Objective: To introduce a new rehabilitative technique using a dynamic counterstrain with a weighted kypho-orthosis (WKO) in an exercise program to reduce neck pain and cervicogenic headache in kyphosis.
Background: Cervicogenic headaches can often be related to forward neck and head posture and subsequent overstraining of the supporting extensor muscles. This can be seen in patients with reduced axial muscle strength or kyphotic posture. We postulated that the introduction of a WKO worn behind the back can help produce counterstrain, enhance spinal extension, and reduce pain.
Methods: Twenty-seven patients (age range 31-83, mean age 60.6 years) with headache, neck pain, and hyperkyphosis (thoracic kyphosis ³ 40º) which was not responsive to common interventions were included in this case series. Anteroposterior and lateral spine radiographs were obtained; patients underwent neurologic and musculoskeletal evaluations and assessment of pain, gait, and physical activity. Patients who had pain reduction with the initial trial of a weighted support of 0.5 to 1.5 kg WKO were enrolled in the Spinal Proprioceptive Extension Exercise Dynamic (SPEED) program. Patients were instructed to perform the SPEED exercises while wearing the WKO support (wear 20-30 minutes 2 or 3 times daily) to decrease the pain and kyphosis. Each was asked to decrease the use of WKO when improvement in pain was noted. At follow-up, patients had assessment of headache, cervicothoracic pain, and posture.
Results: The Medical records of 27 consecutive patients with diagnosis of cervicogenic headache were reviewed. Duration of follow up ranged from 1-12 months, mean 5.5 months. All patients showed reduction of both headache and analgesic use along with improvement in kyphosis and neck pain. Complete pain relief was achieved in 21 of the 27 patients.
Conclusions: Reduction of kyphosis through the SPEED program may affect reorientation of cervicothoracic facet joints through mechanical dynamic counterstrain. Mechanical alignment of spine decreases contraction of cervicothoracic extensors and reduces cervicogenic pain. This intervention in this group of patients with kyphosis can decrease neck pain and decrease use of analgesics , especially important in the elderly with a higher risk of falls.
cervicogenic headache, kyphosis mechanical intervention, weighted kypho-orthosis
Abbreviations
ICHD-3 beta: The International Classification of Headache Disorders, 3rd Edition (beta version); SPEED: Spinal Proprioceptive Extension Exercise Dynamic; WKO: weighted kypho-orthosis
Headaches are very common problem. In the United States, 3-month prevalence of severe headaches ranges from 16.6 to 22.7% while in some countries headache prevalence as high as 60% has been reported [1,2]. It is therefore not surprising that headache is one of the most common disorders seen in outpatient clinics. Defining the aetiology of headaches may require diagnostic tests to distinguish between primary and secondary headache disorders. The International Classification of Headache Disorders, 3rd Edition (beta version) (ICHD-3 beta) is the currently accepted diagnostic manual and classification system for the multiple-headache disorders [3]. Although pharmacotherapy is often the first approach for management of most primary headaches, for certain secondary headaches, such as cervicogenic headaches, physical and mechanical managements may also need to be considered.
According to ICHD-3 beta, cervicogenic headache is caused by disorders of the cervical spine, including its bony, disc, or soft tissue components in any combination [3]. We report a cohort of patients with kyphosis-related cervicogenic headaches which responded favourably to an exercise program incorporating a weighted kypho-orthosis (WKO) aimed at correction of posture.
There is dearth of published literature on the role of spinal proprioceptive re-education through mechanical loading to improve cervicogenic headache. Treatment programs have included traction, corticosteroid injection, and exercises to improve posture usually in conjunction with analgesic medications. The underlying problem of malalignment and overload of cervicothoracic extensors is often ignored. Corticosteroid injections of the painful areas may have temporary effect but do not address the fundamental problem of cervico-thoracic malalignment. In this communication, we present the outcome of a defined intervention [5], a dynamic counterstrain device placed on the thoracic spine, that potentially reduced cervicogenic pain by reducing thoracic kyphosis, improving alignment of the cervico-thoracic spine and affecting the proprioceptors of the vertebral facet joints.
