In the 20 years after introducing our original technique-EPDBD (Endoscopic Pancreatic Duct Balloon Dilation) in 1996, we treated 599 cases of pancreas stone, pseudocyst and divisum cases at our hospital by this method. With this procedure, pancreatic stone recurrence rate dropped remarkably, and the success rate of endoscopic pseudocyst and divisum treatments rose dramatically. Complications were moderate pain and light bleeding from the orifice at the time of treatment and slight pancreatitis for several days. This method is very useful and safe, and shows big possibilities for endoscopic treatment of pancreatic diseases.
Endoscopic Pancreatic Duct Balloon Dilation-EPDBD, pancreatic stone, chronic pancreatitis, pseudocyst, divisum
Balloon dilation of choledochus is a popular procedure for bile duct stone treatment. In 1996, we got a hint from this technique, and started our clinical application of pancreatic duct balloon dilation to treat pancreatic diseases [1,2]. The balloon was inserted into the pancreatic duct and dilation of orifice and narrow portion of the duct was done. The objective of this was to
① ease the discharge of pancreatic stones by expanding the narrow pancreatic duct
② facilitate the placement of a stent after stone removal
③ suppress stone recurrence by expanding the narrow duct (Table 1).
We then expanded the indication to non-calcified divisum and non-calcified pseudocyst complicated with narrow duct.
In this article, we would like to point out the indications and precise method of this treatment as well as its limitations (Although some cases may overlap, we will examine EPDBD cases in order of pancreatic stone, pseudocyst, and divisum cases).
Of the 630 cases of pancreatic stone disease that we experienced over the last 27 years, 588 cases received medical treatment (Table 2). The breakdown of the treatment was as follows: 50 cases of ESWL alone, 90 cases of endoscopy alone, and 448 cases of ESWL + endoscopy. EPDBD was conducted in a total of 538 cases. (via major papilla 445 cases, via minor papilla 93 cases) The purpose of EPDBD in pancreatic disease is shown in table 1. EPDBD is normally performed after EPST of major papilla, but when the Wirsung duct is markedly bent or constricted due to inflammation, or in cases of stone impaction in Wirsung duct, in cases of divisum (complete, incomplete), treatment was performed via the minor papilla.
The balloon dilation catheter that we used (Rapid Exchange Dilatation Balloon catheter 6 mm diameter-Boston Scientific) is extremely useful in that it has a breakthrough strength equivalent to that of the Soehendra type dilation catheter. Gradually the pressure was increased to 6 atmospheres in the papillary part and stenotic pancreatic duct and dilation was performed for one minute multiple times. In our hospital by medical treatment, the percentage of stone disappearance was 75.3% and the rate of pain disappearance was 97.1%, like results reported by other authors. The stone recurrence rate, however, was 5.6%, lower than other reports, thought to be the effect of EPDBD [3,4] (Table 3).
As for complications, there was only some pain and light bleeding at the time of treatment, with the former able to be treated with pain relievers such as pentazocine. Several days after treatment, symptoms of pancreatitis improved with conservative treatment.
Case 1
A 22-year-old male with idiopathic chronic pancreatitis and pancreatic stones (the first implementation of EPDBD at our hospital) with epigastric pain prompting was hospitalized. We performed ESWL several times on large stones in the duct, but small stones remained. Not able to remove the stones and with severe pain continuing, EPDBD was performed under good informed consent (Figure 1). When the papilla and head duct of the pancreas were dilated several times at 6atm for 1 minute, a mechanical crushing tool (ML) could easily be inserted into the pancreatic duct from the open papilla orifice and the stones were crushed and removed easily. Pain improved promptly after treatment and no complications were observed. The patient has been pain-free without restenosis or stone recurrence for 20 years till now.

Figure 1. 22 y/o m idiopathic chronic pancreatitis (the first implementation of EPDBD) After EPST, ESWL was done, but fragments could not be removed and severe pain continued. So EPDBD was done (6 atm, 1 minutes, several times). Then stones were removed through opened orifice easily by ML.
Case 2
A 72-year-old male with chronic alcoholic pancreatitis and pancreatic stones. Hospitalized with abdominal pains, the patient was found to have a 5-mm stone impacted in the head duct. After EPST of the papilla, EPDBD was performed and the stone easily extracted (Figure 2).

Figure 2. 72 y/o m alcoholic. Small stone (5mm) was impacted in the head duct. After EPST+EPDBD, stone was removed.
Case 3
A 70-year-old male with alcoholic chronic pancreatitis and pancreatic stones. After ESWL, with the Wirsung-duct occluded due to stone impaction, EPST and EPDBD of minor papilla were performed and stone fragments were removed easily via minor papilla (Figure 3).

