Background: High volume intensive care units with high expertise on respiratory distress syndromes are familiar with extracorporeal CO2 elimination procedures in regard to their maintenance. In contrast, small intensive care units offer a lack of this experience. So, a novel approach (passive, invasive, without any further specification) plugs this lack of experience.
Case Report: A 60 years old male patient in poor health conditions was presented to our small intensive care unit due to shortness of breath in regard to bilateral pneumonia in septic shock. Sedated and intubated, we monitored blood gas analyses and observed pCO2 problems, raising to 150mmHg with stable pO2 85mmHg. We used interventional arteriovenous lung assist system iLA (Novalung®, Heilbronn, Germany) and improved respiratory conditions by reduction of pCO2 to normal levels constantly for 10 days. Using iLA (Novalung®) on our small ICU we healed passively and invasively the patient for discharging on day 15.
Conclusion: This case report clearly demonstrates the unspectacular use of the highly effectual passive and invasive CO2 elimination system iLA, Novalung® (Heilbronn, Germany) even on a small intensive care unit of a hospital for basic and regular care in Germany.
CO2 retention, passive and invasive CO2 elimination, interventional Lung Assist system: iLA (Novalung®, Heilbronn, Germany), septic pneumonia.
Extracorporeal gas exchange by extracorporeal membrane oxygenation (AVCO2R) has been established clinically in patients with acute lung failure [1]. The interventional lung-assist (iLA) Membrane Ventilator device (Novalung®) is a sophisticated representative of a new generation of pumpless extracorporeal lung-assist devices that are driven by the patient’s cardiac output and therefore, do not require extracorporeal pump assistance. The system is characterized by a new membrane gas exchange system with optimized blood flow that is integrated in an arteriovenous bypass established by vascular cannulation. This particular pumpless extracorporeal lung-assist device was applied in 1800 patients for artificial lung assistance with easy use and low cost [2]. AVCO2R is commercially available through Novalung® (Heilbronn, Germany) and marketed as the interventional lung assist (iLA) membrane ventilator. The membrane lung, frequently called the ‘Novalung’, utilizes a low resistance design allowing blood flow using the patient’s own arteriovenous pressure gradient. Cannulas are placed percutaneously in the femoral artery and vein [1,3]. A similar system has been developed in the United States using the Affinity NT (Medtronic, Minneapolis, MN) [4]. Pumpless systems require an arteriovenous pressure gradient ≥60 mmHg, which is unsuitable for hemodynamically unstable patients [5]. Further, cannulation of a major artery can result in distal ischemia [3], although measuring the artery diameter with ultrasound and selecting a cannula that occupies no more than 70% of the lumen reduces this risk [1]. AVCO2R has been successfully used to facilitate LPV in patients with ARDS [6], severe asthma [7] and as a bridge to lung transplantation [8].
High volume intensive care units with high expertise on respiratory distress syndromes are familiar with extracorporeal CO2 elimination procedures in regard to their maintenance (see 1-13). In contrast, small intensive care units offer a lack of this experience [5]. So, a novel approach (passive, invasive, without any specification) plugs this lack of experience [1].
A 60 years old male patient in poor health conditions (180cm length, 55kg weight) suffering severe septic bilateral pneumonia reported and confirmed on chest x-ray slides (Figure 1) was supported to the small intensive care unit (ICU: 4 beds – personally adjusted for breathing) of a hospital with in total 196 beds, distributed to the departments for internal medicine [cardiology, gastro-enterology and hematology/oncology], orthopedics, neurology, obstetrics-gynecology and anesthesiology and critical care medicine, neurology, orthopedics and trauma surgery, gynecology for basic and regular care in South Germany due to shortness of breath in the emergency room. As co-morbidities, we had to handle with schizophrenia, multiple sclerosis, epilepsy, chronic obstructive lung disease due to extreme consume of nicotine.
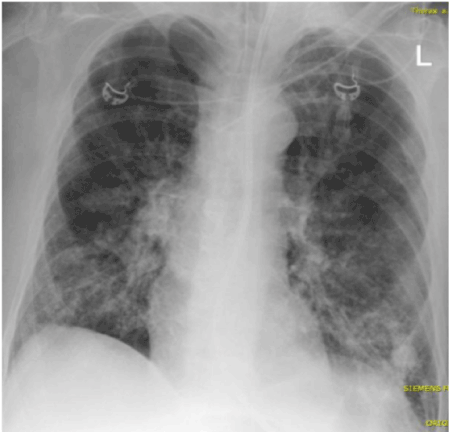
Figure 1. Chest X-Ray. Chest x-ray slides were performed ad admission to the hospital/ intensive care unit, after supply of additive catheters (breathing tube, central vein catheter, probe for stomach) and in episodes of time course to manage pneumonia infiltrations and lung-targeted specific antibiotics. Here is an example for the chest x-ray ad admission demonstrating emphysema of the lung, signs of chronic obstructive lung disease, old fractions of the ribs on left lower side, infiltrative changes in both lower and middle lobs of the lung, diaphragm plane and extremely down and some electro-cardiogramm cables (ecg).