The review of the present case series was approved by our Institutional Review Board. Baseline patient characteristics were gathered by retrospective review of the electronic health record. Twenty-seven patients who had headache and neck pain with hyperkyphosis (thoracic kyphosis ³ 40º), and who had not responded to standard interventions were included in this program. Only patients that had cervicogenic headaches that failed all standard management options were recruited. Magnetic resonance imaging had been obtained for all patients to rule out relevant intracranial pathologies as a cause of the headache. Giant cell arthritis had been ruled out before referral of the patients to the physical medicine department. The reported past interventions included common pharmaco-therapeutic measures for management of headache, kyphosis and osteoporosis; physical therapy; heat and massage; and relaxation exercise for headache and for neck and back pain. Extensive chiropractic and physical therapeutic measures, including manipulation, traction, and conventional posture training programs and spinal orthotics, had been provided for neck pain, without any success. All patients before enrolment in the present program had reported a failure of previous therapeutic trials. The average duration of pain was 4.5 (SD: 5.8) years before participating in the program. Characteristics of the patients are reflected in table 1.
Table 1. Baseline characteristics of the 26 patients with persistent neck pain and headaches
Line No |
Sexa |
Age, yb |
Pain Scorec
(Range, 4–10) |
Diagnosis |
1 |
F |
78 |
8 |
Kyphosis, thoracic compression, HA |
2 |
F |
69 |
5 |
Osteopenia, severe kyphosis, lumbar hyperlordosis, HA |
3 |
F |
47 |
10 |
Migraine HA, kyphosis, myofascial pain, anxiety disorder, osteopenia |
4 |
M |
64 |
8 |
Kyphosis, osteoporosis, HA, vert comp fx |
5 |
F |
31 |
9 |
Leg length discrepancy, DJD C-spine, HA, kyphosis, myofascial pain, migraine |
6 |
M |
51 |
8 |
DJD C-spine, neck pain, HA, kyphosis |
7 |
F |
58 |
6 |
Kyphosis, HA, DJD C-spine, kyphoscoliosis, leg length discrepancy |
8 |
F |
39 |
10 |
HA, kyphotic posture, post heart and kidney transplantation, osteoporosis |
9 |
M |
77 |
10 |
HA, kyphosis, neck pain, DJD C-spine |
10 |
F |
58 |
7 |
HA, osteopenia, kyphosis |
|
11 |
F |
83 |
6 |
Kyphosis, anterior subluxation C4/C5 and C7 on T1, HA |
12 |
M |
64 |
8 |
HA, kyphosis, osteoporosis, vert comp fx |
13 |
F |
83 |
8 |
HA, neck pain, kyphosis, osteoporosis |
14 |
M |
62 |
7 |
Degenerative arthritis at multilevels of spine, malposture,HA |
15 |
F |
72 |
8 |
Severe kyphosis, vert comp fx, DJD C-spine, unsteady gait,HA |
16 |
F |
53 |
8 |
Myofascial C-Th pain, kyphosis, DJD C-spine,cervicalgia |
17 |
F |
70 |
4 |
HA, myofascial C-Th pain, kyphosis |
18 |
F |
31 |
10 |
Kyphosis, lumbar lordosis, myofascial C-Th pain, HA, leg length discrepancy |
19 |
F |
31 |
9 |
Myofascial C-Th pain, HA |
20 |
F |
64 |
8 |
Pain in neck, upper back, bilateral shoulder, HA |
21 |
F |
77 |
5 |
Kyphosis, HA, unsteady gait, osteoporosis |
22 |
M |
62 |
8 |
Kyphosis, HA, DJD C-spine |
23 |
F |
69 |
9 |
HA, osteoporosis, kyphosis, DJD C-spine |
24 |
F |
66 |
8 |
HA, subluxation C4/C5 and C7/T1 |
25 |
F |
55 |
8 |
HA, myofascial C-Th pain, kyphosis |
26 |
M
| 64
| 8
| Osteogenesis imperfecta, C-Th pain, HA, osteoporosis with vert comp fx |
27 |
F |
56 |
8 |
HA, cervicalgia, flexion yoga poses |
C-Th: Cervicothoracic; C-spine: Cervical Spine; DJD: Degenerative Joint Disease; F: Female; HA: Headache; M: Male; Vert comp fx: Vertebral compression fracture; OP: Osteoporosis
a of patients, 20 were women and 7 were men.
b Mean age, 60.7 years.
c Mean pain level at baseline, 8
Radiographs
All patients had anteroposterior and lateral radiographs of the entire spine obtained at a standard target-to-film distance. Radiographs from the baseline and follow up evaluations were compared when available [7]. All radiographs were reviewed for evidence of compression fractures in the spine. Using the Cobb technique [7], thoracic kyphosis was measured to define kyphosis greater than 40°. For the patients who could not return for radiographic evaluation (9/27), their medical histories were reviewed for the outcome of the intervention as related to their neck pain and headaches.
