Case Presentation
A 25-year-old male, presented to our emergency department with a one day history of a right sided abdominal pain. His medical history revealed a herniated nucleus pulposus and a deep vein thrombosis, a year before presentation. No medication was used. The differential diagnosis was cholecystitis or appendicitis.
Physical Examination Findings
The patient was afebrile, his pulse was 86 beats per minute and his blood pressure was 150/72 mm Hg, He was not tachypneic, his respiratory rate was 18 breaths per minute and his oxygen saturation was 97 % on room air.His physical examination was remarkable for abdominal tenderness at the right lower quadrant. The reminder of the physical examination was completely normal.
Diagnostic Studies
Laboratory results were unremarkable, except his C-reactive protein level of 181 mg/L. His abdominal ultrasound showed no signs of appendicitis or cholecystitis. To further exclude abdominal disorder an abdominal ct was performed showing no abdominal abnormalities but a pulmonary infiltrate Figure 1.
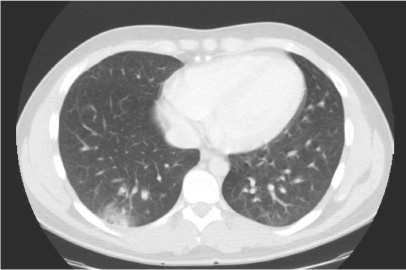
Figure 1. Abdominal CT shows a peripheral based pulmonary opacity (in the right lower lobe).
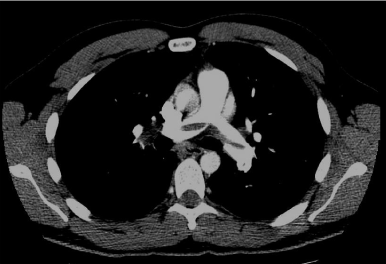
Figure 2.CTA shows a saddle pulmonary embolism.
What is the diagnosis?
What study should be considered to make the diagnosis?
Diagnosis
Saddle pulmonary embolism with a peripheral based opacity consistent with pulmonary infarction (Hampton’s hump). The next diagnostic procedure is a CT pulmonary angiography.
Discussion
Acute pulmonary embolism (PE) occurs relatively frequently (an annual rate is 1-2 per 1000 persons).It has nonspecific, variable presentation and could be the great masquerader [1-5]. The diagnosis could only be confirmed in 10-20% of suspected patients (that means that 80-90 % of suspected patients have no PE, PE was in those patients excluded after they have been evaluated,) [2].
There is no pathognomonic sign or symptom for PE and the diagnosis remains difficult. Pulmonary emboli frequently originate from lower extremity (deep vein thrombi, 80-90 %) [4] and could be clinically silent. That was described in a deep venous thrombosis study, in which 40 % of deep vein thrombi had silent accompanying pulmonary embolism (4). In symptomatic patients thoracodynia (88 %) and dyspnoea (84 %) are the most common symptoms, the rest of symptoms are less frequently reported (cough 53 %, haaemoptysis 30 %) [4].
The chest pain is usually sudden, sharp and respirophasic, that is why among others angina pectoris, myocard infarction or herpes zoster should be considerd as a differntial diagnosis. So abdominal pain is an unusual presentation of the pulmonary embolism and could be seen in 6.7% of patients with pulmonary embolism [3-5]. The precise mechanism of abdominal pain in pulmonary embolism is still unknown. It could be due to right heart strain and hepatic congestion or it could be due to diaphragmatic pleurisy after pulmonary infarction [6].
Clinical Course
We admitted this saddle pulmonary embolism patient with an abdominal pain and treated with a low-molecular-weight-heparine given subcutaneously combined with an oral anticoagulant therapy, acenocoumarol (low-molecular-weight-heparine was stopped after the apropriate target INR range has been reached).
Inspite the fact that he had a saddle pulmonary embolism, he had no signs of massive pulmonary embolism, his hemodynamic stability was the reason we did not use thrombolysis.He recovered completely within ten days and he was discharged.The patient was seen in the post-discharge clinic for three years . He had no symptoms, no signs of chronic thromboembolic pulmonary hypertension (CTEPH) or recurrent pulmonary embolism. Due to his two thrombotic events (a deep vein thrombosis a year before his pulmonary embolism), a lifelong anticoagulat therapy was adviced.
Abdominal pain could either originate from pulmonary embolism or pneumonia and it should be considered by physicians as a diagnosis in all patients with an abdominal pain when abdominal source of their symptoms could not be identified.
- Pulmonary embolism has nonspecific, variable presentation and could be the great masquerader.
- PE presenting as abdominal pain is an unusual presentation of the pulmonary embolim and could be seen in 6.7 % of patients. The precise mechanism of abdominal pain in pulmonary embolism is still unknown. It could be due to right heart strain and hepatic congestion or it could be due to diaphragmatic pleurisy after pulmonary infarction.
- It should be considered by physicians as a diagnosis in all patients with an abdominal pain when abdominal source of their symptoms could not be identified.
Acknowledgments Financial/nonfinancial disclosures
None declared.
Authorship
All authors had access to the data and played a role in writing this manuscript.
References
- Giorgi-Pierfranceschi M, Cattabiani C, Mumoli N, Dentali F (2017) Abdominal pain as pulmonary embolism presentation, usefulness of bedside ultrasound: a report of two cases. Blood Coagul Fibrinolysis 28: 107-111. [Crossref]
- van der Hulle T, Dronkers CE, Klok FA, Huisman MV (2016) Recent developments in the diagnosis and treatment of pulmonary embolism. J Intern Med 279: 16-29. [Crossref]
2021 Copyright OAT. All rights reserv
- Meyer G, Vicaut E, Danays T, Agnelli G, Becattini C, et al. (2014) Fibrinolysis for patients with intermediate-risk pulmonary embolism. N Engl J Med 370: 1402-1411. [Crossref]
- Unlüer EE, DenizbaÅŸi A (2003) A pulmonary embolism case presenting with upper abdominal and flank pain. Eur J Emerg Med 10: 135-138. [Crossref]
- Smith DC (1996) Pulmonary embolism presenting as an acute surgical abdomen. J Emerg Med 14: 715-717. [Crossref]
- Sethuraman U, Siadat M, Lepak-Hitch CA, Haritos D (2009) Pulmonary embolism presenting as acute abdomen in a child and adult. Am J Emerg Med 27: 514. [Crossref]


