Abstract
Background: Caesarean section is the most commonly performed major abdominal operation in women. Although rare, it can be complicated by cervico – isthmic adhesions and haematometra.
Case summary: We report the case of 24 year old African female gravida 1 para 1 with haematometra following obstruction of outflow tract due to prior caesarean delivery manged by dilatation and evacuation with complete return of normal menses.
Conclusion: Uterine outflow obstruction should be excluded in women presenting with amenorrhoea after caesarean section.
Key words: Cervico-isthmic adhesions, haematometra, caesarean section, amenorrhoea, case report
Abbreviations
CS – Caesarean Section
Introduction
Haematometra is a rare condition caused by obstruction of the lower female outflow genital tract resulting in an accumulation of menstrual fluid in the uterine cavity [1]. Although most commonly a result of congenital abnormalities, in older women, the obstruction is usually acquired and occurs at the level of the cervix. Haematometra can be a rare complication of caesarean section [2]. Management is usually by dilatation and evacuation of the haematometra followed by placement of intrauterine catheter for continuous drainage [3]. We present the case of a 24 year old female with haematometra following obstruction of outflow tract due to prior caesarean delivery manged by dilatation and evacuation with complete return of normal menses.
Case presentation
Madam X is a 24 year old African (Cameroonian) female gravida 1 para 1 with an amenorrhoea of 11 months since delivery who presented with cyclical lower abdominal pains of 5 months duration. The pains were cyclical, intermittent occurring every month, crampy in nature and lasting about 4 – 6 days per month. It was associated with progressive abdominal distension but no vomiting and no constipation. The past history reveals that an emergency caesarean section (CS) was done 11months ago indicated for cephalo-pelvic disproportion. The CS was complicated in the early postoperative period by postpartum endometritis and postpartum peritonitis treated by laparotomy. She admits eating well and denies weight loss. On examination she was clinically pale, vital signs normal. The abdomen was mildly distended with the presence of a mass arising out of the pelvis, tender on palpation and dull on percussion. On vaginal examination, the cervix was long, firm and closed. Digital bimanual examination revealed a uterus increased in size about that of a 14 weeks pregnancy, right adnexa mass. A Transvaginal ultrasound was done and it showed an intrauterine collection of 76cc of blood (Figure 1). Following the transvaginal ultrasound, re-vaginal examination was done with a uterine sound and the uterine sound could not pass through the cervical os. We concluded on a working diagnosis of haematometra from cervico-isthmic adhesions. Misoprostol 800µg was inserted into the vagina for dilatation and 8 hours later dilatation was done with Hager’s dilator with evacuation of 150cc of brown chocolate colour blood (fig. 2). An intrauterine Foley catheter was left in place for 48 hours for continuous drainage. Her menses resumed and flow monthly for the 3 months period of follow up.
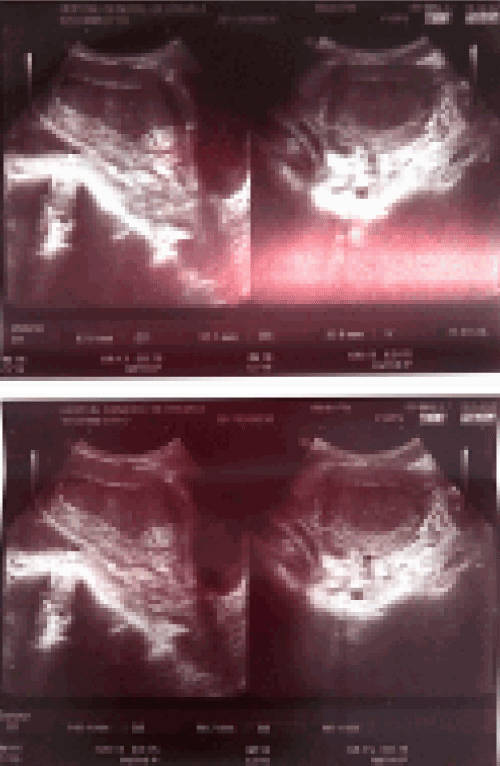
Figure 1. Transvaginal sonography showing intrauterine collection of about 76cc of blood.

