Introduction: In the scenario of airway obstructions, orthognathic surgery consists of the surgical procedure that aims to correct deformities of the bones of the maxilla and mandible and represents today reality in the world. The growth and function of the nasal, nasopharyngeal and oropharyngeal cavities are associated with normal skull growth. Objective: To make a review of the literature on the Orthognathic Surgery and the efeitos nas vias aéreas superiores em pacientes Classe II.
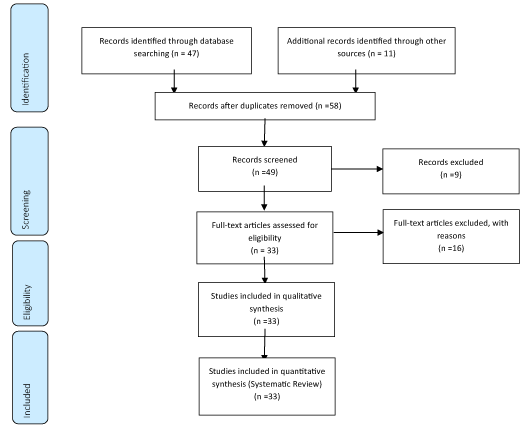
Methods: A total of 58 articles were found involving mesh terms about Orthognathic Surgery. Initially, it was held the exclusion existing title and duplications following the interest described this work. After this process, the summaries were evaluated, and a new exclusion was held. 33 articles were included and discussed in this study. Results and conclusion: The results of the present study provided promising and effective results of the main effects of orthognathic surgery in the upper airways in Class II patients. However, complications may occur. Attention is drawn to the fragility points, to encourage compulsory and detailed recording of the occurrence of complications, as well as the elaboration of a protocol to monitor its evolution.
orthognathic surgery, upper airways, dentofacial deformities, obstructive sleep apnea, malocclusion
In the scenario of airway obstructions, orthognathic surgery consists of the surgical procedure that aims to correct deformities of the bones of the maxilla and mandible and represents today reality in the world [1,2]. The technique has undergone great evolution in the last two decades and has been steadily increasing. The records of the first surgeries for the correction of dentofacial deformities date from the mid-nineteenth century and were initially limited to mandibular surgeries [2].
The pharyngeal airspace is generally described as the distance between the posterior and anterior pharyngeal walls, the tongue being the anterior border. Its width depends on the position of the soft palate, tongue and hyoid bone, whose position change may adversely affect the dimensions of the airway [2,3]. The growth and function of the nasal, nasopharyngeal and oropharyngeal cavities are associated with normal skull growth. In this context, the size of the nasopharynx increases in conjunction with the growth of the base of the skull and the development of the middle third of the face [3]. The importance of airway dimensions is that these are related to respiratory disorders, since narrow upper airway dimensions in the oropharyngeal area cause respiratory problems and may lead to reduced growth hormone levels in children [3].
Patients with maxillary retrognathism can be submitted to advancement of the maxilla, as they promote a natural appearance in the filling of the paralateronasal area. Regarding the cases of patients with horizontal deficiency in the mandible, the correction can be made with mandibular advancement, and the mentoplastias can be used in a complementary way [4].
In this context, the facial deformity, with destructive psychological and social potential, has a negative impact, which may influence not only patient self-confidence but also external relationships, resulting in social and psychological disadvantages [4]. The objectives of the patient with dentofacial deformity, related to the repair, are also psychosocial and this can express the expectation of solving their personal and social difficulties with the physical change, that is, with the improvement of their appearance by the surgical correction [4].
Thus, orthognathic surgery intervenes in patients with moderate and severe dentofacial deformities of the face, with the main objective being to centralize the achievement of functional balance and harmony in facial aesthetics [5]. Obstructive sleep apnea is the arrest of the airway through the upper airway, in the presence of respiratory effort, lasting more than 10 seconds. The hypopnoea, constitute a reduction in the passage of air, in said area, in this same period of time. These respiratory events occur innumerable times and exclusively during sleep, determining symptoms and signs that characterize Sleep Obstructive Hypopnea Apnea Syndrome [5].
