In 1963, Levy and colleagues [1] precisely introduced the term "aortico-left ventricular tunnel" (ALVT), a rare congenital cardiac paravalvar communication extending from the lumen of aorta above sinotubular junction to the cavity of left ventricle (Figure 1). Subsequently, Hovaguimian and colleagues [2] proposed a classification based on local anatomic findings of ALVT as follows:
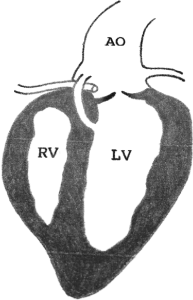
Figure 1. Aortico-left ventricular tunnel (ALVT), a very rare congenital cardiac malformation, communicates from the ascending aorta to the left ventricle which bypasses the aortic valve and rarely enters ventricular septum. AO: Aorta; RV: Right ventricle; LV: Left ventricle.
Type I: A slit like aortic orifice without valvular distortion.
Type II: A larger, oval shaped aortic orifice with an extracardiac aneurysmal tunnel.
Type III: An oval aortic orifice with a septal (intracardiac) aneurysmal tunnel.
Type IV: A combination of type II and III.
The incidence of ALVT ranges from 0.03% to 0.46% of congenital heart disease [3-5]. To date, more than 200 cases has been reported around the world since the first case reported by Levy and colleagues. The clinical presentations can range from subtle symptom, congestive heart failure, sudden death to even intrauterine death [6,7]. The variabilities of clinical presentation result from hemodynamic changes depending on the size of tunnel diameter, the severity of compression of coronary arteries or narrowing of ventricular outflow tract [8]. Retrograde diastolic blood turbulence passing through the tunnel contribute to congestive heart failure eventually [9]. The right ventricular outflow tract obstruction is owing to the right ventricular infundibulum which is close to the sinus of Valsalva suppressed by the end of aneurysmal tunnel [10]. Heart failure and aortic regurgitation often present in the first year of life, however, there are a variation of clinical presentations in different age groups [11,12]. Up to half patients might have associated cardiac anomalies, mainly composed of coronary artery anomalies and valve abnormalities [3,11,13].
The aspect of differential diagnosis, several congenital heart defects should be carefully ruled out. The septal defect such as aortopulmonary window or ventricular septal defect with aortic regurgitation, aortic sinus pathology including ruptured aneurysm or fistula, coronary artery fistula, common arterial trunk with valvular regurgitation, patent ductus arteriosus (PDA), aortic valve stenosis and regurgitation, and even the cerebral arterio-venous malformation need to be distinguished based on presenting similar clinical features [13,14].
By auscultating the heart, “to-and-fro murmur” is often heard when the tunnel exists. This abnormal heart sound could be mimicked by tetralogy of Fallot with absent pulmonary valve, coronary artery fistula or patent ductus arteriosus. Thus, a complete differential diagnosis should also be considered based on heart auscultation [14,15]
Recent years, it has been highlighted the importance of prenatal image development and advanced knowledge of ALVT placed on early diagnosis. There are some invasive and non-invasive tools for us to diagnose and locate the tunnel if ALVT is suspected [13] and nearly 80% accuracy rate of the ultrasound diagnosis has been reported [16]. The echocardiography is the convenient and cost-effective way compared with other imaging modalities and can be arranged in intrauterine life by fetal echocardiography to detect the lesion reliably after 18 weeks of gestation [17]. Combined with different techniques including color-doppler, two-dimensional (2D) or real-time three-dimensional (3D) can help physicians diagnosing and evaluating the severity of ALVT [13]. When transthoracic echocardiography window is poor, transesophageal echocardiography (TEE) could be considered [10]. TEE is demonstrated preoperatively and intraoperatively to detect the morphology of ALVT and function of valves within a single transducer in both 2D and real-time 3D techniques. The latter was regarded as an important adjunct to the standard 2DTEE examination when making decisions for management or intraoperation, and even predicting outcomes are considered [12,18]. Although the magnetic resonance angiography can provide more details about the relationships of the tunnel to adjacent cardiac and mediastinal structures, it’s not popular in clinical use despite non-invasive [13,15]. On the other hand, cardiac catheterization is considered when associated defects or coronary arterial origins cannot be well delineated by noninvasive examinations [13,19]. Nevertheless, ultrasound should it be the first choice in small infant to prevent unnecessary radiation exposure.