Figure 3. 70 y/o m alcoholic. W-duct was obstructed due to stone impaction, so after EPST and EPDBD stone was removed.
EPDBD for pseudocyst and abscess
Endoscopic procedure via duodenal papilla (ENPD, EPS) is the treatment of first choice at our hospital with percutaneous or trans gastric-wall drainage as necessary. When good ERP showed traffic between the cysts and the pancreatic duct, a guide wire was inserted into cysts beyond the constricted section and after EPDBD of the stricture, ENPD or long EPS was placed (Figure 4). Of the 152 cases in which this method was attempted, the above treatment was possible in 111 cases with a high rate of placement and effective cyst drainage. The possibility of endoscopic treatment of pseudocysts has been greatly expanded by this method [5,6].

Figure 4. Treatment of pseudocyst. (A) into the cyst. (B) just before the cyst (C) beside the cyst
Pancreas pseudocyst treatment-case presentations
Case 4
A 29-year-old female with chronic alcoholic pancreatitis and pancreatic stones was hospitalized with fever, abdominal pain and dyspnea due to pancreatic pleural effusion. ERP showed stones impacted in the Wirsung duct, so EPDBD was performed via minor papilla. ENPD was placed beyond the ruptured point and exchanged for EPS one week later (Figure 5).

Figure 5. 29 y/o f alcoholic. W-duct was obstructed due to stone impaction, so ENPD and long EPS were placed beyond the rupture point via minor papilla.
Case 5
A 56-year-old male with chronic alcoholic chronic pancreatitis and pseudocysts. The patient was hospitalized with abdominal pain. ERP showed stricture and pseudocysts. After EPDBD, EPS was placed into the cyst (Figure 6).

Figure 6. EPDBD of the narrowed duct in body.
Case 6
A 68-year-old male with chronic alcoholic pancreatitis and pseudocysts. Stenotic pancreatic duct in the body was dilated and ENPD-EPS was placed into the cyst (Figure 7).

Figure 7. Treatment of pseudocyst by EPDBD+ long EPS. After dilation of the stricture, long EPS was placed into the cyst.
EPDBD for complete and incomplete divisum
There were 17 cases of divisum (8 complete, 9 incomplete-12 with stones, and 5 stone-free) treated at our hospital. EPDBD was done in 2 cases via the major papilla and 14 cases via the minor papilla respectively, then EPS was placed successfully. One case without symptoms was followed up without therapy.
pancreas divisum treatment-case presentations
Case 7
A 72-year-old male with chronic alcoholic pancreatitis, pancreatic stones, and type 2 incomplete divisum [7,8] was hospitalized. A large stone impacted in the Wirsung duct was fragmented by ESWL. Then ERP showed type 2 incomplete divisum. EPST and EPDBD of minor papilla was performed, and stones were expelled (Figure 8-1 and 8-2).