Patients with anatomical abnormalities that contribute to the narrowing or obstruction of the pharyngeal air space during sleep are benefited with orthognathic surgery to normalize the soft and hard tissues of the face [6].
The present work had as objective to make a review of the literature on the Orthognathic Surgery and the efeitos nas vias aéreas superiores em pacientes Classe II.
Eligibility and study design
A total of 58 articles were found involving Orthognathic Surgery; Upper Airways; dentofacial deformities; Obstructive sleep apnea; Malocclusion. Initially, it was held the exclusion existing title and duplications following the interest described this work. After this process, the summaries were evaluated, and a new exclusion was held. 33 articles were included and discussed in this study.
Experimental and clinical studies were included (case reports, retrospective, prospective, randomized trials and systematic review and meta-analysis) with qualitative and/or quantitative analysis. Initially, the keywords were determined by searching the DeCS tool (Descriptors in Health Sciences, BIREME base) and later verified and validated by MeSh system (Medical Subject Headings, the US National Library of Medicine) in order to achieve consistent search, following the rules of systematic review- PRISMA (Transparent reporting of systematic reviews and meta-analyses- http://www.prisma-statement.org/).
Literature review and discussion
This review has demonstrated the main benefits of orthognathic surgery on the airways in relation to the length of the soft palate, nasopharynx air space, oropharynx air space, air space of the hypopharynx and air space of the hypopharynx at the time of pogonium
Thus, as literary results, Foltán R, et al. [5], in a study on the influence of orthognathic surgery on ventilation during sleep, found an average age of 22 ± 0.8 years, ranging from 16 to 28 years, which contrasts with our study in which the mean of patients were older, 36.50 ± 12.10 years, with ages ranging from 23 to 52 years and with a higher prevalence in the female gender. There is little data available on the predominance of facial features. However, Sant'ana E, et al. [6] showed that the Brazilian profile presented a substantial difference when compared to the North American profile.
In addition, Faria, et al. [7], Who demonstrated, through comparisons of cephalometric radiographs, that in each millimeter of maxillo-mandibular advancement, there is an increase of 0.76 mm in the retropalatal region and 1.2 mm in a retrolingual region. However, there was a decrease in the upper airway space in patients submitted to maxillary advancement associated with mandibular retreat, confirming with Mattos, et al. [8] that in orthognathic surgery mandibular retreatment leads to a decrease in parapharyngeal space and maxillary advances, combined with indentations can lead to a moderate decrease in the upper airways.
The treatment of dentofacial deformities is currently one of the most discussed fields in the area of Buccomaxillofacial and Craniomaxillofacial Surgery [1-3]. His study has encompassed biological, pathophysiological, surgical and anesthetic techniques, preoperative and postoperative management, as well as craniofacial growth and development, and harmony and facial aesthetics [4].
This procedure aims to establish a harmonious facial esthetics, optimal functional occlusion and improvement of airway conditions, which are the most important goals of orthodontic-surgical treatment [1,9]. The correct diagnosis of a malocclusion associated with skeletal deformity is essential for indication of treatment, leading to a multidisciplinary planning, which leads to an aesthetic and functional correction of the case, providing the patient with functional occlusion and facial harmony [9]. Maxillo-mandibular advancement surgery promotes anteroposterior, vertical and lateral-lateral movement, due to the displacement of the bone bases to a new position, generating tensions in the soft tissues of the region, and may present significant changes in facial appearance and pharyngeal space [10-14].
