Key words
Elbow; Wrist; Distal radioulnar joint; Ligamentous injury; Static instability; Salvage procedures; Sauvé-Kapandji procedure; "Quadrangular-construct" modification
Abbreviations
PA: posterior-anterior; UPV: ulnar positive variance; DRUJ: distal radioulnar joint; IOM: interosseous membrane; RUL: radioulnar ligaments; TFCC: triangular fibrocartilagenous complex; CT: computed tomography; MRI: magnetic resonance imaging; UIS: ulnocarpal impaction syndrome; USO: ulnar shortening osteotomy; ORIF: open reduction and internal fixation; UHR: ulnar head replacement; TWA: total wrist arthroplasty.
Case presentation
A 26-year-old male sustained a left wrist injury after an occupational fall from height that was diagnosed as wrist sprain and treated conservatively by a plaster splint in another institution. Eight weeks after injury, the patient could be re-employed in his original occupation as a truck driver. Six years after injury, the patient came in our institution for the first time, and reported increasing pain in his left wrist accompanied with marked restriction of his left forearm's supination and pronation leading to the non-ability to carry out his occupational job 8 weeks previously. On clinical examination, there was pronounced dorsal subluxation of the ulnar head without any given possibilities for it manual closed reduction (i.e. static instability in transverse plane) (Figure 1A). Posterior-anterior (PA) radiographs of both wrists showed no concomitant ulnar positiv variance (UPV) (i.e. no longitudinal instability) and no posttraumatic arthritic changes in the distal radioulnar joint (DRUJ), but the configuration of the ulnar styloid at the formerly injured left wrist could not be well assessed that suggested an additional rotation deformity of the ulnar head (Figure 1B). Lateral radiographs of both wrist showed marked fixed subluxation of the ulnar head in dorsal direction (i.e. static instability in transverse plane) (Figure 1C). Due to these findings, the Sauvé- Kapandji procedure, modified by creating a "quadrangular-construct", was detected by us. At the preoperative radiographs of the left elbow in both planes there were no signs of any pre-existing degenerative changes with specific regard to the radiocapitellar joint. Intraoperatively, first, the 2 cm long ulna segment was excised typically proximal to the DRUJ, then a Kirschner-wire was drilled into the ulnar head parallel to the plane of the operation table on which the left forearm was positioned at terminal range of pronation (i.e. 90°) (Figure 2A). After that, the ulnar head was rotated 90° perpendicular to the operation table's plane in dorsal direction using the formerly drilled Kirschner-wire, and so the neutral position of DRUJ could be achieved in which the arthrodesis had to be performed (Figure 2B). Then, the cartilage of both corresponding surfaces in DRUJ was excised, and the DRUJ arthrodesis in neutral position was carried out using a 3.5 mm titanium malleolar screw, and the Kirschner-wire was removed. The next step included the several years later introduced "quadrangular-construct" modification of the original Sauvé- Kapandji procedure: After decorticalization of the corresponding radius and ulna shafts proximal to the DRUJ arthrodesis and distal to resection plane of the ulna segment, the formerly excised ulna segment has been inserted transversely between both forearm bones and fixated with a second 3.5 mm titanium cortical screw through the ulna segment graft, and finally, complete restoration of rotation motion arc could be achieved (Figures 2C-D). The correctly performed surgical procedure was confirmed intraoperatively by fluoroscopy in both planes (Figure 2E). Noted that small pedicled muscle flaps of the pronator quadratus were sutured on top of both ulna stumps in order to avoid postoperative re-ossifications. Postoperatively, the left arm was immobilized in a plaster splint for 4 weeks, then the motion in elbow and wrist joint was freed, and strengthening was started 6 weeks after surgery. Twelve weeks after surgery, the patient could be re-employed completely in his original occupation as a truck driver. For this reason, the patient received an individually customized thermoplastic brace for his left forearm that did not restricts motion in elbow and wrist joint. At the 2-years follow-up, radiographs in both planes demonstrated complete union of the DRUJ arthrodesis in correct neutral position, complete osseointgration of the ulna segment graft without any signs of avascular bony resorption, and no signs of static instability of the proximal ulna stump in the absence of radioulnar impingement (Figure 3A). Supination/pronation had improved from 70°/60° to 90°/90°, and the forearm rotation arc with 180° was equal to right (Figures 3B-C). Function in Patient-rated wrist evaluation score (scale 0-100) had improved from 58 to 9. Pain at rest in visual analogue score (scale 0-10 points) had improved from 4 to 0, and under occupational load without brace from 9 to 2 and with brace to 1. The patient reported discomfort (snapping in the soft tissue around the proximal ulna stump while supination/pronation) only when not using the brace in his job. The patient also reported that he would have the same procedure again if it would be necessary.

Figure 1. (Case presentation, initial findings): (A) Clinical photograph of both wrists showing at the formerly injured left wrist static fixed subluxation of the ulnar head in dorsal direction (white arrow). (B) PA radiographs of both wrists showing right well aligned ulnar styloid (green arrow), whereas left the ulnar styloid cannot be well assessed that suggests rotation deformity of the ulnar head (red arrow). (C) Lateral radiographs of both wrists showing right correct aligned ulnar head (green line), and left static fixed subluxation of the ulnar head in dorsal direction (red line in comparison the white line). (D) PA and lateral radiographs of the left elbow showing no signs of preexisting degenerative or posttraumatic arthritic changes.
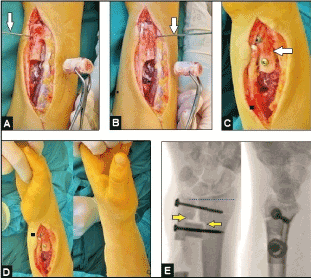
Figure 2. (Case presentation, intraoperative findings): (A) Clinical photograph showing the excised 2 cm long ulna segment proximal to the DRUJ, and the Kirschner-wire which was drilled into the ulnar head parallel to the operation table's plane (white arrow). (B) Clinical photograph demonstrating rotation of the ulnar head by the Kirschner-wire (white arrow) 90° perpendicular to the operation table's plane resulting in neutral position of DURJ in which the arthrodesis had to be performed. (C) Clinical photograph showing the radioulnar transversely positioned ulna segment (white arrow) which was fixed with a screw through it. (D) Clinical photographs demonstrating complete restoration of supination/pronation motion arc. (E) Fluoroscopy in both planes demonstrating correct "quadrangular-construct" in which the ulna segment was positioned after decorticalization of the corresponding radius and ulna shafts (yellow arrows), note that there is no UPV (transverse blue pointed line).

Figure 3. (Case presentation, 2-years follow-up): (A) PA and lateral radiographs demonstrating complete osseointgration of the ulna segment graft without any signs of avascular bony resorption, note that there is no static instability of the proximal ulna stump nor static radioulnar impingement (green oval circles), the ulnar styloid can be well assessed (green arrow) that means that there is no rotation deformity of the ulnar head and the arthrodesis was performed correctly in neutral position. (B) Preoperative clinical photographs showing marked restriction of forearm rotation. (C) Clinical photographs at the 2-years follow-up demonstrating complete restoration of forearm rotation motion arc that is with 180° equal to contralateral again.
Discussion
The synovial-lined DRUJ has evolved from the primitive pectoral fin of early fish to its current form in human wrist involving development of a distinctly separate joint, recession of the distal ulna from the ulnar carpus, and development of a distinct ulnocarpal meniscus that allows a supination-pronation motion arc of 180° [1]. It is formed by the concave but often not uniform surface (flat face, ski slope, C type, S type) of the sigmoid notch of distal radius and the semicylindrical surface of the ulnar head. Typically, in case of a hereditary (i.e. idiopathic) UPV the surface of the ulnar head is sharpened (Figures 4 and 5) which can be a mainly differential diagnosis to a posttraumatic UPV. During supination-pronation of the forearm, initiated in the proximal radioulnar joint and transferred over the interosseous membrane (IOM), the distal radius rotates around the fixed ulna in the DRUJ. The larger arc of curvature of the sigmoid notch than the ulnar head allows a translational movement. During supination the ulnar head translates 5,4 mm in volar direction from neutral position accompanied with an ulna shortening, whereas in pronation the ulnar head translates 2.8 mm in dorsal direction from neutral position accompanied with an ulna lengthening. Because of the differences in the arc of curvature of both articulating partners the bony contact surface is 60% to 80% in neutral position and its significantly decreases to 10% only at terminal ranges of rotation, and so, the bony articulation accounts for only 20% of the overall DRUJ stability. The DRUJ is mainly stabilized by soft tissues such as the IOM with it important distal oblique bundle, and the triangular fibrocartilaginous complex (TFCC) consisting of the dorsal and volar radioulnar ligaments (RUL) as primary stabilizers, and the extensor carpi ulnaris tendon sheath, the ulnolunate and ulnotriquetral ligaments, and the lunotriquetral interosseous ligament as secondary stabilizers [2-12]. Typically, on PA radiographs (i.e. positioning of the forearm in pronation) the configuration of the ulnar styloid of a normal wrist can be well assessed, whereas in case of a dorsal subluxation of the ulnar head in dorsal direction in the absence of a UPV, based on isolated disruptions of RULs, the configuration of the ulnar styloid cannot be well assessed that suggests an additional rotation component to the normal translation in dorsal or volar direction in a non-injured DRUJ, and so, a possible concomitant ulnar styloid fracture also can be overlooked primarily (Figures 1B-C, 6 and 7A-F). DRUJ instability also can be easily overlooked radiographically regarding static or dynamic instabilities; therefore, a heightened awareness of the injury is helpful [13]. It must be noted generally that comparing radiographs with the uninjured joint of the patients are likely the best investigation to assess abnormalities from normal anatomic variances in his injured or operated joint [14]. When conventional radiographs are inconclusive, computed tomography (CT) scans especially with measurement of the subluxation ratio under dynamic conditions (i.e. neutral to terminal ranges of supination and pronation) in comparison to the opposite uninjured wrist is the preferred method of choice, whereas magnetic resonance imaging (MRI) with or without combined arthrography is able for safe assessment of concomitant soft tissue injuries such as TFCC lesions or disruptions of the IOM, but it role in evaluating direct signs of DRUJ instability remains unclear [9,12,13,15-19]. For differential diagnosis in assessment of ulnar-sided wrist pain the instillation of bupivacaine in the DRUJ can be helpful (Figure 5).
