In the last decades, glucose 5% injections have gained more interest [1-3]. Some have even compared its effectiveness to corticosteroid injections [4]. To bring more attention to this new technique, the term Glucopuncture was introduced in January 2021. Glucopuncture is a medical procedure which applies isotonic glucose injections for the management of non-rheumatic musculoskeletal conditions [5]. The technique consists of multiple injections of G5W (Glucose 5% in Water) in the region of complaint. Intradermal injections are given for pain modulation, intralesional injections are given in, for example, muscles, tendons, and ligaments to stimulate tissue repair. One can also apply these injections adjacent to peripheral nerve endings [6] or in the epidural space [7]. In this case report, both intradermal and intraligamentous injections were applied.
Pain modulation and tissue repair
Most hypotheses about glucose injections are focused on pain modulation (e.g., vanilloid receptors, neural inflammation, gate control). But these theories do not explain the beneficial effects of Glucopuncture on tissue repair. Apparently, local glucose injections support cellular function and consequently lead to less stiffness when injecting into muscle, and more joint stability when injecting into collateral bands or ligaments. To explain this functional component, a new hypothesis has been proposed, the ATP hypothesis.
The ATP hypothesis
Glucose is the major energy source for cellular health. One glucose molecule gives rise to more than 30 ATP molecules during the aerobic respiration. The conversion of ATP into ADP releases about 30 kJ/mol energy to the cells. In other words, glucose can be considered as a direct provider of energy (one molecule delivers more than 900 kJ/mol) to cell metabolism.
When tissues are damaged because of trauma, overuse or other causes, the cells need to regenerate as quickly as possible. This physiological tissue regeneration requires an additional amount of energy in the cells. In normal circumstances, energy supply is abundant to meet the higher demand. But when the need for ATP is elevated after an injury, there may be a temporary lack of ATP and as a result physiological recovery of that tissue may become impossible. The latter may lead to poor tissue healing. Providing extra glucose to the cells during these moments of repair might lead to extra ATP production. In this sense, it is hypothesized that Glucopuncture improves tissue repair of, for example, muscles, tendons, and ligaments. Unfortunately, there is not much research regarding the effects of ATP for pain modulation. However, it has been illustrated that ATP injection increases expression of several markers for regenerative activity in sensory neurons, including phospho-STAT3 and GAP43 [8].
The effect of glucose on tiny nerve branches
Especially peripheral nerve endings seem to respond well to adjacent glucose injections. One can approach the peripheral nerves directly, for example, when injecting close to the supraorbital nerve, suprascapular nerve, median nerve (carpal tunnel) or greater occipital nerve. But clinical experience has illustrated that it is not always necessary to inject adjacent to peripheral nerves. Injecting near finer nerve branches with glucose seems to be very interesting as well. These extremely tiny nerve endings are present in muscles, tendons, ligaments, and so on. These branches are not mentioned in the anatomy textbooks because they are extremely thin. That is why multiple injections are given in the entire region.
The effect of glucose on dermal sensory nociceptors
Sensory receptors are found everywhere in the body [9]. They are also abundant in dermis. These receptors include mechanoreceptors, nociceptors, and thermoreceptors. Especially dermal nociceptors are important to explain the pain modulating effects of Glucopuncture while injecting glucose intradermally.
Glucose transport across the cell membrane
Glucose is transported across the cell membrane [10] by a specific saturable transport system, which includes two types of glucose transporters: 1) sodium dependent glucose transporters (SGLTs) which transport glucose against its concentration gradient and 2) sodium independent glucose transporters (GLUTs), which transport glucose by facilitative diffusion in its concentration gradient.
The nonspecific effects of Glucopuncture include all clinical effects which are not related to the glucose itself. These explain why dry needling and water injections also have temporary effects on pain modulation.
Needle effect
Dry needling may act by reducing dorsal horn neuron activity, and by modulating brainstem areas [11]. Some articles [12] suggest that the physiological mechanism of dry needling includes a combination of peripheral effects (such as spinal [i.e., gate control] and supraspinal [i.e., endogenous opioid system] mechanisms). It is hypothesized that dry needling may activate the serotonergic (5-HT) and noradrenergic descending inhibitory systems, which in turn may decrease pain [13]. However, effects are usually seen at short-term and effect sizes are rather small [14].
Sensitization of the transient receptor potential ion channel vanilloid 1 (TRPV1) is critically involved in inflammatory pain [15]. Recent data demonstrate that TRPV1 is crucial for the needle effect and that it can initiate the excitatory pNR1-pCaMKII pathway, at peripheral DRG and central SC-SSC level [16]. Dry needling might downregulate proinflammatory neuropeptides, proinflammatory cytokines, and neurotrophins, and modulating transient receptor potential vanilloid [17-21].
