Dental anxiety and phobia is common and has serious consequences for oral health. It is estimated that more than one in seven of the population of Western countries avoid dental care due to fear. The aim of this paper is to combine dentistry and psychology by looking at dental anxiety and phobia within the Western world, identifying its key causes, establishing what impacts it has on sufferers, and examining what dentists and others can do to alleviate these problems. Key treatments and specific psychological therapies are reviewed and suggestions are made for future strategy and research.
Studies have shown that up to 15 per cent of the Western population has a form of extreme dental anxiety that stops them from accessing dental care due to their fear [1,2]. As a person’s dental health deteriorates their self-esteem and social confidence are negatively affected. The pattern of their subsequent avoidance sets up a ‘vicious cycle’ of worsening fears and declining oral health.
In the past decade it has become increasingly recognised that more effort is needed to work to alleviate people’s fears across a wide range of health interventions using behaviour management techniques and psychological interventions. The aim is to help people better understand the clinical processes and procedures and teach them strategies to manage their anxiety and grow their self-confidence to cope without resort to pharmacological interventions.
The treatment of fear generally starts with basic education and follows a ‘stepped care’ model [3] where the least complex types of help are offered first, up to specific psychological therapies delivered by experts for those in need of this most complex intervention. It is widely acknowledged that phobias can be successfully treated and that the harmful avoidance that prevents the patient from accessing a necessary treatment can be successfully challenged and overcome. The sooner that this outcome can be achieved, the greater is the emotional, practical and financial saving to the patient, the service and the treasury.
Fear, anxiety and phobia
Fear is a normal response to any stimulus perceived as threatening that may involve discomfort or pain. When a fear becomes excessive, beyond the proportional response to the external threat, and interferes with the individual’s ability to function, then this fear may meet the criteria for an anxiety spectrum disorder such as a specific phobia.
How are fears acquired?
The development of fear can be considered within two broad frameworks where fears are viewed as learned or naturally occurring.
The first of these proposed by Rachman [4] is based on Learning Theory and suggests three ways in which fear is acquired:
- Direct Conditioning where a single exposure to cues associated with an intensely aversive event can lead to a person becoming fearful of those cues alone.
- Modelling or Vicarious Learning, where a learned fear is acquired through observing another’s fearful reactions to specific events or stimuli. Infants actively search for the appropriate responses to stimulants from their caregivers to gain cues as how to react to specific situations - known as ‘social referencing’.
- Instruction /Negative information. This increases a person’s negative beliefs about a proposed danger and the expectation of threat and discomfort that they will gain from it.
A second framework for the acquisition of fear highlights our nature: Biological Preparedness and Genetic Factors.
Biological Preparedness was first suggested by Seligman [5] who stated that certain fears are innate and evolutionarily advantageous, ensuring the survival of the species. Such fears include; heights, crawling insects, or thunder and lightning. Fears of pain and injury are thought to be universal and protective, promoting healthy responses to avoid threats and danger.
Genetic Factors linked to fear acquisition are partly based on research from twin studies, where fears in one twin predict those in the other. There also appears to be strong correlations of intergenerational fears in families. This research is sometimes difficult to interpret and learning theorists interpret these findings differently, highlighting that twins share similar environments and parenting. It could therefore be considered that these factors influence their fear responses, rather than exclusively their genes.
Differences between dental phobia and anxiety
Dental anxiety is the normal psychological response to a dental stimulus that has been interpreted as harmful or dangerous to the individual. This can be experienced as a level of uneasiness around dental appointments or specific dental procedures. Dental phobia however, according to the Diagnostic and Statistical Manual of Mental Disorders [6] is described as a, “Marked and persistent fear that is excessive or unreasonable”. Phobic patients are invariably avoiders of dental care and therefore have more severe consequences that those with dental anxiety.
Dental anxiety is much more common as it is essentially a fear of the unknown throughout a dental experience. This phenomenon is felt by many people regardless of country, culture and living conditions [7].
Weiner and Sheehan, [8] proposed that there are two types of dental anxiety, exogenous (due to a traumatic experience) and endogenous (deriving from other anxiety disorders). However, the University of Washington has categorised dental fear into four different groups; Fear of Specific Stimuli, Distrust of Dental Personnel, Generalized Anxiety, and Fear of a Medical Catastrophe. All of which can still be classified into either the exogenous form of dental anxiety or the endogenous [9].