The patient got immediately intubated, ventilated and physically dependent to the respiratory breathing system (Evita, Infinity V500, Draeger®, Lübeck, Germany). Related to the ventilation, we were forced to decrease the observed CO2 retention and we monitored blood gas analyses with pCO2 rising to 150mmHg under all additive ventilatory support (bronchoscopy, kinetic mobilization, lung-targeted use of antibiotics, lung-protective ventilation support, respectively) with pO2 maximum stable to 85mmHg. On top, pH levels decreased to lowest 6.99. Additionally, the septic shock was attacked using nor-epinephrine and hydrocortisone, preventive support was applied as well: pantoprazole or i.e. support of enteral nutritive factors up to 1.75 liter a day (correspondence to 1750kcal a day). The daily medications in reflection to his co-morbidities were applied as well orally. We decided additionally to use a passive, invasive interventional Lung Assist system to eliminate CO2 [9]: iLA (Novalung®, Heilbronn, Germany) (Figure 2) in regard to the lack of physicians in afternoon- /night worktime on the ICU board maintaining an active extra corporal lung assist, i.e. CARDIOHELP, Marquet® or LIFEBRIDGE 2.0, Zoll® [10]. We assumed 15 French (15F) artery support to the iLA femoral left, set the iLA system (Novalung®) between his legs and re-insufflated the blood venously (15F) to the right femoral vein passively (see figure 2). Flow of oxygen was initially adapted to 10 liters per minute and nor-epinephrine was used to support blood flow to 1.2 liters per minute in the iLA system and to abolish the CO2 monitored through external device (Figure 3) with a “device related receptor” fixed on the venous blood flow system (Figure 4). The iLA Novalung® system was developed as passive as well as invasive artery-venous Shunt system for diffusion and displacement of CO2 to O2 in the patient own blood flow [11]. Therefore, the circulatory cardiac conditions have to be improved, monitored intensively and supported (norepinephrine). Inside of the iLA, the membrane ventilation occurs, and displaces CO2 to O2 in the blood flow maintained through the own patient’s circulation. In general, the use of these CO2 elimination systems was maintained on ICU’s with fast turnover and effective experiences. Meanwhile in the time course, we were able to reduce passively pCO2 from 150mmHg on iLA-day 1 to 50mmHg on day 10 reducing the initial oxygen flow of 10 liters per minute through the iLA system to almost 0 liter per minute under circulatory stable conditions: norepinephrine supported 1.2 liters per minute venous blood flow through the system and 99% saturation of O2 using diffusion to eliminate CO2 on the membranous filters of the iLA system (see figure 5–upper diagram) – without any further medical support and without having physicians continuously monitoring the iLA system throughout the afternoon-/ night worktime. Oxygen levels stayed stable throughout the whole use of the device (Figure 5–lower diagram). Additionally, initial decreased pH levels to lowest 6.99 were maintained to increase to normal levels over the complete use of iLA on ICU and marked stable (Figure 6). The patient was sedated in a RASS-State -3—4 (Richmond Agitation and Sedation Scale) with Sevoflurane via the AnaConDa-S®-System.
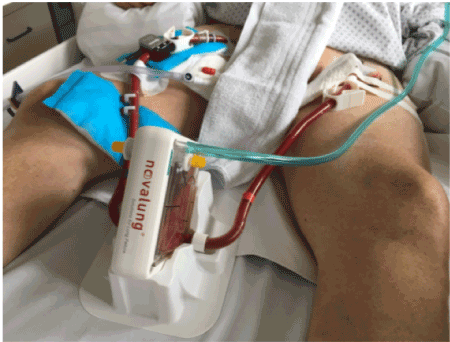
Figure 2. iLA Novalung® CO2 elimination system, passive, invasive, comfortable. Interventional Lung Assist system iLA (Novalung®, Heilbronn, Germany) to eliminate CO2 and to displace it with O2 on membranes in the devices was used for this patient on the intensive care unit of the small hospital for basic and regular care in Germany. The device maintaining the membranes was put in the bed between the legs. Incoming arterially blood was managed through 15F success of left femoral artery and goes into the device, oxygen support (divers oxygen flow from 0 liter per minute up to 10 liters per minute – see green tubing on the device) will manage diffusion of CO2 and will displace CO2 to O2 in the device. Back to the patient, blood flow will get monitored and successfully maintained through 15F access to right femoral vein.

