A 24-year-old 0-para presented to our department with a history of severe dysmenorrhea and pelvic pain refractory to intensified analgesia and continuous hormonal contraceptive treatment. She underwent expert 2D- and 3D-ultrasound assessment. We used transvaginal (TVU) and transrectal ultrasound (TRU). We found a thick-walled cystic lesion with hypoechoic to ground-glass content, protruding from the right lateral uterine wall below the insertion of the round ligament. There were no signs of adenomyosis or deep invasive endometriosis (DIE). No other pathologies or anatomical anomalies were found on ultrasound or magnetic resonance imaging (MRI). The mass was highly suggestive of ACUM given its morphology, the normally shaped uterine cavity and the absence of adenomyotic features. Due to failure of conservative treatment and ongoing severe interval pain the patient was scheduled for uterine-sparing robotic assisted laparoscopic surgery. The postoperative recovery was uneventful and the woman reported substantial symptom relief at the 3-months follow-up visit. Pathologic analysis suggested ACUM and no histological features of adenomyosis were found. We believe that ACUM is a diagnosis that is not commonly known. TVU or TRU are non-invasive and cost-effective examination techniques to evaluate congenital uterine malformations. Robotic assisted laparoscopic surgery is a safe and feasible way to treat this condition.
ACUM, uterine malformation, dysmenorrhea, gynaecology, adenomyosis, endometriosis, juvenile cystic adenomyosis
Severe dysmenorrhea in young adults and adolescents is known to be associated in about 10% with lesions corresponding to endometriosis and adenomyosis. This leaves a great number of women with a primary dysmenorrhea without clinical findings or lesions [1,2].
In the last years, case reports have been published presenting rare causes of severe, therapy refractory dysmenorrhea. Juvenile cystic adenomyoma (JCA) [2] and accessory cavitated uterine masses (ACUM) [3] are sometimes found to be the reason of dysmenorrhea. Surgical removal has been shown to give symptom-relief or cure for both types of lesions [4,5]. The lesions are described morphologically very much alike each other. The etiology of these conditions is poorly understood. One theory is that ACUM is a uterine malformation resulting from a different etiology than common Müllerian uterine malformations described in the ESHRE/ESGE consensus [6]. The current explanation is that a gubernaculum dysfunction may be responsible for duplication or persistence of paramesonephric tissue leading to accessory uterine tissue [7]. Another theory is that young women in adolescence can develop adenomyotic cysts resulting in Juvenile Cystic Adenomyosis (JCA) [8,9]. The diagnostic criteria are based on a report established in 2007 by Takeuchi et al. Recent data suggest that many of the case reports published as JCA might in fact be ACUM cases [3,10].
Diagnostic accuracy can be achieved using TVU or TRU and in some reports MRI is suggested as a complementary exam to rule out adenomyosis or other Müllerian malformations [11]. The purpose of this report is to raise awareness of ACUM and highlight the importance of systematic ultrasound assessment in young adults and adolescents with severe dysmenorrhea. We also want to highlight the feasibility of robotic laparoscopic surgery as an effective treatment [10,12].
A 24-year-old nulliparous woman was admitted to our emergency outpatient clinic due to severe dysmenorrhea and long history of intermittent lower abdominal pain episodes. Symptoms were intense, periodic pain radiating to right lower quadrant and backpain radiating towards the right leg. The pain was refractory to analgesic medication and oral contraceptives and was escalating in intensity while ongoing menses. The patient had undergone various clinical exams, laboratory and microbiological exams and transabdominal ultrasound (TAS) imaging excluding appendicitis, hip dysplasia, inguinal herniation and muscular causes and had been conservatively treated for suspicion of
liquified myoma.
The patient was referred to our expert ultrasound center where we performed TVU using VolusonⓇ E10 system with a 5-9 MHz 3D transvaginal probe (GE Healthcare, Chicago Illinois, USA).