Measuring dental anxiety
The level of dental anxiety varies greatly from person to person and can be assessed using various different scales. It is frequently measured on the Modified Dental Anxiety Scale, MDAS [10], a simplified rating system, adapted from Corah’s original Dental Anxiety Scale [11]. The scale used widely in the UK, asks five questions such as, ‘If you went to the dentist tomorrow for treatment how would you feel’ and ‘If you were about to have a tooth drilled how would you feel’. These questions are rated by the patient on a five-point scale from ‘Not anxious’ to ‘Extremely anxious’. This simple measure is a widely used and reliable. It allows for comparison of data to be collected between different investigations, to see trends and patterns for clinical research purposes. The highest possible score is 25. A score of 5-9 indicates low/no dental anxiety, 10-18 suggests moderate dental anxiety, and the cut off score of 19 or more equates to severe dental anxiety.
Triggers and causes of dental anxiety/phobia
Eighty percent of dental phobia is believed to be acquired exogenously, through negative experiences [12]. Traumatic experiences in childhood can lead to a lifetime of severe dental anxiety and phobia. Often this can be the hardest to treat as the memories can sometimes have been forgotten, making the phobia seem more irrational.
The stereotypes of dentists being cold and controlling in character can have a huge psychological impact on phobics, exacerbating their fear. Pain caused by a dentist who is perceived as caring is much less likely to result in psychological trauma [13]. These perceived images of professional dentists predict the avoidance behaviours in phobics, as the negative images discourage a person further from jumping the first hurdle to make an appointment to see the dentist and gain the beneficial effects of dental care.
A study by Oosterink et al. [13] found that the most fear provoking stimuli was associated with invasive stimuli such as surgical work, compared with the least anxiety provoking stimuli which was non-invasive for instance, meeting the dentists themselves. This shows that the phobia can be subjective and underpinned by specific items which can generalise, such that the whole event collectively induces fear and anxiety.
Dental anxiety can also be vicariously learned through exposure to the phobia. This is learning that is derived through indirect sources such as observing other’s behaviour.
This can come through relatives, close friends or the experience of strangers that react negatively to dental stimuli, but it may also be catalysed through a common negative image of dental phobia/anxiety portrayed within society and the media. However, some interesting research from Townsend et al. [14] showed that this factor of vicarious learning though significant in some people, is generally only of minor importance and is not a major cause of dental anxiety.
Other causes of dental anxiety and phobia can be as simple as an incompatibility between patient and professional that undermines confidence, increases a feeling of not being in control and creates an expectation of discomfort or pain [15]. Often specific dentists caring for a patient in childhood continue to be blamed by the same patients in adulthood for their on-going anxiety. This highlights the importance of successful and reassuring early contacts with a dentist as a key factor in minimising dental anxiety.
Who is most susceptible to dental anxiety/ fear?
The UK 2009 NHS Adult Dental Health Survey [16] indicates that women exhibit significantly greater dental anxiety than men, with 17% of women scoring above 19 on the MDAS – a score indicating extreme dental anxiety. This finding is further supported within a study by Heft et al. [17], showing that only 8% of men report that they are dentally anxious. However, these data can be questioned as Buchanan et al. [18] found no apparent differences between men and women in their level of dental anxiety, or their independent efforts to overcome their fear. The added issue in the interpretation of these data is whether men and women are equally willing to admit they have a phobia of the dentist? The theory of men having a harder time admitting to certain fears is backed up by the widely observed pressure of societal norms to be tough, and strong – and not being afraid of things like the dentist. Whereas the average woman does not face the same conventions from society, so is perhaps more willing to admit her fears.
Another result from the UK NHS Adult Dental Health Survey [16], showed that those from a lower socio-economic background have a higher MDAS score across all questions within the scale. This could be due poorer understanding of the processes involved in dentistry or lower attendance of a dental practice. The costs of dentistry are subsidised with the NHS though this cost can still be a barrier. Those with more money can pay more for private dental treatment where there is often more time to build a relationship with the dentist and address any anxiety the patient may have.
Young children especially are susceptible to being fearful of the dentist. The clinical environment in which dentistry is practiced is often experienced as strange and foreboding. The feelings of being constrained during the examination and procedures, the smells, poking and prodding from fearsome instruments, and the harsh noises are all likely to induce fear, even before any discomfort from the procedures. These fearful experiences are able to incubate in the minds of the young and can thereby grow between consultations. The fears are often carried through and beyond childhood, and those initial perceptions and experiences whether these are positive or negative will likely underpin dental anxiety in the future.
