AF: Atrial Fibrillation; ANP: Atrial Natriuretic Peptide; ART: Atrioventricular Reentrant Tachycardia; AV: Atrioventricular; AVNRT: Atrioventricular Nodal Re-entrant Tachycardia; BNP: B-Type Natriuretic Peptide; BPM: Beats per Minute; CHF: Congestive Heart Failure; CRT: Cardiac Resynchronization Therapy; IHD: Ischemic Heart Disease; LV: Left Ventricular; LVEDV: Left Ventricular End-Diastolic Volume;LVEF: Left Ventricular Ejection Fraction; PJRT: Permanent Junctional Reciprocating Tachycardia; PV: Pulmonary Vein; PVC: Persistent Ventricular Ectopy; RAAS: Renin-Angiotensin-Aldosterone System; RF: Radiofrequency; RV: Right Ventricular; RVEDV: Right Ventricular End-Diastolic Volume; RVEF: Right Ventricular Ejection Fraction; RVOT: Right Ventricular Outflow Tract; TIC: Tachycardia-Induced Cardiomyopathy; VES: Ventricular Extrasystoles; VT: Ventricular Tachycardia
Congestive Heart Failure (CHF) is an important clinical problem with significant morbidity and mortality, and often always the final clinical presentation of majority of cardiovascular disorders. Thus, the increasing prevalence and severity of CHF has re-focused importance on the search for reversible etiologies of left ventricular (LV) systolic dysfunction. Pathologic effect of tachyarrhythmias on ventricular morphology and/or function is emerging as an important research area. Numerous studies have implicated incessant or chronic tachyarrhythmias as important causes of tachycardia-induced cardiomyopathy (TIC), which is potentially reversible through the administration of tachycardia-targeted rate or rhythm control therapies. The goal of this review is to aggregate current research evidence on description, epidemiology, clinical presentation, prognosis, pathophysiology, diagnosis and clinical management of TIC. The intention is to advance the knowledge and understanding of pathogenesis and clinical management of potentially reversible form of secondary cardiomyopathies that have not been well defined or studied but associated with increasing morbidity and mortality.
Congestive heart failure (CHF) and arrhythmias are usually co-occurring pathologic cardiac conditions. Within a cohort of CHF patients with systolic heart failure, ventricular dysfunction can be the result rather than the cause of abnormal cardiac rhythm, a cardiac condition referred to as tachycardia-induced cardiomyopathy (TIC) [1]. Although research into TIC has been relatively recent compared to other forms of cardiomyopathies, the first mention of TIC in literature was in 1913 by Gossage and Hicks [2] referring to a patient diagnosed with atrial fibrillation (AF) and heart failure symptoms. Later in 1949, Phillips and Levine [3] described an association between rapid AF and reversible heart failure. However, it was not until 1962 that Whipple et al. [4] described an experimental animal model mimicking pacing-induced cardiomyopathy in humans, which led to the identification of TIC as a distinct clinical entity. The model, based on right ventricular pacing in a canine using transvenous endocardial leads, greatly inspired subsequent generations of research on pathogenesis and etiology-specific clinical management of TIC.
Different studies have used different terminologies to describe TIC, including pacing-induced cardiomyopathy [11,12], tachycardiomyopathy [10,13], tachycardia-induced cardiomyopathy [14-16] or arrhythmia-induced cardiomyopathy [17-19], which has made clinical understanding tenuous. In addition, there are significant definitional variation of TIC in medical literature that has seriously undermined its universal understanding and problematized research consensus on diagnosis guidelines and clinical management. Table 1 lists some of the most commonly cited clinical definitions of TIC.
Table 1 reveals TIC is a reversible cardiac condition characterized by ventricular systolic and/or diastolic dysfunction occurring in the setting of chronic (incessant or persistent) atrial, supraventricular or ventricular tachyarrhythmias. Having a universally accepted definition of TIC is critical in facilitating the development of diagnosis and management guidelines since TIC is a potentially reversible cardiac condition [18,20].
1st Author [Ref #] |
Clinical Definition |
Mohamed, et al. [9] |
A heart condition caused by persistent supraventricular or ventricular tachyarrhythmia characterized by ventricular systolic dysfunction and dilatation and clinical manifestation of heart failure but reversible with normalization of heart rate. |
Povolny [15] |
A cardiac condition due to prolonged tachycardia leading to dilatation and systolic dysfunction with clinical manifestation of heart failure, which is reversible after normalization of heart rate. |
Gopinathannair, et al. [18] |
A cardiac condition in which atrial/ventricular tachyarrhythmias or frequent ventricular ectopy result in LV dysfunction, leading to systolic HF. The hallmark is partial or complete reversibility after achieving arrhythmia control. |
Ahmadi, et al. [20] |
A reversible form of dilated cardiomyopathy (DCM) occurring in the setting of supraventricular and ventricular tachyarrhythmias and whose diagnosis requires a high index of suspicion because the culprit tachyarrhythmia may not always be apparent. |
Jeong, et al. [21] |
A heart condition of atrial or ventricular systolic/diastolic dysfunction induced by elevated atrial or ventricular rates occurring in the absence of prior history of structural heart disease. |
Okada, et al. [22] |
A reversible form of ventricular systolic dysfunction caused primarily by a rapid ventricular response to tachyarrhythmias. |
Types of tachyarrhythmias
Different types of tachycardia have been associated with the development of TIC. The most common ones include atrial flutter, incessant supraventricular tachycardia, ventricular tachycardia (VT) and frequent ventricular extrasystoles (VES) [15]. Table 2 summarizes the common categories and types of tachycardia associated with TIC. Both supraventricular and ventricular tachycardia can cause TIC as well as other less common types such as sinus tachycardia associated with thyrotoxicosis.
Tachycardia-induced cardiomyopathy is an under-recognized clinical entity as well as has poorly understood prevalence and incidence. In addition, the incidence of TIC varies depending on the underlying type of tachycardia [23]. Donghua et al. [24] studied a cohort of 625 patients referred for radiofrequency ablation of tachyarrhythmias and found 2.7% had TIC. The incidence for specific arrhythmias has been reported between 10% for focal atrial tachycardia [25-26], 20% to 50% for permanent junctional reciprocating tachycardia [27-28] and 25% for chronic atrial flutter [19]. The incidence of AF-associated TIC ranges between 10% and 50% in HF patients [29]. In patients with frequent ventricular tachycardia referred for electrophysiological evaluation, the incidence of TIC was 9% to 34% [30-32]. However, the incidence of TIC in ventricular tachycardia have not been adequately described in literature [23].
