Abstract
Cysts and masses originating from the placenta or umbilical cord have poor evidence regarding their clinical relevance. While small placental cysts are most likely harmless, larger cysts may be associated with an increased risk of intrauterine growth retardation. The rare extra-abdominal umbilical vein varices can be acutely life-threatening for the fetus. In the case presented, the change in the morphology of the cyst was of particular concern, so that a choice had to be made between immediate delivery at 32 weeks of pregnancy and prolongation under close monitoring. Self-monitoring through a remote CTG could avoid repeated clinic visits in times of pandemic and at the same time ensure a safe continuation of the pregnancy until the end of prematurity.
Key words
placental cyst, umbilical cord cyst, extra-abdominal umbilical vein varix, remote CTG, home monitoring, telehealth, pandemic
Introduction
True placental cysts, also called chorionic plate cysts are anechoic thin-walled structures with an estimated prevalence of 2%–7% [1]. Typically, placental cysts are located near the insertion of the umbilical cord or along the fetal surface of the placenta without visible perfusion. Small cysts are probably harmless, when larger than 45mm, an association with IUGR has been described [2]. There is also evidence that the cyst fluid has prothrombotic properties; in ruptured cysts adjacent thrombi have been observed in the placenta [3].
The sonographic differential diagnosis to placental cysts are umbilical cord cysts or extra-abdominal umbilical vein varices.
Cord cysts may be associated with chromosomal abnormalities or with structural abnormalities such as an omphalocele. Therefore, when a cord cyst is diagnosed it is recommended to look for other abnormalities in a comprehensive ultrasound examination. Genetic testing should be offered in case of IUGR or other sonographic findings. Isolated cord cysts are likely to have a favorable prognosis [4,5].
Extra-abdominal umbilical vein varices are extremely rare fetal vascular anomalies. They are associated with adverse fetal outcome such as fetal anemia, fetal heart failure and hydrops fetalis or fetal death [6,7].
The sonographic differentiation as well as the assessment of the clinical relevance can be very difficult, therefore in the following case an intensified pregnancy monitoring was carried out by remote CTG and home monitoring.
Case
A 33-year-old woman in 32 weeks and 3 days of her third pregnancy was transferred to our unit for immediate delivery due to mayor concerns of her outpatient obstetrician regarding a rapidly developing cystic mass at the base of the placental umbilical cord with significant morphological changes within the last 14 days. The pregnancy had been uneventful up to this point. Sonography showed a timely developed fetus with a normal amount of amniotic fluid and normal Doppler parameters. There was a cystic structure of 42mm x 29mm x 41mm close to the placental insertion of the umbilical cord. Within the anechoic cystic mass, a spherical echo-rich structure of 23mm x 26mm x 28mm on a thin stalk without detectable vascularization was visible (Figures 1 and 2). The cyst was first noticed in the 3rd ultrasound scan at 30 weeks of gestation, but at that time it was still without internal structure. Due to the change in morphology the considered differential diagnosis were a thrombosed extra-abdominal umbilical vein varix as well as a placental or umbilical cord cyst.
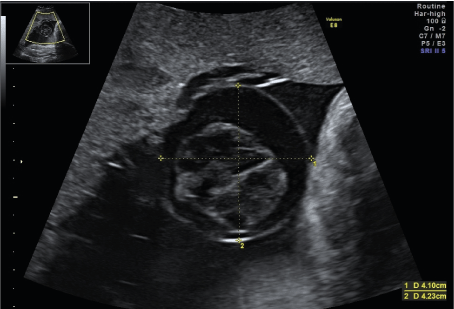
Figure 1. Cystic structure of 42mm x 29mm x 41mm close to the placental insertion of the umbilical cord. Within the anechoic cystic mass, a spherical echo-rich structure of 23mm x 26mm x 28mm on a thin stalk without detectable vascularization was visible
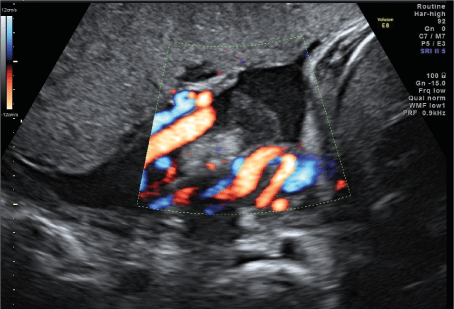
Figure 2. Difficulty in differentiating whether the cyst originates primarily from the placenta or the umbilical cord
Due to the unclear morphology and clinical relevance, the possible risks and complications of prolonging the pregnancy versus the risks of prematurity in case of early delivery were discussed in detail with the patient. Finally a prospective approach with close CTG and ultrasound monitoring was chosen. Antenatal steroid prophylaxis was administered. To avoid long inpatient stays and frequent clinic visits, especially during the SARS-CoV-2-pandemic, the patient was equipped with a remote CTG monitoring system. She was able to record a daily CTG from home, which were transmitted to the clinic and assessed there. Twice a week, the patient came to the clinic for a sonographic check-up. The patient learned how to record the CTGs correctly with the help of software (Figure 3) and support by a midwife. After a learning curve of a few days the CTG acquisition worked increasingly smoothly and the time of recording until an interpretable CTG trace was transmitted decreased (Figure 4).