Dental anxiety is also shown to be more common in those who have endured sexual abuse in the past [12]. Visits to the dentist can leave victims with flashback’s or dissociative episodes, dazed, lack or response, or unexplained sudden crying. The link between dental anxiety and a history of abuse is put down to the mirrored experiences sufferers would face in a dental appointment. These can include being told what to do, lack of control laying in the dentist’s chair, with all power given to the dentist, an inability to move, trust issues and objects focused around the mouth.
Responses to exposure to fear
The immediate cognitive response when any phobia is triggered is based in three specific exaggerations;
- The likely adversity of the event,
- The probability of the worst case scenario happening
- An underestimation of their ability to cope.
This will be followed or prefaced by elements of physiological response such as involuntarily freezing [19] or changes in facial muscle tension. Added to this, is the patient’s mounting feelings of dread, terror or panic. An escape response from the patient would be the next expected behaviour after exposure if the chance occurs, with repeated avoidance behaviours following in the months afterward.
In general, children and adults tend to respond in different ways to dental stimulants. Children respond in overt ways, often because they do not feel the pressures of societal convention to behave in a way that will not offend people or create negative attention towards them. Adults on the other hand are more likely to respond in a more constrained way to either remain dignified or not offend others.
Impacts of dental anxiety
Through various research a significant correlation has been found between dental anxiety and avoidance of dental care in the general population [20,21], indicating that avoidance behaviours are prevalent in those with dental anxiety. It has also been shown that the higher the level of a person’s dental anxiety, the longer is the avoidance period, leading to a higher risk of decay and dental problems, inevitably leading to overall worsening oral health.
In a study by Hakeberg et al. [22] they measured difference in oral health between those with dental phobias compared with a control group of non-phobic dental patients. The two groups were matched by age, marital status, and housing standard. Overall, the results showed phobic patients had a fewer number of teeth, higher number of caries, and a worse condition of their gums, but overall fewer restored, filled teeth surfaces. This shows clearly that despite their significantly poorer oral health, phobic patients were much less inclined to hold regular dental appointments, thereby exacerbating the deterioration in their teeth and gums.
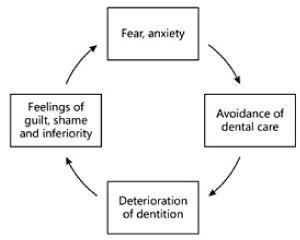
These avoidance behaviours shown by patients are an example of the ‘vicious cycle of dental anxiety’ [23] which some patients can fall into. The initial fear within dental anxiety patients can overwhelm them leading to avoidance of dental care, which results in deterioration of their dental health. Continued avoidance means a patient’s oral health can suffer greatly, creating negative thoughts over the appearance of teeth [24]. This leads to a lowering of self-esteem and causes guilt and embarrassment within the individual. This increased self-consciousness can escalate further leading to isolation and withdrawal from social groups and an increased level of social anxiety. Over time this pattern of events can lead to heightened anxiety, isolation, depression and the maintenance and continuation of this ‘vicious cycle’.
The highest levels of cognitive and physiological impact surround the time of a booked dental appointment according to research conducted by Cohen et al. [25]. These impacts were found to range from smaller reactions that are more common within the general population, such as sweating and faster heart rates whilst in a dental waiting room, to sleepless nights leading up to an appointment for the more acute dentally anxious, to severe cognitive reactions of picturing catastrophic dentally related scenarios, or suggesting extreme measures such as extracting all teeth from their mouth in order to prevent future oral pain which would lead to requiring further dental work.
The impact of dental phobia on a patient is also often evident within their daily routines. Disturbing intrusive thoughts can prevent sufferers from even watching television programmes that include scenes of dentists within them, as it triggers too much anxiety [25]. Due to poor oral health based on ongoing issues that are not treated as a result of a phobic patient’s avoidant behaviours, their diet may be impacted, being unable to eat hard or chewy foods at very cold or hot temperatures, due to discomfort.
Further research shows that high levels of dental anxiety are also linked with increased substance abuse, increased alcohol and drug use, poorer diet, low self-confidence, increased emotional volatility, and greater absence from work and avoidance of human contact, leading to loneliness and isolation. Nonetheless, all of these negative effects have been found to be reversible following successful psychological and oral treatment [26,27].