Symptoms/risk factors
Tachycardia-induced cardiomyopathy maybe preceded by any tachycardia mechanisms – chronic or frequently recurring paroxysmal tachyarrhythmias (Table 2) but with a more frequent involvement of supraventricular tachycardia than ventricular arrhythmias [33] TIC can present at any age [9,34]. It has been already reported in infants and children [35], adolescent [13] and adults [36-37]. It is not well established why some TIC patients with chronic tachycardia develop ventricular dysfunction while others tolerate and maintain normal systolic function [9]. However, suggested risk factors for the development of TIC may include the type, rate and duration of tachycardia, the age of the patient, any determined underlying cardia disease, medication and co-occurring medical condition [10].
Table 2. Types of Tachyarrhythmias Associated with Tachycardia-Induced Cardiomyopathy. Adapted from Gupta, et al. [23]
Category |
Specific Type of Tachycardia |
Supraventricular |
Atrial fibrillation/flutter |
Atrial tachycardia |
Permanent junctional reciprocating tachycardia (PJRT) |
Atrioventricular (AV) nodal re-entrant tachycardia (AVNRT) |
AV reentrant tachycardia (ART) |
Inappropriate sinus tachycardia (a very rare cause) |
Ventricular |
Right ventricular (RV) outflow tract (RVOT) ventricular tachycardia (VT) |
Fascicular tachycardia |
Bundle branch re-entry ventricular tachycardia |
Ectopy |
Premature ventricular complexes |
Pacing |
Persistent rapid ventricular pacing |
High-rate pacing |
Other |
Thyrotoxicosis (sinus tachycardia/atrial fibrillation) |
In children
In children, TIC maybe difficult to detect on presentation. Although they may exhibit shortness of breath, fatigue, exercise intolerance and palpitation, these symptoms are often non-specific [38]. Infants may exhibit poor feeding and tachypnea, with increased risk of death reported at 10% [19]. Physical examination may detect tachyarrhythmia that is not proportional to age in the presence or absence of edema, poor skin perfusion, gallop rhythm, and regurgitation murmurs due to atrioventricular valve insufficiency. Other important clinical signs may be increased jugular venous pulse, enlargement of the liver and presence of basal rales [38].
Prognosis
Prognostic predictors: Prognosis of TIC is generally favorable. Recovery of ventricular function follows the restoration of sinus rhythm or slowing down of the atrioventricular conduction [39]. Prognosis mainly depends on two factors that have been well demonstrated to influence the severity of ventricular dysfunction: (a) the rate of arrhythmia and (b) the duration of the arrhythmia [33,38]. However, recovery is extremely variable, which maybe complete, partial, or even absent [10,39-40].
Recurrent or new tachycardia have also been reported to predict prognosis but their effect on LV function have not been fully assessed. Cruz et al. [16] followed 17 TIC patients for 12 years and observed recurrent tachycardia caused a rapid decline of LV function, symptomatic heart failure and high incidence of sudden cardiac death (SCD). The findings associated recurrent tachycardia with poorer prognosis. Age has also been associated with variable prognosis. Younger children, particularly newborns and infants, tend to have complete recovery [19].
Recovery period: Both experimental animal models and human studies have demonstrated the greatest LV function recovery (defined by LVEF ≥ 50%) occurs within one month after the termination or control of the culprit tachycardia, followed by a slower improvement until complete normalization up to one year [41-44]. The gradual period of recovery of LV function following sinus rhythm control resembles the period of LV function recovery in hibernating myocardium following revascularization, which may take up to one year [10,39,45]. Recovery of LV function is also significantly greater in TIC patients with substantially depressed LV function on initial assessment [46].
Chronic atrial or ventricular pacing in animal models has been reported to induce symptoms and physical signs of congestive heart failure [47-49]. The models reveal that LV-remodeling and heart failure occur in a time-dependent and predictable nature similar to TIC in humans [50-56], as such, research on pathophysiology of TIC has focused on natural history of LV re-modelling and dysfunction, neuro-hormonal activation and signaling, and cell viability and molecular pathways. Figure 1 provides a schematic illustration of the natural history, and the pathological cellular and molecular changes occurring in the development of TIC.
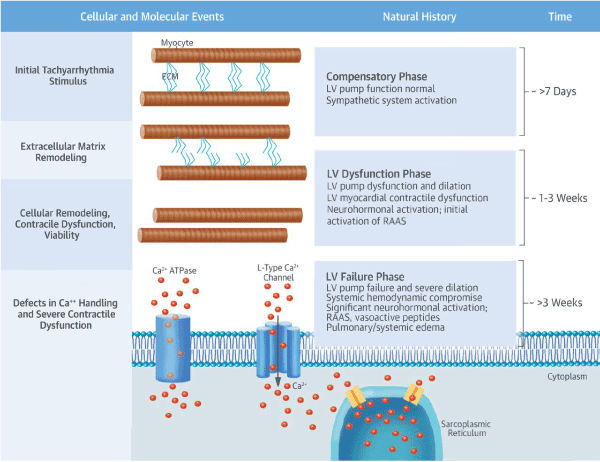
Figure 1. Natural History and Pathophysiology of Tachycardia-Induced Cardiomyopathy. The natural history (pathophysiology) of TIC takes approximately over three weeks divided into three phases. The first phase after seven days is the compensatory phase characterized by initial tachyarrhythmia stimulus (neurohormonal activation) and the onset of extra cellular remodeling. The second phase between 1and 3 weeks is LV dysfunction characterized by continued extra cellular remodeling and cellular remodeling leading to contractile dysfunction. The third and last phase occurring at three weeks and later is LV failure characterized by defects in calcium homeostasis and severe dysfunction in contractility. Adapted from Gopinathannair, et al. [18]
LV Remodeling and LV Failure
In the early developmental stages of TIC (between three to seven days), rapid cardiac pacing occurs accompanied by dilatation of LV and declining LV ejection fraction [50-54]. However, these early changes are not sufficient to cause an interference to either cardiac output or systemic perfusion pressures. By the second week, LV dilates, LVEF falls accompanied by an increase in central venous and pulmonary capillary wedge pressure, and systemic vascular resistance [50-52]. Eventually, these pathologic changes cause the development of heart failure. Although initial HF manifestations are adaptive, sustained rapid cardiac pacing affects LV load-ejection relationships [55-56]. LV dilatation and dysfunction cause a decline in intrinsic myocardial contractility [18].
