Abstract
Objectives: To evaluate and compare the peri-operative parameters of the “surgery first approach” against the conventional approach within a consecutive series of 25 patients who underwent bimaxillary orthognathic surgery.
Design: Case series.
Setting: A private oral maxillofacial specialist surgical facility in Hong Kong.
Patients: Patients who were treated with bimaxillary orthognathic surgery by one surgeon with the same Anaesthesiologist and in the same private Hospital in Hong Kong between June 2008 and March 2015.
Interventions: Bimaxillary orthognathic surgery performed by “surgery first approach” and conventional approach.
Main outcome measures: Estimated blood loss and operating time.
Results: Our results showed that there was no statistical difference between the conventional group and the surgery first group in perioperative parameters namely, level of surgical complexity score, estimated blood loss and operating time. The pre-surgical preparatory phase was significantly shortened by 14.6 months in the surgery first group than in the conventional approach.
Conclusions: This study confirmed similar perioperative outcome for “surgery first approach” and the conventional approach in addition to a shortened preoperative preparatory phase. All the outcome measures in this study hopefully could initiate discussion and quality research to substantiate the new paradigm shift of orthognathic surgical protocol in future.
New knowledge added by this study
- This is the first report of bimaxillary orthognathic surgery performed by the “surgery first approach” in Hong Kong.
Implications for clinical practice or policy
- The outcome of this study could initiate the local surgeons and orthodontists in considering the viability for such a new paradigm shift of orthognathic surgical protocol in future
Introduction
Traditionally, orthognathic surgery requires a variable length of time for pre-surgical orthodontic dental alignment and arch co-ordination to optimize the inter-digitation during surgery. This pre-surgical phase could last 15 to 24 months [1,2] which patients always rate it as the worst part of their treatment owing to the visible orthodontic appliance, the pain caused and the duration required [3]. The progressive deterioration of the facial aesthetic appearance resulted from orthodontic decompensation could encumber patients’ social life. Recently, medical literature reiterates the “surgery first (SF) approach” which eliminates the conventional pre-operative orthodontic treatment to expedite the whole treatment process [4].
Back in 1960s, surgeons rarely depended on orthodontic treatment to move the teeth prior to surgery. Thus, skeletal correction was the prime treatment objective as illustrated by Poulton, et al. [5] in 1963 by five cases of mandibular prognathism successfully treated with bilateral vertical osteotomy without any preoperative orthodontic treatment. Since 1970s, with refinement of pre-surgical orthodontic mechanics, orthodontic treatment has been adopted as a standard approach by most orthognathic teams [6,7]. The emphasis of comprehensive orthodontic dental alignment, incisor decompensation, tooth rotation, and arch co-ordination have to be conducted 8 to 18 months before surgery [8]. This lengthy pre-surgical orthodontic preparation poses psycho-social inconvenience to patients and compromises their oral health. In 2007, Bell commented orthognathic surgery currently remains too complex and time consuming that needs further improvement to cope with the healthcare demands [9]. The nomenclature of “surgery first approach” in orthognathic surgery was first introduced by Nagasaka, et al. [10] in 2009 to correct Class III skeletal malocclusion with mandibular setback surgery and followed by orthodontic alignment. Further elaboration of this concept in bimaxillary surgery and its workflow had been documented by Hernandez-Alfaro et al that the treatment time was significantly reduced with high satisfaction score [11].
The purpose of this article is to evaluate and compare the peri-operative parameters of the “surgery first approach” against the conventional approach within a consecutive series of 25 patients who underwent bimaxillary orthognahtic surgery. As this is the first report of bimaxillary orthognathic surgery performed by the “surgery first approach” in Hong Kong, the studied outcome hopefully could provide more evidence to support this treatment protocol for local population.
Methods
A retrospective study was conducted on 25 patients who were treated with bimaxillary surgery by one surgeon with the same Anaesthesiologist and in the same private Hospital (Hong Kong Sanatorium & Hospital) over a 7-year period (June 2008 to March 2015), amongst them eight patients (32%) were managed with a SF approach. Preoperatively, a joint consultation with the attending orthodontist was conducted to confirm, discuss and finalise the orthodontic-orthognathic treatment plan for each patient. A standardized work-up protocol which included clinical assessment, panoramic radiograph, lateral cephalometric radiographic tracing and analysis, study cast analysis and clinical photograph record were performed for all cases.