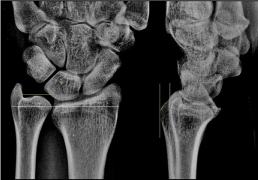
Figure 4. (Example for a hereditary UPV, 51-year-old female, left wrist): PA and lateral radiographs demonstrating longstanding hereditary UPV with 5 mm accompanied with fixed subluxation of the ulnar head (i.e. static instability) in dorsal direction (yellow transverse and longitudinal lines in relation to the white lines of normal positioning) that led to an UIS, note that the ulnar head is pathologically sharpened that also suggests that a secondary osteoarthritis in DRUJ could be responsible for the ulnar-sided wrist pain [20]. The well aligned ulnar styloid demonstrates that there is no rotation deformity (the further course is demonstrated in Figure 5).
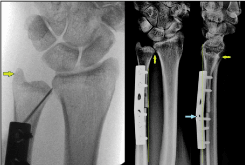
Figure 5. (Example for bupivacaine instillation in DRUJ for differential diagnosis of ulnar-sided wrist pain, same patient as in Figure 4): The diaphyseal USO was performed that resulted in sufficient ulnocarpal decompression, note that the ulnar styloid is well aligned (green arrow) in the absence joint space widening in DRUJ that means that there is no misalignment postoperatively, confirmed by postoperative radiographs in both planes. Note that the axes of the ulna are correctly aligned in both planes (longitudinal green lines), and there is no subluxation of the ulnar head whether in dorsal nor in volar direction in comparison to the preoperative findings (Figure 4). The correctly ulnar-dorsal positioned osteosynthesis plate was bent convex to the axis of the ulna shaft (blue arrow) that provides sufficient dynamic compression of the transverse osteotomy, and the positioning of the plate does not lead to an impingement with the IOM. Also note the unchanged pathologically sharpened ulnar head (yellow arrows) pointing the way for existence both of a hereditary etiology of disease and occult osteoarthritis. A osteocartilage specimen of the ulnar head was taken intraoperatively that revealed in histological examination advanced stage of osteoarthritis, hence, the diagnosis of occult osteoarthritis as preoperative suggested was confirmed. Postoperatively, the patient was not pain-free. For differential diagnosis of the persistent ulnar-sided wrist pain, the instillation of bupivacaine in DRUJ was performed under fluoroscopy. Fifteen minutes after instillation, the patient was pain-free that confirmed definitively the histological diagnosis of advanced stage of osteoarthritis. For those cases, the secondary UHR would be the treatment option of choice in the further course [20].
Acute traumatic injuries of the DRUJ are isolated TFCC injuries, purely ligamentous injuries by disruption of the RULs and generally accompanied with detachment or disruption of the TFCC (i.e. DRUJ dislocation injuries) (Figures 1A-C and 6), fracture-dislocation injuries involving the radius shaft (i.e. Galeazzi) (Figures 7A-F) accompanied with disruptions of the RULs and TFCC, fracture-dislocation injuries of the wrist (i.e. greater arc injuries) that can be accompanied with luxation in DRUJ, and the fracture of the radial head with or without its dislocation in elbow joint accompanied with proximal migration of the radius (i.e. impingement in radiocapitellar joint) based on complete disruption of the IOM and subsequent leading to DRUJ instability (i.e. additional disruptions of the stabilizing RULs and TFCC) with distal migration of the ulna (i.e. longitudinal instability) with or without its subluxation in the lateral plane (i.e. transverse instability) first described in 1946 by Curr and Coe in the absence of previous reference to similar cases in the literature, and later clearly investigated by Essex-Lopresti in 1951 [8,21-25]. The merit of Essex-Lopresti is that he has first described the mechanism as well as the approach of this injury as follows in the original: "The mechanism of injury appears to be a violent longitudinal compression force in the long axis of the radius and differs from the usual mechanism of forcible abduction at the elbow joint which is responsible for most fractures of the radial head....The crux of the problem is in the distal joint and, since the radius can be pushed down more easily than pulled down, the following lines of approach are suggested: 1) Reconstruction of the head....2) ... Alternatively, after immediate excision a prosthesis could be used temporarily in place of the radial head to hold the radius down until the distal joint and interosseous membrane had healed and become stable" [24]. Noted that the first radial head implant using a vitallium cap was placed in 1941 by Speed to prevent heterotopic ossifications after radial head resection [26].
Acute isolated DRUJ dislocation injuries are rare, and its more common occur with dislocation of the ulnar head in dorsal than in volar direction [9,27,28]. It was first described in 1777 by Desault, but at this time the physiopathology as well as a standard treatment were unknown [28]. Dislocation in dorsal direction is the result of axial loading of the wrist in extension and hyperpronation of the forearm, whereas the injury mechanism for dislocation in volar direction is axial loading of the wrist which is locked in supination combined with hypersupination of the forearm [29,30]. In contrast, the injury mechanism of Essex-Lopresti injury is axial compression loading of the forearm on the extended elbow [31]. It is important to know that both primarily isolated DRUJ dislocation and fracture-associated DRUJ dislocation (i.e. Galeazzi) can be initially misdiagnosed radiographically up to 1 month (Figures 7A-F), and additionally, only 20% of the Essex-Lopresti injury are fully recognized at time of initial presentation, and initial radiographs are often unremarkable that often results in undertreatment in the acute stage [27,31-35]. It has also been reported that in case of a radial head fracture associated with an initially misdiagnosed Essex-Lopresti injury, primarily treated by ORIF and followed secondarily (6 months later) by radial head resection due to painful degeneration of the radial head, the proximal radial migration as result of the primarily misdiagnosed Essex-Lopresti injury could only been assessed 1 month after the radial head resection [36]. In contrast to the acute traumatic DRUJ dislocation injury, the Essex-Lopresti injury is primarily associated with a longitudinal radioulnar instability only whereas (sub)luxation in the lateral plane mostly occurs secondarily [24,34-37]. However, in every instance in which an Essex-Lopresti is suggested, based on radiographic signs of a longitudinal instability in DRUJ, preexisting posttraumatic or degenerative changes which can be responsible for DRUJ instability must be clearly assessed to avoid an overtreatment (Figures 8A-B).

Figure 6. (Example for a purely ligamentous injury in the absence of UPV based on disruptions of the primary stabilizing RULs after an accidental fall from height, 24-year-old male, left wrist): The PA radiograph of the non-injured right wrist demonstrating correct positioning of the ulnar styloid (white arrow), whereas the ulnar styloid in PA radiograph of the left injured wrist several years previously cannot be well assessed that suggests that there is a pathological rotation deformity of the ulnar head (yellow arrow) accompanied with its fixed subluxation in dorsal direction (white and yellow longitudinal lines in the lateral radiograph). This patient was surgically treated by the "quadrangular-construct" modification of the Sauvé-Kapandji procedure with decorticalization of the corresponding radius and ulna shafts as well as the 32-year-old patient in our case presentation (Figures 1A-D, 2A-E and 3A-C).
