Hip fractures are one of the most serious, debilitating and even deadly fall-related injuries that are all too common in the elderly. Elderly and the disabled struggle to recover from a hip fracture and afterward many people are not able to live on their own. As the U.S. population gets older, the number of hip fractures is likely to go up. The hip protector is a protective garment to cover the greater trochanter and seems like a straightforward method to reduce impact forces on the hip. In practice however, the elderly infrequently wear hip protector products - pants, undergarments, or outer wear. Acknowledging that patient adherence to hip protector clothing remains a barrier for implementation, technology advances are removing barriers among the elderly. One such promising innovation recently emerged onto the commercial market is a hip protection “smart belt” (Tango Belt, Active Protective Technologies). Motion-sensing and companion mobile application technologies combine to measure efficiency and effective of this innovation, articulated through a case-study.
Aging, hip fracture, smart technology
The population of older adults who are at risk for or experiencing falls and resulting injuries in the United States is increasing. Adults aged ≥85 years are the fastest-growing age group among U.S. residents, and are projected to reach approximately 8.9 million in 2030 [1]. More than 1 in 4 adults ages 65 and older reported falling and one in 10 reported a fall-related injury in 2014 [2]. Among older adults, falls account for approximately 60% of all injury-related ED visits and over 50% of injury-related deaths annually [3].
According to Burns and Kakara (2018) [4], the overall rate of older adult deaths from falls increased 31% from 2007 to 2016 (3.0% per year). Nationwide, 29,668 (61.6 per 100,000) U.S. residents aged ≥65 years died from fall-related causes in 2016. The annual rate increase was larger among adults aged ≥85 years (3.9% per year) than among those aged 65–74 years (1.8%) and 75–84 years (2.3%).
Hip fractures are one of the most serious, debilitating and even deadly fall-related injuries that are all too common in the elderly. Over 10 years ago, estimates suggested that 1 in 3 women and 1 in 12 men will sustain a hip fracture in their lifetime [5]. Additionally, hip fractures are predominately a burden to the elderly because 86% of hip fractures occur in individuals aged 65 years and older [6].
Elderly and the disabled struggle to recover from a hip fracture and afterward many people are not able to live on their own. As the U.S. population gets older, the number of hip fractures is likely to go up. According to CDC (2017) [7], “each year over 300,000 older people—those 65 and older—are hospitalized for hip fractures. More than 95% of hip fractures are caused by falling, usually by falling sideways.; Women experience three-quarters of all hip fractures”.
Hip protectors: State of the science and implementation
The hip protector is a protective garment to cover the greater trochanter and seems like a straightforward method to reduce impact forces on the hip. Indeed, external hip protectors have been shown to attenuate the peak impact force on the hip by 37% to 95%, depending on type, model, and applied force impulse [8,9]. Comparative biomechanical testing has shown that, not surprisingly, the hip protectors most effective at attenuating peak impact force are those that are the hardest and thickest [10].
In clinical studies, hip protectors retain protective properties to shield a hip from fracture [11]. When pooling data from cluster randomized trials involving elderly in nursing homes, hip protectors were found to decrease risk of hip fracture [12]. In clinical practice, hip protectors are offered to patients at risk for or history of hip fracture. Hip protectors are also used along with floor mats and have the greatest protective properties to reduce trauma due to falls and are feasible paired interventions to reduce trauma for vulnerable populations: 85 years of age and older and those at risk for fracture or fracture history [13]. Weighing benefit versus harm, national guidelines, toolkits, and population-based programs have recommended the use of hip-protective clothing as an injury reduction intervention to reduce hip fracture risk. Hip-protective clothing absorbs trauma and reduces hip fracture risk and should be included in injury prevention programs [14-16].
In practice however, the elderly infrequently wear hip protector products - pants, undergarments, or outer wear. In studies concluding that hip protectors had no significant effect on hip fracture risk [17-20]. Patient adherence was generally poor [21]. Kannus et al. [22] in a randomized clinical trial have shown that hip protectors, when worn, reduced the risk of hip fracture by more than 80 percent and listed a 31% refusal of participants to wear the passive hip. Barriers to wearing hip protectors have been reported to be patient comfort, illness and physical difficulties, caregiver burden of extra time and effort needed to take them on and off, appearance and cost [20,23,24].
