Rectus sheath hematoma is an uncommon but potentially dangerous and life threatening condition. It is important for the physician to be familiar and comprehend the pathophysiology behind this condition as well as the means to confront it. The rectus sheath hematoma can mimic nearly every abdominal condition. Usually it is self-limited but in some rare cases it can cause hypovolemic shock and endanger the patient's life if remain untreated correctly.
In this article we present a case of a female patient with a history of acute myeloid leukemia, who was treated for thrombosis of the right femoral vein with LMWH. While the patient was hospitalized she presented abdominal pain, a growing mass in the abdominal wall, hemodynamic instability and a drop in the hemoglobin.
The patient initially was treated conservatively with blood transfusion, discontinuation of LMWH and intravenous fluids resuscitation.
The patient was stabilized and abdominal CT revealed a large hematoma of the right rectus sheath with arterial exavascation from a branch of the right inferior epigastric artery (Figure 1).
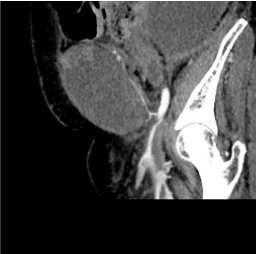
Figure 1. Inferior epigastric artery, Arterial blushing.
Embolization of the right inferior epigastric artery was unavailable and due to continued arterial leakage surgery was proposed.
Intraoperatively, the hematoma was drained and the right inferior epigastric artery ligated. Packing of the remaining cavity was performed with surgical gauzes and the patient was successfully stabilized and revived.
Postoperatively she remained hemodynamically stable and the hemoglobin was increased. On the first postoperative day, the patient was readmitted to the operating room, for second look laparotomy, were the gauzes were removed, there was no sign of hemorrhage and a drainage was placed in the cavity.
Her postoperative course was uneventful.
As a conclusion we want to stress out that the spontaneous rectus sheath hematoma (Figure 2) is a condition that can mimic acute abdomen and the gold standard examination for depicting such a condition is CT scan with IV contrast median. Conservative approach in most cases is sufficient and the condition is self limited (Figures 3,4 and 5). If the conservative approach fails vascular embolization or surgical repair is indicated [1-3].
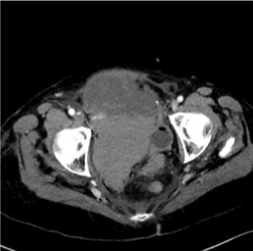
Figure 2. Rectus sheath hematoma.
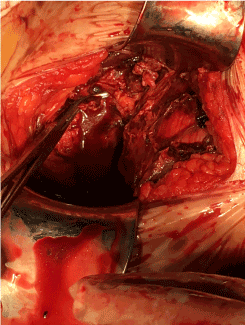
Figure 3. Ligation of the inferior epigastric vessels.
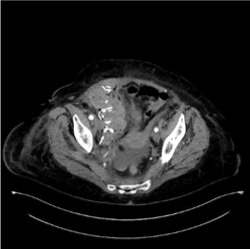
Figure 4. Post-operative image, packing of the cavity.
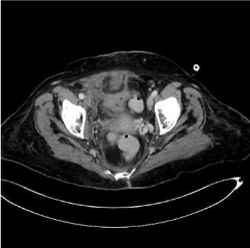
Figure 5. Post-operative evaluation.
- Gradauskas A, Venclauskas L, Pažusis M, Karpavicius A, Maleckas A (2018) Comparison of the different treatment strategies for patients with rectus sheath haematoma. Medicina (Kaunas) 54: E38. [Crossref]
- Delgado Ramos GM, Flor Ramos L, Freire AX (2019) Rectus sheath hematoma manifesting as hemorrhagic shock. Intern Emerg Med 14: 181-182. [Crossref]
- Romic I, Pavlek G, Mance M, Romic M, Moric T (2018) Fatal case of spontaneous rectus sheath hematoma caused by anticoagulant and steroid therapy during hospital admission. Visc Med 34: 225-227. [Crossref]