Intervention
All patients had neurologic and musculoskeletal evaluations and had assessment of pain, gait, and physical activity. They were instructed in a home exercise program with emphasis on relaxation of cervical extensors and strengthening of back extensors to decrease kyphosis (Figure 2). To compensate for the forward weight of the head (a deforming force, contributing to the mal-alignment of spine) a weighted kypho-orthosis (WKO) was applied posteriorly to the thoracic spine to help bring the head to a more neutral position. Patients were instructed to apply the weight below the inferior angles of the scapulae (Figure 2). The pouch contained 0.5 to 1.5 kg based upon patients’ upper body anatomy. This was determined at the time of initial evaluation. The WKO was to be applied for 20 to 30 minutes, 2 to 3 times daily until the axial posture training and contraction of the thoracic extensors could be performed without difficulty [4,8] (Figure 3). To improve the compliance with the program, all patients had a trial of WKO initially and were provided the details of the program, and diagrams of the exercises to follow at home while wearing the WKO.
Postural exercises to improve use of cervicothoracic extensors and relaxation exercises for posterior neck, trapezii, and pectorals were provided through Spinal Proprioceptive Extension Exercise Dynamic (SPEED) program [5,8,9] (Figure 3). Before and after pain scores were obtained, and student’s t-test was used to calculate change.
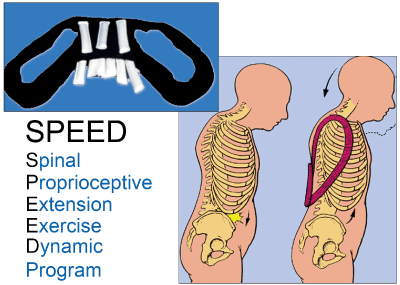
Figure 2. Application of weighted kypho-orthosis as used in the SPEED Program. Figure shows the effect of the addition of 1- to 3-lb weight in the pouch, in accordance with the patient’s musculoskeletal need. Weighted kypho-orthosis is applied below T10 or at a lower level of the spine that would decrease kyphosis. SPEED (Spinal Proprioceptive Extension Exercise Dynamic)
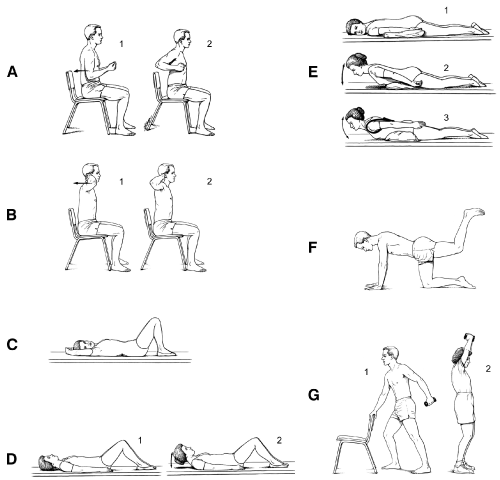
Figure 3. Figures depict progressive back extension exercise program. The rehabilitation of osteoporosis exercise program (ROPE) was designed to address posture and reduce risk of vertebral fracture. (Adapted from Sinaki M. Exercise for patients with osteoporosis: management of vertebral compression fractures and trunk strengthening for fall prevention. PM R. 2012 Nov 4;4[11]:882-8. Used with permission.)
This cohort of 27 patients consisted of twenty women and 7 men (Range: 31–83 years, average: 60.6 years, SD: 16 years). The duration of follow up ranged from 1–12 months, average: 5.5 months.
Patients’ neurologic evaluations showed no relevant deficits. Initially all patients had thoracic hyper kyphosis (kyphosis > 40°). On radiographic follow up the kyphosis angle had decreased more than 5 degrees (Figure 4). Table 1 shows patient gender, age, diagnoses, and pain level at baseline (0 [no pain] to 10 [maximum, unbearable pain]). Initial pain ranged from 4 to 10 on the pain scale (average: 7.8, SD: 1.7); on follow-up, pain ranged from 0 to 4 (average:1.0, SD: 2.3), resulting in a mean change of 6.8 (p < 0.0001) complete pain relief was achieved in all but 6 of the 27 patients. Their symptoms, which initially varied from severe headache, neck and upper back pain and sometimes also nagging flank pain had subsided or reduced substantially. All reported reduction in use of analgesics and no further complaint of headaches. During the trial the patients were able to decrease forward position of the head, neck and thoracic kyphosis while wearing the weight. (Figure 3,4).