Selection of patients for the SF sequence was based on the following inclusion criteria: 1. Stable 4-pointed occlusal contacts in trial model surgery; 2. The sagittal transitional occlusion should be fully corrected without compromising the dentofacial profile and the alignment of mid-dental and facial lines; 3. Patient’s social commitment had obviated their choice of long pre-surgical orthodontic phase; 4. All patients were well informed for this novel protocol; 5. Consent of this treatment plan by the attending orthodontist experienced in orthognathic surgery.
A standard approach had been adopted for the peri-operative management of these 25 patients, including pre-operative preparation, intra-operative and post-operative care. All patients had general anaesthesia with the same protocol for induced hypotension and pain relief. Blood loss was measured in all cases with the same criteria.
In order to, evaluate the peri-operative outcomes of SF approach, a quantitative analysis of both SF and conventional group were applied. Other than the indicators of demographic data and the dentofacial deformities, some important outcome parameters, namely the level of surgical complexity (LSC), estimated blood loss (EBL), operating time (OT) were taken for statistical comparison. Furthermore, the pre-surgical preparatory time was also studied from the joint consult date to the operating date (JCOT) for comparison of the two groups.
All the data were retrieved from the computerized medical record information system, ClinicSolutionTM including all the studied peri-operative parameters in this series of 25 patients. Our aim was to compare these outcome parameters of the SF group versus the conventional group.
We first conducted Shapiro-Wilk test to check normality of data in each group. If the data are normally distributed, independent t-test was conducted to compare the means between two groups. If the data are not normally distributed, Mann-Whitney U test was conducted to compare differences between two groups. Fisher’s exact test was conducted to see if there was an association between two categorical variables (gender vs surgery first approach/conventional approach). In addition, we conducted correlation analysis to study the correlations between different pairs of peri-operative parameters and between different combinations of explanatory variables and peri-operative parameters.
All statistical analyses were conducted by using IBM Corp. Released 2011. IBM SPSS Statistics for Windows, Version 20.0. Armonk, NY: IBM Corp.
Results
The demographics and dentofacial parameters are shown in Table 1. During this 7-year period, 9 women and 16 men were managed by bimaxillary surgery. Mean age at time of surgery was 23.0 (range, 16.3-45.6) years, standard deviation (SD)=5.8 years. Amongst them, eight patients (three women and five men) were selected as SF approach. The age range at which patients received SF operation was 18.3 to 45.6 years, mean was 25.7-year-old (SD=8.8 years).
Table 1. Comparison of baseline characteristics of patients and peri-operative parameters between surgery first approach and conventional approach.
|
Overall*
(n=25) |
Surgery first*
(n=8) |
Conventional*
(n=17) |
P value |
Baseline characteristics |
Age (years) |
23.0 (5.8) |
25.7 (8.8) |
21.7 (3.3) |
0.344† |
Gender |
|
|
|
|
Female |
9 (36.0%) |
3 (37.5%) |
6 (35.3%) |
1.000‡ |
Male |
16 (64.0%) |
5 (62.5%) |
11 (64.7%) |
|
ANB (degrees) |
-2.5 (6.5) |
-1.6 (7.4) |
-2.9 (6.2) |
0.646§ |
AOB¶ (mm) |
3.3 (1.7) |
3.5 (0.7) |
3.3 (1.8) |
0.758† |
JCOT (months) |
11.8 (11.8) |
1.9 (1.4) |
16.5 (11.6) |
< 0.001† |
Peri-operative parameters |
LSC |
4.3 (0.5) |
4.3 (0.5) |
4.3 (0.6) |
0.842† |
OT** (in hours) |
6.0 (0.7) |
6.1 (0.7) |
6.0 (0.8) |
0.707§ |
EBL (in ml) |
380.0 (172.0) |
387.5 (133.0) |
376.5 (191.3) |
0.885§ |
Abbreviations: ANB = A Point-Nasion-B Point Angle value; AOB = Anterior Open Bite; JCOT = joint consult date to the operating date; LSC = level of surgical complexity; OT = operating time; EBL = estimated blood loss
* Data are shown as mean (standard deviation), or no. (%), unless stated otherwise
† Mann-Whitney U test
‡ Fisher’s exact test
§ Independent t-test
¶ Only including 12 patients (two patients of the surgery first group and 10 patients of the conventional group) who suffered from AOB deformities