Figure 8. 72 y/o m alcoholic, stone type 2 incomplete divisum. After EPST+EPDBD of minor papilla stones were removed and EPS was placed.
Case 8
A 38-year-old male with pancreatic stones and type 2 incomplete divisum was admitted into the hospital. A guide wire passed through the thin connecting duct between Wirsung and Santorini duct, EPDBD was performed, then stones were expelled and EPS was placed deeply via major papilla (Figure 9).
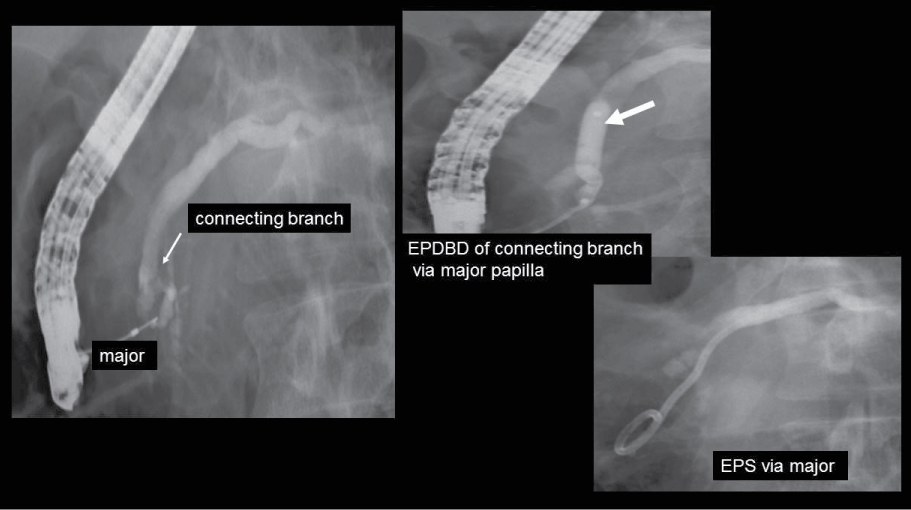
Figure 9. 38 y/o m pancreatic stone, type 2 incomplete divisum. After dilation of connecting branch, EPS was placed via major papilla.
In endoscopic treating via minor papilla, it is necessary to incise the minor papilla safely [9,10].
We introduced EPDBD (Endoscopic Pancreatic Duct Balloon Dilation) therapy in 1996. Dilation of the main pancreatic duct in the major papilla and head was performed, initially with the aim of improving the effectiveness of pancreatic stone removal. It became clear that in repeated cases, the therapy contributed to improvement in pain reduction and decreased recurrence rate. Since then we have gradually expanded its indications and use it to treat non-calcified divisum via minor papilla as well as perform drainage of pseudocyst. A total of 599 cases (538 cases of pancreatic stone, 56 cases of non-calcified pseudocyst, and 5 cases of non-calcified divisum) have been treated with this method. As for complications,
some pain and slight bleeding as well as symptoms of pancreatitis were observed after therapy, but all improved with conservative treatment promptly.
According to reports from other authors, the balloons used in EPDBD had diameters of 4mm, 6mm, and 8mm with the purpose of dilation being stent pretreatment, aiding in stone removal, prevention of stone recurrence, improving the flow of pancreatic juice, easy insertion of treatment tools, increasing the stone-free rate, and reducing the rate of recurrence. Regarding dilation time and pressure, procedures at 3-6 atmospheres, or 1-2 minutes, continuously for 30 seconds after the notch disappears, 6-10 atmospheres for 1 minute several times until the notch disappears, usually dilating until the notch disappears have also been reported. There are also reports of the notch occasionally not disappearing due to unremoved stones, and in those cases, pressurization above the prescribed pressure should be avoided to prevent pancreatic duct injury. If EPDBD was done when small stones remain in the duct, it sometimes becomes difficult to expel the stone because small stones enter the small branch cavity. The balloon at the time of dilation also sometimes breaks due to sharp residual stones and it becomes necessary to replace the balloon catheter. It is also recommended that EPS should be placed just after EPDBD to prevent re-stenosis [11,12].
In some authors’reports, stone excretion rate with ESWL and endoscopy was 72.6%, disappearance of symptoms was 91.1%, recurrence rate was 22% at 25.1 months later. Excretion rate and symptom disappearance rate results at our hospital were similar but recurrence rate was significantly lower at 5.6%, considered to be an effect of combined EPDBD therapy [13-21]. However, some limitation is that the effect is not permanent; negative effects on the pancreatic duct and parenchyma is unknown; not knowing how much air pressure and time is best; and not having specialized tools available [22-29].
We believe that even in the deep pancreatic duct, if pressure is lowered and care is taken, large tissue damage will not occur. It is not known however, whether the pancreatic duct and pancreatic parenchyma are histopathologically affected, so cautious treatment is required in the future.
Our hospital’s objectives, responses, and methods are explained previously. We believe that this method has a huge effect on lowering the recurrence rate of pancreatic stones, rising the success rate of pseudocyst drainage and the treatment via minor papilla. As treatment tools are improved and the above unknown points become clearer in the future, it is expected that this method will further contribute to the endoscopic treatment of pancreatic stones, pseudocysts, and other pancreatic disorders.
- Tsuji T (2001) Treatment of Chronic Pancreatitis and Pancreas Stone by EPDBD-Endoscopic Pancreatic Duct Balloon Dilation. Tan to Sui 22: 127-137.
- Tsuji T (2004) Endoscopic Treatment of Pancreatolithiasis-Efficacy and Safety of EPDBD (Endoscopic Pancreatic Duct Balloon Dilation). Tan to Sui 25: 411-420.