However, there is other interesting research that demonstrates that the impact of dental anxiety can vary greatly and not all patients with dental fears who avoid treatment will experience poor oral health. Cohen et al. [25] researched the impacts of anxiety on daily life of patients with an average MDAS score of 21.5. Through in-depth interviews, some patients explained that their dental anxiety motivated them to practice high standards of oral health, making sure to brush twice a day, using floss and mouthwash, in order to enable them to reduce or avoid the need for any dental interactions.
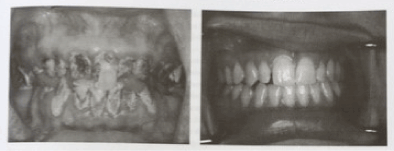
These images were taken within a study carried out in a dental anxiety research clinic in Gothenburg, Sweden, comparing two different patients with matched for level of dental anxiety, period of avoidance, and age of referral [28]. These markedly differing states of oral health highlight the varying impact dental anxiety can have on different people, showing there is not a standardised relationship between oral health and dental anxiety.
Dentists’ behaviours and responsibilities
The dentist has the primary role in minimising the emergence of dental anxiety, and preventing low dental anxiety from snowballing into dental phobia. Research shows that this is achieved by establishing rapport and trust with patients to build up and maintain a friendly and trusting working relationship.
The Four Habits Model illustrates how this may be done. This model developed by Frankel and Stein [29], stresses the importance of four key behaviours as a guide for optimal medical appointments. This also appears to be a very good template to follow for dentists meeting new patients.
- Invest in the beginning:
This stage can often be ignored in a busy dental practice with limited time. However, the initial moments to establish a kind, trusting relationship and giving verbal and nonverbal reassurance are invaluable. The actions of meeting the patient in the waiting room with a warm smile and clear introduction can be key in setting the tone for a successful therapeutic relationship to follow.
- Extract the patient’s perspective:
Asking the patient how anxious they are about coming to the dentist and if necessary, to rate their feelings on a 10point scale, provides important insight from the beginning, allowing a dentist to adjust their professional manner accordingly.
- Demonstrate empathy:
If the patient’s response indicates higher levels of anxiety, the dentist should firstly try to normalise dental anxiety and explain how common this response is. They can then ask what might be done to make the patient feel less anxious. Giving the patient choice and handing over some control is often helpful in reducing their fear.
- Invest in the end:
When a patient has faced their fears and coped as well as they could with the appointment it is very important to offer abundant praise. Walking out of the consultation with a positive mind-set will greatly reduce the chances of any avoidance behaviours or anxiety developing in the patient between meetings.
Pharmacological sedation
This intervention is first explained and agreed with the patient and can commonly be used to allow work within a person’s mouth that would normally be difficult or impossible without sedation. There are different types of sedation, ranging from simple nitrous oxide, which is commonly used within a medical setting to calm a person down to a level where they could cope with treatment; to intravenous sedation taking effect more quickly and allowing a more precise effect from a specific dosage of the drug. This method can be used in combination with nasal spray to sedate a person initially at a lower level, so as to make the experience of injection easier. The more extreme version of sedation is a general anaesthetic, where a person is made fully unconscious and treatment becomes straightforward and free of any awareness or overt anxiety. However, this method is only used when it can be ethically balanced out with the usual risks that come with a general anaesthetic.
The most common criticism of the use of general anaesthetic is that this merely allows for treatment to improve a person’s dental status, without solving the problem at heart – an individual’s phobia. This conclusion is supported by a study carried out by Hakeberg et al. [22] on 29 dentally anxious patients in three groups. They compared the use of Behavioural Therapy (BT) treatment in one group, treatment under sedation with a benzodiazepine, a minor tranquilliser on the next, and lastly a group under general anaesthesia (GA). They compared the long-term effects on anxiety, oral health, and attendance rates of each of these different interventions styles. After 10 years following initial treatment, the patients were re-assessed to show that dental anxiety on MADS scale was reduced for all except the group who received treatment under general anaesthetic. This finding was mirrored again in the finding of 92% of BT recipients regularly attending the dentist, compared with only 33% of patients under GA, highlighting its ineffective use in addressing dental anxiety and phobia itself. However, sedation can be the necessary reality for phobic patients if immediate treatment is required to solve an issue that would otherwise not be possible to go ahead without the aid of sedation.