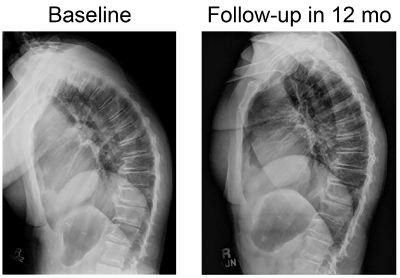
Figure 4. Radiographs show reduction of kyphosis from baseline to 12-month follow-up.

Figure 5. Initial change in height and posture with application of weighted kypho-orthosis.
In agreement with the ICHD-3 beta, cervicogenic headache is pain referred to the head from a source in the cervical spine, and its definitive diagnosis requires evidence of a cervical source of pain [3,10]. The exact prevalence of cervicogenic headache is unknown but appears to occur in 0.17 to 4.10% of the general population [11,12] and is believed to be one of the most common secondary headache disorders, typically presenting as chronic daily headache syndrome [12,13].
Many causes for cervicogenic headache have been reported, including tumours, infections, rheumatoid arthritis, and other processes affecting the upper cervical spine. Although the C2-C3 intervertebral disk and lateral atlantoaxial joint have been implicated as a source for pain in cervicogenic headaches, the C2-C3 facet joint disorder [10] is thought to be the predominant mechanism for pain referral resulting from convergence between cervical and trigeminal afferents in the trigeminocervical nucleus, where nociceptive afferent fibers from C1, C2, and C3 spinal nerves converge on second-order neurons that also receive afferents from adjacent cervical nerves and the trigeminal nerve through the trigeminal nerve spinal tract [14]. This convergence allows pain perception in distributions beyond the expected upper cervical dermatomes and into the parietal, frontal, and orbital regions [14]. Currently there is paucity of information on cervicogenic headache caused by cervicocephalic malalignment posture. Our patients’ headaches strictly met ICHD-3 beta criteria for cervicogenic headaches. To our knowledge, this is the first study that documents occurrence of cervicogenic headaches in the setting of cervicothoracic malalignment supported by response to correction of posture. Pain reduction was achieved through mechanical loading for facet reorientation and proprioceptive re-education.
Some headaches are related to overuse of posterior cervical muscles in the setting of mal-posture of the spine [15]. Several factors can influence one’s posture (i.e., strength of supportive muscles, axial spinal integrity, aging and breast size). When there is thoracic kyphosis, the cervical spine shifts to the front of the line of gravity. This line normally passes through an aligned cervical spine. Therefore, the weight of the head will add to the deforming forces (Figure 1). Neck extensors then would need to work harder. Kyphosis -related myofascial strain can result in neck pain, cervico-occipital pain, back fatigue, and reduced level of physical activity.
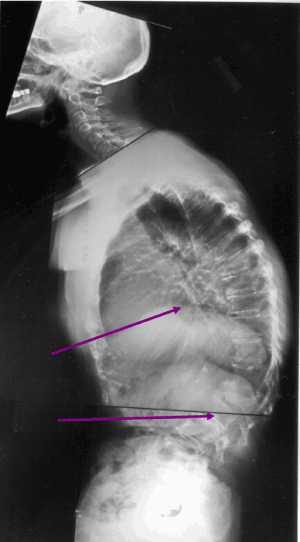
Figure 1. Midthoracic and thoracolumbar kyphosis. Kyphosis can occur with or without vertebral fracture. Vertebral fractures (arrows) usually occur in the midthoracic and thoracolumbar spine.
The improvement in the pain levels after using WKO suggests that the WKO may help realign the spine. We noted positive results from the mechanical intervention aimed at decreasing thoracic kyphosis. Maintenance of axial posture is a dynamic process governed by relationship of the anatomical units of spine to one another at any given moment. Given the weight of the head, it is unlikely that a 1-1.5kg weight could balance out the weight of the cranium without other mechanisms. The efficacy of this particular program may be related to the alignment of the zygapophyseal joints. These joints may be reoriented with the WKO, and the better alignment may improve proprioceptive feedback, thus improving posture. Measures that can be implemented for prevention or treatment of kyphosis could potentially decrease cervicalgia of mal alignment (4) (Figure 2).