Figure 3. Monitoring of blood flow. The Monitoring of the blood flow on venous side of the device (Novalung®, Heilbronn, Germany). Saturation data of O2 in the probe will care for the successful diffusion of CO2 on the membranes (data on the left of the display), blood flow [liter per minute] will maintain correct and adequate circulation to support effective blood flow to the iLA device (data on the right of the display).
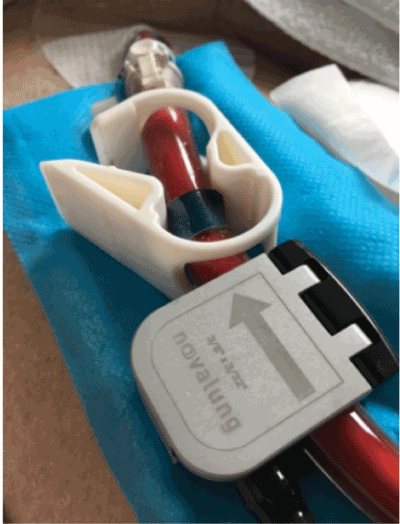
Figure 4. Receptor to monitor the blood flow. The Monitoring of the blood flow on the venous side of the device will achieved through the device related receptor (Novalung®, Heilbronn, Germany).
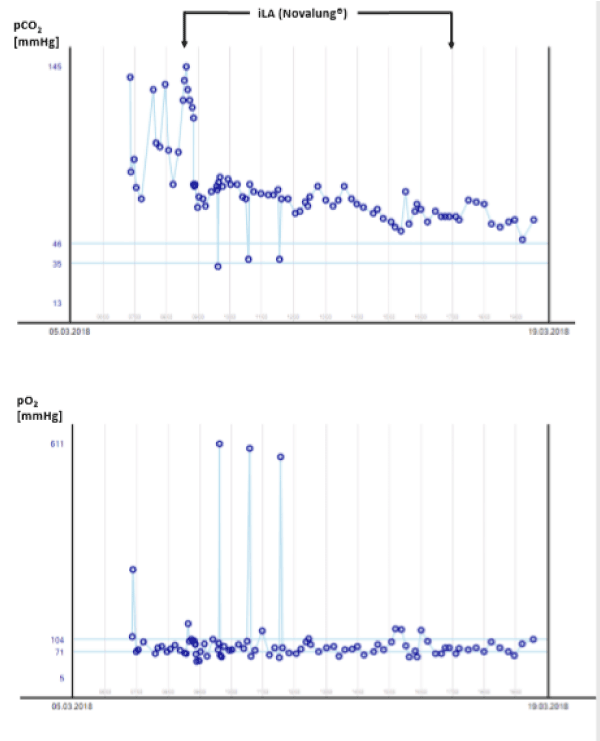
Figure 5. pCO2 and pO2 measurements in blood gas analyses (BGA). Shown here are the various BGA’s of pCO2 levels and pO2 levels in relation to the use of the iLA system for 10 days. The upper diagram shows the course of the pCO2 levels, the lower diagram the course of the pO2 levels for the patient on the intensive care unit in our hospital for basic and regular care. Due to known severe chronic obstructive lung disease committed by active consumption of nicotine, we decided to remove the iLA system while pCO2 levels were below 70mmHg and pO2 levels above 85mmHg – see diagrams.
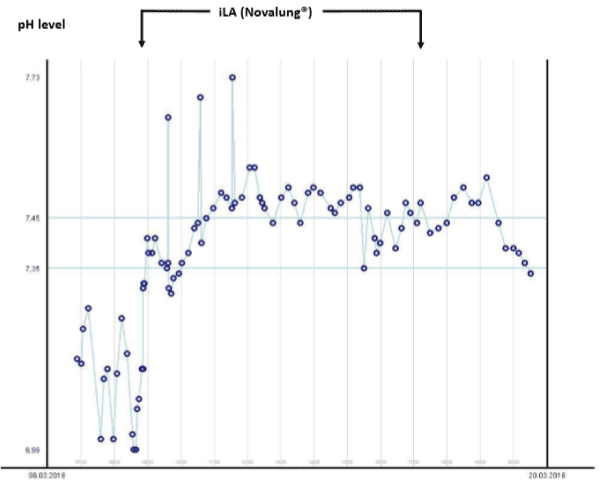
Figure 6. pH measurements in blood gas analyses (BGA). Shown here are the various BGA’s of pH levels in relation to the use of the iLA system for 10 days. The use of the passive and invasive iLA system (Novalung®, Heilbronn, Germany) improved quickly the reduced pH levels from 6.99 to normal and kept these normal levels during the ICU stay as demonstrated in the shown diagram.