Neurohormonal activation
Chronic rapid pacing in animal models have demonstrated predictable and time-dependent changes in neurohormonal pathways, neurohormonal synthesis and secretion of bioactive peptides [57-60]. The concentrations of atrial natriuretic peptide (ANP) and B-type natriuretic peptide (BNP) increase in the early stages of TIC accompanied by LV dilatation but eventually decrease or plateau because of suppressed synthesis [57-61]. In the neurohormonal activation mechanisms, there is also activation of sympathetic pathways leading into norepinephrine spillover. With progressive LV dysfunction, chronic rapid pacing activates the renin-angiotensin-aldosterone system (RAAS) [61,62]. Other molecular changes include the activation and secretion of endothelin and inflammatory cytokines – tumor necrosis factor alpha [59]. Further, mediators of vasoconstriction are induced but those of vasodilation such as response to nitric oxide are impaired [60,63]. Changes in neurohormonal activation and bioactive signaling pathways are important in the pathophysiology and prognosis of TIC. Changes in neurohormonal pathways such as ANP and BNP, and RAAS suggests changes in underlying LV functional status from compensated to de-compensated. As such, neurohormonal change may be a valuable prognostic factor (biomarker) for assessing the progressive nature and status of TIC. Changes in key bioactive signaling pathways such as the adrenergic and cytokine systems could contribute to myocardial dysfunction [18].
Defect in calcium ions handling
Under healthy conditions, elevated contraction frequency creates a positive force-frequency relationship characterized by progressive increase in myocardial contraction resulting from changes in calcium ions (Ca2+) handling and in myocardial response to Ca2+. Under TIC conditions, the positive force-frequency relationship is weaker accompanied by prolonged myocardial Ca2+ transients and defects in Ca2+cycling [64,65]. Changes in force-frequency relationship and Ca2+ handling suggest chronic rapid pacing manifesting after demonstrable changes of LV systolic function have occurred [65-68]. Changes in Ca2+ handling leads to impaired excitation-contraction coupling process, which in turn results into impaired myocyte contractility and inotropic responsiveness [66-68]. These changes have been observed during the development of TIC [18].
Extracellular matrix remodeling
In addition to remodeling within the myocyte, there are pathological changes (remodeling) manifesting within the extra-cellular matrix. Particularly, the loss of normal fibrillary collagen contented and distribution, which causes alterations in myocyte support and alignment in the LV wall accompanied by diminished capacity of myocyte to bind in the extracellular matrix [6,47,69]. These changes in myocyte suggest abnormalities in the extra-cellular matrix and integrin interface [18]. Elevated activity and expression of metalloproteinase contribute to the loss of support and architecture of extra-cellular matrix, which precedes the impairment in myocyte contractile function. Together, these observed abnormalities in extra-cellular matric suggest a likely pathologic mechanism of LV modeling includes the loss of structure, composition and function of myocardial extracellular matrix [69].
Diagnostic clues
Unlike other forms of cardiomyopathies such as dilated, hypertrophic and restrictive, TIC lacks established diagnostic criteria. Various studies have assessed possible diagnostic clues for TIC [18,13,34]. Gopinathannair et al. [18] report that the key diagnostic clues of TIC is the presence of pathological tachyarrhythmia or persistent ventricular ectopy (PVC) in the setting of unexplained cardiomyopathy (Figure 2). However, Gopinathannair et al. [18] goes further to report the lack of a clear understanding of the association between tachyarrhythmia and cardiomyopathy because tachyarrhythmia could exist for several years before recognition or before cardiomyopathy develops. Although a high index of clinical suspicion may suggest subtle diagnostic clues, TIC may go unrecognized for years. Clinical presentation of TIC could delay until after the manifestation of symptomatic heart failure or the arrhythmia could be detected but if no aggressive management is considered, the symptoms may progressively worsen and precede insidious development of TIC. Another important diagnostic challenge is the determination whether the detected arrhythmia is the etiology or the consequence of cardiomyopathy [18].
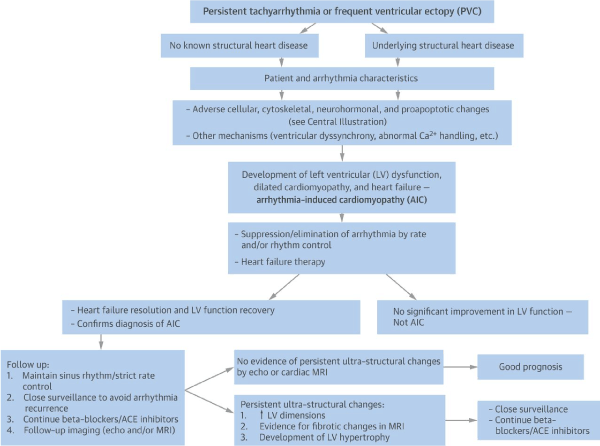
Figure 2. Overview of Mechanism, Diagnosis and Management of TIC. Diagnosis of TIC begins with the presence of persistent tachyarrhythmias or frequent ventricular ectopy then the detection of underlying structural heart disease, and finally the suppression of HF and LV function recovery after rate or rhythm control confirms diagnosis of TIC. If there is no significant improvement in LV function, the condition is not TIC. Adapted from Gopinathannair, et al. [18]
In a related study, Gupta et al. [23] also noted the lack of established clinical guidelines for the diagnosis of TIC but goes further to suggest the presence of subtle clinical clues could suggest TIC in clinical settings (Table 3). The study reports that a patient presenting with an onset of LV dysfunction and sustained or recurrent tachyarrhythmia with a cardiac rate of 100 beats or more per minute, and after physical, laboratory or echocardiography findings have excluded ischemic cardiomyopathy suggests the diagnosis of TIC. Table 3 summarizes frequently encountered subtle clinical clues that may lead to confirmatory diagnostic of TIC as reported by Gupta et al. [23].
Table 3. Diagnostic Clues Leading to the Detection of TIC Adapted from Gupta, et al. [23]
Step |
Clinical Description or Outcomes |
1. |
No other determinable cause of non-ischemic cardiomyopathy such as hypertension, alcohol, drug use and stress |
2. |
The absence of LV hypertrophy |
3. |
Relatively normal LV dimensions such as LV-end diastolic dimension < 5.5cm |
4. |
Restoration of LV function following control of tachycardia using rate control, radio-frequency ablation or cardioversion between one and six months |
5. |
Rapid decline in LV ejection fraction after recurrence of tachycardia in patients with restored LV function following control of tachycardia. |
Diagnostic algorithms
Based on etiology: Jeong et al. [21] investigated diagnosis and treatment of TIC in 21 patients (men = 15; mean age, 50 years, SD = 14) and proposed a diagnostic algorithm for etiologic differential diagnosis of heart failure in the setting of tachycardia as illustrated in Figure 3. According to Jeong et al. [21], clinical suspicion for TIC begins with the detection of underlying cardiac abnormalities (heart rate of > 100 beats per minute and severe dyspnea and/or chest pain) detected using patient/family history, physical and laboratory examination and/or echocardiograph findings. The study also reports that an important clinical feature for initial diagnostic differentiation of TIC from idiopathic dilated cardiomyopathy (DCM) with tachycardia is echocardiography defined smaller LV dimensions and volume in TIC patients at presentation. After the exclusion of IHD and LV hypertrophy due to other demonstrable causes such as hypertension, diagnosis of TIC should be considered in all patients with normal LV dimensions but without idiopathic cardiomyopathy and any other demonstrable causes [21].