Graduated exposure
Positive early experiences of the dentist are key to maintaining lifelong oral health appointments. They are especially important in reducing dental fear as 33.3 percent of patients in one study had become dentally anxious in adolescence [30]. Young children should be ideally seen every 6 months for non-invasive treatments where they have an opportunity to learn, interact with instruments and experience procedures that can help build confidence. Studies that have tried to achieve this familiarity of the dentist for children in primary schools have shown significant positive effects of reducing subsequent anxiety and avoidance in attending the dentist later on in life.
Cognitive behaviour therapy (CBT)
Cognitive Behaviour Therapy is based on the theory that events themselves do not cause us distress but instead the thoughts, images and beliefs that we have about these events predict our emotional reactions and behaviour [31].
The key to CBT is to help a person to identify the key thoughts and images that are causing them to be anxious in a particular situation and learn to gradually challenge and change these into a more adaptive and helpful pattern of thinking. The evidence for CBT treating specific phobias is substantial. A study within a community based clinic for fearful patients in Sweden showed that attendance was significantly higher in those who had received a simple cognitive-behavioural therapy treatment, in comparison to those who had just had more exposure to a dental setting [32].
The dentist can help re-educate the patient’s thinking where misconceptions arise, and seek to involve, inform and instruct the patient throughout the intended procedures. The widely quoted NHS motto, ‘No decision about me, without me’ is a key component of the clinician and patient partnership associated with effective CBT.
Cognitive Behaviour Therapy has the most clinical evidence to support its use in treating fear. However, if a patient is not intent in overcoming their phobias then the therapy is unlikely to work. High levels of motivation from the patient are invariably the best predictor of response to any psychological interventions
Professional psychological therapy for dental phobia
Professional NHS therapy for Dental Phobia in the UK is now becoming widely available within ‘Talking Therapies’ – the government initiative to make CBT accessible to those suffering with anxiety and depression. This gives many more people access to try and overcome their fears. For more complex dental phobias, clinical psychologists will provide therapy within secondary care mental health services.
Advanced cognitive behavioural therapy
Ӧst [33] has pioneered a prolonged, single session of CBT for phobias that is highly effective, avoiding the reoccurrence of fear between sessions. More gradual therapy with a number of hourly sessions each week is also commonly used.
A full personal history is taken at the outset of therapy and from this and an analysis of the patient’s experiences, a formulation is developed. This sets a context to explain how past experience has led to the specific pattern of unhelpful thoughts that form the basis for a person’s fear. The therapy then explains the process by which the past context in which fears were developed, is compared with the present, and the key differences are highlighted. A hierarchy of fear is then created in collaboration with the patient and a gradual exposure to each of the fears is then slowly conducted whilst challenging the negative thoughts and encouraging non-avoidance. A lot of emphasis is placed on progress, however minimal it may be, and this should always be highly praised and encouraged throughout the course of treatment.
The primary goal of Cognitive Behavioural Therapy is not to eliminate the fear altogether but rather to help a person to understand and manage their phobia better and so be able face the feared situation in a more confident way, thereby reconceptualising the situation with significantly less fear.
Eye movement desensitisation and reprocessing (EMDR)
Eye Movement Desensitisation and Reprocessing is a relatively new therapy that was first formulated to treat trauma [34]. Although the mechanism by which the treatment works is still not fully understood, it is assumed that by mimicking the rapid eye movement that is associated with sleep, it is possible to help people better process past traumatic memories that have become stuck in their memory network.
Generally, clients are asked to follow their therapist’s finger with their eyes moving rapidly back and forth whilst focussing their thoughts on a specific past trauma. Alternatively, this same procedure can be carried out using buzzers or headphones that repetitively buzz in left and then right hands or bleep in left and right ears.
Thinking about past trauma whilst alternately stimulating the left and right sides of the brain, will often produce a rapid decline in fear. Doering et al. [35] found that 87% of people with extreme levels of dental phobia reported a “horrific” event occurring during a past dental procedure. Of those which were treated with EMDR, 83.3% were in regular dental treatment one year later, showing how effective this method of treatment can be.
Prevention must be a focal point and primary goal for future programmes of research that want to understand the acquisition and reduction of dental anxiety and phobia. The effects of phobia that causes poor oral hygiene and the negative physical, psychological and social consequences that ensue must be tackled early on.