- Tsuji T, Shiratori K, Katoh M, Yamafuji K, Okamoto N (2009) Treatment of 225 cases of chronic pancreatitis and pancreatic stone-the effect of ESWL + endoscopy therapy and its prognosis. Pancreas 24: 62-73.
- Maeki K (2001) Endoscopic Pancreatic Duct Balloon Dilation for Pancreatic Duct Stricture. Tan to Sui 22: 121-1: 6.
- Imbe (2014) Therapeutic endoscopy for pancreas disease. Kan Tan Sui 69: 245-254.
- Mimura (2015) Efficacy of combined endoscopic treatment and extracorporeal shock wave lithotripsy for pancreatic lithiasis. Pancreas 30: 154-163.
- Tsuji T (2012) Endoscopic Treatment of Pancreatic Diseases via Minor Papilla. Tan to Sui 33: 995-1003.
- Tsuji T (2009) Treatment of the Pancreas Diseases Via Minor Papilla. Tan to Sui 30: 1187-1194.
- Tsuji T, et al. (2014) Endoscopic treatment of the Pancreas Diseases Via Minor Papilla. Tan to Sui 35: 439-446.
- Isayama H (2008) Endoscopic Balloon Dilation for minor Papilla: Efficacy and Safety for the patient with Pancreas divisum Tan to Sui 29: 1003-1008.
- Atomi Y (2003) Multicenter Survey about Pancreatic Stone Treatment. Japan ESWL Society.
- Inui K (2014) Guideline of Pancreatic Stone Treatment Japan Pancreatic Society. Pancreas: 22:142-143.
- Inui K, Tazuma S, Yamaguchi T, Ohara H, Tsuji T, et al. (2005) Treatment of pancreatic stones with extracorporeal shock wave lithotripsy: results of a multicenter survey. Pancreas 30: 26-30. [Crossref]
- Yamaguchi T (1996) Treatment of pancreatic stone-Endoscopic treatment and its indication. Kan Tan Sui 33: 407-412.
- Sauerbruch T, Holl J, Sackmann M, Werner R, Wotzka R, et al. (1987) Disintegration of pancreatic duct stone with extracorporeal shock wave in a patient with chronic pancreatitis. Endoscopy,19: 207-208. [Crossref]
- Sauerbruch T, Holl J, Sackmann M, Paumgartner G (1992) Extracorporeal lithotripsy of pancreatic stones in patients with chronic pancreatitis and pain: a prospective follow up study. Gut 33: 969-972. [Crossref]
- Delhaye M, Vandermeeren A, Baize M, Cremer M (1992) Extracorporeal shock-wave lithotripsy of pancreatic calculi. Gastroenterology 102: 610-620. [Crossref]
- Schneider HT, May A, Benninger J, Rabenstein T, Hahn EG, et al. (1994) Piezoelectric shock wave lithotripsy of pancreatic duct stones. Am J Gastroenterol 89: 2042-2048. [Crossref]
- Brand B, Kahl M, Sidhu S, Nam VC, Sriram PV, et al. (2000) Prospective evaluation of morphology, function, and quality of life after extracorporeal shockwave lithotripsy and endoscopic treatment of chronic pancreatitis. Am J Gasroentorol 91: 1388-1394. [Crossref]
- Tadenuma H, Ishihara T, Yamaguchi T, Tsuchiya S, Kobayashi A, et al. (2005) Long-term results of extracorporeal shockwave lithotripsy and endoscopic therapy for pancreatic stones. Clin Gastroenterol Hepatol 3: 1128-1135. [Crossref]
- Parsi MA, et al. (2010) Extracorporeal shock wave lithotripsy for prevention of reccurent pancreatitis caused by obstructive pancreatic stones. Pancreas 39: 153-155.
- Lawrence C, et al. (2010) Chronic calcific pancreatitis: combination ERCP and extracorporeal shockwave lithotripsy for pancreatic duct stones. South Med J 103: 505-508. [Crossref]
- Milovic V, Wehrmann T, Dietrich CF, Bailey AA, Caspary WF, et al (2011) Extracorporeal shock wave lithotripsy with a transportable mini-lithotripter and subsequent endoscopic treatment improves clinical outcomes in obstructive calcific chronic pancreatitis. Gastrointest Endosc 74: 1294-1299. [Crossref]
- Tandan M, Reddy DN, Santosh D, Vinod K, Ramchandani M, et al. (2010) Extracorporeal shock wave lithotripsy and endotherapy for pancreatic calculi – a large single center experience. Indian J Gasroentorol 29: 143-148. [Crossref]
- Guda NM, Partington S, Freeman ML (2005) Extracorporeal shock wave lithotripsy in the management of chronic calcific pancreatitis: a meta-analysis. JOP 6: 6-12. [Crossref]
- Adamek HE, Jakobs R, Buttmann A, Adamek MU, Schneider AR, et al. (1999) Long term follow up of patients with chronic pancreatitis and pancreatic stones treated with extracorporeal shock wave lithotripsy. Gut 45: 402-405. [Crossref]
- Rosch T, Daniel S, Scholz M, Huibregtse K, Smits M, et al. (2002) Endoscopic treatment of chronic pancreatitis: a multicenter study of 1000 patient with long -term follow up. Endoscopy 34: 765-771. [Crossref]
- Kozarek RA, Brandabur JJ, Ball TJ, Gluck M, Patterson DJ, et al. (2002) Clinical outcomes in patient who undergo extracorporeal shock wave lithotripsy for chronic calcific pancreatitis. Gastrointest Endosc 56: 496-500. [Crossref]
- Choi EK, Lehman GA (2012) Update on endoscopic management of main pancreatic duct stones in chronic calcific pancreatitis. Korean J Intern Med 27: 20-29. [Crossref]