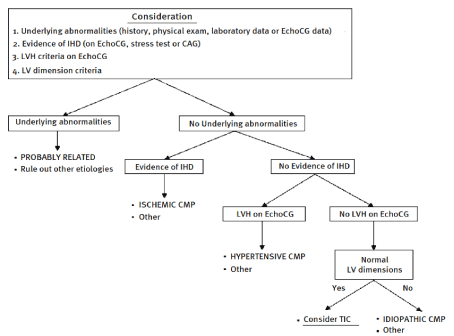
Figure 3. Etiologic Differential Diagnosis of Heart Failure with Tachycardia. Diagnosis based on etiology depends on three steps: (a) detection of underlying abnormalities; (b) evidence of ischemic heart disease; (c) presence of LV hypertrophy by echocardiography: and (d) normal LV dimensions. Adapted from Jeong, et al. [21]
In another study, Okada et al. [22] examined 102 consecutive patients with newly diagnosed LV dysfunction and atrial tachyarrhythmias and reports TIC patients had significantly lower RVEF/LVEF ratio and higher RVEDV/LVEDV ratio compared to DCM patients than LV volume or LV mass. The study conclude that RV systolic dysfunction and RV dilatation are characteristic diagnostic features of TIC, which facilitate differential diagnosis from DCM better than LV dysfunction (mass and volume abnormalities).
Based on clinical-presentation: Based on a case report and a review of literature, Lishmanov et al. [34] proposed a diagnostic algorithm based on clinical presentation, which limits invasive cardiac testing (Figure 4).

Figure 4. Diagnostic Algorithm for TIC Based on Clinical Presentation. Diagnosis based on clinical presentation depends on the presence of tachycardia and the onset of LV dysfunction, no evidence of ECG abnormalities, no underlying cardiac causes, rate/rhythm control normalizes cardiac function confirms diagnosis of TIC. Adapted from Lishmanov, et al. [34].
Although TIC lacks established diagnostic guidelines at initial visit, Lishmanov et al. [34] proposes that TIC should be suspected when LV systolic dysfunction occurs in the setting of persistent tachycardia. Prolonged heart rate of > 100 beats per minute may be deleterious and could suggest ventricular rate that may lead to TIC. Initial evaluation may follow current guidelines for evaluation of patients with systolic heart failure. However, it may be complicated by reports that TIC may manifest in morphologically normal hearts and in various types of structural heart disease, suggesting TIC is may not be easily excluded by evidence of other forms of structural heart disease. Lishmanov et al. [34] suggest that diagnosis of TIC may be inferred after observing restoration or improvement of ventricular function following control or management of heart rate (Table 4). Even without specific diagnostics criteria, LV dimensions provides important clinical evidence for distinguishing between TIC and idiopathic DCM accompanied by supraventricular tachycardia [21-23].
Table 4. Summary of Studies on Diagnosis of Tachycardia-Induced Cardiomyopathy
Authors |
Year of Publication |
Sample |
Men (%) |
Mean Age |
Initial
Heart Rate (bpm) |
Initial LVEF (%) |
Follow-up LVEF (%) |
Mean Follow-up
(Months) |
Jeong, et al. [21] |
2008 |
21 |
71 |
50 |
>100 |
30.0 |
58.0 |
38 |
Okada, et al. [22] |
2016 |
55 |
75 |
58 |
126 |
29.5 |
55.1 |
12 |
Medi, et al. [25] |
2009 |
30 |
60 |
39 |
117 |
35.0 |
≥50 |
12 |
Chin, et al. [71] |
2012 |
33 |
76 |
44 |
119 |
32.4 |
53.2 |
82 |
Mountantonakis, et al. [72] |
2011 |
69 |
62 |
51 |
NR |
35.0 |
57.4 |
11 |
Nia, et al. [73] |
2011 |
40 |
60 |
57 |
118 |
30.2 |
63.3 |
1 |
Calvo, et al. [74] |
2013 |
61 |
90 |
52 |
NR |
40.0 |
53.7 |
6 |
Janjua, et al. [75] |
2009 |
13 |
62 |
62 |
NR |
27.0 |
55.0 |
7 |
Dandamudi, et al. [76] |
2008 |
24 |
88 |
64 |
NR |
31.2 |
55.0 |
NR |
Fujino, et al. [77] |
2007 |
30 |
93 |
63 |
132 |
26.6 |
NR* |
49 |
Watanabe, et al. [78] |
2008 |
12 |
75 |
52 |
156 |
31.9 |
54.3 |
53 |
Total/Average |
--- |
388 |
73.8 |
53.8 |
128.0 |
31.7 |
56.1 |
27.1 |
Based on a review of TIC literature assessing the diagnosis of TIC, Riedlbauchova et al. [70] suggests that all suspected patients should undergo 12-lead ECG to determine basic heart rhythm and heart rate at presentation (on admission). The ECG tests is of particular importance in patients presenting with persistent atrial tachycardia. Owing to the observation that cardiac rate changes over time because of mental or physical activity, suspected TIC patients should undergo ECG for at least 12 hours. If underlying cause of tachyarrhythmia is indeterminable, electrophysiologic testing particularly the gold standard transthoracic echocardiography should be considered. Diagnosis should also document LV dysfunction with or without ventricular dilatation, which is smaller compared to DCM patients [21].
Imaging modalities also have clinical significance in the diagnosis of TIC. Upon documented ventricular dysfunction and LV dilation, other reasons for DCM should be excluded prior to the diagnosis of TIC. For adult patients, coronary angiography is always recommended to exclude ventricular dysfunction due to coronary artery disease or other structural heart disease [22]. Other importance causes considered for exclusion are chronic alcohol intake, drug abuse, cancer and cancer treatment or metabolic or congenital diseases. Finally, serial assessment of BNP levels is also useful in differentiating between TIC and cardiomyopathies in the setting of structural heart diseases [29]. All suspected cardiomyopathy patients have elevated levels of BNP but following successful cardioversion, the decreases in BNP levels is much quicker in TIC patients with 90% sensitivity, 95% specificity and 90% accuracy in the prediction of TIC [22,29].
