Occipitocervical fusion is a common surgical method to treat cervical spine instability caused by atlantoaxial joint dislocation, upper cervical spine injury and degenerative disease of upper cervical spine. However, there are serious complications after occipitocervica fusion, which may even threaten the life of the patient. Airway management may be challenging in patients undergoing OCF. Changes in the occipital neck fusion Angle after surgery may lead to acute airway obstruction, dyspnea and/or dysphagia. The purpose of this study was to review the airway management of the latter patient, determine the incidence, nature and risk factors of postoperative airway adverse events, and determine the relationship between airway adverse events and changes in dOC2A. Factors such as difficulty in intubation, degree of vertebral fusion, and operation time should be considered. The o-c2 Angle is an independent medical factor that determines postoperative dyspnea and dysphagia, which should be mainly considered.
occipitocervical fusion, cervical spine, joint dislocation
The patient is male and 73 years old. Preoperative diagnosis: atlantocone comminuted fracture, atlantoaxial joint subluxation, brain contusion and laceration, right frontal and temporal bone fractures, right zygomatic arch fractures, calf intermuscular vein thrombosis. Induction of intravenous general anesthesia, loss of consciousness and muscle relaxation were followed by UE visual laryngoscope, combined with visible glottis exposure, and the No. 7.5 strengthened tracheal catheter was inserted through the mouth. Cervical occipital fixation (C3 and occipital protuberance fixation) was performed in prone position. The operation time was 2 hours and 27 minutes. The blood loss was 120ml.
Supine position was restored after the operation and sputum aspiration was observed. After the patient's consciousness was restored, the patient could shake hands, and the tidal volume of spontaneous breathing reached 8ml/kg, the tracheal catheter was pulled out. The patient has wheezing in the airway, oxygen is given to the mask, and the patient cannot open his mouth when trying to breathe sputum. After 3min, the blood oxygen saturation was not maintained well, which decreased from 87% to 60%. Emergency UE laryngoscope was performed to expose the glottis, and the patient had difficulty opening his mouth. Only epiglottis is visible. Blind intubation is attempted. Fails. Continue mask oxygenation. Call for assistance.
1min later, colleagues from the department arrived to assist in mask assisted ventilation, and the patient's SPO2 was maintained at 95%. Intravenous propofol and cisatracurium were injected. After another attempt to expose the glottis with UE laryngoscope, it was found that the patient's mandibular joint was stiff, the laryngeal wall was bleeding, and the endotracheal intubation failed again. Continue mask assisted ventilation, patient SPO2 can maintain 93%, ventilation resistance at 30cm water column. Attempts to intubate via nasal fiberoptic bronchoscopy failed, and SPO2 was only maintained by 88% of patients. Contact the otolaryngologist. The otolaryngologist arrived 3 minutes later for tracheotomy and the tracheotomy cannula was inserted 3 minutes later. Patients with SPO2 can maintain 98%, blood pressure at 160/80mmhg. Transport to ICU after full discharge of accumulated CO2.
The patient returned to the spinal surgery ward 6 days later and was found to have dislocated mandibular joint. Eight days after the operation, the patient underwent manual reduction in oral surgery, and had difficulty breathing. 14 days after surgery, the otorhinolaryngology department closed the tracheostomy, and the mandibular joint manual reduction was performed. The patient suffered from dyspnea and dysphagia, and the tracheotomy was performed again 16 days after the surgery. Electronic laryngoscope examination showed chronic congestion of the mucosa of the pharynx, no redness and swelling in the epiglottis, poor movement, only 5mm gap between the epiglottic laryngeal surface and the posterior pharyngeal wall, and the glottis could not be seen 。There was still mandibular joint dislocation after maxillary arch splint fixation 28 days after surgery.
Dysphagia continued to exist. The patient's dysphagia lasted for 60 days after consultation with the department of oral and traditional Chinese medicine rehabilitation, which was considered to be related to anatomical changes.
Obstruction of the upper respiratory tract is a serious complication of high cervical spine surgery. Especially in the neck OCF surgery, although it is not common but very critical. After cervical spine surgery, including anterior, posterior and anterior combined surgery, the incidence of postoperative airway complications is about 1.7 ~ 7% [1]. The rate of reintubation after posterior cervical surgery was 3.9% [1], while the rate of reintubation after anterior and posterior combined cervical surgery was 1.7% ~ 30% [2]. Potential causes of postoperative cervical obstruction include pharyngeal edema, hematoma, cerebrospinal fluid leakage, fixation of cervical hyperflexion, neurogenic edema, and recurrent laryngeal nerve injury [3].
In this case, the airway obstruction occurred immediately after extubation. Preoperative fractures of the right frontal bone and temporal bone co-existed, and the right zygomatic arch fracture resulted in the patient's obviously limited cervical spine fixation and the failure of re-intubation. The patient's pharyngeal cavity was narrowed and the epiglottis was difficult to lift.