Figure 3. The patient is learning how to record the CTG correctly with the help of a software
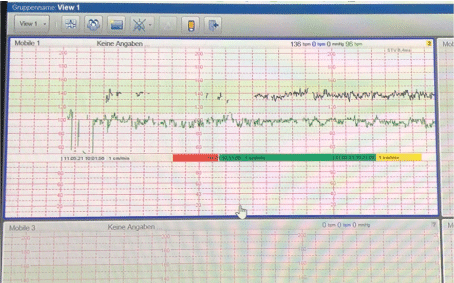
Figure 4. Display of the CTG traces including an automated assessment accoring to FIGO guidelines in a standard browser
Thirty-eight CTG records were transmitted from the patient to the clinic between 32+3 and 37+2 weeks of pregnancy and 11 ultrasound scans were performed. The CTG records totaled 15.49 hours, with a mean of 25 minutes.
At 37+2 weeks a timely developed girl was born after induction of labour (weight 3080g/54th percentile, length 50cm/54th percentile, APGAR 9/10/10, umbilical cord arterial pH 7.32).
The placenta itself was macroscopically inconspicuous, directly at the umbilical cord outlet there was a cyst measuring 45 mm (Figure 5). After opening it serous fluid as well as brownish soft tissue (27 x 12 x 10mm) was discharged.
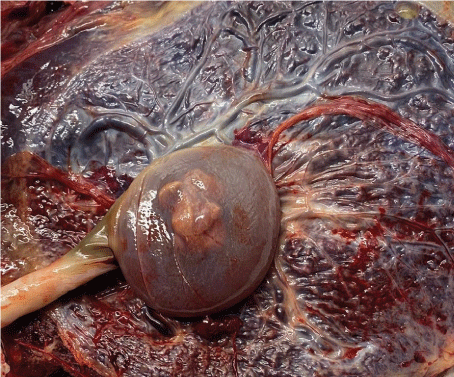
Figure 5. The placenta itself was macroscopically inconspicuous, directly at the umbilical cord outlet there was a cyst measuring 4.5 cm. The brownish solid structure inside the cyst correlate to the internal structure shown sonographically. Histomorphologically the structure consisted of fibrin, so that a true placental cyst was diagnosed
Microscopically the cyst was located between the amniotic cavity and the chorionic plate, in the region of the umbilical cord without vascularization. Histomorphologically the internal structure consisted of fibrin without evidence of fetal or teratoma parts, so that a true placental cyst was diagnosed.
Discussion
Due to the increasing quality in ultrasound diagnostics, prepartum diagnosis of cysts or masses in the area of the placenta and umbilical cord is becoming more frequent. As clinical studies with larger case numbers are lacking and only case series and case reports are available, there is no evidence of the clinical relevance of such findings. While small placental cysts are most likely harmless, larger cysts may be associated with an increased risk of intrauterine growth retardation [2]. The rare extra-abdominal umbilical vein varices can be acutely life-threatening for the fetus [6]. Thus, the clinician faces a dilemma between a harmless incidental sonographic finding and a potentially life-threatening pathology. Close monitoring of the pregnancy with ultrasound and CTG can prevent premature delivery and gain maturity for the child. For the pregnant woman, however, this means a large number of outpatient check-ups and clinic visits or a longer stay in the hospital. Both should be avoided if possible, especially during the SARS-CoV-2 pandemic.