Meta-analysis of diagnosis methods
The hallmark of the diagnosis of TIC is the presence of persistence tachyarrhythmias and the reversibility of LV function after rate and rhythm control. However, there are no standardized guidelines of characterizing LV morphology to distinguish DCM with secondary tachycardia from TIC. The current meta-analysis reviews studies on diagnosis of TIC to identify the common methods used in the diagnosis.
Search strategy
Studies were searched from online databases PubMed and EMBASE as well as Google Scholar for studies investigating diagnosis of TIC. The search used a combination of broad search terms combined using the option “AND”. The keywords used included various TIC terminology: “tachycardia-induced cardiomyopathy” OR “tachycardiomyopathy” OR “pacing-induced cardiomyopathy” OR “arrhythmia-induced cardiomyopathy” AND “diagnosis” OR “detection”. Studies were included if they met the following criteria: (a) they were prospective or retrospective; (b) reported original data; (c) assessed humans; (d) assessed at least one diagnostic method; and (e) included at least one of the following diagnostic or prognostic outcomes. (a) Sustained tachycardia (heart rate > 100 beats per minute (bpm)’ (b) initial and follow-up LVEF percentage; (c) follow-up period.
Titles and/or abstracts of the retrieved studies believed to satisfy the inclusion criteria were included for further review pending inclusion. Additional studies overlooked by the electronic search were obtained from references included in previously published articles, and from a search of abstracts of international meetings. All qualifying studies were included irrespective of date of publication and duration of study. Case reports with less than five patients or studies with data that was not readily extracted were excluded. Each included study was reviewed against the inclusion criteria, data extracted and recorded on Microsoft Excel Worksheet. The extracted data was name of the first author, year of publication, number of patients recruited (sample), percentage of men, mean age, initial heart rate, initial LVEF, follow-up LVEF and mean follow-up period. Table 5 presents a summary of the studies and selected diagnostic or prognostic factors.
Table 5. Summary of Studies on Diagnosis of Tachycardia-Induced Cardiomyopathy *NR: Reported LV function normalized within 6 months but no data provided
1st Author [Ref. #] |
Year of Publication |
Sample |
Men (%) |
Mean Age |
Initial
Heart Rate (bpm) |
Initial LVEF (%) |
Follow-up LVEF (%) |
Mean
Follow-up (Months) |
Jeong, et al. [21] |
2008 |
21 |
71 |
50 |
>100 |
30.0 |
58.0 |
38 |
Okada, et al. [22] |
2016 |
55 |
75 |
58 |
126 |
29.5 |
55.1 |
12 |
Medi, et al. [25] |
2009 |
30 |
60 |
39 |
117 |
35.0 |
≥50 |
12 |
Chin, et al. [71] |
2012 |
33 |
76 |
44 |
119 |
32.4 |
53.2 |
82 |
Mountantonakis, et al. [72] |
2011 |
69 |
62 |
51 |
NR |
35.0 |
57.4 |
11 |
Nia, et al. [73] |
2011 |
40 |
60 |
57 |
118 |
30.2 |
63.3 |
1 |
Calvo, et al. [74] |
2013 |
61 |
90 |
52 |
NR |
40.0 |
53.7 |
6 |
Janjua, et al. [75] |
2009 |
13 |
62 |
62 |
NR |
27.0 |
55.0 |
7 |
Dandamudi, et al. [76] |
2008 |
24 |
88 |
64 |
NR |
31.2 |
55.0 |
NR |
Fujino, et al. [77] |
2007 |
30 |
93 |
63 |
132 |
26.6 |
NR* |
49 |
Watanabe, et al. [78] |
2008 |
12 |
75 |
52 |
156 |
31.9 |
54.3 |
53 |
Total/Average |
--- |
388 |
73.8 |
53.8 |
128.0 |
31.7 |
56.1 |
27.1 |
*NR: Reported LV function normalized within 6 months but no data provided
Study characteristics
Eleven studies published between 2007 and 2013 meeting the inclusion criteria were included in this meta-analysis. Initial analysis reveals that a greater majority of the studies (9 or 82%) were retrospective [21,22,25,71-78] while the remaining two (18%) [73,75] were prospective. In the eleven studies, there were a total number of 388 patients diagnosed with TIC and their initial heart rate and initial and follow-up left ventricular function (LVEF) assessed using ECG and echocardiography. The patients were generally older (mean age = 53.8 years) with a marked gender discrepancy, where men constituted 73.8% of the sampled patients. They were followed for a mean period of 27.1 months, range 1 month [73] to 82 [71].
Key diagnostic features
All the eleven studies considered chronic tachycardia on admission as a key diagnostic feature of TIC in a clinical setting. Six studies [22,25,71,73,77,78] measured heart rate (beats per minute at presentation) and reported a mean heart rate of 128 bpm, range 117 [25] to 156 [78]. The remaining five studies [21,72,74,75,76] mentioned heart rate of >100 bpm in all the sampled patients but did not provide specific heart rate. Another important diagnostic feature that emerged from the findings of the eleven studies is rapid reversal or restoration of LV function within a period of six months. Mean Initial LVEF at presentation was 31.7% range 26.6% [77] to 40.0% [74]. After sinus rate control, LVEF significantly improved with a mean of 56.1% range 53.2% [71] to 63.3% [73].
The diagnosis of tachycardia-induced cardiomyopathy (TIC) has been challenging because of the lack of pathognomonic morphological and functional myocardial features. A key diagnostic challenge is differentiating between TIC and dilated cardiomyopathy in the presence of sustained ventricular tachyarrhythmias, which usually share similar LV morphological alterations [22,32]. Since the presence of persistence ventricular tachyarrhythmias is the basis of diagnosis of TIC, the present meta-analysis reviewed the use of electrocardiography (ECG) for TIC diagnosis. The present analysis also reviewed the detection of morphological changes in the myocardium using echocardiography, which is the leading imaging modality for characterizing functional and morphological myocardial alterations because of its ease of use and availability [34].
The present findings confirm that the presence of persistence ventricular tachyarrhythmias raise the primary suspicion for TIC and the main clinical reason for considering the diagnosis of TIC. The mean initial heart rate for the 388 patients was 128 beats per minute. Consistent with the findings of several earlier studies, ventricular arrhythmias defined as > 100 beats per minute at presentation is the primary reasons to raise the suspicion of TIC [21,22,34]. The second key diagnostic clue for confirming TIC is rapid reversal of LV function defined as echocardiography-defined LVEF < 40% to LVEF > 50% after controlling rate and rhythm. The present findings find significant improvement in LV function from LVEF = 31.7% at presentation and LVEF = 56.1% at follow-up, translating to LVEF = 24.4% improvement. Rapid reversal of LV function has already been demonstrated as the key clinical feature used to differentiate TIC from DCM. In DCM, LV dysfunction persists longer than six months even after rate and rhythm control [22,25,77].