The etiology of ALVT is poor understanding. The potentially underlying mechanisms to elaborate the pathogenesis were proposed as follows: coronary artery anomalies, fragility of the intercommissural line, abnormalities of the distal part of bulbus cordis, early or intrauterine rupture of Valsalva sinus aneurysm, early aortic dissection similar to connective tissue disease such as Marfan syndrome, or a remnant of the fifth aortic arch [2,20]. Surgical intervention is recommended as soon as possible after diagnosis is made because of high medically-treated mortality, even in asymptomatic patients [3]. The surgical aim is not only to reduce the impact of turbulence caused by the to-and-fro blood but also to preserve the coronary and heart circulation and strengthen the aortic wall [13,21]. We found that direct suture has a higher risk of postoperative AR caused by aortic valve distortion [11]. Honjo and co-workers showed remarkable results in small infant receiving patch closure because of minimal effect on aortic valve [22]. Early surgical outcomes are good in most cases. Nevertheless, 16-60% patients have residual aortic regurgitation (AR), a major concern in the postoperative period [22]. Postoperative AR might be secondary to damaged valve, congenital valve anomalies, annuloectasia, or lack of support for the aortic annulus [3].
On long-term follow-up, several studies emphasized that significant AR and recurrent ALVT could happen [3,23] and the requirement for aortic valve replacement ranges from 0% to 50% [3]. Residual or recurrent ALVT, another long-term follow-up concern, is a well-recognized complication after surgical repair which might be caused by suture dehiscence [23,24]. Djukic and colleagues reported successful transcatheter closure of a residual aortico-left ventricular tunnel using an Amplatzer duct occluder which is a promising alternative and safe method for residual or recurrent ALVT to decrease surgical risk [9]. However, the timing and method of reoperation for these complications are difficult to decide for surgeons [23]. Recently, several investigators pointed out that the risk for the dilation of ascending aorta, even progression to ascending aorta aneurysm in adulthood [25-28]. Long-term hemodynamic burden, connective tissue disease or congenital valve abnormality might be the factor in the pathogenesis of the dilation of ascending aorta, but the etiology remains unclear nowadays [25-28]. In some cases, ascending aorta replacement was performed in order to prevent aortic rupture or dissection [25-28]. Based on the chronological sequence in the long-term outcome after repaired ALVT, regular surveillance imaging follow-up is recommended for repaired ALVT.
In summary, early diagnosis and surgical intervention are important for the patient with ALVT. While postoperative AR and recurrent ALVT are well-known for their concern, the aneurysmal formation of ascending aorta should also be kept in mind during their long-term follow-up. The appropriate timing to correct these problems is difficult to decide for surgeons because of associated cardiac anomalies and the risk of reoperation. Of key importance is that postoperative regular imaging follow-up is recommended in order to detect earlier the aforementioned complications.
References
- Levy MJ, Lillehei CW, Anderson RC, Amplatz K, Edwards JE (1963) Aortico-left ventricular tunnel. Circulation 27: 841-853.
- Hovaguimian H, Cobanoglu A, Starr A (1988) Aortico-left ventricular tunnel: a clinical review and new surgical classification. Ann Thorac Surg 45: 106-112.
- Martins JD, Sherwood MC, Mayer JE Jr, Keane JF (2004) Aortico-left ventricular tunnel: 35-year experience. J Am Coll Cardiol 44: 446-450. [Crossref]
- Li D, Yan J, Shen X, Guo S, Tao T, et al. (2009) Surgical treatment of aortico-left ventricular tunnel: a 12-year experience. Cardiology 114: 150-156. [Crossref]
- Okoroma EO, Perry LW, Scott LP III, McClenathan JE (1976) Aortico-left ventricular tunnel. clinical profile, diagnostic features and surgical considerations. J Thorac Cardiovasc Surg 71: 238-244.
- Roberts WC, Morrow AG (1965) Aortico-left ventricular tunnel. A cause of massive aortic regurgitation and of intracardiac aneurysm. Am J Med 39: 662-667.
- Sousa-Uva M, Touchot A, Fermont L, Piot D, Delezoide AL, et al. (1996) Aortico-left ventricular tunnel in fetuses and infants. Ann Thorac Surg 61: 1805-1810. [Crossref]
- Maghrabi K, Gandhi S, Harris KC (2017) Valvar aortico-ventricular tunnel: an insight into the development of the great arteries. Cardiol Young 27: 788-790.