Volume effect
Injecting a certain amount of liquid into the extracellular space creates a temporary local expansion and thus change of the extracellular pressure. The latter may influence the peripheral nerve endings in the extracellular matrix (ECM). This may explain partly the temporary pain modulating effects of intradermal water injections [22-25]. The extracellular matrix is a non-cellular three-dimensional macromolecular network composed of collagens, proteoglycans, elastin, fibronectin, and several other glycoproteins [26]. Recently, it has been investigated in more detail how extracellular matrix remodeling, ligand binding, and hemostasis are regulated by mechanical forces [27]. The viscoelasticity of the ECM plays a major role on cell behavior [28].
Bleeding effect
Each soft tissue injection can create a tiny bruising when the needle injures a blood vessel, small or large. This is especially true when injecting in muscular tissue. The more injections one gives and the thicker the needle, the more bleeding may occur in the tissue, thus creating a small amount of whole blood in the extracellular matrix. Blood contains platelets and growth factors, which may play a role in tissue regeneration [29]. It is widely accepted that platelets release substances that promote tissue repair and influence the reactivity of vascular and other blood cells in angiogenesis and inflammation [30]. Platelets contain storage pools of growth factors including PDGF, TGF-beta and VEGF as well as cytokines including proteins such as PF4 and CD40L [31].
Gate control effect
The gate control theory of pain describes the modulation of sensory nerve impulses by inhibitory mechanisms in the central nervous system [32]. Other important features include the convergence of small and large sensory inputs on spinal neurons that transmit the sensory information to the forebrain as well as the ability of descending control pathways to affect the biasing established by the gate [33]. The gate control theory according to Melzack and Wall proposes that Aβ mechanoreceptor inputs to spinal pain transmission T neurons are ‘gated’ (downregulated) via feedforward inhibition. Peripheral nerve stimulation exhibits its neuromodulatory effect both peripherally and centrally [34]. Prolonged relief may require the disruption of reverberatory neural circuits responsible for the "memory" of pain [35].
Placebo effect
Placebo is the use of a substance or procedure without specific activity for the condition that is trying to be treated [36]. Placebo effects are embodied psycho-neurobiological responses capable of modulating pain and producing changes at neurobiological and cognitive levels [37]. Over the past decades, the mechanisms underlying placebo effects have begun to be identified in more detail [38]. At the same time, placebo effects are also found in surgical trials, thereby posing the question whether non-pharmacological interventions such as surgical interventions should be placebo-controlled to a greater extent [39].
A 30-year-old architect (born October 7, 1990) came to the clinic for back pain which was present continuously for 5 years. The pain was localized in the dorsal back region. He had had several previous treatments, including physiotherapy and manual therapy. The physiotherapeutic measures did not help him. Dorsal spine manipulations lessened the pain for about half a day and then recurred (Figure 1).
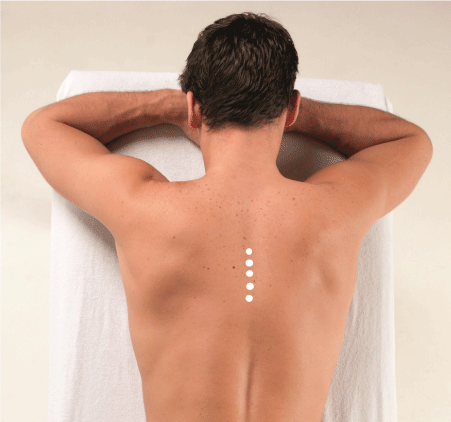
Figure 1. GP Dorsal Ligament G5W Casus
On his first visit (March 16, 2021), he mentioned both chronic pain between his shoulder blades and regular “clicking” of the dorsal spine. He could not recall how the pain had started. No X-rays or scans were available.
During clinical examination, putting a thumb on the supraspinal ligament on several points in the mid-dorsal region evoked ‘his’ pain immediately. Because of this clinical finding, it was hypothesized that he suffered from ligamentous pain on the dorsal level. The ligament involved was most likely the supraspinal ligament and not the interspinal ligament because only light pressure was required to evoke the pain. As a test, he received intradermal injections (SC) with Lidocaine 0.2% into the pain region (5 x 1 mL). These injections on the midline of the back did not provide any improvement of the clinical picture.
On the second visit (March 23), he received intradermal injections (SC: subcutaneous) with Glucose 5% (G5W) into the pain region (5 x 1 mL). No local anesthetics were added. After this first Glucopuncture session, he noticed a slight improvement of the pain for a few hours. However, the clicking in the dorsal back did not change. As glucose 5% injections typically produce short term results in the beginning, it was explained to the patient that a series of sessions is required.