Whereas sustained ventricular tachyarrhythmias and rapid reversal of LV function are the hallmark for TIC diagnosis, there is a need for additional functional and morphological imaging criteria to strengthen differential diagnosis of TIC from DCM as well as other secondary cardiomyopathies occurring with tachyarrhythmias. LV morphological characteristics such as the absence of LV hypertrophy and normal LV dimensions (LV end-diastolic dimension < 5.5 cm) have been suggested as possible criteria for differentiation of TIC from HCM and DCM [23]. While the absence of LV hypertrophy and LV mass have been widely accepted in the differential diagnosis of TIC, RV systolic dysfunction and dilatation are also characteristic of TIC. Thus, the ratio of RVEF/LVEF ratio and RV end-diastolic volume/LV end-diastolic volume have been shown to provide more accurate differentiation of TIC and DCM them LV hypertrophy or LV mass [22]. However, additional large-scale clinical trials are warranted to establish the value of RVEF/LVEF and RVEDV/LVEDV ratio in distinguishing TIC from DCM. Cardiac imaging modalities are also important to exclude underlying causes of ventricular dysfunction. In particular, coronary angiography excludes ventricular dysfunction secondary to coronary artery disease (CAD) in adult patients [22]. Besides ECG and imaging, patient characteristics such as chronic alcohol intake, drug abuse, anthracycline treatment, a quick decrease in BNP levels provide additional diagnostic clues for determining the underlying cause of ventricular dysfunction [29].
In summary, clinical diagnosis of TIC principally depends on the presence of sustained ventricular arrhythmias at presentation usually detected by ECG. Rapid reversal of LV function detected mainly by echocardiography imaging is the key differentiating feature between TIC and DCM in the setting of persistent ventricular arrhythmias. Other differentiation methods are RVEF/LVEF and RVEDV/LVEDV ratios and a quick decline in BNP levels. Coronary angiography and patient characteristics such as alcohol intake or anthracycline (anti-cancer) treatment may provide important supportive clues for TIC diagnosis.
Therapeutic targets
Clinical management for TIC includes rate control and heart failure treatment [70]. It is both well recognized and well established that clinical restoration of normal sinus rhythm in TIC patients improves LV systolic function and reverses clinical manifestation of heart failure [77-81]. Thus, the mainstay treatment of TIC is to obtain normal sinus rhythm. However, the most effective clinical means to obtain normal sinus rhythm varies depending on the types of causative tachyarrhythmias [34]. Most of the data available for heart rate control are from patients with atrial fibrillation, which is an important underlying etiology for TIC [33]. The 2014 American College of Cardiology/American Heart Association Task Force on Practice Guidelines and the Heart Rhythm Society (AHA/ACC/HRS) practice guidelines for management of atrial fibrillation (AF) recommend both pharmacological and non-pharmacological approaches [99].
Sinus rhythm control
In TIC patients, conversion to normal sinus rate is an important therapeutic goal, which targets to improve clinical and hemodynamic outcomes in TIC patients secondary to atrial fibrillation. However, there is inconclusive evidence as to whether rhythm control or rate control is a more superior therapy [23,34]. Two largescale trials: Atrial Fibrillation Follow-Up Investigation of Rhythm Management (AFFIRM) [82] and Rate Control Versus Electrical Cardioversion for Persistent AF (RACE) [83] reported no beneficial outcomes of rhythm control therapy and revealed a trend towards harm in the general population compared to rate control. The results were attributed to toxicity of anti-arrhythmic medication and difficulty in maintaining sinus rhythm but the two trials did not directly assess rhythm and rate control in TIC patients. However, subsequent analyses have demonstrated that non-pharmacologic therapies especially curative catheter ablation is beneficial in controlling sinus rhythm and rate. The two common therapies are pulmonary vein isolation and AV node ablation being the most frequently reported.
Pharmacological management
The 2014 AHA/ACC/HRS practice guidelines suggest the main objectives of sinus rhythm control in AF patients include relief of symptoms, prevention of embolism and avoidance of TIC [98]. Figure 5 provides pharmacological management of sinus rhythm in AF patients with heart disease.
The 2014 AHA/ACC/HRS practice guidelines (Figure 5) recommend different antiarrhythmic drugs for maintenance of sinus rhythm based on the absence or presence of heart diseases: heart failure (HF), coronary artery disease (CAD) or hypertension. However, beta-blockers or Sotalol are usually the initial drugs of choice. However, when medication rails to achieve sinus rhythm restoration, non-pharmacological options should be considered [99].
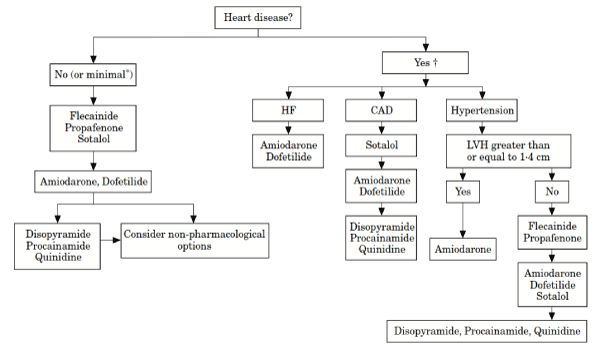
Figure 5. Antiarrhythmic Drug Therapy to Maintain Sinus Rhythm in AF Patients. Management of sinus rhythm in AF patients using medical therapy begins with the diagnosis of heart disease. The choice of medication depends on the presence of overt disease with heart failure, coronary artery disease and/or hypertension. Adapted from 2014 AHA/ACC/HRS Practice Guidelines, p. 1874 [99]
Pulmonary vein isolation
It is well recognized that the origin of paroxysmal atrial fibrillation is ectopic beats in the pulmonary vein musculature. Thus, pulmonary vein (PV) ablation is a rhythm control strategy that works by isolating the causative ectopic foci in the pulmonary vein and eliminates paroxysmal AF. PV ablation can be achieved either surgically or through radiofrequency catheter ablation [34]. However, due to concerns of recurrent PV connections, approximately 30% of TIC patients may require more than one procedure [84]. Gentlesk et al. [85] studied patients undergoing PV isolation, 18% having reduced LVEF (<50%), the mean LVEF improved significantly after PV ablation with those achieving successful AF control similar to patients with normal LV function. In a related study, Hsu et al. [86] investigated TIC patients with heart failure and observed significant improvement in mean LVEF (35-56%). The greatest improvement occurred in the first three months. Of the TIC patients with structural heart disease, 92% had significant improvement in mean LVEF (<20%).
