The patient arrives with his symptoms; the doctor prescribes a drug or gives advice. What really happens during the consultation in general medicine? What really happens in the short time of 10 minutes? It is a magical moment. The general practitioner (GP) in a few minutes makes a diagnosis and prescribes a treatment. How can the GP do that? Where does this magic reside? Mainly it is in the doctor-patient relationship. But where lays the enormous diagnostic and therapeutic potential of the doctor-patient relationship?
There is a lack of data on the mechanisms and tools, in diagnosis and treatment, of the doctor-patient relationship. We must investigate the nature of this transaction that takes place between the patient and his doctor, and the factors that are involved in that doctor-patient relationship. The doctor-patient relationship is a professional, complex, multiple and heterogeneous social relationship.
But, it can be said that, this relationship, generally continued over time, allows the GP to: 1) Know a large amount of biopsychosocial data of the patient and its context in a way that facilitates successive diagnoses and treatments; 2) The form taken by the doctor-patient relationship, in itself, provides valuable information to interpret the reasons for consultation; 3) The doctor-patient relationship itself is therapeutic; And 4) The doctor-patient relationship is the main factor that influences compliance with treatment. These elements fit together and allow the GP to build the patient's clinical care (Figure 1).
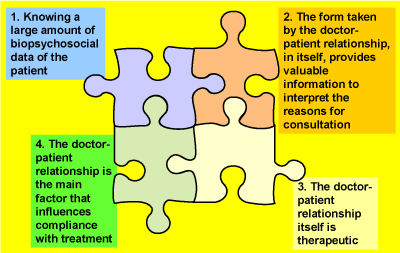
Figure 1. The doctor-patient relationship, generally continued over time, allows GP “to build the puzzle" of patient care.
The sense of "clinical expertise" is associated with the ability to manage the uncertainty of the query. Clinical judgments cannot be true or false in the abstract (in the generalization of the protocol), but case by case. The doctor-patient relationship frames the specific context of each "clinical case" of each patient [1,2].
The doctor-patient relationship implies different decision-making models (diagnostic and treatment). Since the symptoms are subjective evidences of health problems and are expressed differently according to the context of the doctor-patient relationship, this variable limits the degree to which the physician obtains psychosocial information from the patient, and involves different diagnoses, and treatment [3].
In addition, for the proper understanding of the reason for consultation, the GP usually needs to pass from the material manifested by the patient initially, to the latent and unexpressed material. In this way, the GP can transform a slightly understandable material into a broader, more comprehensive and more comprehensible material. In this basic process, which begins the preparation of the diagnosis, the relationship that the patient tends to create with the doctor has an important meaning [4,5].
And on the other hand, the medicine most frequently used by GPs is the doctor himself. But little is known about the doses and intervals of administration of this "drug" [6].
Giving a medication is the tangible expression of attending and giving help. Thus, the prescription is a complex issue; It is a ritual. There are many elements in this exchange: promise and expectation of giving and receiving, of instructing, of evolving, of caring for and accepting care, and others, that are not within the active ingredients of pharmacology. The prescription indicates relationship. For every specific patient, the style of this transaction must be accommodated to ensure the success of the relationship [7].
On the other hand, whether the drug is proven effective, although it depends in part on the prescription process, also depends on what expectations the patient has wanted to hear from the doctor [8].
In the biological dimension of treatment (for example, antibiotics or surgery), interventions are used with the expectation that they will achieve healing. But we must bear in mind that many drugs also act through the psychological dimension (placebo effect), and that they also modify the doctor-patient encounter. The treatment in the psychological dimension is mainly directed to modify feelings-emotions, the functional capacities, and the well-being of the patient. It is based especially on the doctor-patient relationship and its placebo effect. The probabilities of success are directly proportional to the quality of this relationship [5,9,10].
In relation to all this, we must remember the concept of placebo. The concepts of placebo and nocebo are important in medicine, especially in family medicine and mental health. The placebo effect is often reconsidered as the effects of an "inert substance", but that characterization is misleading. In a broad sense, placebo effects are improvements in the symptoms of patients that are attributable to their participation in the therapeutic encounter, with their rituals, symbols and interactions. The placebo effect can be observed in any medical encounter and not only in clinical trials that incorporate a placebo treatment group. It is possible that the prescription of any therapeutic regimen will produce a placebo effect [11,12].