On iLA-day 10 (in total day 12 on the ICU) we successfully retracted the system by primarily removing the venous tubing (15F) manually and secondly the arteriosus system (15F) using Femostop, St. Jude Medical® for at least 12 h. Finally, we found unremarkable conditions on both groins and warm pulsed feed. Lastly, the patient recovered quick and got discharged from hospital on day 15 in total for rehabilitation in reflection to medical purposes.
This case report clearly demonstrates (i) the unspectacular use of the highly effectual passive and invasive CO2 elimination system iLA from Novalung® (Heilbronn, Germany) even on a small intensive care unit of a hospital for basic and regular care in Germany [12]. (ii) The effectual elimination of CO2 in patients suffering septic pneumonia will support faster recovery, will lower breathing mechanics [13] for the patients under specific intensive care unit conditions and ventilatory support even when no further problem for oxygenation occurs [10]. Therefore, (iii) pH levels and pCO2 levels were improved as fast as possible. Without specific vascular surgeons (iv) we handled and managed the device successfully. During afternoon and night-shift, (v) no additional physician was necessary to maintain the CO2 elimination system.
- Zimmermann M, Bein T, Philipp A, Ittner K, Foltan M, et al. (2006) Interhospital transportation of patients with severe lung failure on pumpless extracorporeal lung assist. Br J Anaesth 96: 63-66. [Crossref]
- Walles T (2007) Clinical experience with the iLA Membrane Ventilator pumpless extracorporeal lung-assist device. Expert Rev Med Devices 4: 297-305. [Crossref]
- Bein T, Weber F, Philipp A, Prasser C, Pfeifer M, et al. (2006) A new pumpless extracorporeal interventional lung assist in critical hypoxemia/hypercapnia. Crit Care Med 34: 1372-1377. [Crossref]
- Conrad SA, Green R, Scott LK (2007) Near-fatal pediatric asthma managed with pumpless arteriovenous carbon dioxide removal. Crit Care Med 35: 2624-2629. [Crossref]
- Cove ME, Federspiel WJ (2015) Veno-venous extracorporeal CO2 removal for the treatment of severe respiratory acidosis. Crit Care 19: 176.
- Bein T, Zimmermann M, Hergeth K, Ramming M, Rupprecht L, et al. (2009) Pumpless extracorporeal removal of carbon dioxide combined with ventilation using low tidal volume and high positive end-expiratory pressure in a patient with severe acute respiratory distress syndrome. Anaesthesia 64: 195-198. [Crossref]
- Elliot SC, Paramasivam K, Oram J, Bodenham AR, Howell SJ, et al. (2007) Pumpless extracorporeal carbon dioxide removal for life-threatening asthma. Crit Care Med 35: 945-948. [Crossref]
- Bartosik W, Egan JJ, Wood AE (2011) The Novalung interventional lung assist as bridge to lung transplantation for self-ventilating patients - initial experience. Interact Cardiovasc Thorac Surg 13: 198-200. [Crossref]
- Kopp R, Bensberg R, Stollenwerk A, Arens J, Grottke O, et al. (2016) Automatic Control of Veno-Venous Extracorporeal Lung Assist. Artif Organs 40: 992-998. [Crossref]
- Iwashita Y, Imai H (2015) Extracorporeal lung assist for sepsis and acute respiratory distress syndrome. Cardiovasc Hematol Disord Drug Targets 15: 46-56. [Crossref]
- Gorjup V, Fister M, Noc M, Rajic V, Ribaric SF (2012) Treatment of sepsis and ARDS with extracorporeal membrane oxygenation and interventional lung assist membrane ventilator in a patient with acute lymphoblastic leukemia. Respir Care 57: 1178-1181. [Crossref]
- Yalindag-Ozturk N, Vuran C, Karakoc F, Ersu R (2013) Use of pumpless extracorporeal lung assist as rescue therapy in adolescent with cystic fibrosis. Pediatr Int 55: 83-85. [Crossref]
- De Lazzari C, Quatember B, Recheis W, Mayr M, Demertzis S, et al. (2015) Lung assist devices influence cardio-energetic parameters: Numerical simulation study. Conf Proc IEEE Eng Med Biol Soc 2015: 4515-4519. [Crossref]