AV-Node ablation
Atrioventricular (AV) node ablation is a form of rate control therapy considered for patients intolerant to drugs or having difficulty in rate control. In a meta-analysis including 200 patients, Wood et al. [87] reported AV node ablation had beneficial clinical outcomes in improved quality of life, LV function and exercise capacity. In the initial months following AV node ablation, there is the greatest improvement in LV function for patients with LVEF < 45%) because of elimination of AF and toxic effect of inotropic drugs and increased ventricular filling time. AV node ablation with implantation of pacemaker, referred to “ablate and pace” is considered for co-morbid older patients. However, chronic LV pacing may have negative effects on LV systolic function because of LV dyssynchrony [88]. Other reports suggest AV node ablation has beneficial outcomes is concomitant cardiac resynchronization therapy (CRT) is performed for patients meeting the CRT criteria [34].
Other ventricular arrhythmias
In TIC due to idiopathic ventricular arrhythmias such as PVC, LV or RVOT tachycardia), pharmacologic therapy or ablation may be considered for the restoration of sinus rhythm. However, because of myocardial dysfunction, there is limited choice of anti-arrhythmic medication. Usually there is contra-indication for Class IA and IC drugs because of malignant proarrhythmias secondary to myocardial dysfunction [89]. Class IV medication that could adversely affect clinical status of symptomatic patients should be avoided or withdrawn. Because of the limited use of anti-arrhythmic drugs, radiofrequency (RF) ablation is considered an effective and curative strategy for idiopathic ventricular arrhythmias [78,89,90,91].
Meta-analysis of clinical management methods
The primary target of the clinical management of TIC is to control sinus rhythm. Several approaches – medical therapy, pulmonary vein isolation and Av-node ablation – have been described as available therapies to control sinus rhythm. However, there are no clear guidelines for sinus rhythm control in TIC patients and thus current management approaches adopt those of managing ventricular arrhythmias more specifically the AHA/ACC/HRS practice guidelines for management of atrial fibrillation (AF) [99]. Thus, this meta-analysis reviews studies on clinical management of TIC to determine the common approaches and their efficacy in the management.
Search criteria
Studies investigating diagnosis of TIC were searched on electronic databases PubMed, EMBASE, Cochrane and Google Scholar. Search terms were restricted to studies that included in their titles or abstracts the following key terms or their combination “tachycardia-induced cardiomyopathy” OR “tachycardiomyopathy” OR “pacing-induced cardiomyopathy” OR “arrhythmia-induced cardiomyopathy” AND “management” OR “treatment” OR “rate control” OR “rhythm control”. Abstracts presented in major meetings of cardiology societies published in Circulation Journal, European Heart Journal and Pacing and Clinical Electrophysiology journals were searched for additional studies.
Inclusion criteria
The inclusion criteria was the study was: (a) a peer-reviewed full-length publications; (b) included the use of catheter ablation, medical therapy or pulmonary vein isolation to control sinus rate or rhythm; and (c) included numeric expression of the following clinical outcomes. (a) Left ventricular ejection fraction (LEVF); (b, left ventricular end-diastolic diameter (LVEDD); or (c) left atrial diameter (LAD) both at presentation and at follow-up. Titles and abstract suspected to meet the inclusion criteria were included for further review. Additional studies were included based on perusal of list of bibliographies and manual library searches for additional review. Case reports with less than five patients or studies with data that was not readily extracted were excluded.
Data extraction
Each study included in this meta-analysis was screened against the inclusion criteria and all relevant data extracted and recorded on Microsoft Excel Worksheet. Studies examining more than one clinical management method, data for both methods were extracted. Data extracted included last name of first author, number of patients, type of therapy given, LV function (LVEF) at baseline and at follow-up, LV end-diastolic diameter (LVEDD) at baseline and at follow-up, left atrial diameter (LAD) at baseline and at follow-up and the mean follow-up period. Statistical analysis used frequency, mean and standard deviation for categorical data. Table 6 presents a summary of the studies and selected diagnostic or prognostic factors.
Table 6. Summary of Studies on Management of Tachycardia-Induced Cardiomyopathy
1st Author [Ref. #] |
No. of Patients |
Therapy |
LVEF (%)
(Initial and a follow-up) |
LVEDD (mm)
(Initial and at follow-up) |
LAD (mm)
(Initial and 6 months follow-up) |
Mean Follow-up
Period (Months) |
Initial |
Follow-up |
Initial |
Follow-up |
Initial |
Follow-up |
Cruz, et al. [16] |
7 |
PVI |
36.3 |
58.6 |
55.7 |
49.0 |
NR |
NR |
22 |
Yokokawa, et al. [31] |
76 |
PVI |
36.0 |
56.0 |
NR |
NR |
NR |
NR |
95 |
Khan, et al. [42] |
41 |
PVI |
27.0 |
35.0 |
NR |
NR |
49.0 |
NR |
6 |
40 |
AVNA/PM |
29.0 |
28.0 |
NR |
NR |
47.0 |
NR |
6 |
Mountantonakis, et al. [72] |
68 |
PVI |
35.0 |
50.0 |
58.0 |
52.0 |
NR |
NR |
11 |
Calvo, et al. [74] |
61 |
PVI |
40.0 |
54.2 |
55.4 |
53.4 |
45.9 |
42.4 |
6 |
Gentlesk, et al. [85] |
67 |
PVI |
42.0 |
56.0 |
NR |
NR |
NR |
NR |
6 |
Hsu, et al. [86] |
58 |
PVI |
35.0 |
55.0 |
60.0 |
54.0 |
50.0 |
NR |
12 |
Chen, et al. [92] |
94 |
PVI |
36.0 |
41.0 |
NR |
NR |
47.0 |
NR |
14 |
Tondo, et al. [93] |
40 |
PVI |
33.0 |
47.0 |
NR |
NR |
NR |
NR |
14 |
Hunter, et al. [94] |
26 |
PVI |
31.8 |
40.0 |
NR |
NR |
52.0 |
NR |
6 |
Ozcan, et al. [88] |
56 |
AVNA/PM |
26.0 |
34.0 |
NR |
NR |
NR |
NR |
6 |
Brignole, et al. [95] |
28 |
AVNA/PM |
43.0 |
44.0 |
59.0 |
59.0 |
52.0 |
55.0 |
12 |
26 |
Medication |
44.0 |
41.0 |
58.0 |
59.0 |
49.0 |
48.0 |
12 |
Basiouny, et al. [96] |
16 |
PVI |
46.7 |
60.5 |
56.6 |
49.3 |
NR |
NR |
6 |
Lakkireddy, et al. [97] |
65 |
AVNA/CRT |
26.2 |
32.7 |
68.3 |
65.1 |
NR |
NR |
12 |
Total/Average |
769 |
|
35.4 |
45.8 |
58.9 |
55.1 |
49.0 |
48.5 |
15.4 |
PVI: Pulmonary Vein Isolation; LVEF: Left Ventricular Ejection Fraction; LVEDD: LV End Diastolic Diameter; LAD: Left Atrial Diameter; AVNA: AV node Ablation; PM: Pacemaker; CRT: Cardiac Resynchronization Therapy
Based on key words search and review of bibliographies, the search strategy yielded over 200 published studies. However, only fourteen (14) studies with a combined patient population of 769 met the inclusion criteria and were included in this meta-analysis. Clinical outcomes of the studies relevant to this meta-analysis are summarized in Table 5. All the 14 studies included patients with tachycardia, depressed LV function defined as LVEF < 45% and symptomatic heart failure. The most studied clinical management method was catheter ablation (pulmonary vein isolation) in 11 studies [16,31,42,72,74,86,86,92-94,96], followed by arteriovenous node ablation in four studies [42,88,95,97] and finally pharmacotherapy in one study [96] comparing with AVNA. Outcomes analysis assessed restoration of sinus rhythm expressed as echocardiography defined changes in LV function at presentation and follow-up. Mean follow-up period for the 14 studies was 15.4 months, range 6 months [42,74,88,94,96] and 95 months [31]. Two studies compared clinical management methods, PVI and AVNA [42], and AVNA and pharmacotherapy [95].