Putting in place programmes of oral education within nursery and primary schools allows for early introduction and familiarity to dentists and their procedures. Simple rewards for completing procedures, such as through using stickers and goodie bags, can strongly reinforces a child’s positive experience of the dentist.
Future studies should continue to compare different types of child friendly environments in which dentists operate. Researching change to the stark clinical rooms of a usual dental practice and creating additional fun distractions for children and adults that decrease their anxiety are needed. In this way optimal clinical environments can become widespread . Children with fears must be coaxed back to confidence and we need to understand what behaviours, rewards and skills are best suited to this task.
For adults with severe dental anxiety we must first find those who have continued to display avoidance behaviours due to fear. Public education programmes need to be put in place to reiterate the importance of good dental hygiene and provide advice, support and interventions for those who avoid. Specialist clinics with multi-disciplinary teams including clinical psychologists are being set up in Norway to cater for this avoidant group of dentally phobic patients and this practice should become more widespread.
Dentistry is also required to continue refining its approach and methods to be less frightening. Although the profession has changed immensely over the past 50 years, some current procedures still undermine the sense of control for a patient, create pain and feel too invasive. New technology, i.e. the use of lasers rather than drills in dental practices, despite still being a novelty, offers the opportunity for better patient experience with less need for anaesthesia and therefore no needles, no harsh sounds, and less overall anxiety.
Experimental trials to demonstrate these and other benefits are needed urgently.
Dental anxiety is common and affects up to 15 per cent of the population. It has many severe negative effects impacting people beyond just fear to seriously undermine their oral health, their social status, and their confidence to interact with others in work and socially. Accessing these dentally phobic people within the population is a challenge. Their lack of optimism that things can change for the better and their avoidance behaviours mean they are rarely present at the dentist. Those with a phobia could be reached by national campaigns, and then given education, increased hope and appropriate help to overcome their fears and avoidance. Most can be treated using simple psychological and clinical methods, others may need referral to specialist treatment in order to overcome their fears.
New ways of engaging the avoidant phobic groups must be found, so that we can prevent the next generation from developing fears and risking their oral health by avoidance of the dentist. With 21st Century technologies to improve the patient experience, it is hoped that dental anxiety amongst the population will decrease and with concerted public education programmes around oral health and the need to visit the dentist regularly, we can begin to look forward to improved oral health for everyone.
- Öst, L. G. and Skaret, E. (2013). Cognitive Behaviour Therapy for Dental Phobia and Anxiety. Wiley-Blackwell, John Wiley & Sons.
- Gatchel, R. J., Ingersoll, B., Bowman, L., Robertson, C. M. and Walker, C. (1983). The prevalence of dental fear and avoidance: A recent survey study. Journal of American Dental Association, 107(4), 609-610.
- Davison, G. (2000). Stepped care: doing more with less? Journal of Consulting and Clinical Psychology,68, 580-585.
- Rachman, S. (1977). The conditioning theory of fear acquisition: A critical examination. Behaviour Research and Therapy, 15, 375-387.
- Seligman, M. (1971). Phobias and preparedness. Behaviour Therapy, 2, 307–320
- American Psychiatric Association (1994). Diagnostic and Statistical Manual of Mental Disorders, 4th edn. Washington DC: American Psychiatric Association.
- Armfield, J., Spencer, J., and Stewart, J. (2006). Dental fear in Australia. Who’s afraid of the dentist? Australian Dental Journal, 51, 78-85.
- Weiner, A. A. and Sheehan, D. V., (1990) Etiology of dental anxiety: psychological trauma or CNS chemical imbalance? General Dentistry, 38(1), 39-43.
- Locker, D., Liddell, A. and Shapiro, D. (1999). Diagnostic categories of dental anxiety: a population-based study. Behaviour Research and Therapy, 37(1), 25-37.
- Humphris, G.M., Morrison, T. & Lindsay, S.J.E. (1995). The modified dental anxiety scale: Validation and United Kingdom norms. Community Dental Health, 12, 143–150.
- Corah, N. L. (1969). Development of a Dental Anxiety Scale. Journal of Dental Research, 48, 596.
