The unprecedented COVID-19 crisis has deeply modified the functioning of French society. French public hospital, in first line facing this epidemic, was in crisis for several years and healthcare before the COVID-19’ crisis. In this Short Communication, we describe, how, despite these difficulties, a middle-sized hospital adapted both structurally and humanly, in a very fast and totally new way. We emphasize many individual and collective skills that ensured quality care for all patients, without our hospital ever being overwhelmed. We show, with this is example, that COVID-19 epidemic is a unique, and not to be missed, opportunity for the French public hospital to reinvent itself.
Finally, the Extracellular Vesicles (EVs) secreted after the entry of these ECGS in the target cells, would perform, among other functions, that of second messengers of the viral message from abroad, defining the immune response of the receptor.
COVID-19, SARS-CoV-2, hospital, france
On January 24, 2020, the first three COVID-19 cases in Europe were diagnosed in France [1]. It was the beginning of the French epidemic. According to the national strategy implemented by the French Ministry of Solidarities and Health, the first suspected or positive patients were admitted to regional reference centers (three of these centers exist in Paris) [2]. These centers belong to Assistance Publique – Hôpitaux de Paris, the largest hospital system in Europe composed of 39 hospitals. Rapidly, these structures were overwhelmed, while the virus contaminated an exponential number of people, despite the rapid activation of a national epidemic risk control procedure [3]. In this situation, it became essential to adapt the other hospitals to the care of more and more COVID-19 patients.
Tenon hospital is a middle-sized public university-teaching hospital with 477 beds employing 3000 people. It is located in the East of Paris, in one of the poorest and densest districts, near some disadvantaged suburbs [4]. In this hospital, the first COVID-19 positive patient was diagnosed on February 26 in the Emergency Department. At that moment, the national recommendation was to transfer each confirmed COVID-19 patient to a regional reference center, in order to keep other hospitals “COVID-free”. As expected, Tenon hospital remained “COVID-free” for a very short time. In early March 2020, 33 beds for COVID-confirmed patients were opened in the Pneumology Department, and a unit of ten beds of Infectious Diseases was created in an unused area of the hospital. The renovation of this unit, which opened on March 16, took less than two weeks, proving the resilience of the structure and technical teams. This resilience was also demonstrated by the creation, ex nihilo, in two days, of a screening consultation for symptomatic hospital healthcare workers, providing up to 60 screenings a day. More than 750 healthcare workers have been screened in two months. The rapid kinetics of bed creation for COVID-confirmed patients in the hospital is shown in figure 1A. The number of these beds increased to 187 beds in only one month, thanks to the involvement of many departments (Geriatrics, Internal Medicine, and Nephrology). This adaptation to the epidemic was permitted by the cancellation of all non-essential and non-urgent hospitalizations (scheduled surgery for example) and the essential collaboration of other public and private hospitals which received 263 patients from Tenon hospital. At the peak of the crisis, 56% of hospital beds were occupied by COVID-positive or COVID-undetermined patients. Severe COVID-19 cases requiring ICU increased extremely quickly, as showed in figure 1B. In just a few days, the amount of ICU beds went from 15 to 42 beds. This was made possible in particular by the rapid conversion of eight nephrological intensive care beds into COVID-positive ICU beds. On March 28, given the total absence of free ICU beds in the hospital, six new ICU beds were opened, in one night, in unused operating rooms. This extension of ICU capacity, associated with the transfer of patients in other public or private hospitals, allowed to provide intensive care to all patients who were eligible for. Of note, two patients were transferred to other French regions by high-speed train: a technical feat. In order to avoid cross-contaminations in COVID-19 negative units, patients waiting for the PCR results were hospitalized in COVID-undetermined units, as showed in figure 1C. Another challenge during this crisis was to provide care to COVID-negative patients. Ten ICU beds for COVID-negative patients were created in the post-anesthesia care unit. As described in figure 1D, the number of beds for COVID-19 negative patients decreased, but, as the number of patients coming in for other reasons than COVID-19 decreased at the same time, the system has not been submerged.