Another study explored how mandibular advancement without maxillary involvement would affect posterior air space in patients with mandibular retrognathism [4]. Cone-beam computed tomography (CT) was performed for 20 patients before and six months after the mandibular advancement. Cephalometric analysis at both moments included two-dimensional and three-dimensional upper airway evaluation. Eight men and 12 women presented preoperative mean W values (7.4) (1.54) mm, with airway area of 7.11 (1.88) cm2 and volume of 14.92 (4.46) cm 3. Six months postoperatively presented a Wits value of 2.7 (0.41) mm, an airway area of 11.33 (3.49) cm2 and a volume of 25.7 (6.10) cm3. There was an average increase (range) of 59 (22-82)% of the area and 73 (29-108)% of the volume. A preoperative figure (Flow chart) of 8.0 mm or greater was significantly correlated with a greater increase in posterior air space (p = 0.002). At the same time, an improvement in the Reasoning value of 4.5mm or more correlated significantly with an increase in volume (p = 0.016). The effect of mandibular advancement on posterior air space was significant, and the volumetric effect appears to be even more relevant than two-dimensional changes [4].
The need for development of centers for the correction of dentofacial deformities in our country is notable for the increase in demand for these services as shown in this study during the period studied from 2002 to 2016 [17-20]. These data demonstrate the need for constant scientific and technical improvement, as well as understanding the profile of these treatments for the increasingly objective treatment of these deformities [20].
In continuation, orthognathic surgery treats dentofacial deformities and its importance is found not only in the correction of occlusion, but also in facial aesthetics [21-24]. This means that the psychosocial aspects are directly related to this type of treatment, since the facial appearance influences the formation of the body image, the identity and the self-esteem [25-28], with greater demand for the women. However, the gender homogeneity of the present study can be explained because these orthognathic surgery patients treat not only aesthetic-functional deformities [29].
Furthermore, some studies have shown a statistically significant association between respiratory problems and Class II skeletal discrepancies [30]. The growth and function of nasal, nasopharyngeal and oropharyngeal cavities are strongly associated with normal skull growth. Patients with Class II malocclusion are characterized by having a maxillary protrusion, a mandibular retrusion or both, most of which can be attributed to a retromandibular [30]. These are considered a risk factor for the development of upper airway disorders and deficits in the oropharyngeal route, since the space between the cervical spine and the mandible body is diminished, which leads to a posterior position of the tongue and of the soft palate, increasing the likelihood of a compromised respiratory function during the day and possibly causing nocturnal problems, such as snoring, upper airway resistance syndrome, or obstructive sleep apnea syndrome [30-33].
Thus, this surgery has an effect on the maxillo-mandibular function, the stability of the hard tissues and the facial esthetics of the patient [31]. The effects on the facial profile and the relationship between soft and soft tissue changes have been reported in both the short and long term. The different surgical techniques, the natural aging process, the initial growth direction and the remodeling process should be considered when evaluating the positional stability of these tissues [31].
Jung and Park [32] report the restoration of facial harmony and ideal occlusion in individuals with severe skeletal occlusion. Much is discussed in the scientific environment regarding the effect of orthognathic surgery on the maxillofacial complex, because there are biomechanical, occlusal and sensorial relationships between the structures of this complex [32]. Thus, there was a restoration of masticatory and speech functions, as well as improvement of facial aesthetics [32].
A similar study to the present study presented similar findings. An important finding in this study was that 56.0% of the patients had operated exclusively on the maxilla and 20.5% of the patients had the maxilla and mandible operated, representing 76.5% of the analyzed sample [10]. It can be observed that many of the patients with malocclusions have maxillary problems in association with mandibular problems, which calls us to a precise and detailed diagnosis of the malocclusion and face, considering all the structures involved, both separately and together, so that the treatment plan is successful, not only due to the occlusal aspect, but also aesthetic and functional, guaranteeing stability to the skeletal, dental, muscular structures and respiratory function aiming at the treatment of retropalatal and retrolingual collapse in patients with Obstructive Apnea Syndrome and Obstructive Hypopnea Syndrome Sleep [10].
The results of the present study provided promising and effective results of the main effects of orthognathic surgery in the upper airways in Class II patients. However, complications may occur. Attention is drawn to the fragility points, to encourage compulsory and detailed recording of the occurrence of complications, as well as the elaboration of a protocol to monitor its evolution.