- Dental Fear Central, (2004-2017) www.dentalfearcentral.org/fears/dental-phobia/
- Oosterink, F. M. D., de Jong, A., Hoogstaten, A., Aartman, I. H. A. (2008). The Level of Exposure–Dental Experiences Questionnaire (LOE-DEQ): a measure of severity of exposure to distressing dental events. European Journal of Oral Science,116, 353-361
- Townend, E., Dimigen, G. and Diane F. (2000) A clinical study of child dental anxiety. Behaviour Research and Therapy, 30(1), 31-46.
- Pohjola, V., Mattila, A., Joukamaa, M. and Lahti, S. (2011). Anxiety and depressive disorders and dental fear among adults in Finland. European Journal of Oral Sciences, 119, 55-60.
- White, D. A., Tsakos, G., Pitts N. B., Fuller E., Douglas, G. V. A., Murray, J. J. and Steele, J. G. (2012) Adult Dental Health Survey 2009: Common oral health conditions and their impact on the population. British Dental Journal, 213, 567 - 572
- Heft, M. W., Meng, X., Bradley, M. M. and Lang, P. J. (2007) Gender differences in reported dental fear and fear of dental pain. Community Dentistry and Oral Epidemiology, 35, 421-428.
- Buchanan, H. and Coulson, N.S. (2007). Accessing dental anxiety online support groups: An exploratory qualitative study of motives and experiences. Patient Education and Counselling, 66, 263–269.
- Rosenhan. D. L. and Seligman, M. E. P. (1989). Abnormal Psychology. New York: W. W. Norton.
- Hakeberg, M. and Berggren, U. (1992). Prevalence of dental anxiety in an adult population in a major urban area in Sweden. Community Dentistry and Oral Epidemiology, 20, 97-101.
- Hagglin, C., Berggren, U., Hakeberg, M. and Ahlqwist, M. (1996). Dental anxiety among middle-aged and elderly women in Sweden. A study of oral state, utilisation of dental services and concomitant factors. Gerodontology, 13, 25-34.
- Hakeberg, M., Berggren, U., Carlsson, S.G. & Grandahl, H.G. (1993). Long-term effects on dental care behaviour and dental health after treatments for dental fear. Anesthesia Progress, 40(3), 72–77.
- Berggren, U. (1984). Dental Fear and Avoidance: A study of Aetiology, consequences and treatment. Goteborg University.
- Berggren, U. and Meynert, G. (1984). Dental fear and avoidance – Causes, symptoms and consequences. Journal of the American Dental Association, 109, 247-251.
- Cohen S.M., Fiske, J., and Newton, J. T. (2000) The impact of dental anxiety on daily living. British Dental Journal, 189, 385–390.
- Berggren, U. and Carlson, S. G. (1986). Qualitative and quantitative effects of treatment for dental fear and avoidance. Anesthesia Progress, 33, 9-13.
- Hakeberg, M. and Berggren, U. (1988). Changes in sick leave among Swedish dental patients after treatment for dental fear. Community Dental Health, 10, 23-29.
- Hakeberg, M. and Lundgren, J. (2014) Chapter 1: Symptoms, Clinical Characteristics and Consequences. Pgs 3-19. In Öst, L. G. and Skaret, E. (2013). Cognitive Behaviour Therapy for Dental Phobia and Anxiety. Wiley-Blackwell, John Wiley & Sons.
- Frankel, R. M. and Stein, T. (2001). Getting the most out of the clinical encounter: the four habits model. Journal of Medical Practice Management, 16(4), 184-191.
- Milgrom, P., Fiset, L., Melnick, S. and Weinstein, P. (1988). The prevalence and practice management consequences of dental fear in a major United States city. Journal of the American Dental Association, 116, 641-647.
- Beck, A. T. (1976). Cognitive Therapy and the Emotional Disorders. New York : International Universities Press.
- Berggren, U. (1986). Long term effects of two different treatments for dental fear and avoidance. Journal of Dental Research, 65, 874-876.
- Ӧst, L. G. (1989). One-session treatment for specific phobias. Behaviour Research and Therapy, 27(1), 1-7.
- Shapiro, R. (2005). EMDR Solutions: Pathways to Healing. New York. W.W. Norton.
- Doering, S., Ohlmeier, M. C., De Jongh, A., Hofmann, A., and Bisping, V. (2013). Efficacy of a trauma-focused treatment approach for dental phobia: a randomized clinical trial. European Journal of Oral Science, 121(6), 584-593.


