the polymerization contraction.
This volumetric alteration can damage the restorations marginal sealing, causing the formation of slits in the adhesive interface, postoperative sensitivity, marginal pigmentation of the restoration or recurrent caries [19]. Therefore, for conventional composite resins, the use of the incremental technique with a maximum of 2 mm is indicated [15].
In order to overcome the problems of the polymerization contraction, bulk fill composites were introduced. In general, these materials have a composition similar to that of conventional resins, differing in the size of the silanized barium particles, with a larger size and the photoactivation system differentiated by the presence of APS (Advanced Polymerization System) [3]. The presence of the silanized barium glass allows the particles of the Bulk Fill resin to become more translucent, and thus, together with the photoinitiators, there is a greater penetration and reflection of the light, allowing its use in increments greater than 2 mm [8].
The viscosity of the Bulk Fill Flow resins associated with the possibility of larger increments makes them an alternative for Class V lesions, whose cavity preparation shows a high contraction factor (Factor C) and the location of the cervical wall is in dentin in the largest part of the cases [5].
Another alternative for this type of cavity are glass ionomer cements (GIC) as a base material in aesthetic restorations. This material was one of the first that appeared to fill large cavities, replacing the lost dentin, having as advantage in its use the linear thermal expansion similar to this structure, remineralization capacity of the dental remnant, adhesion to dental structure, fluoride release and biocompatibility, being indicated for class V lesions [18].
Whatever the material of choice, at the time of restoration it is important that adequate cavity cleaning be performed to avoid recurrent caries. Among the cavity cleaning solutions, chlorhexidine (CHX) is the most used because it has strong basicity and two-capillary charge, because it contains two rings of 4-chlorophenyl and two groups of bisguanide, connected by a central chain of hexamethylene. When in contact with dentin, CHX inhibits the action of metalloproteinases (MMPs), enzymes responsible for hybrid bed degradation. Thus, its use as a cleaning solution may increase the clinical longevity of aesthetic restorations23. In this way, the objective of this research is to observe the importance of CHX as a cleaning agent in the pretreatment of restorations by the marginal microleakage test in class V restorations in three types of restorative materials (conventional composite resin, bulk fill flow composite resin and cement of resin-modified glass ionomer) with influence of CHX pretreatment and aging in acid solution.
Sample calculation
After the pilot study, a completely randomized design was used, with the aid of the Bioestat 5.3 program, 10 cavities were defined per subgroup, with analysis power equal to 90% and standard error of 0.01, and the distribution of the groups was in the in Figure I on page 19.
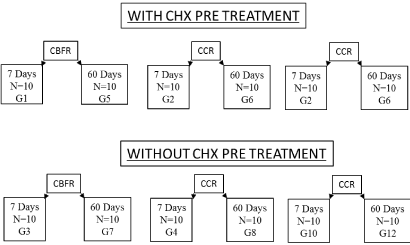
Figure 1.Sample groups distribution n = 10
Samples preparation
Sixty healthy, clean bovine incisors with no periodontal tissue adhered were collected. Later, the crowns were separated from the roots by means of a section with a double - sided diamond disk (KG Sorensen, Cotia, São Paulo - Brazil), and stored in saline solution until preparation.
Restorative procedures
In all groups, the cavities were made in a region of the cement-enamel boundary with the aid of a diamond tip 1014 (KG Sorensen, Cotia, São Paulo - Brazil), 4 mm long and 2 mm deep, in the vestibular region and in the lingual of the teeth. The phosphoric acid conditioning (Condac 37% / FGM, Joinville, Santa Catarina - Brazil) was done in enamel for 30 seconds and in dentin for 15 seconds. The cavities were dried with absorbent filter paper and with the aid of the microbrush, two layers were applied with 20 second friction of the adhesive system (Ambar Universal / FGM, Joinville, Santa Catarina - Brazil) and photoactivation with a light led apparatus (Poly Wireless, Factory KaVo do Brasil Ind. Com. Ltda., Joinville, Santa Catarina - Brazil) with power density of 1100 mW / cm², for 20 seconds.
