Abstract
Introduction: Computed Tomography (CT) is the most widely utilised imaging modality in the adult trauma setting. Accurate interpretation is vital for the appropriate management to be instigated. Given that many radiology training programs do not expose trainees to significant volumes of major trauma, we surmised that there was a need for a dedicated trauma teaching program. Our aim was to determine how confident radiology registrars and radiologists are when reporting trauma and to develop an online teaching trauma case series that will enable them to improve their competency and confidence.
Methods: A list of the trauma pathologies to cover in the case series was compiled in consultation with radiology consultants at a level one trauma centre. A questionnaire was designed to collect information from participants accessing the series.
Results: Multiple trauma CTs were reviewed and 25 were selected, covering all of the trauma pathologies on the generated list. These cases form a teaching series accessible on Radiopaedia.org. Participants are able to scroll through the images and are provided with the findings and teaching points. Eighty-nine radiology registrars and radiologists completed the case series. Forty-four percent reported that they were not exposed to high level trauma during their radiology training. Fifty-two percent stated that they reported trauma frequently or routinely. Forty-seven percent were not confident reporting trauma CTs.
Conclusion: Exposure to trauma radiology is highly variable and a substantial number of radiology trainees and radiologists are not confident reporting trauma CT scans. This comprehensive online trauma case series serves as a valuable teaching tool and resource.
Key words
trauma, teaching, e-learning, radiology, case series
Introduction
Imaging plays a vital role in the initial assessment and management of major trauma. Computed tomography (CT) is the key modality used in the trauma setting and an accurate interpretation of the CT is required in order for the appropriate management to be instigated. Interpreting trauma CT is therefore an important skill for all radiologists to have. The teaching radiology registrars receive on trauma as well as the level of trauma they are exposed to, varies significantly depending on the sites at which they train. Once qualified, radiologists may be exposed to high level trauma if they work in a level 1 trauma centre, in a remote area or for a tele-radiology company.
Trauma patients present around-the-clock to emergency departments (ED). In many public hospitals a single radiology trainee is responsible for reporting all after hours CTs and a recent study of accredited training facilities in Australia and New Zealand showed a 16.2% increase in the number of ‘out of hours’ ED CTs performed between 2011 and 2013 [1]. Some hospitals are also opting to utilise teleradiology companies to report after-hours studies.
Through our work in a level 1 trauma centre that employs both radiology trainees and tele radiology services for out of hours trauma imaging, we saw the need for a trauma teaching program for radiology registrars as well as radiologists who are not regularly exposed to high level trauma. Case based learning was chosen as the method to deliver the teaching series as this is the best way to mimic what happens in real life [2]. Furthermore, designing an e-learning resource and making it available online, would enable it to be accessed by a large audience at any time, from any location.
Method
Consultant radiologists at The Royal Melbourne Hospital were emailed a comprehensive list of important trauma pathologies. They were asked to contribute to the list to ensure it was all-inclusive.
To obtain cases to include in the teaching series, the supervising radiologist’s extensive trauma film library was reviewed to find cases that were the best possible teaching examples. Following this, a word search of the Radiology Information System was performed to find additional cases. Departmental radiology consultants and registrars were also asked to contribute cases. Subsequently the trauma study list generated was reviewed in consultation with two consultant radiologists with trauma expertise (DS who has 19 years experience working in a level 1 trauma centre and CH who has 9 years experience working in a trauma centre) to select cases that were the most useful teaching examples.
The short-listed studies were uploaded to form a case series accessible via the "Playlists" platform hosted by Radiopaedia.org (http://bit.ly/traumaradcases).
A short questionnaire was designed to collect information from participants completing the case series. Information was collected on their level of training, exposure to high level trauma, current trauma reporting practice and confidence reporting trauma.
Results
The list of trauma pathologies compiled that were covered in the case series is provided in Table 1.
Table 1. List of the trauma pathologies compiled and covered in the case series.
