Opinion
A 23 year old female was admitted to The Invasive Cardiology Department in October 2013 with suspicion of pulmonary arterial hypertension (PAH) estimated by transthoracic echocardiography.18 and 34 year old cousins of the patient suffers from idiopathic PAH and another one died in age of 14 from PAH, what suggested familial PAH.
On admission patient presented NYHA (New York Heart Association) class III. Echocardiography revealed enlarged right ventricle (RV-47 mm), dilated pulmonary trunk, paradoxical motion of intraventricular septum, D-shaped left ventricle, pulmonary and tricuspid insufficiency with estimated RV systolic pressure (RVSP) 46 mmHg and mean pulmonary arterial pressure (mPAP) 34 mmHg. In the right heart catheterization (RHC) the following values were measured: RV–59/12(15) mmHg, PAP–56/45(51) mmHg, pulmonary capillary wedge pressure (PCWP)–7 mmHg, cardiac output-4,95 l/min, cardiac index-2,86 l/min/m2, PVR-15,3 Woods Units. Vasoreactivity test with iloprost reaveled negative response (PAP - 57/40(48) mmHg, PCWP-7 mmHg). The patient was qualified to treatment with Sildenafil (60 mg/day).
In January 2014 patient checked herself into outpatient’s department in the 3th week of pregnancy. Woman was informed of the extensive risk to her and her fetus.
During 30 weeks of pregnancy she had an estimated in echocardiography PAPs on 70mmHg and mPAP on 57 mmHg. The iloprost (6 inhalations/day) was added to sildenafil.
In 35th hbd patient’s state was moderate with symptomps in NYHA class IV. Cesarean section at 35-week gestation was decided, with subarachnoid analgesia. After uncomplicated newborn (APGAR score of 10, birth weight 2400g, crown-rump length 49cm) and placenta delivery, bradycardia (20 bpm) and hypotonia with nondetectable blood pressure occurred. Finally short sudden cardiac arrest was observed. Hemodynamic stability was recovered by ephedrine and atropine administration. During the following days patient’s condition was stable. PAH therapy (sildenafil, iloprost) was continued.
Three-year follow-up shows that the patient’s state was stable with NYHA class I.
Echocardiographic examination (Figure 1) displayed PAP 34 mmHg. The PAH therapy consists of sildenafil (60 mg/day) and iloprost (8 inhalation/day- vial 20 mcg/dL). In April 2017 she started to use Breelib, the new nebulizer for iloprost as a first patient outside clinical trials. The Breelib nebulizer was developed to provide a device specifically for iloprost inhalation, to reduce inhalation times and thereby to improve convenience for patients. After reduction iloprost dose (from 20 to 10 mcg/mL/inhalation) clinical condition improved. The Breelib nebulizer offers better absorption of iloprost in lungs and good tolerability. Just after switch she presented headache, redness of the face, without significant decrease of blood pressure.
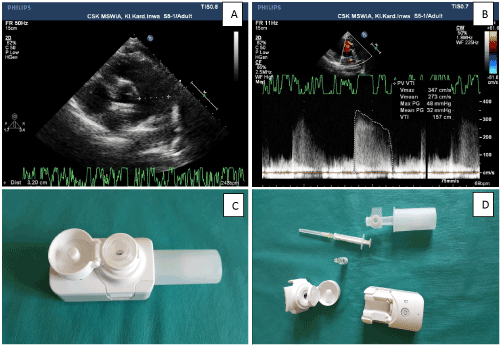
Figure 1. Echocardiographic assessment of pulmonary hypertension: A. enlargment of pulmonary trunk, B. Estimated pressure in pulmonary trunk, C&D Breelib nebulizer.
When initiation of therapy with BreelibTM is considered in patients treated previously with iNebTM nebulizer initial dose of iloprost should be reduced and subsequently increased only in case to ensure the good tolerance.