The wells that were restored with bulk fill flow (Opus ™ Bulk Fill Flow / FGM, Joinville, Santa Catarina - Brazil) and glass ionomer cement (Vitremer ™ / 3M ESPE, St. Paul, MN, USA) were filled with single increment. The wells that were restored with the conventional composite resin (Opallis ™ / FGM, Joinville, Santa Catarina - Brazil) were filled with two increments, and photoactivation for 40 seconds for all groups. The compositions of the materials used are listed in Table 1, Figure II, on page 20.
Table 1. Composition of the materials used in this study
Material |
Manufacturer |
Composition |
Color |
Opus™ Bulk Fill Flow |
FGM |
Siliconized barium glass, UDMA, TEGDMA, Bis-GMA, silanized silica, ethyl 4-dimethylaminobenzoate (DABE), trifluoride, ytterbium, camphorquinone, tinuvin P, butyl hydroxytoluene, luminux blue, red iron oxide and white titanium dioxide |
A3 |
Opallis™
|
FGM |
Bis-GMA, BisEMA, TEGDMA, diurethane dimethacrylate, silanized ceramics, silanized silicon dioxide, camphorquinone and ethyl 4-dimethylaminobenzene |
A3 |
Vitremer™
|
3M ESPE |
Powder: glass treated with silane and potassium persulfate; Liquid: water and 2-hydroxyethyl methacrylate (HEMA); Glazer: triethylene glycol dimethacrylate (TEGDMA) and Primer: ethyl alcohol and 2-hydroxyethyl methacrylate |
|
Condac™ 37% |
FGM |
37% ortho-phosphoric acid |
|
Ambar™ Universal |
FGM |
Methacrylic silicon monomers, photoinitiators, co-initiators and stabilizers; Inactive ingredients: inert filler, silica nanoparticles; Vehicle: ethanol |
|
Chlorhexidine digluconate 2% |
Rioquímica |
Gluconato a 2%, água, glicerina, etanol, polisorbato20, sacarinato de sódio, FD&C blue n°1 |
|
Basic Fucsin 0.5% |
|
Handled at the Chamomilla pharmacy (Cascavel / PR) |
|
For groups pre-treated with CHX, the phosphoric acid conditioning was performed for 20 seconds, followed by washing.
Storage
The teeth were divided into two groups: half of the samples were stored for 7 days in saline and another in ethanol and water (3: 1) for 60 days.
Microleakage test
To perform the microleakage test, the apical portion of the dental crowns were sealed with sticky wax. The teeth were waterproofed with two layers of Royal blue nail polish (Colorama / L'oréal, Rio de Janeiro, Rio de Janeiro - Brazil), not involving 1 mm short of the restoration margin. The teeth were then immersed in 0.05% basic fuchsin buffer for a period of 24 hours.
The teeth were washed in running water for 20 minutes to remove excess dye and allowed to dry for 24 hours at room temperature. After this, the teeth were sectioned parallel to their long axes with diamond disc (KG Sorensen, Cotia, São Paulo - Brazil) with the aid of a straight piece, obtaining two cuts of the restoration. The cut with the highest degree of infiltration of each restoration was selected and then evaluated by an examiner calibrated with a magnitude of 20 times (Pires, 2009) using a stereoscopic magnifier Sz4045 (Olympus, São Paulo, São Paulo - Brazil). The evaluated scores are described in Table 2, in Figure III, on page 21.
Table 2. Microleakage scores for sample analysis
Scores |
Penetration of dye in dentin margin |
0 |
No penetration of dye |
1 |
Dye penetration to 1/3 of the distance between the cavity margin and the axial wall |
2 |
Dye penetration up to 1/2 the distance between the cavity margin and the axial wall |
3 |
Dye Penetration to the axial wall |
4 |
Dye penetration beyond the axial wall |
The values of the obtained scores were submitted to statistical analysis by Kruskall-Wallis analysis of variance, p <0.05, by the program Bioestat 5.3.
After the microleakage test, the scores were obtained by groups, which are shown in Table 3, Figure IV, on page 22, where all groups had score zero, that is, there was no marginal microleakage occured, except for the G4 groups (conventional composite resin, without CHX with 7 days in storage), G6 (conventional composite resin, with 60 days storage CHX) and G8 (conventional composite resin without 60 days in aging CHX) [3].