Chest |
Abdomen/pelvis |
Brain and Face |
Spine |
Aortic injury |
Liver trauma |
Epidural haematoma |
Atlanto-occipital disassociation |
Tension pneumothorax |
Splenic haematoma |
Skull base fracture |
C1/2 fractures |
Haemopericardium |
Collecting system leak |
Petrous temporal bone fracture |
Dens fracture |
Pulmonary contusion |
Mesenteric injury |
Subdural haematoma |
Flexion/extension injuries |
Flail Chest |
Bowel injury |
Epidural haematoma |
Perched facets |
Mediastinal haematoma |
Free intraperitoneal gas |
Diffuse axonal injury |
Three column spinal injuries |
Pneumatocele |
Adrenal haemorrhage |
Cerebral contusion |
|
Sternal fracture |
Pancreatic laceration |
Subarachnoid haemorrhage |
|
Oesophageal injury |
Traumatic ascites |
Depressed skull fracture |
|
Tracheal injury |
Active bleeding in the abdomen |
Nasal bone fracture |
|
Drop lung |
Unstable pelvic fractures |
Le Fort fracture |
|
Pneumomediastinum |
Sacroiliac joint disruption |
Orbital wall fractures |
|
Penetrating trauma |
Bladder rupture |
Globe rupture |
|
|
Placental abruption |
Tripod fracture |
|
|
Penetrating injury |
Mandible fracture |
|
Over 150 trauma studies were identified for review. Twenty-five cases were ultimately selected to cover all of the trauma pathologies on the list. This meant that many cases had multiple pathologies. Cases were also selected that had anatomical variants that can mimic trauma. The majority of cases include a whole body trauma CT (Pan-Scan), including both normal and abnormal regions. Participants are able to scroll through the series of images and are provided with different window settings to reflect what they would have available in real life. There are teaching questions with answers linked to each case and at the end of each case, the findings are described. Following each case, comprehensive teaching points applicable to the case are provided. Participants are able work through the series at their own pace in one or more sittings.
The case series has been distributed to all radiology trainees in Australia and New Zealand as well as to tele-radiology companies.
A total of 89 radiology registrars and radiologists have completed the case series. The majority of participants (74%) were radiology registrars or radiologists who had only recently completed their radiology training. Forty-four percent of participants reported that they were not exposed to high level trauma during their radiology training (Figure 1). Regarding current trauma CT reporting, 48% of participants reported that they rarely (<2 times per month) or infrequently (3-5 times per month) reported trauma cases (Figure 2). The remainder (52%) stated that they report trauma frequently (6-10 times per month) or routinely (>10 times per month). Forty-seven percent of participants were ‘not confident at all’ or ‘not very confident’ reporting trauma, whilst 48% were ‘confident’ (Figure 3). Only 5% were very confident. A small number of participants answered the question about how confident they were reporting trauma CTs after completing the case series, with all responding that they were now ‘confident’ or ‘very confident’.
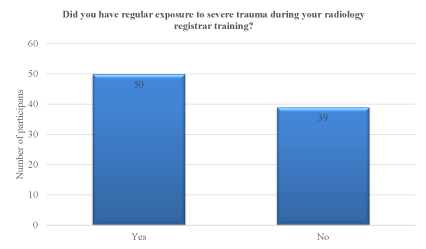
Figure 1. Participants’ response to the question “Did you have regular exposure to severe trauma during your radiology registrar training?”.
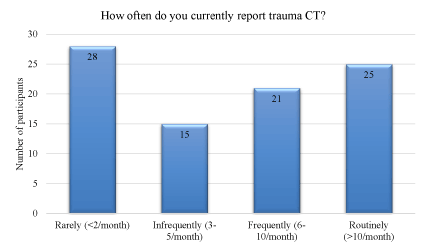
Figure 2. Participants’ response to the question “How often do you currently report trauma CT?”.
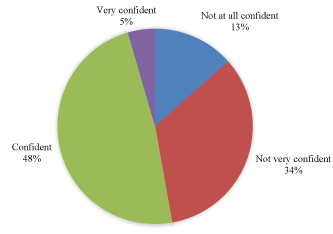
Figure 3. Participants’ response when asked their diagnostic confidence when reporting trauma CTs.
Discussion
CT is the most widely utilised imaging modality in the adult trauma setting. Correctly identifying injuries on CT in a timely manner is of utmost importance as it can significantly affect the early management a patient receives and thus their outcome [3,4]. Although on-the-job training provides invaluable learning experiences, reviewing cases in a safe environment within tutorials and through self-directed learning, is also necessary. This increases the likelihood of a radiologist making a correct diagnosis and forms the basis of all radiology training programs. The fact that almost fifty percent of participants were ‘not confident at all’ or ‘not very confident’ reporting trauma confirms the need for more trauma radiology education than most trainees currently receive. This probably reflects the fact that major trauma is sequestered at select sites in most cities/countries around the world.
The number and variety of injuries that may be seen on trauma CTs is immense. Whilst it is not possible to include an example of every possible injury in a teaching series, we felt that by including the most common and important injuries, participants completing the case series would be well equipped to report. Furthermore, as the series provides teaching notes on each case, participants learn about the mechanisms of injuries, what associated injuries to look for, which injuries need urgent attention and what the management might entail. We chose to include the whole body trauma CT (Pan-Scan) for many cases, including both normal and abnormal regions, as this also allows participants to practise detection.