Placebo effects are based on complex neurobiological mechanisms involving neurotransmitters and activation of specific, quantifiable and relevant areas of the brain. Many common medications also act through these pathways. Psychosocial factors that promote the therapeutic effects of placebo also have the potential to cause adverse consequences, known as nocebo effects. Not infrequently, patients perceive the side effects of medications that are actually caused by the anticipation of negative effects or greater attention to the normal background discomforts of daily life in the context of a new therapeutic regimen [13-15].
Thus, placebo can be defined as a beneficial effect produced by positive expectations, and this is related to personality traits such as the ability to recover from adversity, direct temperament and altruism, which are positive predictors of the placebo effect. The reverse side of the placebo effect is the nocebo: the personality traits of anger and hostility, anxiety and depression are predictive factors. Therefore, patient expectations and personality traits are important determinants of unwanted adverse effects, and physicians should have strategies to encourage optimal treatment outcomes [5,6,10,16]. And these clinical implications of placebo, in numerous pharmacological treatments, may be more important that the efficacy of the drugs themselves.
Finally, we must remember that many factors influence the adherence in pharmacological treatment, which on the other hand overlap, but the two main factors are the doctor-patient relationship and the complexity / simplicity of the pharmacological treatment. In any case, the discontinuity of the treatment indicates in some way a discontinuity of the doctor-patient relationship. The doctor-patient therapeutic relationship is the environment where the rest of the therapeutic instruments, pharmacological or not, is housed. Each type of doctor-patient relationship implies a different relationship with pharmacological treatment [16].
In short, family doctors do not treat diseases, but take care of people. They need to understand that the disease process is socially constructed within the patient's life and expressed in the doctor-patient relationship. The GP has to mediate between the subjective experience of the patient's illness and the scientific explanation. In that space is the enormous potential of the doctor-patient relationship.
- Turabian JL, Perez Franco B (2005) A way to make clinical pragmatism operative: systematization of the actuation of competent physicians. Med Clin (Bar) 124: 476.
- Turabian JL (2018) The general physician along the patients ‘High and Low Tides’. Journal of Public Health and General Medicine 1: 1-3.
- Turabian JL (2018) Doctor-Patient relationship epidemiology and its implications on public health. Epidemol Int J 2: 000116.
- Freud S (1966) Interpretation of dreams. London: Sigmund Freud Copyright, Ltd.
- Balint M, Hunt J, Joyce D, Marinker M, Woodcock J (1970) Treatment or diagnosis. A study of repeat prescriptions in general practice. London: Tavistock publications.
- Balint E, Norell JS (1973) Six minutes for the patient: interactions in general practice consultations. London: Tavistock Publications.
- Turabian JL (2018) Doctor-Patient relationship as dancing a dance. Journal of Family Medicine 1: 1-6.
- Turabian JL (2018) Why do patients not meet the pharamalogical treatment? Arch Pharmacol Ther 1: 1-8.
- Leigh H, Reiser MF (1992) The patient, biological, psychological, and social dimensions of medical practice. New York: Plenun Medical Book Company.
- Turabian JL, Pérez Franco B (2010) The concept of treatment in family medicine: A contextualised and contextual map of a city hardly seen. Aten Primaria 42: 253-254.
- Benedetti F, Amanzio M (2011) The placebo response: how words and rituals change the patient's brain. Patient Educ Couns 84: 413-419. [Crossref]
- Chavarria V, Vian J, Pereira C, Data-Franco J, Fernandes BS, et al. (2017) The placebo and nocebo phenomena: Their clinical management and impact on treatment outcomes. Clin Ther 39: 477-486.
- Sedgwick P (2011) The placebo effect. BMJ 343: d7665.
- Kaptchuk TJ, Miller FG (2015) Placebo effects in medicine. N Engl J Med 373: 8-9. [Crossref]
- Weimer K, Colloca L, Enck P (2015) Placebo effects in psychiatry: mediators and moderators. Lancet Psychiatry 2: 246-257.
- Turabian JL (2018) Doctor-Patient relationship in pharmacological treatment: discontinuation and adherence. COJ Rev & Res 1.