** Operating time started from anesthesia induction including the ligation of surgical arch bar till extubation.
Dentofacial deformities diagnosis
Of this series of 25 patients under study, 20 patients had Class III, four had Class II and one had Class I malocclusion. Amongst these patients, 12 of them were also suffered from Anterior Open Bite (AOB), 16 of them had co-existing mandibular asymmetry and one patient had Class III cleft deformities. Therefore, the most prevalent deformity was Class III prognathic facial form (accounting for 80%) while 48% had anterior open bite.
We retrieved the lateral cephalometric data including A Point-Nasion-B Point Angle (ANB) value, AOB measurement and the presence of asymmetry to reflect the three dimensional skeletal discrepancy. The mean ANB of these 25 patients submitted for bimaxillary surgery were -2.5 degrees ranging from -12 to +11 (SD=6.5) degrees. Whilst the mean AOB was 3.3 mm, ranging from 1 to 6 (SD=1.7) mm. 16 out of these 25 patients were presented with maxillomandibular asymmetry. When we look into the main diagnosis of the SF group, two patients were skeletal Class II both with vertical maxillary excess whilst the remaining six patients were skeletal Class III deformities, with four of them presented with asymmetry deformities.
Surgical complexity
We devised a quantitative score to reflect the complexity of surgical procedures for statistical analysis as Level of Surgical Complexity (LSC): Score 1 for Genioplasty or Anterior segmental osteotomy, Score 2 for 1 or 2 pierces Le’Fort I maxillary osteotomies or Bilateral sagittal split mandibular osteotomies, Score 3 for Multiple segmental maxillary osteotomies. The definitive score will be a summation of score points according to the surgical planning. For example, for a patient submitted for Le’Fort I maxillary osteotomies and Bilateral sagittal split mandibular osteotomies, the LSC score is 4 points.
Correlation analysis
By conducting a correlation analysis, it was found that LSC was moderate positive correlated with OT (Spearman’s rank correlation coefficient(r)=0.508, P=0.009). The correlations between other pairs of peri-operative parameters and between different combinations of explanatory variables and peri-operative parameters were statistically insignificant.
In addition, separate correlation analyses were also performed for the convention group and the SF group. It was found that LSC was moderate positive correlated with OT (r=0.655, P=0.004) for the conventional group, nevertheless the correlations between LSC and OT was statistically insignificant (r=0.129, P=0.761) for the SF group. The correlations between other pairs of peri-operative parameters and between different combinations of explanatory variables and peri-operative parameters were statistically insignificant for both the conventional group and the SF group.
Spearman’s rank correlation coefficients between different pairs of peri-operative parameters and between different combinations of explanatory variables and peri-operative parameters are summarized in Table 2.
Table 2. Spearman’s rank correlation coefficients between different pairs of peri-operative parameters and between different combinations of explanatory variables and peri-operative parameters.