Technology Design to Reduce Barriers to Implementation
Acknowledging that patient and provider adherence to hip-protective clothing remains a barrier for implementation, technology advances are removing barriers among the elderly. One such promising innovation recently emerged onto the commercial market is a hip protection “smart belt” (Tango Belt, Active Protective Technologies). The smart belt utilizes motion-sensing technology built into a light weight, unobtrusive form factor that is able to accurately detect when the wearer is experiencing a fall-in progress that will likely result in a hip impact. When a serious hip-impacting fall is sensed, the belt activates a slim airbag, encompassing the anatomical hip bilaterally prior to the person hitting the floor to attenuate the impact force at the hip. Accurate detection of serious hip-impacting falls-in-progress is accomplished via an algorithm that has been developed using machine learning techniques to analyze thousands of hours of motion data collected from elderly subjects. The smart belt has the capability of connecting to Wi-Fi to relay communication to caregivers regarding need of assistance by the belt wearer as well as mobility data. The communication relay includes urgent alerts to caregivers of a fall incident in order to initiate care to the wearer in such situations. The belt may also communicate when the wearer may need assistance in cases of improper belt positioning on the torso, low battery charge, if the wearer has experienced an impact force as well as if the wearer is requesting assistance with the call button located on the front of the belt buckle.
The motion-sensing system of the belt is located on the wearer’s lower torso, enabling the inertial measurement unit an accurate capture of the person’s centre of mass during functional mobility and locomotion (Figure 1).

Figure 1. Tango Belt shown on typical wearer
Data capabilities of the belt include wear time of the protection device, tracking of individual wearers self-reported fear of falling, steps taken and centre of mass deviation.
A companion mobile application can be used by members of the wearer’s care team to enable viewing of clinically relevant metrics extracted from the wearer’s belt data. This mobile app allows community administrators and caregivers easy access to manage the smart belt. Using the app, a caregiver is able to assign and unassign the safety device to wearers, establish the settings desired for the wearer’s belt including the local feedback of the belt (sound volume, light brightness and strength of haptic feedback (Figure 2).

Figure 2. Tango Belt with accompanying mobile app
The alert communication of low battery, buckle/unbuckle, impact occurrence and enablement of the call button are optional and manageable by a community administrator in the mobile app.
When a belt is assigned to an individual, mobility data is collected as it is worn. Smart technology metrics include utilization, compliance and daily wear hours, balance (Short version of Falls Efficacy Scale – International), and stability (calculated by the centre of mass average deviation from vertical axis and mobility in terms of step count) (Figure 3).
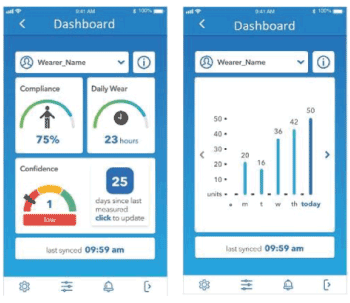
Figure 3. Individual belt wearer’s Dashboard metrics
The roadmap for the Tango Belt includes progression of the data captured and reporting of an individual’s distance-over-surface, gait speed, Timed-Up-and-Go testing, stride time variability and a composite fall risk score.
Successful implementation of the smart hip protection technology includes the interdisciplinary management of falls in three parts: identification of appropriate user, implementation of the smart belt technology with the patient and care team and achievement of adherence to the utilization of the product. The hip protection belt was recently evaluated in a large long-term care facility with the goals of embedding the wearable technology into daily care, improve safe mobility, decrease fall injuries, and establish consistent use.
Identification of residents most appropriate for use of the wearable technology was achieved with inclusion of the technology in the fall management team rounds in the centre. The quality and risk management lead nurse lead the discussion and members of the environmental services, recreational therapies, rehabilitation and nursing teams attended the rounds for patient specific care planning. During the fall management care planning sessions, the team reviewed the risk at which the identified residents were for falling with the inclusion of how often they had been experiencing a fall. Current methods of fall prevention as well as injury prevention are noted with an interdisciplinary discussion for the patient specific indications of risk of fall. The hip protection smart belt was embedded into the fall management “toolbox” of the team for consideration of most appropriate and beneficial utilization. With identification of the appropriate resident for use of the belt, the unit nurse would offer insight into patient need specific wear schedule for inclusion into the treatment orders and initiate introduction of the safety technology to the POA to receive a signed agreement. Once the user agreement signature was received, the quality nurse fit the resident for the most appropriately sized belt, wear orders were confirmed in the electronic care system for consistency with care planning and initiation of the smart belt into the daily care for the resident was initiated.