There is no conflicts of interest between authors.
- Jang SI, Ahn J, Paeng JY, Hong J (2018) Three-dimensional analysis of changes in airway space after bimaxillary orthognathic surgery with maxillomandibular setback and their association with obstructive sleep apnea. Maxillofac Plast Reconstr Surg 40: 33. [Crossref]
- Gong X, Li W, Gao X (2018) Effects of craniofacial morphology on nasal respiratory function and upper airway morphology. J Craniofac Surg 29: 1717-1722.
- Louro RS, Calasans-Maia JA, Mattos CT, Masterson D, Calasans-Maia MD, Maia LC (2018) Three-dimensional changes to the upper airway after maxillomandibular advancement with counterclockwise rotation: a systematic review and meta-analysis. Int J Oral Maxillofac Surg 47: 622-629.
- Dalla Torre D, Burtscher D, Widmann G, Rasse M, Puelacher T, Puelacher W (2017) Long-term influence of mandibular advancement on the volume of the posterior airway in skeletal Class II-patients: a retrospective analysis. Br J Oral Maxillofac Surg 55: 780-786.
- Foltán R, Hoffmannová J, Pavlíková G, Hanzelka T, Klíma K, et al. (2011) The influence of orthognathic surgery on ventilation during sleep. Int J Oral Maxillofac Surg 40: 146-149. [Crossref]
- Sant´Ana E., Furquim LZ, Rodrigues MTV, Kuriki EU, Pavan AJ, et al. (2006) Planejamento digital em cirurgia ortognática: precisão, previsibilidade e praticidade. Rev ClinOrtodon Dental Press Maringá 5: 92-102.
- Faria AC, Xavier SP, Silva Jr. SN, VoiTrawitzki LV, de Melo-Filho FV (2013) Cephalometric analysis of modifications of pharynx due to maxilla-mandibular advancement surgery in patients with obstructive sleep apnea. Int J Oral MaxillofacSurg 42: 579-584.
- Mattos CT, Vilani GN, Sant'Anna EF, Ruellas AC, Maia LC (2011) Effects of orthognathic surgery on oropharyngeal airway: a meta-analysis. Int J Oral Maxillofac Surg 40: 1347-1356. [Crossref]
- Angle EH (1899) Classification of malocclusion. Dent Cosmos 41: 248-264.
- Marques, Caroline Gabriele; Maniglia, José Victor and Molina, Fernando Drimel (2010) Perfil do Serviço de Cirurgia Ortognática de uma escola médica. Braz j otorhinolaryngol 76: 5.
- Petry C, Pereira MU, Pitrez MC, Jones MH, Stein RT (2008) The prevalence of symptoms of sleep-disordered breathing in Brazilian schoolchildren. J Pediatr 84: 123-129.
- Ibrahim AS, Almohammed AA, Allangawi MH, A Sattar HA, Mobayed HS, et al. Predictors of obstructive sleep apnea in snorers. Ann Saudi Med 276: 421-426. [Crossref]
- Pinto, Leonardo Augustus Peral Ferreira (2013) Avanço maxilomandibular no tratamento da Síndrome da Apneia e Hipopneia Obstrutiva do Sono. Rev. cir. traumatol. buco-maxilo-fac., Camaragibe.
- Schendel S, Powell N, Jacobson R (2011) Maxillary, mandibular, and chin advancement: treatment planning based on airway anatomy in obstructive sleep apnea. J Oral Maxillofac Surg 69: 663-676. [Crossref]
- Bailey LJ, Proffit WR, White R Jr (1999) Assessment of patients for orthognathic surgery. Semin Orthod 5: 209-222. [Crossref]
- Castro V, Do Prado CJ, Neto AIT, Zanetta-Barbosa D (2013) Assessment of the epidemiological profile of patients with dentofacial deformities who underwent orthognathic surgery. Journal of Craniofacial Surgery 24: 271-275.