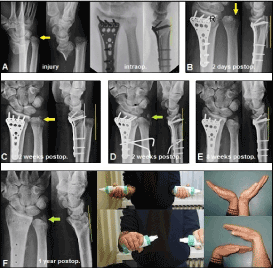
Figure 7. (Example for a right initially overlooked Galeazzi-like injury in 49-year-old male after a high-energy motorcycle accident): (A) Initial radiographic findings, and primarily treated in another hospital by ORIF using a volar distal radius plate that did not show evidence of concomitant subluxation of the ulnar head by fluoroscopy intraoperatively (green longitudial line). Note that the ulnar styloid could not be well assessed at time of injury that suggests that there is a pathological rotation deformity of the ulnar head, and so it was unclear if an additional ulnar styloid base fracture is or is not present (yellow arrow). (B) Two days later, first sign of subluxation of the ulnar head in dorsal direction (white and yellow longitudinal lines), note that the ulnar styloid could not be well assessed at this time again (yellow arrow). (C) Two weeks after primary surgery, the patient firstly came into our hospital, the right forearm was clinically fixed in pronation that was based on a complete dislocation of the ulnar head in dorsal direction radiographically (white and yellow longitudinal lines). Note that the ulnar styloid could not be well assessed at this time again as well (yellow arrow). (D) The closed reduction of the ulnar head was unsuccessful that required an open reduction by us. Intraoperatively, there was evident interposition of the extensor digiti minimi tendon into the DRUJ which was responsible for unsuccessful closed reduction. After open repositioning of the tendon, the ulnar head could be positioned uneventfully into the sigmoid notch in 90° flexion of the elbow while manual rotation of the forearm from pronation to supination. Finally, a radio-ulnar transfixation using 2 Kirschner-wires was performed in supination of the forearm, and the wrist and elbow was immobilized with a plaster splint for 6 weeks. The postoperative radiographs demonstrating correct alignment of the ulnar head in the sigmoid notch (green longitudinal line). Note that at this time the ulnar styloid firstly could be well assessed and it revealed firstly as well concomitant ulnar styloid base fracture (green arrow) that was treated conservatively by the plaster splint. (E) Six weeks after performing the second surgical procedure, both Kirschner-wires and the plaster splint were removed, and strengthening of the right upper extremity was started. Note that there was unchanged correct positioning of the ulnar head and ulnar styloid (green longitudinal line and arrow). (F) One year after primary surgery, the volar distal radius plate was removed and the patient was excellent recovered functionally in both injured joints. Radiographically, there was unchanged a stable DRUJ (green longitudinal line and arrow).

Figure 8. (Example for necessity to exclude an Essex-Lopresti injury in order to avoid overtreatment): (A) Fracture-dislocation injury of the left elbow associated with a fracture of the radial head type Mason III primarily treated by radial head replacement using a cemented bipolar cobalt-chromium prosthesis with a long stem (same patient as in Figure 10B) that led to an excellent functional outcome [65]. (B) Same patient, radiograph of her left wrist at time of injury demonstrating evident longitudinal DRUJ instability with widening of the radioulnar gap (yellow arrow) and UPV longer than 2 mm (transverse yellow pointed line) mimicing an Essex-Lopresti injury, but clinical assessment revealed a pre-existing longstanding posttraumatic UPV based on a distal forearm fracture in her childhood and followed by a longstanding distal radius physeal arrest. The patient reported a history of painless restriction of forearm rotation several years previously to the recent injury, hence, surgical revision of the DRUJ became not necessary. Note that the configuration of the ulnar styloid can be clearly assessed that means that there is no rotation deformity of the distal ulna such as found in cases of an additional instability in the transverse plane (i.e. subluxation in dorsal direction) (Figures 1A-C, 6 and 7A-F).
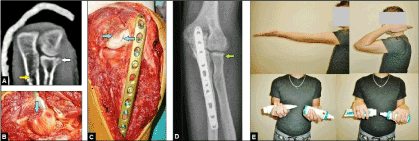
Figure 9. (Example for surgical management of a left Monteggia-like injury in a 23-year-old male after occupational fall from height): (A) CT scan after closed reduction of radiocapitellar dislocation in dorsal direction and temporarily immobilization of the elbow in a plaster splint showing the fracture of the ulna shaft at its proximal third (yellow arrow) and accompanying Mason type I fracture of radial head (white arrow). (B) Same patient intraoperatively, the osteocartilage rim fragment of radial head was removed completely (blue arrow). (C) Same patient intraoperatively, the proximal ulna shaft fracture was stabilized with the use of a 3.5 mm locked titanium plate that allowed early mobilization. Note the semicircular cartilage lesion on the dorsal aspect of capitellum (blue arrows) due to radiocapitellar dislocation in dorsal direction. (C) Same patient postoperatively, correct alignment of elbow joint without any signs of instability after removal of the osteocartilage rim fragment of radial head (green arrow). (D) Same patient at the 1-year follow-up, excellent functional outcome.
Acute traumatic TFCC injuries mostly affecting the triangular fibrocartilage are commonly treated by surgical repair both in arthroscopic and open techniques [38,39]. However, when pre-existing UPV is present then there are some difficulties in particular in rating of the diagnostic findings. An ulnocarpal impaction syndrome (UIS) is characterized by UPV longer than 2 mm that leads to a painful impingement between the ulnar head and the corresponding carpal bones in which the triangular fibrocartilage as one part of the TFCC is compressed [40]. However, UIS may also occur in the presence of neutral or minus ulna during pronation called as dynamic UIS [41,42]. Longstanding UPV is generally associated with secondary degenerative lesions of the triangular fibrocartilage due to it compression, and additionally, primary degenerative lesions of the triangular fibrocartilage with or without UPV and in the absence of any clinical symptoms are also well known but it mostly occur in elderly patients aged 60 years and older [43-47]. Hence, it cannot always be concluded that a lesion of the triangular cartilage, assessed by MRI and wrist arthroscopy, in a young patient with evident acute traumatic UPV in which the triangular cartilage is generally detached or disrupted could mainly be caused by a pre-existing non-traumatic degenerative lesion, or that a chronic ulnar-sided wrist pain in an elderly patient with evident longstanding UPV longer than 2 mm (Figures 4 and 5) is based on a lesion of the triangular cartilage that consequently would requires MRI and wrist arthroscopy. Furthermore, with the use of wrist arthroscopy it appears that rating of TFCC tears as traumatic or degenerative is very subjective, and despite high experiences by the surgeons it does not appear reliable enough to draw any useful conclusions to the origin of the lesion [48]. MRI of the wrist is indicated when the conventional radiographs are inconclusive (i.e. UPV shorter than 2 mm), and also noted that wrist arthroscopy is associated with a complication rate of 6 % respectively [49,50]. Likewise, recent evidence suggests that ulnar shortening osteotomy (USO) accompanied with wrist arthroscopy does not always lead to satisfactory outcomes in patients with long duration of symptoms, and it does not confer any additional benefit over USO alone as well [40,51-53]. Furthermore, evident UPV is considered to be contraindication for arthroscopy of the DRUJ [54].
In every instance when a fracture-dislocation injury of the wrist or elbow (i.e. Galeazzi, Monteggia, greater arc injury) is present, open reduction and internal fixation (ORIF) is absolutely required to provide joint stability and alignment, and early mobilization as well (Figures 9A-E) [21-24]. Likewise, open reduction and internal fixation (ORIF) of the radial head in case of an Essex-Lopresti injury is the essential prerequisite to obtain the length of radius and to avoid subsequent longitudinal instability of the DRUJ (i.e. UPV) [31-37,55]. In every instance as well when evident DRUJ instability after closed or open reduction of traumatic DRUJ luxation in case of a Galeazzi injury (Figures 8A-F), greater arc injury, acute isolated DRUJ dislocation injury, or Essex-Lopresti injury persists, radioulnar transfixation using Kirschner-wires is absolutely required to provide DRUJ stability as well as to give the IOM the chance for spontaneous healing [21,27,31-37,55]. If a closed DRUJ reduction is unsuccessful due to soft tissue interposition such as the extensor digiti minimi tendon or the traumatically detached TFCC, the open reduction becomes necessary (Figures 8A-F) [27]. When ORIF of the radial head in case of the Essex-Lopresti becomes not possible, resection of the radial should be avoided [56,57]. It was already stated by Essex-Lopresti in 1951 that resection of radial head is inappropriate to avoid subsequent proximal radial migration [24]. The radial head acts as a secondary valgus stabilizer and transfers up to 60% of the axial force load applied through the elbow, which is related to the amount of flexion [58,59]. After resection of the radial head, the load will be transferred to the ulnohumeral joint only and making that joint prone to subsequent osteoarthritis that could only be treated by total elbow arthroplasty, whereas radiocapitellar osteoarthritis can be treated by unicompartmental resurfacing radiocapitellar replacement which has been lesser complications and it allows higher loading for activities of daily living than total elbow arthroplasty (Figure 10C) [60,61]. It was already stated by Essex-Lopresti in 1951 as well that a radial head prosthesis would be the method of choice to obtain the length of radius [24]. In case of resection of the radial head, then the mechanical radioulnar integrity for load transmission from wrist to the elbow is uncoupled, and none other surgical salvage procedures (immediate radioulnar transfixation, silicone interposition arthroplasty, USO, ulnar head resection, Sauvé-Kapandji procedure) than a radial head prosthesis are able to provide proximal radial migration [62,63]. Currently, cobalt-chromium implants with a relative portion of 70% of all types (15% pyrocarbone / 9% titanium / 6% vitallium) are most commonly in use both utilizing monopolar (70%) and bipolar (30%) heads which can be inserted in a non-cemented as well as in a cemented (21%) manner (Figures 10A-B), and recent evidence revealed that there are no significant differences in functional outcomes between the various types in setting of prosthesis materials and polarity, and fixation techniques [64].