Ultrasound findings showed a round thick-walled cystic mass protruding from the right lateral uterine wall caudal to the round ligament insertion and cranial of the uterine artery insertion. It partly bulged into the broad ligament and measured 23x24x27mm. It had a central ground-glass to hypoechoic cystic compartment measuring16x15x15mm. The wall consisted of a thin hyperechoic inner lining of about 1mm surrounded by an 8mm of smooth muscle layer (Figure 1). Sono-palpation directly onto the mass revealed site-specific tenderness. 3D-ultrasound reconstruction showed an otherwise normally shaped uterine cavity (Figure 2). There were no signs of adenomyosis, deep infiltrating endometriosis and the ovarian and renal-ureteral anatomy was normal. To optimize pre-operative planning contrast enhanced MRI was performed.
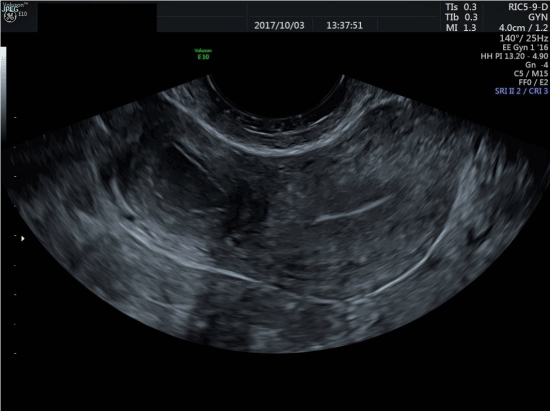
Figure 1. 2D TVU in a transverse section showing an ordinary uterine cavity to the right in the image (patients left) with laterally protruding ACUM, with a visible endometrial lining, and echogenic content suggesting old blood
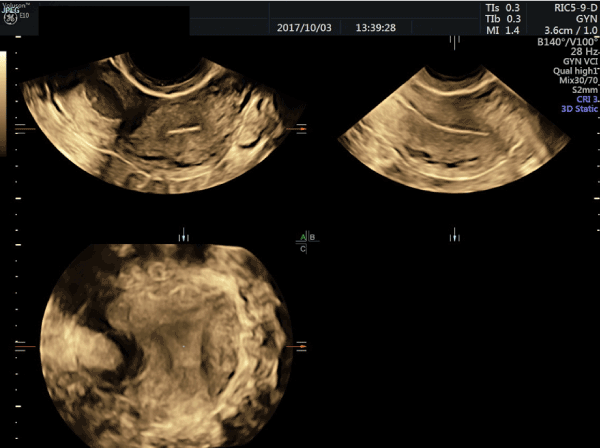
Figure 2. 3D volume of the ordinary shaped uterine cavity and cornua
MRI confirmed a 2-3cm cystic mass protruding from the right uterine wall caudal of the insertion of the round ligament and surrounded by 7-8mm of myometrium (Figure 3). The cyst-content was liquid with high T1 signal suggestive of old blood. Urogenital anatomy was otherwise normal. As the clinical, sonographic, and radiological findings strongly suggested ACUM we planned for uterus-sparing robotically-assisted laparoscopic resection of the mass.
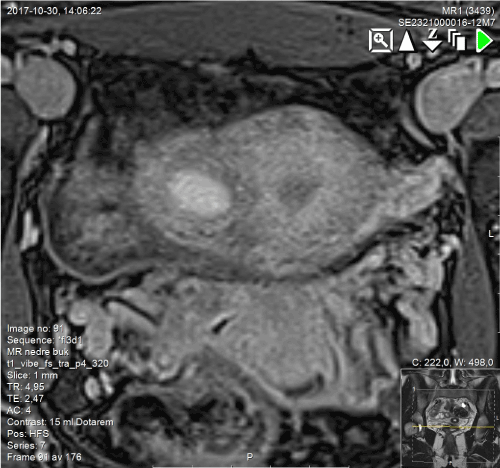
Figure 3. Coronal view in T1 weighed MRI showing transversal section of the uterine fundus incorporating the ACUM and the pericystic enhancement corresponding to a smooth muscle ring
Surgery was performed using Da Vinci S-High definition systemⓇ (Intuitive surgical, Inc, Sunnyvale, CA). The transvaginal intrauterine manipulator was applied to allow better positioning intraoperatively. An intra-abdominal ultrasound probe, the Robotic Drop-In Ultrasound Transducer 8826 was docked to the Da Vinci System and connected to the BK Flex focus 800 Ultrasound SystemⓇ (BK medical, Herlev, Denmark) to localize the mass intraoperatively. The robotic trocars were placed following gynecologic surgery standard procedure. When inspecting the pelvis, the uterine outer contour was found to be asymmetric with a 3cm protrusion between the insertion of the round ligament and the uterine artery. The fallopian tubes had a normal shape and insertion into the uterine body. No other duplications or malformations could be seen intraabdominally. There were signs of superficial peritoneal endometriosis and a biopsy from rectouterine pouch was taken to confirm the diagnosis.