Outcome analysis of changes in LV function at presentation and follow-up shows mean improvement in LV function. There was 10.4% increase in LVEF from 35.4% to 45.8%, and a decrease in LV end-diastolic diameter (LVEDD) by 3.8 points from 58.9 mm to 55.1 mm. Two studies [74,95] that reported LAD at both presentation and follow-up indicated an insignificant decreased of 0.6 mm from 49.0 mm to 48.4 mm. In the eleven studies [16,31,42,72,74,86,86,92-94,96] that assessed PVI reported in 554 patients, there was a marked improvement in LV function: LVEF (36.3% to 50.3) and LVEDD (57.1 mm to 51.5 mm). These changes were greater compared to outcomes of LV function in four studies [42,88,95,97] that assessed AVNA and pacing in 189 patients: LVEF (31.1% to 34.7%) and LVEDD (63.7 mm to 62.1 mm).
Clinical management of TIC has depended on the restoration of sinus rhythm. However, because of the lack of standardized guidelines, many current approaches have adopted management practices developed for atrial fibrillation (AF), which is one of the key tachyarrhythmias leading to the development of TIC [99]. Consistent with this view, the present studies finds the management of sinus rhythm is the cornerstone of clinical management of TIC. The main management approaches used are pulmonary vein isolation (PVI), AV-node ablation (AVNA) and medical therapy. The three methods have been efficacious in reversing LV function defined with improvement in mean LVEF values from 35.4% at baseline to 45.8% in a mean follow-up of 14 months. During the same period, LV end diastolic diameter improved from 58.9 mm to 55.1 mm and left atrial diameter improved marginally from 49.0 mm to 48.5 mm.
The present studies further reveal that pulmonary vein isolation conveys a better protective effect on LV function, evident with superior reversal of LV function compared to AV-node ablation and medical therapy. According to Lishmanov et al. [34], PVI is an efficacious rhythm control method because it works by isolating pulmonary vein, which is the main source of approximately 90% of atrial fibrillation. The only downside of PVI is it may require more than one procedure for a successful isolation of the pulmonary vein [34]. Two early studies [85,86] have also demonstrated that PVI improves LV function by reversing LVEF values from 35% to 56% within the first three months similar to individuals with normal LV function. AV node ablation on the other hand, is a rate control strategy usually recommended for TIC patients who are refractory to medical therapy or showing difficulties in rate control. The strategy has been shown to be effective in patients with significantly depressed LV function (LVEF < 45%).
In the present findings, PVI has superior protective effect against tachyarrhythmias (especially AF) to AV node ablation. However, the difference might be partly explained by the few studies using AV-node ablation, which also had shorter follow-up period compared to PVI therapy. In addition, other important clinical outcomes such as procedural safety, complications, survival and quality of life associated with PVI and AVNA were not assessed in the present analysis. Overall, clinical management methods suggest that TIC is a potentially reversible form of cardiomyopathy after the restoration of sinus rhythm but recurrent arteriovenous connections may need more than on procedure.
In summary, the cornerstone of clinical management of TIC is the control of rhythm/rate control achieved through medical therapy, pulmonary vein isolation and AV node ablation. While medical therapy may be the preferred choice, patients who are refractory to rate/rhythm control medication re considered for pulmonary vein isolation or AV node ablation. However, there is need for additional clinical trials to develop standardized guidelines for rate and rhythm control for TIC patients instead of the current reliance of guidelines for management of tachyarrhythmias.
Tachycardia-induced cardiomyopathy (TIC) is a cardiac condition occurring as a consequence of chronic atrial/ventricular tachyarrhythmias or frequent ventricular ectopy resulting into left ventricular dilatation and systolic dysfunction, and subsequently clinical manifestation of systolic heart failure. The main types of tachyarrhythmias are supraventricular tachyarrhythmias (atrial fibrillation, flutter and tachycardia), ventricular tachyarrhythmias, ventricular ectopy, and persistent rapid ventricular pacing. The principal risk factors are type, rate and duration of tachyarrhythmias. Its pathophysiologic mechanism is both predictable and time depended beginning with LV remodeling, neurohormonal activation, cell signaling/viability, and ultimately extracellular remodeling. Although TIC lacks well-established diagnostic criteria, the key diagnostic clues are the presence of pathological tachyarrhythmia or persistent ventricular ectopy (PVC) in the absence of other demonstrable etiologies and progressive restoration of LV function. Reversal of LV function is the key diagnostic feature for differentiation TIC from DCM and other cardiomyopathies accompanied with sustained tachycardia. Sinus rhythm restoration is the mainstay therapeutic target in the clinical management of TIC. Restoration can be achieved through pharmacologic therapy. For patients non-responsive to medical therapy, arteriovenous node ablation for rate control, or catheter ablation (pulmonary vain isolation) for rhythm control may be considered. However, the superiority of rate or rhythm control in the management of tachycardia in patients with tachycardia-induced cardiomyopathy remains vaguely understood.