Some cases of postoperative upper respiratory tract obstruction due to excessive cervical flexion were reported. Yoshida reported a case of upper respiratory tract obstruction after cervical spine fusion, and the cervical spine was restored to neutral position after correction of fixed Angle, and the obstruction disappeared immediately [4]. Lee also reported a case of cervical metastatic tumor in which upper respiratory tract obstruction occurred after OCF, and tracheotomy was performed after several failed intubation attempts [5]. In the case of Tsuyoshi, upper respiratory obstruction also occurred after OCF. After successful endotracheal intubation, corrective surgery was performed, and the postoperative obstruction was immediately relieved [6].
Risk factors for complications of OCF were analyzed abroad, and several risk factors were summarized, including the number of fused vertebral bodies (>, 6), the existence of difficulty in intubation, and the operation time (>, 5 hours), which were significantly correlated with airway complications. In this case, the combination of visible glottic exposure during anesthesia induction belongs to the potential difficult airway. Anatomical changes were also considered. OC2A is defined as the Angle between the macgregor line (a line drawn from the back up) from the hard jaw to the caudal point on the occipital midline and the lower endplate line of C2. Changes in OC2A angles, differences between postoperative and preoperative angles, have been identified as a possible cause of acute upper airway obstruction. This may be due to the reduced cross-sectional area of the oropharyngeal cavity, resulting in a smaller gap between the epiglottis and the pharyngeal wall.
In this case, the preoperative O-C2 Angle was -4.4°, and the postoperative O-C2 Angle was -18.6°, and the change of O-C2 Angle was -14.2° (Figure 1).
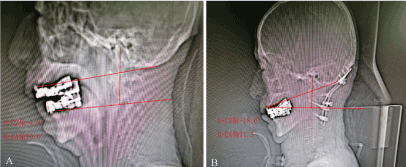
Figure 1. A shows the preoperative CT of the patient with o-c2 Angle of -4.4° and o-ea Angle of 79.9°; B shows the postoperative CT of the patient with o-c2 Angle of -18.6° and o-ea Angle of 71.3°
Dyspnea and dysphagia are more common in anterior cervical surgery, and cervical posterior surgery with OCF is the cause of dyspnea and dysphagia. In this case, extubation immediately resulted in respiratory distress, failure of intubation again, failure of fiberoptic bronchoscopy, and tracheotomy was performed. The analysis of possible causes is of clinical significance to avoid the serious complications of this kind of surgery. The operation time was short and the prone position time was short. Although the cause of oropharyngeal edema could not be completely excluded, no obvious oropharyngeal edema was found through the nasal bronchoscopy. Therefore, we suspect that the cause of postoperative acute upper airway obstruction was caused by physical stenosis of the oropharynx, resulting from a reduced O-C2 angle. Postoperative dysphagia was also significantly associated with changes in O-C2 (Figure 2).
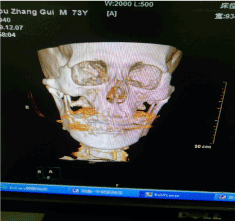
Figure 2. Maxillofacial CT reconstruction
The O-C2 angle should be a most important factor in preventing postoperative complications such as dyspnea and dysphagia and being easily measured during surgery, can be used as a practical and reliable indicator during surgery.
- 1.Wattenmaker I, Concepcion M, Hibberd P, Lipson S (1994) Upper-airway obstruction and perioperative management of the airway in patients managed with posterior operations on the cervical spine for rheumatoid arthritis. J Bone Joint Surg Am 76: 360-365.
- 2.Terao Y, Matsumoto S, Yamashita K, Takada M, Inadomi C, et al. (2004) Increased incidence of emergency airway management after combined anterior-posterior cervical spine surgery. J Neurosurg Anesthesiol 16: 282-286.
- 3.Sheshadri V, Moga R, Manninen P, Goldstein CL, Rampersaud YR, et al. (2017) Airway adverse events following posterior occipito-cervical spinal fusion. J Clin Neurosci 39: 124-129.
- 4.Yoshida M, Neo M, Fujibayashi S, Nakamura T (2007) Upper-airway obstruction after short posterior occipitocervical fusion in a flexed position. Spine 32: E267-E270.
- 5.Lee YH, Hsieh PF, Huang HH, Chan KC (2008) Upper airway obstruction after cervical spine fusion surgery: role of cervical fixation angle. Acta Anaesthesiol Taiwan 46: 134-137.
- 6.Tagawa T, Akeda K, Asanuma Y, Miyabe M, Arisaka H, et al. (2011) Upper airway obstruction associated with flexed cervical position after posterior occipitocervical fusion. J Anesth 25: 120-122.