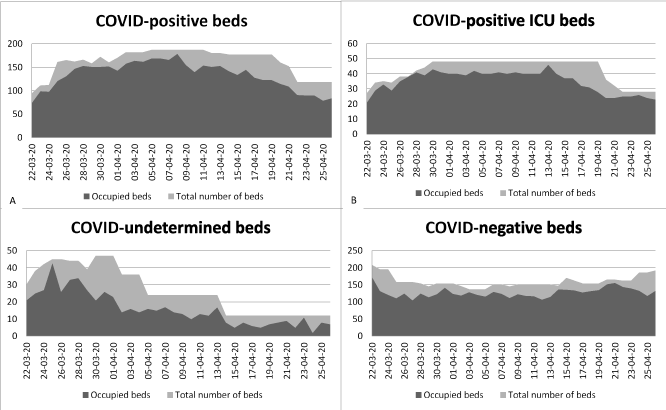
Figure 1. Evolution of the number of beds during the COVID-19 epidemic
Adapting to this constantly changing situation would have been totally impossible without the total investment of all hospital employees. This epidemic has brought to light many individual and collective skills that we, sometimes, had forgotten. Here are some examples. Communication: since the early beginning, a crisis meeting involving the administrative management and medical staff was organized, once or twice a day. Discussions were lively, disagreements expressed, but decisions were taken in a spirit of consensus. Such collaboration between these two usually antagonistic entities was unique. Adaptability: many professionals, during this crisis, performed tasks that were not usually theirs. Pathologists, Nephrologists and medical students provided hundreds of COVID-19 screening consultations. Surgeons ensured the communication with the families of hospitalized patients, who could not receive visits. Other surgeons created the “U-turn” team: each time a patient needed prone positioning; they came to help ICU teams (Figure 2). Collaboration: when the first cases occurred in France, and shortly after in our hospital, the knowledge about the disease was very scarce. Each clinician was confronted to one of the various presentations of this disease. In order to share this real-time knowledge, a specific daily multidisciplinary meeting was, organized, involving Radiologists, Pneumologists, Infectious Diseases Specialists, Intensivists, Internists, Virologists and more. This meeting allowed, especially for patients with severe forms of the infection, to receive the best care. Furthermore, in order to offer patients, the treatments evaluated in clinical trials (CORIMUNO-19 (NCT04324047) and DISCOVERY (NCT04315948) trials, among others), medical referents were identified for each trial, and provided screening, inclusion and feedback for the entire hospital. Solidarity: during this hard period, solidarity emerged as a rule, not an exception. Nurses left their unit for others, according to their experience, especially to strengthen ICU teams. What lessons can we draw, for our hospital, but probably for many other hospitals in the world? The initial amount of beds, especially in the ICU, has quickly been insufficient. From now on, the number of hospital beds to be opened or closed should be considered on the basis of needs (current, but also in case of a sanitary crisis), and not only costs. Hospital governance shared between healthcare workers and administrative management is possible, pragmatic and effective. The involvement of healthcare workers in hospital management should increase sustainably. The current COVID-19 pandemic has forced our Hospitals to rapidly adapt to new ways of working, which may have been quite different from our usual medical practice. The COVID-19 outbreak has deeply tested the adaptation capacity and the resilience of our health care system. Best-case estimates suggest that COVID-19 will stress bed capacity, equipment, and health care personnel in public hospitals in ways not previously experienced. How can health systems prepare to care for a large influx of patients with this disease in case of second wave? [5]. Because some patients will be critically ill and need scarce resources, such as extracorporeal membrane oxygenation and ventilators, hospitals must prepare now for how they will triage patients, allocate resources, and staff wards. Chopra et al. propose 4 critical points : i) to develop a strategy for patient volume and complexity;ii) protect and support heath care worker on the front lines [6], iii) Define a strategy to allocate health care resources; iiii) Develop a robust, transparent, and open communication policy.
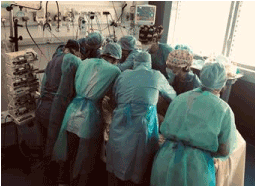
Figure 2. “U-turn” team in action
We know the world after the COVID-19 pandemic won’t and can’t be the same. Social, economic, psychological consequences will certainly be dramatic, and will force everyone to rethink its way of life. The French hospital was ill before the epidemic but survived it.
Dr Marine Nadal and Dr Ruxandra Calin have corrected English language. Hélène Piquet and Sabri Lokmane provided the access to data.
We confirm that the authors have no financial disclosures, competing interests and conflict of interest related to this study. The study has not received any financial support or other benefits from commercial sources for the work reported on in the manuscript. The manuscript represents original work of the authors and identical or similar work has not been published or submitted for publication elsewhere.
- Bernard Stoecklin S, Rolland P, Silue Y, Mailles A, Campese C, et al. (2020) First cases of coronavirus disease 2019 (COVID-19) in France: surveillance, investigations and control measures, January 2020. Euro Surveill 25: 2000094. [Crossref]
- Ministère des Solidarités et de la Santé, "Préparation au risque épidémique Covid-19"(2020; https://solidarites-sante.gouv.fr/IMG/pdf/guide_methodologique_covid-19-2.pdf).
- Mission COREB nationale, "Procédure générique standardisée de prise en charge par les médecins de première ligne des patients suspects d’infections à risque épidémique et biologique (REB) - les 10 points-clés. Recommandation professionnelle multidiscplinaire opérationnelle"(2018; https://www.coreb.infectiologie.com/UserFiles/File/procedures/20200408-procgenvalidee30mai2018-majars-esr.pdf).
- Institut National de la Statistique et des Etudes Economiques, (INSEE), "Dossier complet - Commune de Paris 20e Arrondissement" (2020; https://www.insee.fr/fr/statistiques/2011101?geo=COM-75120#consulter-sommaire).
- Chopra V, Toner E, Waldhorn R, Washer L (2020) How Should U.S. Hospitals Prepare for Coronavirus Disease 2019 (COVID-19)? Ann Intern Med 172: 621-622. [Crossref]
- Wee LE, Ying Sim JX, Conceicao EP, Aung MK, Ng IM, et al. (2020) Compliance with personal protective equipment to protect healthcare workers during COVID-19: ancillary workers count too. Clin Microbiol Infect S1198-743X: 30524-30533. [Crossref]