Trauma patients present around-the-clock. Outside of normal working hours, a single radiology registrar is usually responsible for reporting all after hours CTs [1]. It can be several hours before a consultant radiologist reviews the CTs and thus it is the interpretation of the CT by the registrar that drives the initial management. Missing or misdiagnosing certain injuries has the potential to drastically alter patient treatments and outcomes. The RANZCR have developed a list of key conditions, many of which are trauma related, and teaching of these is mandatory before registrars go on-call [5]. However, a recent survey of Australian and New Zealand radiology registrars reported that only 30% agreed or strongly agreed that their teaching adequately prepared them for being on-call [6]. In this study, 52% reported that they only received 1 to 5 teaching sessions to cover these key conditions [6]. Given the number of key conditions listed, this is unlikely to be sufficient to cover all the topics. The teaching trauma case series we have created covers all of the major trauma topics on the key conditions list [5]. In our level 1 trauma centre, completing the trauma teaching series is now mandatory for all first year registrars before they go on-call. Of the participants who have completed our teaching trauma series so far, the majority have been radiology registrars.
Radiology registrars are not the only group who can benefit from completing this case series. Radiology trainees are exposed to varying degrees of trauma depending on where they train and hence as radiologists, their competence when reporting trauma will also vary. Radiologists may be required to report trauma if they work in a level 1 trauma centre, in a remote area or for a tele-radiology company that reports for trauma centres. In these situations, CTs will not routinely be reviewed by a second radiologist and hence it is vital that the initial report is interpreted accurately. Any radiologist who reports trauma, especially those who report it infrequently, would benefit from completing our trauma case series.
Providing education via e-learning platforms is becoming increasingly popular given the ease at which the internet can be accessed [7]. A systematic review of e-learning in radiology was recently published [9]. This included 19 articles all of which evaluated e-learning tools for undergraduate medical students. Only two studies have been identified that have evaluated an e-learning program designed for radiology trainees [6,10]. The benefits of an online teaching program include the ability to access it any time, from any location [8] which is particularly important given increasing workloads which can make protected teaching time difficult to obtain. E-learning also enables participants to work through the content at their own pace, thus enabling them to focus on topics they are less familiar with [8].
Radiology being an image-based speciality, lends itself particularly well to e-learning. In particular, because the Radiopaedia.org platform offers the option of uploading stacks of images, participants are able to scroll through a CT study. This enhances the learning experience as not only is it more engaging but it also closely mimics real life practice.
Conclusion
Exposure to trauma radiology is highly variable and a substantial number of radiology trainees and radiologists are not confident reporting CT scans for major trauma. We believe that all radiology trainees, radiologists and other doctors who are exposed to trauma would benefit from accessing this e-learning teaching trauma case series. The case series can be accessed at: http://bit.ly/traumaradcases.
References
- Goergen SK, Grimm J2021 Copyright OAT. All rights reserv016) Audit of demand for after-hours CT scanning services in RANZCR-accredited training departments. J Med Imaging Radiat Oncol 60: 35-46.
- Towbin AJ, Paterson BE, Chang PJ (2008) Computer-based simulator for radiology: an educational tool. Radiographics 28: 309-316. [Crossref]
- Stephen DJ, Kreder HJ, Day AC, McKee MD, Schemitsch EH, et al. (1999) Early detection of arterial bleeding in acute pelvic trauma. J Trauma 47: 638-642. [Crossref]
- Romano L, Giovine S, Guidi G, Tortora G, Cinque T, et al. (2004) Hepatic trauma: CT findings and considerations based on our experience in emergency diagnostic imaging. Eur J Radiol 50: 59-66.
- The Royal Australian and New Zealand College of Radiologists (2014) Radiodiagnosis Training Program Curriculum. Sydney. Retrieved from The Royal Australian and New Zealand College of Radiologists website: https://www.ranzcr.com/trainees/clinical-radiology/curriculum.
- Knipe H, Runciman J, Paks M, Ren Y, Phal P, et al. (2014) Teaching radiology key conditions: New e-learning tutorials with local and international feedback. Poster presented at: Combined Scientific Meeting - "Imaging and Radiation in Personalised Medicine", September 4-7; Melbourne, Australia.
- Pinto A, Brunese L, Pinto F, Acampora C, Romano L (2011) E-learning and education in radiology. Eur J Radiol 78: 368-371. [Crossref]
- den Harder AM, Frijlingh M, Ravesloot CJ, Oosterbaan AE, van der Gijp A (2016) The Importance of Human-Computer Interaction in Radiology E-learning. J Digit Imaging 29: 195-205. [Crossref]
- Bister P, Bister D, Markless S (2014) The Role of E-Learning in Radiology Training in the UK. Poster presented at: European Society of Radiology, March 6-10; Vienna, Austria.
- Sparacia G, Cannizzaro F, D'Alessandro DM, D'Alessandro MP, Caruso G, et al. (2007) Initial experiences in radiology e-learning. Radiographics 27: 573-581. [Crossref]