On the third visit (March 30), he received intradermal injections (SC) with G5W into the pain region, and at the same time palpation guided intraligamentous injections (IL) with G5W (less than 1 cm deep). No local anesthetics were added. After these injections (5 x 1 mL), he saw a substantial improvement of the pain for a few days. The clicking in the dorsal back was slightly better as well. The latter may indicate that the injections are not only working on pain modulation but also on tissue repair.
On the fourth visit (April 15), he received again intradermal injections (SC) with G5W into the pain region, and intraligamentous injections (IL) with G5W (less than 1 cm deep). Again, no local anesthetics were added. After these injections (5 x 1 mL), he was pain free for a whole week. The clicking in the dorsal back had disappeared completely.
On the fifth visit (April 22), he was still pain free. In other words, his pain had disappeared after three Glucopuncture sessions. He did not receive further treatment for that lesion at the fifth visit. The patient was asked to send an email when the pain would reoccur. During the fifth visit, he was treated for a new injury (muscle tear). Long term follow-up was planned to check out the effects of G5W on the long term. If the complaints would recur, an MRI would be interesting to rule out underlying pathologies which require a more specific treatment.
As dorsal back pain is very prevalent, it is important that patients have access to treatment modalities which are safe and effective. Several clinicians worldwide have experienced that glucose 5% injections are an interesting treatment modality for non-rheumatic musculoskeletal conditions. More clinical research is necessary to confirm its use to modulate back pain and to support ligament repair. As G5W is an inexpensive solution and this technique does not require fluoroscopy or ultrasound guidance, this approach may become an interesting option for patients in low-income countries (see also www.glucopuncture.com).
The author declares that there are no conflicts of interest or source of funding. The patient has provided a written permission by email to use his medical file for this case report. The author declares that he is the practitioner who has given the regional injections, exactly as described above.
- Mansız-Kaplan B, Nacır B, Pervane-Vural S, Genç H (2020) Pain relief in a patient with snapping scapula after 5% dextrose injection. Turk J Phys Med Rehabil 66: 368-369. [Crossref]
- Özlem Köroğlu, Aydan Örsçelik, Özlem Karasimav, Yasin Demir, İlker Solmaz (2019) Is 5% dextrose prolotherapy effective for radicular low back pain? Gulhane Medical Journal 61: 123-127.
- Lyftogt John (2007) Subcutaneous prolotherapy treatment of refractory knee, shoulder, and lateral elbow pain. Australasian Musculoskel Med 12: 107-109.
- Amanollahi A, Asheghan M, Hashemi SE (2020) Subacromial corticosteroid injection versus subcutaneous 5% dextrose in patients with chronic rotator cuff tendinopathy: A short-term randomized clinical trial. Interventional Medicine and Applied Science IMAS 11: 154-160.
- Kersschot J (2021) Treatment of Sports Injuries with Glucopuncture. Archives in Biomedical Engineering & Biotechnology 5: 2021.
- García-Triana SA, Toro-Sashida MF, Larios-González XV, Fuentes-Orozco C, Mares-País R, Barbosa-Camacho FJ (2020) The Benefit of perineural injection treatment with dextrose for treatment of chondromalacia patella in participants receiving home physical therapy: A pilot randomized clinical trial. J Altern Complement Med 20.
- Maniquis-Smigel L, Reeves KD, Rosen JH (2017) Short term analgesic effects of 5% dextrose epidural injection for chronic low back pain. A randomized controlled trial. Anesth Pain Med 7: e42550.
- Wu D, Lee S, Luo J, Xia H, Gushchina S (2018) Intraneural Injection of ATP stimulates regeneration of primary sensory axons in the spinal cord. J Neurosci 38: 1351-1365.
- Wade NJ (2019) Microscopic anatomy of sensory receptors. J Hist Neurosci 28: 285-306.
- Jurcovicova J (2014) Glucose transport in brain - effect of inflammation. Endocr Regul 48: 35-48. [Crossref]
- Pourahmadi M, Mohseni-Bandpei MA, Keshtkar A, Koes BW, Fernández-de-Las-Peñas C (2019) Effectiveness of dry needling for improving pain and disability in adults with tension-type, cervicogenic, or migraine headaches: protocol for a systematic review. Chiropr Man Therap 26: 27:43.
- Linde K, Allais G, Brinkhaus B, Manheimer E, Vickers A (2009) Acupuncture for tension-type headache. Cochrane Database Syst Rev 21: CD007587.
- Cagnie B, Dewitte V, Barbe T, Timmermans F, Delrue N (2013) Physiologic effects of dry needling. Curr Pain Headache Rep 17: 348.
- Fernández-de-Las-Peñas C, Nijs J (2019) Trigger point dry needling for the treatment of myofascial pain syndrome: current perspectives within a pain neuroscience paradigm. J Pain Res 12: 1899-1911.
- Sondermann JR, Barry AM, Jahn O, Michel N, Abdelaziz R (2019) Vti1b promotes TRPV1 sensitization during inflammatory pain. Pain 160: 508-527.