Table 3. Distribution of the scores found in each group
Group |
Scores |
|
|
0 |
1 |
2 |
3 |
4 |
G1 |
9 |
|
1 |
|
|
G2 |
9 |
1 |
|
|
|
G3 |
10 |
|
|
|
|
G4 |
6 |
1 |
2 |
1 |
|
G5 |
9 |
|
1 |
|
|
G6 |
6 |
|
3 |
1 |
|
G7 |
10 |
|
|
|
|
G8 |
7 |
|
2 |
1 |
|
G9 |
10 |
|
|
|
|
G10 |
10 |
|
|
|
|
G11 |
10 |
|
|
|
|
G12 |
10 |
|
|
|
|
The results obtained after the microleakage test were submitted to the Kruskall Wallis test with p≥0.05 are presented in table 4, in Figure V, on page 23. The table shows that there were no significant differences between materials, storage time and pre-treatment with CHX.
Table 4. Results obtained after microleakage test
Group |
Median |
Interquarological Deviation |
G1 |
0 |
0 |
G2 |
0 |
0 |
G3 |
0 |
0 |
G4 |
0 |
0,75 |
G5 |
0 |
0 |
G6 |
0 |
2 |
G7 |
0 |
0 |
G8 |
0 |
1,5 |
G9 |
0 |
0 |
G10 |
0 |
0 |
G11 |
0 |
0 |
G12 |
0 |
0 |
In order to evaluate the sealing ability between the dentin and the restorative material, the adhesive performance becomes important because of its ability to bond to the tooth structure [21]. In the present study, no significant differences were found in the values of marginal microleakage between the different materials tested. Similar results were found by Guanabara and Araújo (2015), who did not find significant differences with pre-treatment with CHX at a 2-year follow-up evaluation [13].
Nascimento, et al. (2016) [20] showed that the flow composite resins used had a higher marginal sealing capacity in class II restorations after thermocycling, and without the use of CHX as a cleaning agent, proving in their study that, among composites, bulk fill resins did not present significant differences regarding the appearance of marginal microleakage [20], confirming the results found in the present study.
Results similar to the present study were also found by Gorji, et al. (2017) [12], using the Filtek Z250 composite resin (3M ESPE) with four different adhesive systems (Adiper Single Bond 2 / 3M ESPE; Clearfil SE Bond / Kuraray; Clearfil S3 Bond / Kuraray; dividing these groups with and without the use of CHX, demonstrated that there were no statistically significant differences regarding marginal microleakage [12].
The CHX pretreatment reduced the values of marginal microleakage in the study by Saffapour, et al. (2016). This difference may have occurred due to the form of aging, since these authors used thermocycling with 10.000 cycles representing 1 year of aging in the mouth. The clinical benefits with CHX are more easily observed from 12 months because of their substantivity [6].
The studies of Alsagob, et al. (2018) found no statistically significant difference between the comparison of conventional composite resins and flow, and observed that the composite bulk flow resins, when inserted in smaller increments, showed more satisfactory results regarding the microleakage analysis marginal [2], as occurred in the present study. This is because the flow potential of the flow resins allows better adaptation in the cavity, giving a lower incidence of slit formation in the tooth / restoration interface [14]. Another factor that may also have contributed to the absence of significant differences among composite resins is that CCR has been inserted by the incremental technique. As already consolidated in the literature increments of less than 2 mm decrease the force of polymerization contraction and consequently decrease the failures in the adhesive interface [11].
The resin-reinforced GIC also did not present significant marginal microleakage despite its mechanical properties being inferior to the composite resin [4,7]. The ionic bond between GIC and the coefficient of linear thermal expansion close to the tooth may have contributed to the findings of the present study.
Thus, due to the results of the present study, different materials, CHX pretreatment and aging did not interfere in marginal microleakage scores. This may be of great value, since good CHX properties are exploited without causing damage to the adhesive interface, however, further studies are needed to incorporate these techniques into the daily clinic.
It was possible to conclude that the different materials (GIC, CR and CBFR), pre-treatment with CHX and aging time (7 and 60 days) did not interfere in marginal microleakage scores.
- Alonso RC, Sinhoreti MA, Correr Sobrinho L, Consani S, Goes MF (2004) Effect of resin liners on the microleakage of class V dental composite restorations. J Appl Oral Sci 12: 56-61.
