The spleen plays an important role in intraerythrocytic protozoal infections such as malaria and babesiosis. Splenic enlargement, splenic inflammation and splenic rupture are known to occur in Babesia infections. In New Jersey and Pennsylvania, B. microti transmitted by Ixodes scapularis is responsible for babesiosis. Here we report 2 patients who presented initially with left upper quadrant discomfort, who were initially misdiagnosed and treated for left sided pyelonephritis. Both patients had fever and thrombocytopenia on admission. Both were blood smear positive for Babesia and one was western blot test positive for Borrelia burgdorferiss, and the other developed a Jarisch-Herxheimer reaction when started on ceftriaxone and doxycycline, likely due to a Borrelia co-infection. Both patients responded rapidly to treatment with doxycycline, azithromycin and atovaquone.
Babesiosis is an anthropo-zoonotic tick-borne disease. Babesia microti, B. divergens, B. duncani , B. venatorum and a B. crassa like pathogen are known to cause human disease [1-3]. Ixodes scapularis is the principal vector in Eastern United States [2]. The intra-erythrocytic parasite causes an infection ranging from asymptomatic to life threatening [4,5]. More severe cases are in asplenic, elderly or immunocompromised individuals [1,4,6]. Some cases have been acquired from blood transfusions [5,7] and organ transplants [8] or transmission from mother to the fetus [9,10]. Here we report the unusual presentations of 2 patients, presenting with left upper quadrant pain in Warren County, New Jersey, USA, initially misdiagnosed and treated for pyelonephritis.
A 84 year old female presented to the emergency department complaining of feeling generally poor for 2 weeks, and a dull, constant, 8/10 pain in her left flank for 1-week, non-radiating and associated with nausea, vomiting, fever and weight loss of about 10 lbs. Vital signs on admission were: temperature (T) 101.7°F (38.2°C), Pulse (P) 114, blood pressure (BP) 112/58, respiratory rate (RR) 20. The physical examination was unremarkable except for slight left upper quadrant tenderness. She was allergic to penicillin. The white blood cell count (WBC) was 6000 (NL4800-10,800/µL), hemoglobin (HGB) 10.2 (NL 12-16 grams/deciliter), Platelet count (PLT) 77,000 (NL 130-400,000/µL) and aspartate amino transferase (AST) 52 (NL 5-45 units/liter) on admission. She was started on levofloxacin for presumed left pyelonephritis. On day 2 the temperature was 102.1°F (38.9°C). WBC was 4300 with HGB 10.2, PLT 69,000 and AST 65. The treatment was changed to aztreonam. On day 3, the urine culture and blood cultures were reported negative. The fever increased to T 104.6°F (40.3°C), WBC was 4900, HGB 10 and PLT 62,000. The treatment was changed again to tigecycline and gentamicin. On 4th day, the temperature was 102.1°F (38.9°C), WBC 2700, HGB 8.5 and PLT 47,000. Lyme western blot test was reported positive. Doxycycline was started. On day 5 the temperature was 99.6°F (37.5°C). The Babesia smear was reported positive. Her serum LDH was 355 (NL 81-234). Babesia microti IgG and IgM levels were elevated, both 1:320 (NL<1:10). The patient was started on Atovaquone 750 mg twice daily and azithromycin 1-gram loading dose followed by 250 mg daily. The next day she was afebrile, T 97.3°F (36.3°C), WBC increased to 3800 and platelets to 115,000 and AST decreased to 52 (Table 1). She felt well and was continued on the same treatment at home for 2 weeks.