- Chen HC, Chen MY, Hsieh CL, Wu SY, Hsu H (2018) TRPV1 is a responding channel for acupuncture manipulation in mice peripheral and central nerve system. Cell Physiol Biochem 49: 1813-1824.
- McDonald JL, Cripps AW, Smith PK (2015) Mediators, receptors, and signalling pathways in the anti-inflammatory and antihyperalgesic effects of acupuncture. Evid Based Complement Alternat Med 15: 975632.
- Guo ZL, Fu LW, Su HF, Tjen-A-Looi SC, Longhurst JC (2018) Role of TRPV1 in acupuncture modulation of reflex excitatory cardiovascular responses. Am J Physiol Regul Integr Comp Physiol 314: R655-R666.
- Chen HC, Chen MY, Hsieh CL, Wu SY, Hsu HC (2018) TRPV1 is a responding channel for acupuncture manipulation in mice peripheral and central nerve system. Cell Physiol Biochem 49: 1813-1824.
- Huang W, Kutner N, Bliwise D (2013) Complexity of sham acupuncture. JAMA Intern Med 22: 173. [Crossref]
- Dimitrova A, Murchison C, Oken B (2017) Acupuncture for the treatment of peripheral neuropathy: A systematic review and meta-analysis. J Altern Complement Med 23: 164-179.
- Mårtensson L, Nyberg K, Wallin G (2000) Subcutaneous versus intracutaneous injections of sterile water for labour analgesia: a comparison of perceived pain during administration. BJOG 107: 1248-1251.
- Lee N, Kildea S, Stapleton H (2017) “No pain, no gain”: The experience of women using sterile water injections. Women and Birth 30: 153-158.
- Almassinokiani F, Ahani N, Akbari P, Rahimzadeh P, Akbari H (2020) Comparative analgesic effects of intradermal and subdermal injection of sterile water on active labor pain. Anesth Pain Med 10: e99867.
- Lee N, Webster J, Beckmann M, Gibbons K, Smith T (2013) Comparison of a single vs. a four intradermal sterile water injection for relief of lower back pain for women in labour: a randomised controlled trial. Midwifery 29: 585-591.
- Theocharis AD, Skandalis SS, Gialeli C, Karamanos NK (2016) Extracellular matrix structure. Adv Drug Deliv Rev 97: 4-27.
- Hoffmann GA, Wong JY, Smith ML (2019) On force and form: Mechano-biochemical regulation of extracellular matrix. Biochemistry 58: 4710-4720.
- Chaudhuri O, Cooper-White J, Janmey PA, Mooney DJ, Shenoy VB (2020) Effects of extracellular matrix viscoelasticity on cellular behaviour. Nature 584: 535-546. [Crossref]
- Amable PR, Carias RB, Teixeira MV, da Cruz Pacheco I, Corrêa do Amaral RJ (2013) Platelet-rich plasma preparation for regenerative medicine: optimization and quantification of cytokines and growth factors. Stem Cell Res Ther 4: 67.
- Anitua E, Andia I, Ardanza B, Nurden P, Nurden AT (2004) Autologous platelets as a source of proteins for healing and tissue regeneration. Thromb Haemost 91: 4-15.
- Anitua E, Andia I, Ardanza B, Nurden P, Nurden AT (2004) Autologous platelets as a source of proteins for healing and tissue regeneration. Thromb Haemost 91: 4-15.
- Melzack R (1981) Myofascial trigger points: relation to acupuncture and mechanisms of pain. Arch Phys Med Rehabil 62: 114-117.
- Mendell LM (2014) Constructing and deconstructing the gate theory of pain. Pain 155: 210-216.
- Zhang Y, Liu S, Zhang YQ, Goulding M, Wang YQ (2018) Timing mechanisms underlying gate control by feedforward inhibition. Neuron 99: 941-955.
- Melzack R (1981) Myofascial trigger points: relation to acupuncture and mechanisms of pain. Arch Phys Med Rehabil 62: 114-117.
- Dobrila-Dintinjana R, Nacinović-Duletić A (2011) Placebo in the treatment of pain. Coll Antropol 2: 319-323.
- Rossettini G, Carlino E, Testa M (2018) Clinical relevance of contextual factors as triggers of placebo and nocebo effects in musculoskeletal pain. BMC Musculoskelet Disord 19: 27.
- Damien J, Colloca L, Bellei-Rodriguez CÉ, Marchand S (2018) Pain modulation: From conditioned pain modulation to placebo and nocebo effects in experimental and clinical pain. Int Rev Neurobiol 139: 255-296. [Crossref]
- Vase L, Wartolowska K (2019) Pain, placebo, and test of treatment efficacy: a narrative review. Br J Anaesth 123: e254-e262.