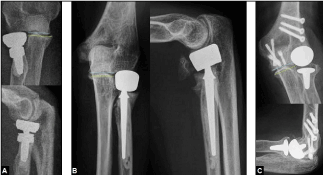
Figure 10. (Examples for various prosthetic replacements in radiocapitellar joint): (A) Cemented bipolar cobalt-chromium radial head prosthesis with a short stem for primary treatment of a highly comminuted radial head fracture. Note that there is no overstuffing (blue and green transverse lines). Cementation was done because the bone stock was poor. (B) Cemented bipolar cobalt-chromium radial head prosthesis for primary treatment of a terrible triad injury (same patient as in Figures 8A-B) [65]. Cementation was done because the bone stock was poor. Note that there is no overstuffing (blue and green transverse lines). (C) Non-cemented unicompartmental resurfacing radiocapitellar replacement utilizing an ultra-high molecular weight polyethylene - cobalt-chromium articulation for treatment of isolated posttraumatic radiocapitellar osteoarthritis [61]. Cementation should only be done when the bone stock is poor. Note that there is no overstuffing (blue and green transverse lines).
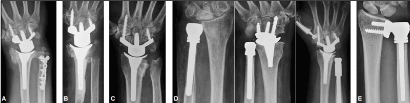
Figure 11. (Examples for salvage procedures at the DRUJ): (A) Metaphyseal USO that was primarily combined with a non-cemented TWA for primary treatment of a highly comminuted distal forearm fracture in an older patient [68]. Note that there is evident DRUJ osteoarthritis radiographically but without any clinical symptoms. Using this TWA type, the non-cemented radial press-fit insertion is the mostly preferred and performed technique when the bone stock is sufficient [103-108]. Noted, that all other third generation TWA types are intended in general for non-cemented fixation as well [109-112]. (B) Darrach procedure that was primarily combined with a cemented TWA for primary treatment of a highly comminuted distal forearm fracture in an elderly patient [20,68]. Using this TWA type, the cemented insertion should only be done when the bone stock is poor such as in this case [68,96,103]. Note that cemented fixation of the third generation TWA types becomes necessary in particular in patients with inflammatory arthritis [113]. (C) Bowers procedure that was primarily combined with a non-cemented TWA for treatment of primary osteoarthritis. The further course is demonstrated in Figure 10D right [82,97,98]. (D) Left: Non-cemented UHR utilizing a metal head with standard offset for treatment of primary osteoarthritis [20]. Middle: Non-cemented UHR utilizing a metal head with standard offset that was primarily combined with another non-cemented TWA type for treatment of posttraumatic osteoarthritis accompanied with UPV based on a longstanding distal radius physeal arrest [95,97]. Using this TWA type, the non-cemented insertion is the mostly preferred and performed technique when the bone stock is sufficient as well, and cementation should also be done only when the bone stock is poor [65,114,115]. Right: Same patient as in Figure 10C, the Bowers procedure has been failed (painful convergence instability) and a conversion to a non-cemented UHR utilizing a metal head with extended (i.e. revision) offset had to be performed, note that an additional thumb carpometacarpal total joint replacement was done due to concomitant evident rhizarthrosis [82,97,98]. (E) Non-cemented semiconstrained total DRUJ arthroplasty utilizing an ultra high molecular weight polyethylene-metal articulation for treatment of hereditary UPV with evident UIS and accompanied with a dysplastic sigmoid notch resulting in secondary painful osteoarthritis involving the sigmoid notch [20].
Salvage procedures for failed primary surgery at the DRUJ are USO, resection or hemiresection of the ulnar head, ulnar head replacement (UHR), total DRUJ arthroplasty, and the Sauvé-Kapandji procedure [66]. USO is indicated for hereditary (Figures 4 and 5) and posttraumatic evident UPV, it can be performed in a diaphyseal or a metaphyseal manner (Figures 4, 5 and 11A), it can also be an option for primary forearm shortening in case of a highly comminuted distal forearm fracture to avoid posttraumatic UPV (Figure 11A), and it is contraindicated when evident osteoarthritis in DRUJ is present [67,68]. When performing a diaphyseal USO, then the osteosynthesis plate should be positioned dorsoulnar (Figure 5) that safely prevents soft tissue complications and painful impingement with the IOM potentially leading to loss of forearm rotation [51-53,69-73]. However, despite of correct performing USO accompanied with a correctly positioned plate, patient's disability is reported to be up to 19% after surgery, and so the postoperative course remains not always predictable [53,74]. That can be based either on long duration of symptoms or occult painful osteoarthritis in DRUJ that does not always correlate with the radiographic findings which is well known from other joints such as the carpometacarpal joint of the thumb (i.e. rhizarthrosis) [40,75]. For those cases it is recommended to take a osteocartilage specimen for histological examination while performing the USO that can be helpful for evaluation of postoperative discomfort (Figures 4 and 5). When USO becomes necessary for treatment of UPV after an Essex-Lopresti injury, then reconstruction of the IOM should be performed in every instance [11,70].
Ulnar head resection (Figure 11B) was first described in 1855 by Malgaigne, and later popularized by Darrach in 1912 and 1913 [76-78]. Ulnar head hemiresection (Figure 11C) was first described in 1985 by Bowers, and 1986 modified with modeling of the ulnar stump by Watson et al. [79,80]. However, both procedures are not free of any problems. First, the third column for load transfer through the wrist is lost, and so it making the radiocarpal joint prone to subsequent degenerative changes. Second, the ulnar head serves as a cantilever, in concert with the flare of the distal radius metaphysis, to keep the radius and ulna separated and the stabilizing structures of the DRUJ under tension. When the ulnar head is partially or completely removed, the radius and ulna are uncoupled, creating an intrinsically unstable construct; most patients dramatically alter their patterns of usage and are limited by painful convergence instability or radioulnar impingement (Figures 11C-D right) [81,82]. However, it can be an option for primary treatment of highly comminuted or unstable distal forearm fractures in elderly patients to avoid posttraumatic UPV (Figure 11B) [68,83,84]. Care must be taken when using the Darrach's procedure in patients with rheumatoid arthritis, due to the natural course of the disease with progressive ulnar carpal translocation it can leads to severe complications such as migration of the lunate bone or dislocation of a total wrist arthroplasty (TWA) [85-89]. Noted that ulnar carpal translocation is also observed as a posttraumatic complication after fracture-dislocation injuries of the wrist in which the ulnar head is obtained, and, due to the unfamiliarity of this injury by treating physicians, this rare injury can mostly be investigated when comparing radiographs with the uninjured wrist were done such as described for the elbow joint as well [14,21,90].
The UHR is a clinically proven means of re-establishing mechanical contact between the distal radius and ulna to restore stability of the entire forearm [81,91,92]. The first UHR with previously performed Darrach or Sauvé-Kapandji procedures utilizing a metal head which articulates with a metal cup proximal to the sigmoid notch was introduced in 1992 by Kapandji, and followed by Herbert and van Schoonhoven using an UHR with a ceramic head they started with its use in 1995 [93,94]. UHR can be performed as primary procedure as well as a salvage procedure after a failed (hemi-) resection procedure at the distal ulna with or without an additional TWA (Figure 11D) [20,65,82,95-100]. However, a recent systematic review revealed that UHR has produced acceptable results in small numbers of patients. Whilst these short-term outcomes are encouraging, the indications should be carefully considered and there should be proper consideration of the potential for later failure [101]. Furthermore, there is a lack of information in the literature on how the patients can load their wrists with an UHR. When the sigmoid notch is involved in osteoarthritis, total DRUJ arthroplasty is recommended (Figure 11E) [20,102].