Table 1. Case 1 reports showing temperature, blood results, liver functions and treatment
|
|
Temperature
|
WBC (NL 4800-10,800/µl)
|
HGB (NL 12-16 g/dl)
|
PLT (NL 130-400,000/µl)
|
AST (NL 5-45 units/l)
|
LDH (NL 81-234 units/l)
|
Treatment
|
|
Day 1
|
101.7°F (38.2°C)
|
6000
|
10.2
|
77,000
|
52
|
|
Levofloxacin
|
|
Day 2
|
103.7°F (39.8°C)
|
4300
|
9.5
|
69,000
|
65
|
|
Aztreonam
|
|
Day 3
|
104.6°F (40.3°C)
|
4900
|
10
|
62,000
|
|
|
Lyme Western blot positive- Tigecycline, gentamicin, doxycycline
|
|
Day 4
|
102.1°F (38.9°C)
|
2700
|
8.5
|
47,000
|
|
355
|
|
|
Day 5
|
99.6°F (37.5°C)
|
|
|
|
|
|
Blood smear positive for Babesia- Doxycycline, azithromycin, atovaquone
|
|
Day 6
|
97.3°F (36.3°C)
|
3800
|
8.7
|
1,15,000
|
52
|
|
Afebrile, feels better
|
Note: WBC: White blood cells; HGB: Hemoglobin; PLT: Platelets; AST: Aspartate amino transferase; LDH: Lactate Dehydrogenase
A 64-year-old female was treated at an urgent care center for a presumed left sided kidney infection with Macrobid for 1 week. She had been having fever and chills for 2 weeks and was admitted with fatigue, T 100.6°F (38.1°C), left flank pain, thrombocytopenia (Platelets 67,000), leukopenia (WBC 4500) and elevated liver enzymes AST 187 and alanine aminotransferase (ALT) 219 (NL 12-78 units/liter) (Table 2). A tick-borne illness was suspected. She was started on 2 grams of intravenous ceftriaxone daily and oral doxycycline 100 mg twice daily. The next day her temperature increased to 103.7°F (39.8°C), with sweating, shaking chills and a new itchy papular skin rash involving the back of trunk and back of thighs (Jarisch- Herxheimer reaction). These symptoms improved after receiving diphenhydramine 25 mg every six hours. Ceftriaxone was discontinued. Her blood cultures were negative. The urine culture had mixed contaminants. The blood smear was positive for babesia and serum Babesia IgG titer was 1:320 and IgM titer 1:160 (Figure 1). The Lyme western blot test did not have the required number of bands to be considered positive. She was started on azithromycin one-gram loading dose followed by 250 mg daily and atovaquone 750 mg twice daily. She was afebrile next morning and felt much better. Doxycycline was continued due to suspicion of concurrent mixed infection with Borrelia. The treatment was continued to complete 2 weeks. The patient made an uneventful recovery.
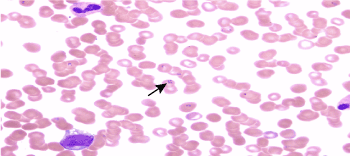
Figure 1. Blood smear showing intra-erythrocytic parasites
Table 2. Case 2 reports showing temperature, blood results, liver functions and treatment
|
|
Temperature
|
WBC (NL 4800-10,800/µl)
|
HGB (NL 12-16 g/dl)
|
PLT (NL 130-400,000/µl)
|
AST (NL 5-45 units/l)
|
ALT (NL 46-116 units/l)
|
Treatment
|
|
Day 1
|
102.5°F (39.2°C)
|
4500
|
13.9
|
67,000
|
187
|
219
|
Rocephin and Doxycycline
|
|
Day 2
|
103.2°F (39.6 °C)
|
4000
|
12.5
|
51,000
|
141
|
165
|
Jarisch-Herxheimer reaction
|
|
Day 3
|
99.7°F (37.5°C)
|
3400
|
12.7
|
45,000
|
127
|
148
|
Smear positive for Babesia Doxycycline continued Azithromycin and atovaquone started
|
|
Day 4
|
96.6°F (37.5°C)
|
3700
|
11.4
|
38,000
|
110
|
120
|
Afebrile, Feels better
|
Note: WBC: White blood cells; HGB: Hemoglobin; PLT: Platelets; AST: Aspartate amino transferase; ALT: Alanine aminotransferase
Splenomegaly, splenic inflammation and splenic rupture [11-15] are known to occur in Babesiosis. The source of left abdominal discomfort in cases 1 and 2 was the spleen. Case 1 did not have CT (computerized tomography) evidence of splenomegaly but in case 2 the spleen was enlarged. The LUQ discomfort appeared to be from splenic inflammation or splenomegaly. Thrombocytopenia, anemia, leukopenia and abnormal liver enzymes were clues to the possibility of a tick transmitted disease.
The Jarisch-Herxheimer Reaction (JHR) in case 2 was likely due to a mixed infection with Borrelia. The patient lived in an area endemic for B. burgdorferi and B. miyamotoi. Treatment of Borrelia, Treponema and Leptospira spirochetal infections have been associated with the Jarisch-Herxheimer reaction [16]. The antibody-based test done for B burgdorferi although specific is insensitive and unreliable for a definitive confirmation of Lyme disease [17].