To minimize possible bleeding during dissection we injected 10 IU diluted PitressinⓇ (Monarch Pharmaceuticals Inc, Bristol,TN) on the surface of the protruding bulge after verifying its position with the drop-in Ultrasound probe. The lesion was dissected from the surrounding myometrium using monopolar cautery and scissors. When opened it was filled with thick brown fluid. The uterine cavity was not affected by surgery. The mass was extracted using a bag and sent for analysis. The uterine myometrial defect was closed in a two-layer technique with barbed loop suture (V-loc 2.0Ⓡ, Medtronic, MN). Finally, adhesion prophylaxis (HyalobarrierⓇ, Nordic drugs, Sweden) was applied on the operation site of the uterus. Duration of surgery was 69 minutes. There was no significant blood loss. The surgical procedure is seen on the Film.
The patient had a normal postoperative recovery and was discharged one day after surgery. Macroscopic pathology showed a 2,0 x 1.8 x 1.6 cm large white tissue fragment with irregular surface (Figure 4). Microscopic histology showed mature smooth muscle tissue with a cavity-like space lined with endometrial mucosa containing single inactive glands. This finding primarily suggested ACUM. There were no signs of cystic adenomyosis. The patient had co-existing endometriosis.
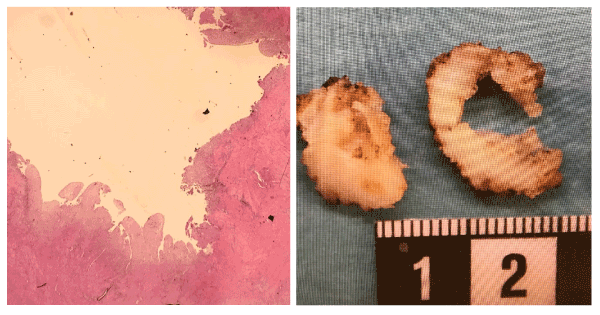
Figure 4. Histology showing a HE staining with a cavity lined by functional endometrial cells without signs of adenomyosis
At the two months of follow-up visit the patient described substantial pain-relief and improved quality of life. TVU showed a normal uterine cavity without signs of pathology.
ACUM is described in literature as an accessory isolated cavitated uterine mass, lined with ordinary endometrial endothelium but with no communication to the normal uterine cavity. It protrudes from an otherwise normally shaped and functional uterus, mostly localized on the lateral uterine wall caudal of the round ligament insertion. The condition is not included in the ESHRE classification systems for uterine malformations, and thus not commonly diagnosed. Lately it has been described in 43 cases [3,10,13,14]. The patients are young, usually less than 30 years old. Their main symptom is severe dysmenorrhea and chronic pelvic pain. There are reports suggesting a co-incidence between ACUM and endometriosis in 5-6% [15].
Traditionally these uterine masses filled with blood have been described as correlated to juvenile cystic adenomoysis (JCA). JCA is described in the literature with defined criteria according to Takeuchi et al. [2]. The morphology and the clinical symptoms are very much alike the ones of ACUM. There are studies implicating that these uterine masses in most cases seem to arise from a malformation rather than being a manifestation of JCA [10]. In several case-reports the mass is always described to be located between the round ligament and the uterine artery. This might support the theory of malformation rather than of an isolated adenomyotic cyst but this has yet to be studied. With a systematic 2D/3D TVU/TRU examination and the knowledge of ACUM as a differential diagnosis, detection should be possible in most cases. The fluid inside the mass has “ground-glass”-echogenicity and it is surrounded by myometrium. With 3D- ultrasound the uterine cavity has normal shape and there are two regular fallopian tubes.