In 1921, Baldwin first described the creation of a pseudarthrosis between the shaft of the ulna and its head by excising a 2 cm long segment out of the ulna proximal to the DRUJ in order to restore forearm rotation at the level of the bony gap in case of a malunited distal radius fracture [116]. Fifteen years later in 1936, Sauvé and Kapandji were the first who inaugurated the DRUJ arthrodesis utilizing 1 screw accompanied with creation of a similar pseudarthrosis that was additionally accompanied with filling of the bony gap by the already liberated pronator quadratus in order to avoid spontaneous reossification between both ulna stumps postoperatively [117]. However, 4 years previously in 1931, Berry published his own technique similar to the later published Sauvé-Kapandji procedure that involved the DRUJ arthrodesis, but he used a bone peg instead of a screw as by Sauvé and Kapandji [118]. In contrast to the Darrach procedure, the advantage of the Sauvé-Kapandji procedure is that the ulnar head (i.e. third column) with it amount of 34% of total for complete load transmission through the wrist is preserved as well as the stability of the wrist is not altered by preservation of the RULs and ulnocarpal ligaments, and so it has been advocated for patients with high-demand claims in their activities of daily living who sustained posttraumatic disorders [119-124]. Additionally, this procedure can also be an option for primary shortening of the forearm in elderly patients with severely comminuted distal radius fractures in order to avoid posttraumatic UPV [125,126]. Essential prerequisite for preservation of the ligamentous wrist stability is that the DRUJ arthrodesis is strictly to be done in its neutral position to obtain the anatomically predetermined alignment of these stabilizing ligaments, and additionally, to avoid postoperative UPV (Figures 2A-E and 3A). However, there are mainly 2 disadvantages. First, lost of the pronator function for the forearm and wrist when using the original Sauvé-Kapandji procedure (i.e. liberation of the pronator teres) can potentially leads to decreased pronation strength [127,128]. To prevent the function of the pronator teres, it is recommended to use only small pedicled muscle flaps of the pronator teres sutured on top of both ulna stumps, such as in our presented patient's case, instead of filling of the gap with the overall liberated pronator teres such as originally described by Sauvé and Kapandji in order to avoid spontaneous reossification postoperatively and potentially resulting in revision surgery [129,130]. Second, the load transmission from the wrist to the humerus takes place exclusively only by the radius over the radiocapitellar joint alone. For development of degenerative or posttraumatic changes in the elbow, Goodfellow and Bullough first described in 1967 that the articular cartilage with ageing in radiocapitellar joint is much more vulnerable than in ulnohumeral joint, and it can be caused by the specific geometry of elbow joint which is anatomically predetermined for load transmission [131]. When a Sauvé-Kapandji procedure was done, then the load transmission in elbow joint over the radial head with its normal amount of 60% in healthy subjects inevitably increases up to 100%, and additionally to the anatomically predetermined higher vulnerability for primary degenerative changes in radiocapitellar than in ulnohumeral joint, making the radiocapitellar joint in particular prone for degenerative changes postoperatively. That means that preexisting degenerative changes in this joint are to be considered as contraindication for the Sauvé-Kapandji procedure, and in every instance when this procedure is detected, degenerative changes in radiocapitellar joint should be excluded radiographically before surgery (Figure 1D). The published outcomes are uniformly good or excellent. Complete restoration of supination-pronation motion arc compared to the opposite forearm is achieved with relative portions ranging from 86% to 100% of all patients, mean supination and pronation improved from 55° and 43° (preop.) to 90°/90° (postop.), only 5% of patients stated subjectively that their outcomes had worsened, 73% to 100% of them reported none or mild pain only, and poor outcome in single cases was associated with non-union or UPV postoperatively [123,132-134]. Calcifications at the ulna osteotomy site were observed in 4 of total 70 patients (5.7%) that was in 3 of whom associated with a simultaneously performed distal radial osteotomy respectively, and 2 of whom required excision of the calcifications because it caused restriction of forearm rotation [122]. Noted that radioulnar synostoses around the wrist are also observed in single cases in patients receiving TWA with or without an additional UHR, and Dohn et al. reported on a patient with a posttraumatic/postoperative radioulnar synostosis of the DRUJ after plate osteosynthesis of distal radius fracture that was surgical treated by excision of a bony segment in the distal third of the ulna shaft similar to the techniques by Baldwin, Berry, and Sauvé-Kapandji [96,104,108,135]. The main problem after the Sauvé-Kapandji procedure can be development of radioulnar instability potentially leading to a radioulnar impingement (i.e. static convergence instability) that is well known from the Darrach procedure, or impingement between the ulnar stump and the surrounding soft tissue that is been reported by the patients as painful snapping while rotation of their forearms (i.e. dynamic divergence instability). To avoid radioulnar instability, it is recommended that the shortening of the ulna stump should not exceed 35 mm proximal to the DRUJ [136]. When postoperative dynamic radioulnar instability occurs, then an individually customized thermoplastic functional forearm brace, formerly introduced by Sarmiento et al. for the non-operative treatment of forearm fractures, is able to reduce postoperative discomfort such as in our presented patient's case [137,138].
Another problem with the original procedure by Sauvé L and Kapandji M utilizing only 1 screw for arthrodesis can be instability followed by non-union and failure of the arthodesis by consecutive fracture of the screw [134]. Hence, it has been recommended in 1986 by Kapandji IA to insert an additional second screw at time of primary surgery to improve stability [139]. Gupta et al. recently published in 2017 a PubMed indexed article (PMID: 28216758) in which the use of the "quadrangular-construct" modification of the original Sauvé-Kapandji procedure (20 patients evaluated at an average follow-up of 34,55 months), that involves an additional radioulnar transverse interposition of the excised ulna segment proximal to DRUJ arthrodesis in which a second fixation screw is inserted through the transverse positioned ulna graft, is also recommended in order to improve stability, and the authors stated as follows in original: "Despite many modifications described in literature for S-K procedure, there is no data supporting one technique over other. We, in our new modification of S-K procedure, describe for the first time the combination of use of resected ulna as interposition graft to form a stable "Quadrangular-construct" at wrist joint along with the stabilization of proximal ulnar stump with pronator quadratus muscle." [140]. That is not true. To our knowledge, the use of the excised ulna segment as radioulnar interposition graft fixated by a second transverse screw through the graft was quite substantially earlier described in 1993 by Pechlaner and Sailer from Austria, and they reported on a case series with 72 patients started with surgery in 1984 and evaluated at an average follow-up of 42 months [129,141]. There is only one modification by Gupta et al., the ulna graft in the formerly described technique by Pechlaner und Sailer is interpositioned after decorticalization of the corresponding distal radius und ulna shafts (i.e. cortico-cancellous contact areas) such as demonstrated with our 2 patients (Figures 2A-E, 3A and 6) in order to improve its osseointegration, whereas the ulna graft in the modified technique by Gupta et al. is interpositioned without decorticalization (i.e. cortico-cortical contact areas). The aim of creating cortico-cancellous contact areas by bony decorticalization is early cancellous bone ingrowth into the intramedullary space which has proven to be useful for ankle arthrodesis in the fibula-to-tibia/talus manner as well [65]. However, with both techniques there were no non-unions, no fractures of the fixation screws, and avascular bone graft resorption could not be observed as well in both studies. Noted that the publication of Pechlaner and Sailer from 1993 was not cited in the recent article by Gupta et al., and further studies with a larger number of patients evaluate in long-term follow-up's are needed to validate this concept.
When all other salvage procedures at the distal ulna (i.e. DRUJ) have been failed, then the "one-bone forearm" surgery is the "last exit" [66,142,143]. This procedure means that both the distal and middle third of ulna are excised and follows by a fusion between the proximal ulna stump and the radius to obtain stability of the forearm for load transmission, but it does no more allow forearm rotation. It can also be an option for primary surgical treatment of severely destroyed open forearm injuries when the ulna is bony unreconstructable, however, this procedure is not free of any complications such as non-union in up to 32% of cases and impingement of the proximal radius on bone or surrounding soft tissue in up to 40% of cases requiring revision surgery [145,146]. In general, it is recommended to perform the radioulnar arthrodesis in neutral position of the overall forearm, but the recommendations varying from 10° pronation to 45° supination [143-149]. However, arthrodeses in supination confers better activities toward to the body, whereas arthrodeses in pronation makes activities away from the body easier [150].
Declarations
The authors declare that they have none conflict of interests concerning this article.
Acknowledgements
None.
References
- Louis DS, Jebson PJ (1998) The evolution of the distal radio-ulnar joint. Hand Clin 14: 155-159. [Crossref]
- Ekenstam F, Hagert CG (1985) Anatomical studies on the geometry and stability of the distal radio ulnar joint. Scand J Plast Reconstr Surg 19: 17-25. [Crossref]
- Ekenstam F (1998) Osseous anatomy and articular relationships about the distal ulna. Hand Clin 14: 161-164. [Crossref]
- Palmer AK, Werner FW (1981) The triangular fibrocartilage complex of the wrist--anatomy and function. J Hand Surg Am 6: 153-162. [Crossref]
5. Pirela-Cruz MA, Goll SR, Klug M, Windler D (1991) Stress computed tomography analysis of the distal radioulnar joint: a diagnostic tool for determining translational motion. J Hand Surg Am 16: 75-82.
- Tolat AR, Stanley JK, Trail IA (1996) A cadaveric study of the anatomy and stability of the distal radioulnar joint in the coronal and transverse planes. J Hand Surg Br 21: 587-594. [Crossref]
- Szabo RM (2007) Distal radioulnar instability. Instr Course Lect 56: 79-89. [Crossref]
- Thomas BP, Sreekanth R (2012) Distal radioulnar joint injuries. Indian J Orthop 46: 493-504. [Crossref]
9. Squires JH, England E, Mehta K, Wissmann RD (2014) The role of imaging in diagnosing diseases of the distal radioulnar joint, triangular fibrocartilage complex, and distal ulna. AJR Am J Roentgenol 203: 146-153.
10. Trehan SK, Orbay JL, Wolfe SW (2015) Coronal shift of distal radius fractures: influence of the distal interosseous membrane on distal radioulnar joint instability. J Hand Surg Am 40: 159-162.
11. Werner FW, LeVasseur MR, Harley BJ, Anderson A (2017) Role of the Interosseous Membrane in Preventing Distal Radioulnar Gapping. J Wrist Surg 6: 97-101. [Crossref]
12. Kim YH, Gong HS, Park JW, Yang HK, Kim K, Baek GH (2017) Magnetic resonance imaging evaluation of the distal oblique bundle in the distal interosseous membrane of the forearm. BMC Musculoskelet Disord 18: 47.