In areas with tick-borne diseases physicians must be vigilant of unusual presentations that mimic common diseases to avoid misdiagnosis and inappropriate treatment.
In Lyme disease endemic areas, Babesia transmitted by the same tick vector may present as a single or mixed infection. Presence of thrombocytopenia and anemia is a clue to the diagnosis of babesiosis. Elevated liver enzymes and leukopenia should raise the suspicion of a mixed infection. In the 2 cases presented, left upper abdominal discomfort originating from the spleen was misdiagnosed for infections of the left kidney. Both patients initially received inappropriate antibiotic treatment. Frequently tick-borne diseases present with symptoms that mimic common conditions and are missed by clinicians [18]. Health care providers in tick endemic areas should be vigilant of uncommon presentations of tick transmitted diseases that could be easily misdiagnosed for common conditions.
- Vannier E, Krause PJ (2009) Update on babesiosis. Interdiscip Perspect Infect Dis doi:10.1155/2009/984568.
- Nassar Y, Richter S (2017) Babesiosis presenting as acute liver failure. Case Rep Gastroenterol 11: 769-773.
- Jia N, Zheng YC, Jiang JF, Jiang RR, Jiang BG, et al. (2018) Human Babesiosis caused by a Babesia crassa – like pathogen: A case series. Clin Infect Dis 67: 1110-1119.
- Kukina IV, Guzeeva TM, Zelya OP, Ganushkina LA (2018) Fatal human Babesiosis caused by Babesia divergens in an asplenic host. ID Cases 13: e00414.
- Zhao Y, Love KR, Hall SW, Beardell FV (2009) A fatal case of transfusion-transmitted babesiosis in the state of Delaware. Transfusion 49: 2583-2587.
- Rosner F, Zarrabi MH, Bnach JL, Habicht GS (1984) Babesiosis in splenectomized adults. Am J Med 76: 696-701.
- Healy GR, Walzer PD, Sulzer AJ (1976) A case of asymptomatic babesiosis in Georgia. Am J Trop Med 25: 376-378.
- Brennan MB, Herwaldt JJ, Kazmierczak JJ, Weis JW, Klein CL, et al. (2016) Transmission of Babesia microti parasites by solid organ transplantation. Emerg Infect Dis 22: 1869-1876.
- Aderinboye O, Syed SS (2010) Congenital Babesiosis in a four-week-old female infant. Pediatr Infect Dis 9: 188.
- Joseph JT, Purtill K, Wong SJ, Munoz J, Teal A, et al. (2012) Vertical transmission of Babesia microti, United States. Emerg Infect Dis 18: 1318-1321.
- Usatii N, Katrian A, Stratidis J (2014) Spontaneous splenic rupture due to Babesia microti infection: case report and review of literature. ID Cases 1: 63-65.
- Dumic J, Patel J, Hart M, Niendorf ER, Martin S, et al. (2018) Splenic rupture as the first manifestation of Babesia microti infection: A case report and review of literature. Am J case Rep 19: 335-341.
- Dkhil MA, Al-Quraishy S, Al-Khalifa MS (2014) The effect of Babesia divergens infection on the spleen of Mongolian gerbils. Biomed Res Int 2014: 483854.
- Ehret WJ, Potgeiter FT, De Waal DT, Van der Lugt JJ, Van der Vyver FH (1987) Chronic splenitis as a possible complicating factor in calves inoculated with an attenuated red water vaccine. J S Afr Vet Assoc 58:131-134.
- Inchley CJ (1987) The contribution of B-cell proliferation to spleen enlargement in Babesia microti infected mice. Immunology 60: 57-61.
- Butler T (2017) The Jarisch-Herxheimer reaction after antibiotic treatment of spirochetal infections: A review of recent cases and our understanding of pathogenesis. Am J Trop Med Hyg 96: 46-52.
- Kannangara DW, Patel P (2018) Report of Non-Lyme erythema migrans rashes from New Jersey with a review of possible role of tick salivary toxins. Vector borne Zoonotic Dis 18: 641-652.
- Patel P, Kannangara D, Sindhu S, Toshniwal R, Amit P, et al. (2018) A case series of unusual presentations associated with arthropod bites: cutaneous, cardiac, articular and other manifestations. Int J Infect Dis 73: 398.