The SARS-CoV-2 pandemic caused an immense acceleration in the development of telemedicine in a wide range of medical disciplines [8] and also in antenatal care. Telehealth can significantly reduce doctor-patient contacts and exposure to COVID-19, even though it is undisputed that telehealth virtual visits do not replace in-person encounters during prenatal care [9]. In addition to telemedical care for risk-free pregnancies [10], it has also been shown for high-risk pregnancies that the combination of face-to-face appointments and telehealth can be a safe option in times of the pandemic [11]. Zizzo et al. go one step further with self-monitoring. In a retrospective study, they evaluated the outcome and safety of extended remote self-monitoring of maternal and fetal health in intermediate- and high-risk pregnancies. Pregnant women with PPROM, fetal growth restriction, preeclampsia, gestational diabetes mellitus, high-risk of preeclampsia or a history of previous fetal or neonatal loss performed remote self-monitoring including C-reactive protein, non-stress test by cardiotocography, temperature, blood pressure, heart rate and a questionnaire concerning maternal and fetal well-being. The authors described home-monitoring as a safe alternative to inpatient or frequent outpatient care, which sets the stage for a new way of thinking in hospital care [9]. Advantages may include higher patient satisfaction, less stress in the home setting and lower costs, in addition to risk reduction of corona virus infection. It should be noted that careful training of the patient and the staff involved is necessary and that self-monitoring requires some practice. In addition, the patient's compliance is essential.
Conclusion
In the case presented self-monitoring was a suitable method to closely monitor a pregnancy with a pathology of unclear relevance without subjecting the patient to a long inpatient stay or numerous clinic visits. In addition, premature delivery could be avoided.
Acknowledgments
None
Funding information
No funding was solicited or required for this work.
Conflicts of interest
MD is managing director of Trium Analysis Online GmbH that is the manufacturer of the monitoring system “mobile fleet” which has been used in this study. It comprises a CTG measuring device (here HeraBEAT), a pre-installed smartphone (here Oukitel WP5, Schutzklasse IP68, MIL-STD-810G, Helio Ass MT6762M Quad Core 2GHz) and CTG analysis software “CTG Online” running in a secure computing centre in Munich.
The other authors declare that they have no competing interests.
References
- Fadl S, Moshiri M, Fligner CL, Katz DS, Dighe M (2017) Placental imaging: Normal appearance with review of pathologic findings. Radiographics 37: 979-998. [Crossref]
- Abramowicz JS, Sheiner E (2008) Ultrasound of the placenta: a systematic approach. Part I: Imaging. Placenta 29: 225-240. [Crossref]
- Stolla M, Refaai MA, Conley G, Spinelli S, Casey A, et al. (2019) Placental chorionic cyst fluid has prothrombotic properties and differs from amniotic fluid. Pediatr Dev Pathol 22: 304-314. [Crossref]
- Zangen R, Boldes R, Yaffe H, Schwed P, Weiner Z (2010) Umbilical cord cysts in the second and third trimesters: significance and prenatal approach. Ultrasound Obstet Gynecol 36: 296-301. [Crossref]
- Ruiz Campo L, Savirón Cornudella R, Gámez Alderete F, Martínez-Payo C, Pérez Pérez P, et al. (2017) Prenatal diagnosis of umbilical cord cyst: Clinical significance and prognosis. Taiwan J Obstet Gynecol 56: 622-627. [Crossref]
- Cassidy-Vu L, Clark S, Cuka N (2019) Extra-abdominal umbilical vein varix in a newborn. BMJ Case Rep 12: e227424
- Io S, Kondoh E, Iemura Y, Minamiguchi S, Chigusa Y, et al. (2021) Severe fetal anemia as a consequence of extra-abdominal umbilical vein varix: A case report and review of the literature. Congenit Anom (Kyoto). 61: 4-8. [Crossref]
- Hollander JE, Carr BG (2020) Virtually perfect? Telemedicine for Covid-19. New Engl J Med 382: 1679-1681. [Crossref]
- Zizzo AR, Hvidman L, Salvig JD, Holst L, Kyng M, et al. (2022) Home management by remote self-monitoring in intermediate- and high-risk pregnancies: A retrospective study of 400 consecutive women. Acta Obstet Gynecol Scand 101: 135-144. [Crossref]
- Fryer K, Delgado A, Foti T, Reid CN, Marshall J (2020) Implementation of obstetric telehealth during COVID-19 and beyond. Matern Child Health J 24: 1104-1110. [Crossref]
- Aziz A, Zork N, Aubey JJ, Baptiste CD, D'Alton ME, et al. (2020) Telehealth for high-risk pregnancies in the setting of the COVID-19 Pandemic. Am J Perinatol 37: 800-808. [Crossref]