The executive and patient care team members in the facility attended on-site training provided by the technology vendor for clear understanding of technology operation as well as care plan communication. Adherence to utilization of the wearable technology was defined as how many hours the resident wore as compared to the documented wear time care orders during the 4-week evaluation. Increasing adherence was reached with care plan adoption, gradual increase in patient and team engagement and ease of use with the demographically designed technology. An overall average adherence rate of 83% was achieved in terms of how many hours residents wore the smart belts as compared to prescribed wear time.
An inventory of 10 belts was initially provided for the protection belt evaluation to the facility with 8 out of 10 belts utilized. The impact of sizing distribution on number of belts allocated to residents as well as available to identified users was identified by the lead quality nurse and upon ending of the evaluation period an altered sizing distribution was facilitated with double the number of belts allocated. During the evaluation timeframe, there were 9 residents who were prescribed and wore the hip protection belt. Most wearers included were long term care residents of the facility with 1 resident expiring, 1 resident discharge home and 1 additional resident added upon admission to the centre. The predominant indications of smart hip protection belt prescription included history of falls, risk of falling, impaired cognition and decreased safety awareness.
A specific scenario in which injury from fall was avoided due to the wearable technology is of an 87-year-old female patient was wearing the hip protection belt within the care plan directed time frame. The user experienced a posterior lateral fall going from a standing position into a flexed position exposing the hip to most likelihood of hip fracture. The belt detected the fall motion, activated the deployment of the hip protection air bags and attenuated the impact of striking the floor. The hip protection belt’s recognition of the developing fall and resultant activation of the air bag performed as intended, and the wearer did not sustain any injury from the fall, including the possibility of sustaining a devastating hip fracture. (Nankaku, et al. 2005) Following the fall event, the belt activated its alert system with local audio and visual feedback alerting the nursing in the hallway and communicated alerts to established email and SMS messaging systems. The patient received immediate care and assessment. She was assisted to her feet by caregivers and walked back to bed where she returned to sleep unscathed. Motion data from the fall was retrieved from belt and clearly revealed that the patient took several steps, and then underwent a low G-force falling phase immediately prior to ground impact (Figure 4).
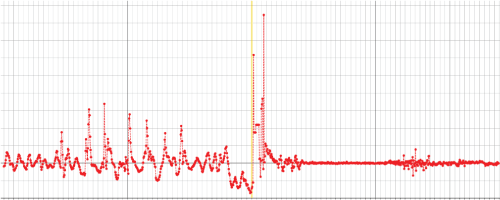
Figure 4. G-force data retrieved from the belt of the 10 seconds surrounding the fall. Wearer can be seen to take seven steps, briefly pause, fall, and then lie still. Airbag deployment occurs at the first G-force spike after reaching near zero-G during the falling phase; the second G-force spike immediately following is ground impact
Hip fractures resulting from falls are a devastating event for our older adult population. The staggering number of older adults who suffer from a hip fracture is anticipated to rise in the coming years if fall mitigation practice continues as current. The introduction of an unobtrusive hip protection technology into the fall risk management for those most at risk of suffering hip fractures has the potential to increase adherence and impact mobility, quality of life and mortality. The successful implementation of wearable smart belt promises to reduce morbidity and mortality associated with hip fractures. In addition, smart app technology will provide valid and reliable data to measure adherence, mobility, fear of falling and balance. The technology will provide clinical support for increased mobility and protection from serious hip-impacting falls to increase quality of life.
- Ortman J, Velkoff V, Hogan H (2014) An aging nation: the older population in the United States. Washington DC: US Department of Commerce, US Census Bureau.
- Bergen G, Stevens J, Burns E (2016) Falls and fall injuries among adults aged ≥ 65 years—United States, 2014. MMWR Morb Mortal Wkly Rep 65: 993-998. [Crossref]
- Centres for Disease Control and Prevention (2018) Welcome to WISQARS (Web-based Injury Statistics Query and Reporting System).