- Cunningham SJ, Moles DR (2009) A national review of mandibular orthognathic surgery activity in the National Health Service in England over a nine year period: Part 2-patient factors. British Journal of Oral and Maxillofacial Surgery 47: 274-278.
- Noffze MJ, Tubbs RS (2011) René Le Fort 1869-1951. Clin Anat 24: 278-281. [Crossref]
- O'Brien K, Wright J, Conboy F, Appelbe P, Bearn D, et al. (2009) Prospective, multi-center study of the effectiveness of orthodontic/orthognathic surgery care in the United Kingdom. Am J Orthod Dentofacial Orthop 135: 709-714. [Crossref]
- Panula K1, Finne K, Oikarinen K (2001) Incidence of complications and problems related to orthognathic surgery: a review of 655 patients. J Oral Maxillofac Surg 59: 1128-1136. [Crossref]
- Proffit WR, Jackson TH, Turvey TA (2013) Changes in the pattern of patients receiving surgical-orthodontic treatment. Am J Orthod Dentofacial Orthop 143: 793-798. [Crossref]
- Robl MT, Farrell BB, Tucker MR (2014) Complications in orthognathic surgery. Oral and Maxillofacial Surgery Clinics of North America 26: 599-609.
- Scariot R, DA Costa DJ, Rebellato NLB, Müller PR, Da Conceição Ferreira R (2010) Epidemiological analysis of orthognathic surgery in a hospital in Curitiba, Brazil: Review of 195 cases. Revista Española de Cirugía Oral y Maxilofacial 32: 147-151.
- Sato FRL, Mannarino FS, Asprino L, De Moraes M (2014) Prevalence and treatment of dentofacial deformities on a multiethnic population: a retrospective study. Oral and Maxillofacial Surgery 18: 173-179.
- Steinhäuser EW (1996) Historical development of orthognathic surgery. Journal of Cranio-Maxillofacial Surgery: official publication of the European Association for Cranio-Maxillofacial Surgery 24: 195-204.
- American Association of Oral and Maxillofacial Surgeons (AAOMS). Clinical Paper. Criteria for Orthognathic Surgery. 2015. Available at: http://www.aaoms.org/images/uploads/pdfs/ortho_criteria.pdf Accessed February 20, 2019.
- Farhad B. Naini, Daljit S. Gill. Orthognathic Surgery: Principles, Planning and Practice is a definitive clinical guide to orthognathic surgery, from initial diagnosis and treatment planning to surgical management and postoperative care. WileyOnline Library.
- Brunetto DP, Velasco L, Koerich L, Araujo MT (2014) Prediction of 3-dimensional pharyngeal airway changes after orthognathic surgery: a preliminary study. J Orthod Dentofacial Orthop 146: 3.
- Foltán R, Hoffmannová J, Pavlíková G, Hanzelka T, Klíma K, et al. (2011) The influence of orthognathic surgery on ventilation during sleep. Int J Oral Maxillofac Surg 40: 146-149. [Crossref]
- Hasebe D, Kobayashi T, Hasegawa M, Iwamoto T, Kato K, Izumi N, et al. (2011) Changes in oropharyngeal airway and respiratory function during sleep after orthognathic surgery in patients with mandibular prognathism. J Oral Maxillofac Surg 40: 584-592.
- Jaspers GW, Booij A, De Graaf J, De Lange J (2013) Long-Term Results of Maxillomandibular Advancement Surgery In Patients With Obstructive Sleep Apnoea Syndrome. J Oral Maxillofac Surg 51: 37-39.
- Jung HD, Jung YS, Park HS (2009) The chronologic prevalence of temporomandibular joint disorders associated with bilateral intraoral vertical ramus osteotomy. J Oral Maxillofac Surg 67: 797-803.
- Kobayashi T, Izumi N, Kojima T, Sakagami N, Saito C (2011) Progressive condylar resorption after mandibular advancement. J Oral Maxillofac Surg 50: 176-180.