While it is difficult to draw firm conclusions based on the case series study design, it is very encouraging that 21/27 patients had complete resolution of their cervical headaches after participating in the program. Future studies looking at the long-term effects of WKO would be interesting, but this is outside the scope of the current study.
Headaches differ in aetiology and therefore frequently need diagnostic tests to establish the exact cause. We report headaches related to overuse of posterior cervical muscles in the clinical setting of thoracic hyperkyphosis. This subtype of cervicogenic headache appears to be a well-defined condition that can be treated conservatively and non-pharmacologically. The SPEED program affects reorientation of cervicothoracic facet joints through dynamic/ mechanical reduction of kyphosis. Application of WKO creates static reduction of kyphosis, facilitation of back extensor counterstrain, trapezius relaxation, and pain relief and reduction in analgesic use.
The authors declare that there is no conflict of interest. The SPEED program has been developed by one of the authors (MS) and the efficacy is evidence based through research at Mayo Clinic. There is no financial disclosure for the authors.
- Radtke A, Neuhauser H (2009) Prevalence and burden of headache and migraine in Germany. Headache 49: 79-89. [Crossref]
- Smitherman TA, Burch R, Sheikh H, Loder E (2013) The prevalence, impact, and treatment of migraine and severe headaches in the United States: a review of statistics from national surveillance studies. Headache 53: 427-36. [Crossref]
- Headache Classification Committee of the International Headache Society (IHS) (2013) The International Classification of Headache Disorders, 3rd edition (beta version). Cephalalgia 33: 629-808. [Crossref]
- Sinaki M (2003) Critical appraisal of physical rehabilitation measures after osteoporotic vertebral fracture. Osteoporos Int 14: 773-9. Erratum in: Osteoporos Int. 2006;17(11):1702. [Crossref]
- Sinaki M, Brey RH, Hughes CA, Larson DR, Kaufman KR (2005) Significant reduction in risk of falls and back pain in osteoporotic-kyphotic women through a Spinal Proprioceptive Extension Exercise Dynamic (SPEED) program. Mayo Clin Proc 80: 849-855. [Crossref]
- Sinaki M (2013) Yoga spinal flexion positions and vertebral compression in osteopenia or osteoporosis of spine: case series. Pain Pract 13: 68-75. [Crossref]
- Itoi E (1991) Roentgenographic analysis of posture in spinal osteoporotics. Spine (Phila Pa 1976) 16: 750-756. [Crossref]
- Sinaki M, Pfeifer M, Preisinger E, Itoi E, Rizzoli R, et al. (2010) The role of exercise in the treatment of osteoporosis. Curr Osteoporos Rep 8: 138-144. [Crossref]
- Sinaki M, Pfeifer M (2015) Treatment of vertebral fractures due to osteoporosis. Role of Posture Training Support (PTS) and Spinal Proprioceptive Extension Exercise Dynamic (SPEED) Program. Osteologie 24: 7-20.
- Bogduk N (2014) The neck and headaches. Neurol Clin 32: 471-487. [Crossref]
- Knackstedt H, Bansevicius D, Aaseth K, Grande RB, Lundqvist C, et al. (2010) Cervicogenic headache in the general population: the Akershus study of chronic headache. Cephalalgia 30: 1468-76. [Crossref]
- Sjaastad O, Bakketeig LS (2008) Prevalence of cervicogenic headache: Vågå study of headache epidemiology. Acta Neurol Scand 117: 173-180. [Crossref]
- Mohammadianinejad SE, Abbasi V, Sajedi SA, Majdinasab N, Abdollahi F, et al. (2011) Zonisamide versus topiramate in migraine prophylaxis: a double-blind randomized clinical trial. Clin Neuropharmacol 34: 174-177. [Crossref]
- Bogduk N, Govind J (2009) Cervicogenic headache: an assessment of the evidence on clinical diagnosis, invasive tests, and treatment. Lancet Neurol 8: 959-968. [Crossref]
- Sinaki M (2010) Kinematics of headaches related to occipito-cervicothoracolumbar malposture: significance of axial muscles in headaches. J Headache Pain S 26