2021 Copyright OAT. All rights reserv
- Djukic M, Djordjevic SA, Dähnert I (2017) Transcatheter closure of a residual aorto-left ventricular tunnel: report of a case with a 6-year follow-up. Cardiol Young 27: 1618-1621. [Crossref]
- Toganel R, Benedek T, Suteu C, Benedek I (2013) Aneurysmal aorto-left ventricular tunnel causing right ventricular outflow tract obstruction, associated with bicuspid aortic valve. Heart Vessels 30: 140-142.
- Chen YF, Chiu CC, Wu JR (1994) Correction of aortico-left ventricular tunnel in a small Oriental infant: a brief clinical review. J Cardiovasc Surg 35: 71-73.
- Xia H, Jiang Y, Xu Y, Tang J, Gao Y (2015) Transesophageal echocardiography for the evaluation of aorto-left ventricular tunnel in adults, with follow-ups. Echocardiography 32: 1270-1276.
- McKay R (2007) Aorto-ventricular tunnel. Orphanet J Rare Dis 2: 41. [Crossref]
- Fesslova V, Boschetto C, Brankovic J, Bonacina E (2012) Unusual aortic valve anomaly in the fetus: a case report. Fetal Diagn Ther 32: 221-224. [Crossref]
- Humes RA, Hagler DJ, Julsrud PR, Levy JM, Feldt RH, et al. (1986) Aortico-left ventricular tunnel: diagnosis based on two-dimensional echocardiography, color flow Doppler imaging, and magnetic resonance imaging. Mayo Clin Proc 61: 901-907.
- Xie M, Yin J, Lv Q, Wang J (2016) Clinical value of diagnosing aortico-left ventricular tunnel by echocardiography. Exp Ther Med 12: 3315-3319. [Crossref]
- Jone PN, Mitchell MB, Campbell DN, da Cruz EM (2014) Prenatal diagnosis and successful outcome in neonate of aorto-left ventricle tunnel. Echocardiography 31: E20-E23.
- Kakadekar AP, Sandor GG, Patterson MW, LeBlanc JG (1995) Role of transesophageal echocardiography in the management of aortic left ventricular tunnel. Pediatr Cardiol 16: 137-140.
- Sadeghpour A, Peighambari M, Dalirrooyfard M, Esmailzadeh M, Maleki M, Noohi F, Ojaghi M, Samiei N. Aorta-to-left ventricle tunnel associated with noncompaction left ventricle. J Am Soc Echocardiogr 19: e1-e5.
- Xu SS, Shi KH, Sha JM, Xie X (2015) Surgical repair of an aortico-left ventricular tunnel with acute infective endocarditis. Ann Thorac Cardiovasc Surg 21: 81-83.
- Serino W, Andrade JL, Ross D, de Leval M, Somerville J (1983) Aorto-left ventricular communication after closure late postoperative problems. Br Heart J 49: 501-506.
- Honjo O, Ishino K, Kawada M, Ohtsuki S, Akagi T, et al. (2006) Late outcome after repair of aortico-left ventricular tunnel: 10-year follow-up. Circ J 70: 939-941. [Crossref]
- Chen HM, Chang PC, Chen YF (2008) Aortic-left ventricular tunnel with late incompetence after 18-year follow-up. Thorac Cardiov Surg 56: 231-238.
- Coskun KO, Bairaktaris A, Coskun ST, El Arousy M, AminParsa M, et al. (2006) Aortico-left ventricular tunnel, an unusual congenital cardiac anomaly in adult: application of a new operative technique. ASAIO J 52: e40-e42.
- Sakurai M, Takahara Y, Takeuchi S, Mogi K (2006) Ascending aortic ventricular tunnel aneurysm repair. Jpn J Thorac Cardiovasc Surg 54: 182-184.
- Kharwar RB, Safal S, Sethi R, Narain VS, Sharma AK, et al. (2015) Aorto-left ventricular tunnel in a multianeurysmal heart. Circulation 131: e11-e14.
- Portelli Tremont JN, Kalra A, Savarese C, Lee LY (2017) Aortic root replacement in a patient following congenital aortico-left ventricular tunnel repair in childhood. J Card Surg 2017: 1-3.
- Yildirim A, Erek E, Uslu Z, Saygili A, Karaagac AT (2013) Aorto-left ventricular tunnel originating from the left coronary sinus with aortic aneurysm in an 11-year-old boy. Tex Heart Inst J 40: 91-94.