- AlSagob EI, Bardwell DN, Ali AO, Khayat SG, et al. (2018) Comparison of microleakage between bulk-fill flowable and nanofilled resin-based composites. Interv Med Appl Sci 10: 102-109. [crossref]
- Associação Brasileira de Normas Técnicas. NBR 14725-4/2014: Dados de segurança do material: DentsCare. Joinville: 1-5 (2016).
- Ayna B, Celenk S, Atas O, Tümen EC, Uysal E, Toptanci IR (2018) Microleakage of glass ionomer based restorative materials in primary teeth: An In vitro study. Niger J Clin Pract 21: 1034-1037.
- Braga R, Ballester R, Ferracane J (2005) Factors involved in the development of polymerization shrinkage stress in resin-composites: A systematic review. Dental Materials 21: 962-970.
- Breschi L, Cammelli F, Visintini E, Mazzoni A, Vita F, et al. (2009) Influence of chlorhexidine concentration on the durability of etch-and-rinse dentin bonds: a 12-month in vitro study. J Adhes Dent 11: 191-198. [crossref]
- Burke FJ, Fleming GJ, Owen FJ, Watson DJ (2002) Materials for restoration of primary teeth: 2. Glass ionomer derivatives and compomers. Dent Update 29: 10-14, 16-7. [crossref]
- Chesterman J, Jowett A, Gallacher A, Nixon P (2017) Bulk-fill resin-based composite restorative materials: a review. British Dental Journal 222. [crossref]
- Cramer NB, Stansbury JW, Bowman CN (2011) Recent advances and developments in composite dental restorative materials. J Dent Res 90: 402-416. [crossref]
- Elkerbout TA, Slot DE, Van Loveren C, Van der Weijden GA (2018) Will a chlorhexidine-fluoride mouthwash reduce plaque and gingivitis? Int J Dent Hyg 7: 1-13. [crossref]
- Ferracane JL (2011) Resin composite--state of the art. Dent Mater 27: 29-38. [crossref]
- Gorji MAH (2017) Effect of 2% chlorhexidine on the enamel microleakage of composite restorations using 5th, 6th, 7th and universal generation of dentine bonding agentes (In Vitro). J Babol Univ Med Sci 12: 36-42.
- Guanabara Araújo MSR (2015) Two-year clinical evaluation of chlorhexidine incorporation in two-step sel-etch adhesive. Journal of Dentistry 43: 140-148.
- Jaganath BM (2017) Influence of composite insertion techniques (bulk-fill and incremental nanofilled composites) on adaptability to the pulpal floor and interfacial gap formation. International Journal Of Preventive And Clinical Dental Research 4: 225-231.
- KeliÄ K, MatiÄ S, MaroviÄ D, KlariÄ E, Tarle Z (2016) Microhardness of bulk-fill composite materials. Acta Clin Croat 55: 607-614. [crossref]
- Kilambi H (2009) Evaluation of highly reactive mono-methacrylates as reactive diluents for BisGMA-based dental composites. Dental Materials 25: 33-38. [crossref]
- Kim RJY (2015) Polymerization shrinkage, modulus, and shrinkage stress related to tooth-restoration interfacial debonding in bulk-fill composites. Journal of Dentistry 43: 430-439.
- Lowe RA (2015) Advances in composite resin materials: The material science behind modern restoratives. Inside Dentistry 11: 1-7.
- Mantri SP, Mantri SS (2013) Management of shrinkage stresses in direct restorative light-cured composites: a review. J Esthet Restor Dent 25: 305-313.
- Nascimento AS (2016) Marginal microleakage in bulk fill resins. Rev Odontol UNESP 45: 327-331.
- Ortega RA, Ibarra JG, Rivas LC (2012) In vitro microleakage of three adhesive systems with three diferente solventes. Revista Odontológica Mexicana 16: 188-192.
- Saffarpour A, Saffarpour A, Kharazifard MJ, Rad AE (2016) Effect of chlorhexidine application protocol on durability of marginal seal of class V restorations. J Dent (Tehran) 13: 231-237. [crossref]
- Stanislawczuk R, Reis A, Loguercio AD (2011) A 2-year in vitro evaluation of a chlorhexidine-containing acid on the durability of resin–dentin interfaces. Journal of Dentistry 39: 40-44.