|
Overall*
(n=25) |
Surgery first*
(n=8) |
Conventional*
(n=17) |
Pairs of peri-operative parameters |
LSC vs OT |
0.508 |
(0.009) |
0.129 |
(0.761) |
0.655 |
(0.004) |
LSC vs EBL |
0.067 |
(0.751) |
0.260 |
(0.534) |
0.043 |
(0.869) |
OT vs EBL |
-0.182 |
(0.385) |
0.327 |
(0.429) |
-0.315 |
(0.219) |
Explanatory variables vs Peri-operative parameters |
ANB vs LSC |
-0.290 |
(0.160) |
0.190 |
(0.652) |
-0.410 |
(0.102) |
ANB vs OT |
-0.013 |
(0.950) |
0.074 |
(0.862) |
-0.031 |
(0.905) |
ANB vs EBL |
-0.099 |
(0.639) |
0.049 |
(0.908) |
-0.125 |
(0.633) |
AOB vs LSC |
-0.082 |
(0.801) |
† |
(†) |
-0.126 |
(0.729) |
AOB vs OT |
-0.009 |
(0.977) |
† |
(†) |
0.016 |
(0.965) |
AOB vs EBL |
0.024 |
(0.942) |
† |
(†) |
0.108 |
(0.767) |
Asymmetry vs LSC |
0.385 |
(0.057) |
0.447 |
(0.267) |
0.361 |
(0.154) |
Asymmetry vs OT |
-0.235 |
(0.258) |
-0.404 |
(0.321) |
-0.141 |
(0.590) |
Asymmetry vs EBL |
0.198 |
(0.344) |
-0.232 |
(0.580) |
0.328 |
(0.198) |
Abbreviations: LSC = level of surgical complexity; OT = operating time; EBL = estimated blood loss; ANB = A Point-Nasion-B Point Angle value; AOB = Anterior Open Bite
* Data are shown as Spearman’s rank correlation coefficient (P value)
† Spearman’s rank correlation coefficients and their associated P values for AOB vs LSC, AOB vs EBL and AOB vs OT were not displayed because there were only two patients in the SF group suffered from AOB deformities
Comparison of the surgery first approach and the conventional approach
The mean LSC score of this series of 25 patients was 4.3 (SD=0.5), mean OT was 6.0 (SD=0.7) hours and mean EBL was 380.0 (SD=172.0) ml. By comparison with the SF group and the conventional group in this series, the following results were found: there was no statistical difference in mean LSC (P=0.842), mean OT (P=0.707) and mean EBL (P=0.885) between the SF approach (n=8) and the conventional approach (n=17). Comparison of the peri-operative parameters between the SF approach and the conventional approach was summarized in Table 1.
Orthodontic preparation time
The pre-surgical orthodontic preparation time was recorded from the JCOT. The mean JCOT for the SF group was 1.9 (SD=1.4) months whilst for the conventional group the mean JCOT was 16.5 (SD=11.6) months. Comparatively, the JCOT was significantly shorter by 14.6 months (P<0.001) in the SF group than in the conventional approach.
Case illustration
A 20-year- old male had been referred by his attending plastic surgeon for the management of his prognathic mandible and depressed maxilla profile. He had undergone primary cleft lip palate repair surgeries in public hospital. He presented an Angle Class III malocclusion of -11mm overjet. The left buccal segment was found to have with a steep occlusal curve towards the repaired alveolar cleft with a rotated left central incisor and palatalized canine. There was minimal crowding in lower arch with a satisfactory occlusal plane (Figure 1). In view of this markedly deranged occlusion, lengthy pre-surgical orthodontic correction time was envisaged. Moreover, he requested corrective surgery as soon as possible within 3 months time so to have a more normal facial profile to commence his first-year university life. After much discussion with him and the attending orthodontist, the SF surgery first approach was adopted. A working diagnosis of Skeletal Class III due to secondary cleft lip and palate deformities resulting in A-P(anterio-posterior) maxilla hypoplasia and mandibular hyperplasia. His pre-surgical orthodontics preparation was done with mainly brackets attachment performed by the orthodontist a week before surgery. The surgical treatment was 2-pierce Le’Fort I maxillary advancement by segmentalization at the repaired alveolar cleft and bilateral sagittal split mandibular setback osteotomies. (Figure 2). The LSC was 4, EBL=400 ml and OT was 7 hours (including 45 minutes for induction of anaesthesia and pre-surgical arch bar application). His post-operative recovery was uneventful with commencement of orthodontics three weeks after operation. Clinical photos showed positive overbite and overjet (Figure 3) with a pleasing profile (Figure 4) and stable occlusion two years after surgery.
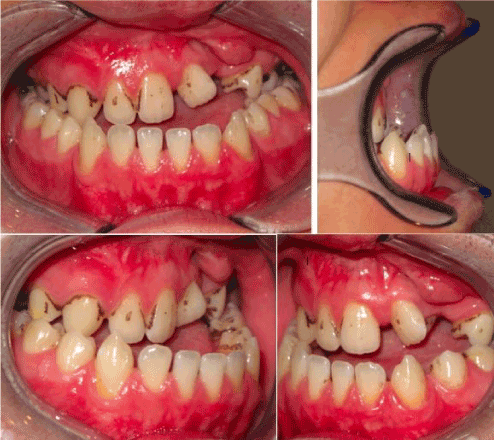
Figure 1. Pre-operative frontal and lateral occlusal views showed the extent of large A-P discrepancy of his secondary cleft dentofacial deformities.