13. Wijffels M, Brink P, Schipper I (2012) Clinical and non-clinical aspects of distal radioulnar joint instability. Open Orthop J 6: 204-210. [Crossref]
14. Rowland AS, Athwal GS, MacDermid JC, King GJ (2007) Lateral ulnohumeral joint space widening is not diagnostic of radial head arthroplasty overstuffing. J Hand Surg Am 32: 637-641. [Crossref]
16. van den Borne MPJ, van't Hoft BWL, Prins HJ, Vincken KL, Schuurman AH, Castelein RM (2007) The distal radio-ulnar joint: Persisting deformity in well reduced distal radius fractures in an active population. Injury Extra 38: 377-383.
17. Mino DE, Palmer AK, Levinsohn EM (1985) Radiography and computerized tomography in the diagnosis of incongruity of the distal radio-ulnar joint. A prospective study. J Bone Joint Surg Am 67: 247-252. [Crossref]
18. Wechsler RJ, Wehbe MA, Rifkin MD, Edeiken J, Branch HM (1987) Computed tomography diagnosis of distal radioulnar subluxation. Skeletal Radiol 16: 1-5.
19. Anderson ML, Skinner JA, Felmlee JP, Berger RA, Amrami KK (2008) Diagnostic comparison of 1.5 Tesla and 3.0 Tesla preoperative MRI of the wrist in patients with ulnar-sided wrist pain. J Hand Surg Am 33: 1153-1159. [Crossref]
20. Schmidt I, Nennstiel I, Muradyan M, Kaisidis A, Großmann D (2017) The rare injury of a closed digital extensor tendon avulsion of the third finger at its musculotendinous junction: Case presentation and brief overview of literature with regard to general, specific and practicable aspects to extensor tendon surgery involving tendon transfer procedures. Trauma Emerg Care 2: doi: 10.15761/TEC.1000155
21. Schmidt I (2017): Posttraumatic ulnar carpal translocation type I accompanied with disruption of the lunotriquetral ligament caused by a severe radiocarpal fracture-dislocation injury type II accompanied with complete luxation of the distal radioulnar joint. What are the salvage options with its special features in indication when patients develop posttraumatic painful wrist joint osteoarthritis? Trauma Emerg Care 2: doi: 10.15761/TEC.1000138
22. Mikić ZD (1975) Galeazzi fracture-dislocations. J Bone Joint Surg Am 57: 1071-1081. [Crossref]
23. Eberl R, Singer G, Schalamon J, Petnehazy T, Hoellwarth (2008) Galeazzi lesions in children and adolescents: treatment and outcome. Clin Orthop Relat Res 466: 1705-1709. [Crossref]
24. Essex-Lopresti P (1951) Fractures of the radial head with distal radio-ulnar dislocation; report of two cases. J Bone Joint Surg Br 33B: 244-247. [Crossref]
25. McGlinn EP, Sebastin SJ, Chung KC (2013) A historical perspective on the Essex-Lopresti injury. J Hand Surg Am 38: 1599-1606. [Crossref]
26. Speed K (1941) Ferrule caps for the head of the radius. Surg Gynecol Obstet 73: 845-850.
27. Zannou RS, Rezzouk J, Ruijs ACJ (2015) Non-reducible palmar dislocation of the distal radioulnar joint. Cas Rep Plast Surg Hand Surg Early Online: 1-3, DOI: 10.3109/23320885.2015.1026348.
28. Caranfil R (2000) Isolated traumatic luxation of the distal radio-ulnar joint. A case report. Acta Orthop Belg 66: 517-520. [Crossref]
29. Kihara H, Short WH, Werner FW, Fortino MD, Palmer AK (1995) The stabilizing mechanism of the distal radioulnar joint during pronation and supination. J Hand Surg Am 20: 930-936. [Crossref]
30. Tsai PC, Paksima N (2009) The distal radioulnar joint. Bull NYU Hosp Jt Dis 67: 90-96. [Crossref]
31. Matson AD, Ruch DS (2016) Management of the Essex-Lopresti injury. J Wrist Surg 5: 172-178. [Crossref]
32. Helmerhorst GT, Ring D (2009) Subtle Essex-Lopresti lesions: report of 2 cases. J Hand Surg Am 34: 436-438. [Crossref]
33. Rodriguez-Martin J, Pretell-Mazzini J, Vidal-Bujanda C (2010) Unusual pattern of Essex-Lopresti injury with negative plain radiographs of the wrist: a case report and literature review. Hand Surg 15: 41-45.
34. Trousdale RT, Amadio PC, Cooney WP, Morrey BF (1992) Radio-ulnar dissociation: A review of twenty cases. J Bone Joint Surg Am 74: 1486-1497. [Crossref]
35. Hutchinson F, Faber KJ, Gan BS (2006) The Essex-Lopresti injury: More than just a pain in the wrist. Can J Plast Surg 14: 215-218. [Crossref]
36. Thomason K, Burkhart KJ, Wegmann K, Müller LP (2013) The sequelae of a missed Essex-Lopresti lesion. Strategies Trauma Limb Reconstr 8: 57-61. [Crossref]
37. Stabile KJ, Pfaeffle HJ, Tomaino MM (2002) The Essex-Lopresti fracture-dislocations factors in early management and salvage alternatives. Hand Clin 18: 195-204. [Crossref]
38. Nakamura T, Sato K, Okazaki M, Toyama Y, Ikegami H (2011) Repair of foveal detachment of the triangular fibrocartilage complex: open and arthroscopic transosseous techniques. Hand Clin 27: 281-290.
39. Moritomo H (2015) Open repair of the triangular fibrocartilage complex from palmar aspect. J Wrist Surg 4: 2-8. [Crossref]
40. Iwasaki N, Ishikawa J, Kato H, Minami A (2007) Factors affecting results of ulnar shortening for ulnar impaction syndrome. Clin Orthop Relat Res 465: 215-219.
41. Tomaino MM (1998) Ulnar impaction syndrome in the ulnar negative and neutral wrist. Diagnosis and pathoanatomy. J Hand Surg Br 23: 754-757. [Crossref]
42. de Novaes França Bisneto E (2017) Dynamic ulnar impaction syndrome in tennis players: report of two cases. Rev Bras Ortop 52: 621-624. [Crossref]
43. Chan JJ, Teunis T, Ring D (2014) Prevalence of triangular fibrocartilage complex abnormalities regardless of symptoms rise with age: systematic review and pooled analysis. Clin Orthop Relat Res 472: 3987-3994.
44. Yoshioka H, Tanaka T, Ueno T, Carrino JA, Winalski CS, Aliabadi P, Lang P, Weissman BN (2007) Study of ulnar variance with high-resolution MRI: correlation with triangular fibrocartilage complex and cartilage of ulnar side of wrist. J Magn Reson Imaging 26: 714-719.
45. Burns JE, Tanaka T, Ueno T, Nakamura T, Yoshioka H (2011) Pitfalls that may mimic injuries of the triangular fibrocartilage and proximal intrinsic wrist ligaments at MR imaging. Radiographics 31: 63-78.
46. Fairag R, Alshareef H, Alharbi A, Alhajjaji B, Khashoggi K, Hamdi H (2017) Prevalence of Triangular Fibrocartilage Complex Abnormalities among Asymptomatic Young Individuals Using Magnetic Resonance Imaging in A Tertiary Center in Saudi Arabia: A Cross-Sectional Study. Med Case Rep 3: 18.
47. Mikić ZD (1978) Age changes in the triangular fibrocartilage of the wrist joint. J Anat 126: 367-384. [Crossref]
48. Löw S, Erne H, Pillukat T, Mühldorfer-Fodor M, Unglaub F, Spies CK (2017) Diagnosing central lesions of the triangular fibrocartilage as traumatic or degenerative: a review of clinical accuracy. J Hand Surg Eur Vol 42: 357-362. [Crossref]
49. Jens S, Luijkx T, Smithuis FF, Maas M (2017) Diagnostic modalities for the distal radioulnar joint. J Hand Surg Eur Vol 42: 395-404.
50. Leclercq C, Mathoulin C; Members of EWAS (2016) Complications of Wrist Arthroscopy: A Multicenter Study Based on 10,107 Arthroscopies. J Wrist Surg 5: 320-326. [Crossref]
51. Kim BS, Song HS (2011) A comparison of ulnar shortening osteotomy alone versus combined arthroscopic triangular fibrocartilage complex debridement and ulnar shortening osteotomy for ulnar impaction syndrome. Clin Orthop Surg 3: 184-190.
52. Baek GH, Lee HJ, Gong HS, Rhee SH, Kim J, Kim KW, Kong BY, Oh WS (2011) Long-term outcomes of ulnar shortening osteotomy for idiopathic ulnar impaction syndrome: at least 5-years follow-up. Clin Orthop Surg 295-301.