Figure 2. Figure showing chocolate colour blood evacuated after dilatation of the cervix for haematometra.
Discussion
Haematometra is accumulation of blood in the uterus due to obstruction of the outflow tract. It may be congenital or acquired [4]. Congenital causes are imperforate hymen and transverse vaginal septum whereas acquired causes may include senile atrophy of endocervical canal, scarring of the isthmus by synechiae, radiation and endocervical malignancy or due to surgical procedures. Various surgical procedures associated with hematometra are dilatation and curettage, cone biopsy, endometrial ablation, cryocoagulation and electrocautery [2]. Although rare, the occurrence of cervico - isthmic adhesions and haematometra can be a complication of caesarean section. Risks factors of cervico-isthmic adhesions may include placenta praevia, placenta accreta, multiple caesarean sections or a scarred uterus and postpartum endometritis, manual removal of the placenta [2,5]. Haematometra in caesarean section could also arise as a result of inappropriate uterine closure due to stitching of anterior and posterior uterine wall creating a uterine pouch where blood could get collected over several years [6]. Risk factors identified in our indexed case included postpartum endometritis, postpartum peritonitis and probably poor surgical technique as the caesarean section was done in a district hospital by a general practitioner.
Transvaginal sonography is most useful in the evaluation of haematometra [7]. In our case transvaginal sonography showed intrauterine collection of 76cc. The goal standard in the management is hysteroscopy followed by insertion of intrauterine Foley catheter [3]. In our patient, misoprostol 800µg was inserted into the vagina for dilatation and 8 hours later dilatation was done with Hager’s dilators with evacuation of the haematometra. An intrauterine Foley catheter was left in place for 48 hours for continuous drainage.
Conclusions
2021 Copyright OAT. All rights reserv
This case is a reminder that genital tract outflow obstruction should always be excluded in women with secondary amenorrhoea.
Declarations
Ethics approval and consent to participate: Ethical approval was obtained from Douala general hospital for publication of this case report.
Consent for publication: Written informed consent was obtained from the patients for publication of this case report and any accompanying images. A copy of the written consent is available for review by the Editor-in-Chief of this journal.
Availability of data and material: The datasets (medical file of the patient) is available in Douala general hospital on reasonable request.
Competing interests
“The authors declare that they have no competing interests" in this section.
Funding
None
Author’s contributions
All authors participated in the design and editing of the manuscript, all authors approved the final version of the manuscript.
Acknowledgement
We express our sincere gratitude to all doctors, nurses and medical students who took part in the management of the patient.
References
- Noor C, Patankar S, Winter-Roach B (2012) An unusual case of hematometra in a postmenopausal woman associated with Manchester repair. J Low Genit Tract Dis 16: 162-164.
- Kaur G, Jain S, Sharma A, Vaid NB (2014) Hematometra formation- a rare complication of cesarean delivery. J Clin Diagn Res 8: OD03-04. [Crossref]
- Pabuçcu R, Atay V, Orhon E, Urman B, Ergün A (1997) Hysteroscopic treatment of intrauterine adhesions is safe and effective in the restoration of normal menstruation and fertility. Fertil Steril 68: 1141-1143. [Crossref]
- Chou B, Bohn JA, Mairs R (2016) Acute abdominal pain caused by hematometra in an adolescent female: a case report. J Med Case Rep 10: 369. [Crossref]
- Golan A, Raziel A, Pansky M, Bukovsky I (1996) Manual removal of the placenta--its role in intrauterine adhesion formation. Int J Fertil Menopausal Stud 41: 450-451. [Crossref]
- Saeed GA (2010) Case of postoperative haematometra in a 40-year-old woman. East Mediterr Heal J Rev 16: 237-239.
- Scheerer LJ, Bartolucci L (1996) Transvaginal sonography in the evaluation of hematometra. A report of two cases. J Reprod Med 41: 205-206. [Crossref]