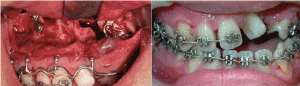
Figure 2. Intraoperative view showed 2-pierce Le’Fort I osteotomies and 3 weeks postoperative frontal occlusal view on left side.
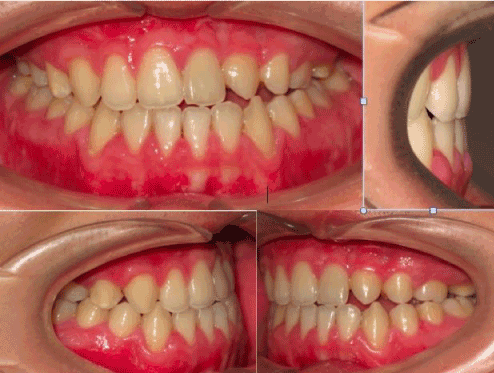
Figure 3. Two years postoperative frontal and lateral occlusal views.
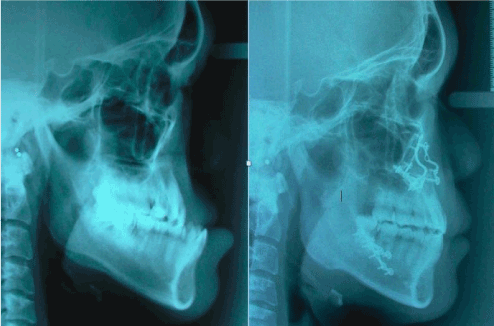
Figure 4. Pre and 2-year postoperative lateral cephalometric profile comparison.
Discussion
More and more scientific studies in recent years have proved the improvement in oral function after orthognathic surgery [12,13]. However, the well-known lengthy pre-surgical orthodontic preparation could deter the patient’s acceptance due to severe discomfort and deterioration of the oral function and the aesthetic appearance. This lengthily pre-surgical orthodontic preparation could last for nearly two years [1,2,8]. Thus, the evolving concept of “surgery first approach” is gaining popularity which alleviates the psycho-social burden albeit from the mentioned problems. In many studies, the overall treatment time was significantly reduced for such elective reconstructive procedures [11,14]. Our SF group’s JCOT was found to be 14.6 months shorter than that of the conventional group. From patient perspective, the most unfavourable pre-surgical orthodontic phase was significantly minimized in SF approach.
Since early 1970s, pre-surgical orthodontics had already been set as the golden standard [15] aiming to provide the best articulation of the opposing dentition to enhance the accuracy of rigid internal fixation and post-operative stability. Therefore, the facial profile soft tissue change will be planned according to the final occlusal scheme. The reverse concept in SF approach will definitely pose challenges to the operating surgeon in the planning phase other than highly demanded surgical precision. So as the orthodontist at the same time must be very experienced in handling the post-surgical orthodontic tooth movement in order to achieve a near perfect occlusion. Therefore, the sagittal transitional occlusion should be fully corrected without compromised the dentofacial profile and the alignment of the mid-dentofacial lines when we planned the model surgery. In our series, about one third of cases were selected as SF approach with most of them having mildly dental crowding. In fact, patients with excessive incisor decompensation or steep curve of Spee for levelling are not good candidate for SF approach. The dentofacial planning should be governed by the sagittal, frontal and transverse skeletal relationship that will finally be corrected in a central position.
Apparently, the best indication for SF approach is skeletal Class III asymmetry cases which in our series had represented half of our main dentofacial deformities diagnosis. This echoed to the commonest dentofacial deformities were Class III facial type which contributed 47% in the non-cleft patient in Hong Kong [16]. Therefore, foreseeable demand and patient acceptance of SF approach will be inevitable in local population. Moreover, soft tissue profile will be planned according to this skeletal movement with projected labiodental relationship with the account of future orthodontic tooth movement. Evidently, the lateral profile parameters such as face convexity, face height, E line, nasolabial angle, overbite, Liao, et al. [14] found no difference amongst the SF and orthodontic group. It would be worth to further investigate labiodental profile change in SF approach to evaluate the effect of such post-surgical dental decompensation.