54. Pillukat T, Fuhrmann R, Windolf J, van Schoonhoven J (2014) Arthroscopy of the distal radioulnar joint. Oper Orthop Traumatol 26: 547-555. [Crossref]
55. Jungbluth P, Frangen TM, Arens S, Muhr G, Kälicke T (2006) The undiagnosed Essex-Lopresti injury. J Bone Joint Surg Am 88: 1629-1633. [Crossref]
56. Chammas M (2014) Post-traumatic osteoarthritis of the elbow. Orthop Traumatol Surg Res 100 (1 Suppl): S15-24. [Crossref]
57. Hilgersom NFJ, Eygendaal D, van den Bekerom MPJ (2017) Disadvantages of having a shortening of the proximal radius. Knee Surg Sports Traumatol Arthrosc doi: 10.1007/s00167-017-4599-2. [Epub ahead of print] [Crossref]
58. Halls AA, Travill A (1964) Transmission of pressures across the elbow joint. Anat Rec 150: 243-247. [Crossref]
59. Morrey BF, An KN, Stormont TJ (1988) Force transmission through the radial head. J Bone Joint Surg Am 70: 250-256. [Crossref]
60. Hilgersom NFJ, Eygendaal D, van den Bekerom MPJ (2017) Is radial head resection the first choice treatment of comminuted radial head fractures without associated instability? Injury 48: 560-561.
61. Schmidt I (2017): A Complicated Course of a Coronal Shear Fracture Type IV of the Distal Part of Humerus Resulting in Resurfacing Radiocapitellar Joint Replacement. Open Orthop J. 11: 248-254.
62. Sowa DT, Hotchkiss RN, Weiland AJ (1995) Symptomatic proximal translation of the radius following radial head resection. Clin Orthop Relat Res 317: 106-113.
63. Bonnevialle N (2016) Radial head replacement in adults with recent fractures. Orthop Traumatol Surg Res 102(1 Suppl): S69-79. [Crossref]
65. Schmidt I (2017) Necessity of secondary Syme amputation of the foot after severely destroyed hindfoot injury due to suicidal jump from height in a psychiatric patient: Case presentation and brief review of literature. Trauma Emerg Care 2: doi: 10.15761/TEC.1000153
66. Yeo CJ, Morse LP, Krishnan J, Bain GI (2016) Salvage Procedures for Distal Radioulnar Joint Complications. J Hand Surg Asian Pac Vol 21: 173-186.
67. Khouri JS, Hammert WC (2014) Distal metaphyseal ulnar shortening osteotomy: technique, pearls, and outcomes. J Wrist Surg 3: 175-180. [Crossref]
68. Schmidt I (2015) Can Total Wrist Arthroplasty Be an Option for Treatment of Highly Comminuted Distal Radius Fracture in Selected Patients? Preliminary Experience with Two Cases. Case Rep Orthop 2015:380935. doi: 10.1155/2015/380935. Epub 2015 Sep 29.
69. Hazel A, Nemeth N, Bindra R (2015) Anatomic Considerations for Plating of the Distal Ulna. J Wrist Surg 4: 188-193. [Crossref]
70. Gaspar MP, Kearns KA, Culp RW, Osterman AL, Kane PM (2017) Single- versus double-bundle suture button reconstruction of the forearm interosseous membrane for the chronic Essex-Lopresti lesion. Eur J Orthop Surg Traumatol doi: 10.1007/s00590-017-2051-4. [Epub ahead of print]
71. Henry M (2009) Subcapital ulnar shortening osteotomy. J Hand Microsurg 1: 103-107. [Crossref]
72. Kamal RN, Leversedge FJ (2014) Ulnar shortening osteotomy for distal radius malunion. J Wrist Surg 3: 181-186. [Crossref]
73. Das De S, Johnsen PH, Wolfe SW (2015) Soft tissue complications of dorsal versus volar plating for ulnar shortening osteotomy. J Hand Surg Am 40: 928-933. [Crossref]
74. Hollevoet N, Declerq J, Vanhove W, Benis S (2016) Outcome of Ulnar Shorting Osteotomy. Hand (NY) 11 (1 Suppl): S124-S125.
75. Larsen SK, Østergaard AM, Hansen TB (2015) The influence of subluxation on the severity of symptoms, disability, and the results of operative treatment in TMC osteoarthritis with total joint arthroplasty. Hand (NY) 10: 593-597.
76. Malgaigne JF (1855) Traité des fractures et des luxations. Vol 2. Paris: JB Braillière.
77. Darrach W (1912) Anterior dislocation of the head of the ulna. Ann Surg 56: 802-803.
78. Darrach W (1913) Partial excision of lower shaft of the ulna for deformity following Colles's fracture. Ann Surg 57: 764-765. [Crossref]
79. Bowers WH (1985) Distal radioulnar joint arthroplasty: the hemiresection-interposition technique. J Hand Surg Am 10: 169-178. [Crossref]
80. Watson HK, Ryu JY, Burgess RC (1986) Matched distal ulnar resection. J Hand Surg Am 11: 812-817. [Crossref]
81. Berger RA (2013) Implant arthroplasty for treatment of ulnar head resection-related instability. Hand Clin 29: 103-111. [Crossref]
82. Schmidt I (2015) Primary combined replacements using the Maestro total wrist and uHead ulnar head implants. J Hand Surg Eur Vol 40: 754-755.
83. Ruchelsman DE, Raskin KB, Rettig ME (2009) Outcome following acute primary distal ulna resection for comminuted distal ulna fractures at the time of operative fixation of unstable fractures of the distal radius. Hand (NY) 4: 391-396.
84. Yoneda H, Watanabe K (2014) Primary excision of the ulnar head for fractures of the distal ulna associated with fractures of the distal radius in severe osteoporotic patients. J Hand Surg Eur Vol 39: 293-299. [Crossref]
85. De Smet L (2006) The distal radioulnar joint in rheumatoid arthritis. Acta Orthop Belg 72: 381-386. [Crossref]
86. Herren DB, Simmen BR (2002) Limited and complete fusion of the rheumatoid wrist. J Am Soc Surg Hand 2: 21-32.
87. de Roeck NJ, Packer GJ (2003) Lunate migration following Darrach's procedure: a case report. J Orthop Surg (Hong Kong) 11: 213-216. [Crossref]
88. Radmer S, Andresen R, Sparmann M (2003) Total wrist arthroplasty in patients with rheumatoid arthritis. J Hand Surg Am 28: 789-794. [Crossref]
89. Halim A, Weiss AC (2017) Total Wrist Arthroplasty. J Hand Surg Am 42: 198-209. [Crossref]
90. Schmidt I (2017) Does Total Wrist Arthroplasty for Treatment of Posttraumatic Wrist Joint Osteoarthritis in Young Patients Always Lead to Restriction of High-demand Activities of Daily Living? Case Report and Brief Review of Recent Literature. Open Orthop J 11: 439-446.
91. Kakar S, Swann RP, Perry KI, Wood-Wentz CM, Shin AY, Moran SL (2012) Functional and radiographic outcomes following distal ulna implant arthroplasty. J Hand Surg Am 37: 1364-71. [Crossref]
92. van Schoonhoven J, Mühldorfer-Fodor M, Fernandez DL, Herbert TJ (2012) Salvage of failed resection arthroplasties of the distal radioulnar joint using an ulnar head prosthesis: long-term results. J Hand Surg Am 37: 1372–80.
93. Kapandji AI (1992) Distal radio-ulnar prosthesis. Ann Chir Main Memb Super 11: 320-332. [Crossref]
94. Herbert TJ, van Schoonhoven J (2007) Ulnar head replacement. Tech Hand Up Extrem Surg 11: 98-108. [Crossref]
95. Schmidt I (2014) Primary combined replacements for treatment of distal radius physeal arrest. J Wrist Surg 3: 203 - 205. [Crossref]
96. Schmidt I (2017) Distal radioulnar synostosis after primary combined replacements for treatment of highly comminuted distal radius fracture in an elderly patient. J Hand Surg Eur Vol 42: 97 - 98.
97. Schmidt I (2017) RE-MOTIONTM total wrist arthroplasty for treatment of advanced stage of scaphoid non-union advanced collapse. Does excision of the entire scaphoid bone prevent impingement at terminal range of radial deviation? Trauma Emerg Care 2: doi: 10.15761/TEC.1000127.
98. Schmidt I (2017): Combined replacements of the wrist, ulnar head, and thumb carpometacarpal joint. Case report, technical note and recent evidence to the ArpeTM prosthesis. Trauma Emerg Care 2: doi: 10.15761/TEC.1000130.
99. Herzberg G (2010) Periprosthetic bone resorption and sigmoid notch erosion around ulnar head implants: a concern? Hand Clin 26: 573-577. [Crossref]
100. Yen Shipley N, Dion GR, Bowers WH (2009) Ulnar head implant arthroplasty: an intermediate term review of 1 surgeon's experience. Tech Hand Up Extrem Surg 13: 160-164. [Crossref]
101. Moulton LS, Giddins GEB (2017) Distal radio-ulnar implant arthroplasty: a systematic review. J Hand Surg Eur Vol 42: 827-838. [Crossref]
102. Ewald TJ, Skeete K, Moran SL (2012) Preliminary experience with a new total distal radioulnar joint replacement. J Wrist Surg 1: 23-30.