- Burns E, Kakara R (2018) Death from falls among persons aged >65 years-United States, 2007-2016. MMWR Morb Mortal Wkly Rep 67: 509-514. [Crossref]
- Chami G, Jeys L, Freudmann M, Connor L, Siddiqi M (2006) Are osteoporotic fractures being adequately investigated? A questionnaire of GP & orthopaedic surgeons. BMC Fam Pract 7: 7. [Crossref]
- Braithwaite RS, Col NF, Wong JB (2003) Estimating hip fracture morbidity, mortality and costs. J Am Geriatr Soc 51: 364-370. [Crossref]
- CDC (2017) Falls are Serious and Costly. Centres for Disease Control and Prevention, National Center for Injury Prevention and Control.
- Kannus P, Parkkari J, Poutala J (1999) Comparison of force attenuation properties of four different hip protectors under simulated falling conditions in the elderly: an in vitro biomechanical study. Bone 25: 229-235. [Crossref]
- Wiener SL, Andersson GB, Nyhus LM, Czech J (2002) Force reduction by an external hip protector on the human hip after falls. Clin Orthop Relat Res 398: 157-168. [Crossref]
- van Schoor NM, van der Veen AJ, Schaap LA, Smit TH, Lips P (2006) Biomechanical comparison of hard and soft hip protectors, and the influence of soft tissue. Bone 39: 401-407. [Crossref]
- Bulat T, Applegarth S, Wilkinson S, Fitzgerald S, Ahmed S, et al. (2008) Effect of multiple I impacts on protective properties of hip protectors. Clin Interv Aging 3: 567-571. [Crossref]
- Sawka AM, Boulos P, Beattie K, Papaioannou A, Gafni A, et al. (2007) Hip protectors decrease hip fracture risk in elderly nursing home residents: A Bayesian meta-analysis. J Clin Epidemiol 60: 336-344. [Crossref]
- Zubkoff L, Neily J, Quigley P, Delanko V, Young-Xu Y, et al. (2018) Preventing falls and fall-related injuries in state veterans homes. Virtual breakthrough series collaborative. J Nurs Care Qual 33: 334-340. [Crossref]
- AHRQ (2013) Making health care safer II. Rockville, MD: Agency for Healthcare Research and Quality.
- Boushon B, Nielsen G, Quigley P, Rita S, Rutherford P, et al. (2012) Transforming care at the bedside how-to guide: Reducing patient injuries from falls. Cambridge, MA: Institute for Healthcare Improvement.
- Pearson KB, Coburn AF (2011) Policy brief. Evidence-based fall prevention in critical access hospitals, Office of Rural Health (PHS Grant No. U27RH01080).
- Cameron ID, Cumming RG, Kurrle SE, Quine S, Lockwood K, et al. (2003) A randomised trial of hip protector use by frail older women living in their own homes. Inj Prev 9: 138-141. [Crossref]
- Birks YF, Porthouse J, Addie C, Loughney K, Saxon L, et al. (2004) Randomized controlled trial of hip protectors among women living in the community. Osteoporos Int 15: 701-706. [Crossref]
- Cameron ID, Venman J, Kurrle SE, Lockwood K, Birks C, et al. (2001) Hip protectors in aged-care facilities: a randomized trial of use by individual higher-risk residents. Age Ageing 30: 477-481. [Crossref]
- van Schoor NM, Asma G, Smit JH, Bouter LM, Lips P (2003) The Amsterdam Hip Protector Study: compliance and determinants of compliance. Osteoporos Int 14: 353-359. [Crossref]
- Lauritzen JB, Petersen MM, Lund B (1993) Effect of external hip protectors on hip fractures. Lancet 341: 11-13. [Crossref]
- Kannus P, Parkkari J, Niemi S, Pasanen M, Palvanen M, et al. (2000) Prevention of Hip Fracture in Elderly People with Use of a Hip Protector. N Engl J Med 343: 1506-1513. [Crossref]
- Bulat T, Powell-Cope G, Rubenstein LZ (2004) Perceived barriers and facilitators for the use of external hip protectors. Gerotechnology 3: 5-15.
- Forsén L, Sandvig S, Schuller A, Søgaard AJ (2004) Compliance with external hip protectors in nursing homes in Norway. Inj Prev 10: 344-349. [Crossref]