Stable inter-ach occlusal contacts is the pre-requisite for precision of rigid internal fixation. Occasionally we might need to perform segmental osteotomies to improve the occlusal contacts and manage the transverse discrepancy as in our illustrated case. Once we could achieve a 4-pointed occlusal contacts in the model surgery planning, the orthodontist will be reassured for the detailing of post-surgical orthodontics. Some clinicians have advocated the use of temporary skeletal fixation devise and occlusal splint to improve the skeletal stability before fixation [10,11]. Of course, the attending orthodontist should be very competent in management of any residual dento-skeletal discrepancy. At last, any minor residual dento-skeletal discrepancy will depend on the competence of the attending orthodontist for final detailing in post-surgical orthodontic phase. It is thus only experienced surgical and orthodontic team could commit in such protocol.
Based on our clinical setting in private practice, patient always prefers minimum pre-surgical orthodontic duration either because of their social commitment or even socially unacceptable to have a deteriorated dentofacial profile after orthodontic decompensation. Therefore, SF approach could provide a minimal duration of orthodontic intervention than those undergoing conventional approach. The known improvement in efficiency of orthodontic forces in SF approach mainly due to two reasons: 1. Immediate resolution of hard and soft tissue imbalance prior to tooth movement [17], 2. The process of demineralization and re-mineralization consistent with the wound-healing pattern of regional acceleratory phenomenon [18-20]. Normally our patient will start orthodontic treatment three weeks after surgery which is close to the suggested postoperative orthodontic workflow by Hernandez-Alfaro, et al. [11]. We obliged to inform the pros and cons of SF approach to suitable patients before they decided to opt for this novel protocol. Other than Taiwan, Korea and Japan in Asia, even in China Yu, Mao, et al. had just published a large case series concluded that this as an ideal and valuable alternative orthognathic surgical approach [21].
Orthognathic surgery is a complex but relatively safe major procedure. With the view of shifting to SF approach, the clinician must answer the question of safety and the demand on surgical complexity to fit this protocol. In this study, we have attempted to compare the perioperative parameters of SF approach versus conventional approach to find out any differences in the surgical planning and the perioperative safety when we adopt the SF approach. Our results showed that there was no statistically significant difference between two groups with respect to OT and EBL (Table 1).
The LSC score used in this study was developed by authors’ own innovation and has not been previously validated. We have devised the LSC score to quantify the complexity of surgical procedures so as to facilitate us for statistical comparison. Tests for its validity and reliability could not be performed because of the small number of cases (i.e. only 25 patients) of this study. This is one of the weakness of the study. Hopefully, some main centers could do further validation and extrapolate it in a wider application.
There was no statistical difference in LSC score between the conventional group and the surgery first group (Table 1). Therefore, we had not aimed for a more complex surgical planning when we adopted the SF approach. Similarly, the EBL and OT showed no difference between two groups which had reassured a similar surgical outcome. One limitation in our study was that there was no data collection for the total orthodontic treatment time in view of the inconsistent postoperative follow-up of this group of patients. Nevertheless, the joint consult date to operating date JCOT was significantly shorter in the SF group by 14.6 months that had inevitably reduced the timing of pre-surgical preparatory phase.
Conclusion
To our knowledge, this is the first report of bimaxillary orthognathic surgery performed by the “surgery first approach” in Hong Kong, though the case number in this series was relatively small. All the outcome measures in this study hopefully could initiate discussion and quality research to substantiate the new paradigm shift of orthognathic surgical protocol in future.
Declaration
The authors declare no conflicts of interest. Andrew KM Kwan, the second author, prepared this article in his personal capacity for academic interest and the opinions expressed in this article are the author’s own and do not reflect the views of his affiliation.
Acknowledgement
All the clinical photos of the dental occlusion were provided by Dr. Tony CK Lee Specialist in Orthodontics for his contribution in supporting the post-surgical orthodontics for this SFA case.