103. Dellacqua D (2009) Total wrist arthroplasty, Tech Orthop 24: 49-57.
104. Nydick JA, Greenberg SM, Stone JD, Williams B, Polikandriotis JA, Hess AV (2012) Clinical outcomes of total wrist arthroplasty. J Hand Surg Am 37: 1580-1584. [Crossref]
105. Schmidt I (2016) An Unusual and Complicated Course of a Giant Cell Tumor of the Capitate Bone. Case Rep Orthop 2016:3705808. Epub 2016 Oct 25. [Crossref]
106. Schmidt I (2017): Kienböck's disease mimicing gouty monoarthritis of the wrist. Int J Case Rep Images 8: 423 - 426.
107. Schmidt I (2017): The MaestroTM Wrist Reconstructive System for treatment of posttraumatic wrist joint osteoarthritis after a devasting course of a distal radius fracture: Case presentation and technical note to the implant. Trauma Emerg Care 2): doi: 10.15761/TEC.1000124.
108. Gaspar MP, Lou J, Kane PM, Jacoby SM, Osterman AL, Culp RW (2016) Complications Following Partial and Total Wrist Arthroplasty: A Single-Center Retrospective Review. J Hand Surg Am 41: 47-53.
109. Reigstad O, Røkkum M (2014) Wrist arthroplasty: where do we stand today? A review of historic and contemporary designs. Hand Surg 19: 311-322. [Crossref]
111. Gil JA, Kamal RN, Cone E, Weiss AC (2017) High Survivorship and Few Complications With Cementless Total Wrist Arthroplasty at a Mean Followup of 9 Years. Clin Orthop Relat Res Jul 18. doi: 10.1007/s11999-017-5445-z. [Epub ahead of print]
112. Adams BD (2004) Total wrist arthroplasty. Orthopedics 27: 278-284. [Crossref]
113. Wagner ER, Srnec JJ, Mehrotra K, Rizzo M (2017) What Are the Risk Factors and Complications Associated With Intraoperative and Postoperative Fractures in Total Wrist Arthroplasty? Clin Orthop Relat Res Jul 7. doi: 10.1007/s11999-017-5442-2. [Epub ahead of print]
114. Herzberg G, Boeckstyns M, Sorensen AI, Axelsson P, Kroener K, Liverneaux P, Obert L, Merser S (2012) "Remotion" total wrist arthroplasty: preliminary results of a prospective international multicenter study of 215 cases. J Wrist Surg 1: 17-22.
115. Boeckstyns ME, Merser S (2014) Psychometric properties of two questionnaires in the context of total wrist arthroplasty. Dan Med J 61: A4939. [Crossref]
116. Baldwin WI. Orthopaedic surgery of the hand and wrist. In: Jones R, ed. Orthopaedic Surgery of Injuries. London, England: Henry Frowde and Hodder & Stoughton; 1921:241–282.
117. Sauvé L, Kapandji M (1936) Nouvelle technique de traitement chirurgical des luxations recidivantes isoleés de l’extremité inferièure du cubitus. J Chir (Paris) 47: 589-594.
118. Berry JA (1931) Chronic subluxation of the distal radio-ulnar articulation. Br J Surg 18: 526–527.
119. Lichtman DM, Ganocy TK, Kim DC (1988) The indications for and techniques and outcomes of ablative procedures of the distal ulna: the Darrach resection, hemiresection, matched resection and Sauvé-Kapandji procedure. Hand Clin 14: 265-277.
120. Gordon L, Levinsohn DG, Moore SV, Dodds RJ, Castleman LD (1991) The Sauvé-Kapandji procedure for the treatment of posttraumatic distal radioulnar joint problems. Hand Clin 7: 397-403. [Crossref]
121. Sanders RA, Frederick HA, Hontas RB (1991) The Sauvé-Kapandji procedure: a salvage operation for the distal radioulnar joint. J Hand Surg Am 16:1125-1129. [Crossref]
122. Millroy P, Coleman S, Ivers R (1992) The Sauvé-Kapandji operation: technique and results. J Hand Surg Br 1992;17:411-414. [Crossref]
123. Lluch A (2013) The Sauvé-Kapandji procedure. J Wrist Surg 2: 33-40. [Crossref]
124. Shaaban H, Giakas G, Bolton M, Williams R, Scheker LR, Lees VC (2004) The distal radioulnar joint as a load-bearing mechanism--a biomechanical study. J Hand Surg Am 29: 85-95.
125. Arora R, Gabl M, Pechlaner S, Lutz M (2010) Initial shortening and internal fixation in combination with a Sauvé-Kapandji procedure for severely comminuted fractures of the distal radius in elderly patients. J Bone Joint Surg Br 92: 1558-1562.
126. Goorens CK, Geurts C, Goubau J (2013) Primary shortening of the forearm and Sauvé-Kapandji for severely comminuted fractures of the distal forearm in elderly patients: a case report. Hand Surg 18: 399-402.
127. Johnsons RK, Shrewsbury MM (1976) The pronator quadratus in motions and stabilization of the radius and ulna at the distal radioulnar joint. J Hand Surg Am 1: 205–209.
129. Pechlaner S, Sailer R (1993) Die Arthrodese des distalen Radioulnargelenks mit Segmentresektion aus der Elle: Operationsverfahren nach Kapandji-Sauvé. Operat Orthop Traumatol (Urban & Vogel, München) 5: 48-59.
130. Welk E, Martini AK (1998) Late outcome of Kapandji-Sauvé distal radio-ulnar arthrodesis. Handchir Mikrochir Plast Chir 30: 394-398. [Crossref]
131. Goodfellow JW, Bullough PG (1967) The pattern of ageing of the articular cartilage of the elbow joint. J Bone Joint Surg Br 49: 175-181. [Crossref]
132. Carter PB, Stuart PR (2000) The Sauvé-Kapandji procedure for post-traumatic disorders of the distal radio-ulnar joint. J Bone Joint Surg Br 82: 1013-1018. [Crossref]
133. Abid H, Shimi M, El Ibrahimi A, El Mrini A (2015) Results of the Sauvé-Kapandji Procedure for Posttraumatic Disorders of the Distal Radioulnar Joint in Young Patients. Open J Orthop 5: 35-40.
134. Daecke W, Martini AK, Streich NA (2003) Kapandji-Sauvé procedure for chronic disorders of the distal radioulnar joint with special regard to the long-term results. Handchir Mikrochir Plast Chir 35: 164-169.
135. Dohn P, Khiami F, Rolland E, Goubier JN (2012) Adult post-traumatic radioulnar synostosis. Orthop Traumatol Surg Res 98: 709-714. [Crossref]
136. Daecke W, Martini AK, Schneider S, Streich NA (2006) Amount of ulnar resection is a predictive factor for ulnar instability problems after the Sauvé-Kapandji procedure: a retrospective study of 44 patients followed for 1-13 years. Acta Orthop 77: 290-297.
137. Sarmiento A, Cooper JS, Sinclair WF (1975) Forearm fractures. Early functional bracing - A preliminary report. J Bone Joint Surg Am 57: 297-304.
138. Boynton JF, Budoff JE, Clifford JW (2005) The effect of forearm bracing on radioulnar impingement. J Hand Surg Br 30: 157-161. [Crossref]
139. Kapandji IA (1986) The Kapandji-Sauvé operation. Its techniques and indications in non rheumatoid diseases. Ann Chir Main 5: 181-193. [Crossref]
140. Gupta RK, Soni A, Malhotra A, Masih GD (2017) "Quadrangular-construct" modification of Sauvé-Kapandji procedure. Indian J Orthop 51: 99-102. [Crossref]
141. Gabl M, Arora R (2011) Distales Radioulnargelenk (DRUG) und triangulärer fibrokartilaginärer Komplex (TFCC). In: Towfigh H, Hierner R, Langer M, Friedel R (eds.), Handchirurgie (Springer, Berlin-Heidelberg-New York) 1: 839-860.
142. Hammert WC (2014) Management of the symptomatic wrist following distal ulna resection. J Hand Surg Am 39: 1833-1836. [Crossref]
143. Castle ME (1974) One-bone forearm. J Bone Joint Surg Am 56: 1223-1227. [Crossref]
144. Varitimidis SE, Venouziou AI, Dailiana ZH, Malizos KN (2009) One-bone forearm reconstruction procedure as salvage operation after severe upper extremity trauma: a case report. Am J Orthop (Belle Mead NJ) 38: 90-92.
145. Jacoby SM, Bachoura A, Diprinzio EV, Culp RW, Osterman AL (2013) Complications following one-bone forearm surgery for posttraumatic forearm and distal radioulnar joint instability. J Hand Surg Am 38: 976-982.
146. Peterson CA 2nd, Maki S, Wood MB (1995) Clinical results of the one-bone forearm. J Hand Surg Am 20: 609-618. [Crossref]
147. Watson-Jones R (1934) Reconstruction of the forearm after loss of the radius. Br J Surg 22: 23-26.
148. Lowe HG (1963) Radioulnar fusion for defects in the forearm bones. J Bone Joint Surg Br 45: 351-359.
149. Hahn SB, Kang HJ, Hyung JH, Choi YR (2011) One-bone forearm procedure for acquired pseudoarthrosis of the ulna combined with radial head dislocation in a child: a case with 20 years follow-up. Yonsei Med 52: 204-206.
150. Helm RH, Pho RW, Tonkin MA (1992) The sequelae of osteomyelitis of the proximal ulna occurring in early childhood. J Hand Surg Br 17: 232-234. [Crossref]