References
- Luther F, Morris DO, Hart C (2003) Orthodontic preparation for orthognathic surgery: how long does it take and why? A retrospective study. Br J Oral Maxillofac Surg 41: 401-406. [Crossref]
- Diaz PM, Garcia RG, Gias LN, Aguirre-Jaime A, Pérez JS, et al. (2010) Time used for orthodontic surgical treatment of dentofacial deformities in white patients. J Oral Maxillofac Surg 68: 88-92. [Crossref]
- Nurminen L, Pietila T, Vinkka-Puhakka H (1999) Motivation for and satisfaction with orthodontic-surgical treatment: A retrospective study of 28 patients. Eur J Orthod 21: 79-87. [Crossref]
- Huang CS, Hsu SS, Chen YR (2014) Systematic review of the surgery-first approach in orthognathic surgery. Biomed J 37: 184-190. [Crossref]
- Poulton DR, Taylor RC, Ware WH (1963) Cephalometric x-ray evaluation of the vertical osteotomy correction of mandibular prognathism. Oral Surg Oral Med Oral Pathol 16: 807-820. [Crossref]
- Graber TM, Vanarsdall RL, Vig KW (2005) Orthodontics: Current principles and techniques. 4th ed. St Louis: Elsevier Mosby; 16: 1213.
- Bell WH, Proffit WR, White RP )1980) Surgical correction of dentofacial deformities. Philadelphia: Saunder; 5: 1-3.
- Proffit WR, Miguel JA (1995) The duration and sequencing of surgical-orthodontic treatment. Int J Adult Orthodon Orthognath Surg 10: 35-42. [Crossref]
- Assael LA (2008) The biggest movement: orthognathic surgery undergoes another paradigm shift. J Oral Maxillofac Surg 66: 419-420. [Crossref]
- Nagasaka H, Sugawara J, Kawamura H, Nanda R (2009) “Surgery first” skeletal Class III correction using the skeletal anchorage system. J Clin Orthod 43: 97-105. [Crossref]
- Hernandez-Alfaro F, Guijarro-Martinez R, Peiro-Guijarro MA (2014) Surgery first in orthognathic surgery: what have we learned? A comprehensive workflow based on 45 consecutive cases. J Oral Maxillofac Surg 72: 376-390. [Crossref]
- Lee S, McGrath C, Samman N (2008) Impact of orthognathic surgery on quality of life. J Oral Maxillofac Surg 66: 1194-1199. [Crossref]
- Murphy C, Kearns G, Sleeman D, Cronin M, Allen PF (2011) The clinical relevance of orthognathic surgery on quality of life. Int J Oral Maxillofac Surg 40: 926-930. [Crossref]
- Liao YF, Chiu YT, Huang CS, Ko EW, Chen YR (2010) Presurgical orthodontics versus no presurgical orthodontics: treatment outcome of surgical-orthodontic correction for skeletal Class III open bite. Plast Reconstr Surg 126: 2074-2083. [Crossref]
- Proffit WR, Fields HW, Sarver DM (2007) Contemporary orthodontics 4th ed. St Louis: Elsevier Mosby; 12: 751.
- Samman N, Tong AC, Cheung DL, Tideman H (1992) Analysis of 300 dentofacial deformities in Hong Kong. Int J Adult Orthodon Orthognath Surg 7: 181-185. [Crossref]
- Kim JH, Mahdavie NN, Evans CA (2012) Guidelines for “surgery first” orthodontic treatment, Orthodontics-basic aspects and clinical considerations; Chpt 12, Prof Bourzgui (ed.); 265-301. Available from: http://cdn.intechopen.com/pdfs-wm/31382.pdf Accessed 1 November 2017.
- Frost HM (1989) The biology of fracture healing. An overview for clinicians. Part I. Clin Orthop Relat Res 283-293. [Crossref]
- Frost HM (1989) The biology of fracture healing. An overview for clinicians. Part II. Clin Orthop Relat Res 294-309. [Crossref]
- Liou EJ, Chen PH, Wang YC, Yu CC, Huang CS, et al. (2011) Surgery-first accelerated orthognathic surgery: postoperative rapid orthodontic tooth movement. J Oral Maxillofac Surg 69: 781-785. [Crossref]
- Yu HB, Mao LX, Wang XD, Fang B, Shen SG (2015) The surgery-first approach in orthognathic surgery: a retrospective study of 50 cases. Int J Oral Maxillofac Surg 44: 1463-1467. [Crossref]