Reviewing existing case reports most women have been treated with laparoscopic surgery. Robotically assisted laparoscopy in uterine malformation surgery has been shown to be of great value and highly feasible and effective [5,16]. Surgical dissection with poorly delineated anatomical borders and uterine suturing technique is simplified by the robotic system´s HD optics, intra-abdominal ultrasound probe, and the wristed robotic instruments. The procedure can be compared to uterine-sparing enucleation of leiomyoma. Patients have shown good recovery and usually leave the hospital same day or day after the surgery.
ACUM is an uncommon Müllerian uterine anomaly not yet classified by ESHRE [3]. There has been a discussion whether it is possible to differentiate ACUM from juvenile cystic adenomyosis (JCA) a condition with similar appearance but presumed different etiology. In both conditions patients are often young and suffer of severe dysmenorrhea. In both conditions surgical approach has shown improvement of pain. We believe that it is important to spread information about the feasibility of ultrasound diagnosis and surgical treatment for patients with ACUM and JCA. 2D and 3D TVU or TRU represents a cost-effective and non-invasive way to diagnose patients with ACUM. MRI should only be considered when specialist-ultrasound is inconclusive. Raised awareness of ACUM diagnosis promotes earlier access to treatment. Surgical treatment by experienced laparoscopic or robotic surgeons was feasible and resulted in substantial symptom-relief.
- Harel Z (2012) Dysmenorrhea in adolescents and young adults: an update on pharmacological treatments and management strategies. Expert Opin Pharmacother 13: 2157-2170. [Crossref]
- Takeuchi H, Kitade M, Kikuchi I, Kumakiri J, Kuroda K, et al. (2010) Diagnosis, laparoscopic management, and histopathologic findings of juvenile cystic adenomyoma: a review of nine cases. Fertil Steril 94: 862-868. [Crossref]
- Acien P, Acien M, Fernandez F, Jose Mayol M, Aranda I (2010) The cavitated accessory uterine mass: a Mullerian anomaly in women with an otherwise normal uterus. Obstet Gynecol 116: 1101-1109. [Crossref]
- Peters A, Rindos NB, Guido RS, Donnellan NM (2018) Uterine-sparing laparoscopic resection of accessory cavitated uterine masses. J Minim Invasive Gynecol 25: 24-25. [Crossref]
- Persson J, Bossmar T, Teleman P (2010) Robot-assisted laparoscopic surgery for a rudimentary uterine horn with two non-communicating cavities. J Robot Surg 4:137-140. [Crossref]
- Grimbizis GF, Gordts S, Di Spiezio Sardo A, Brucker S, De Angelis C, et al. (2013) The ESHRE/ESGE consensus on the classification of female genital tract congenital anomalies. Hum Reprod (Oxford, England) 28: 2032-2044. [Crossref]
- Acien P, Sanchez del Campo F, Mayol MJ, Acien M (2011) The female gubernaculum: role in the embryology and development of the genital tract and in the possible genesis of malformations. Eur J Obstet Gynecol Reprod Biol 159: 426-432. [Crossref]
- Chun SS, Hong DG, Seong WJ, Choi MH, Lee TH (2011) Juvenile cystic adenomyoma in a 19-year-old woman: a case report with a proposal for new diagnostic criteria. J Laparoendosc Adv Surg Tech A 21: 771-774. [Crossref]
- Brosens I, Gordts S, Habiba M, Benagiano G (2015) Uterine cystic adenomyosis: A disease of younger women. J Pediatr Adolesc Gynecol 28: 420-426. [Crossref]
- Garofalo A, Alemanno MG, Sochirca O, Pilloni E, Garofalo G, et al. (2017) Accessory and cavitated uterine mass in an adolescent with severe dysmenorrhoea: From the ultrasound diagnosis to surgical treatment. J Obstet Gynaecol 37: 259-261. [Crossref]
- Acien P, Acien M (2016) The presentation and management of complex female genital malformations. Human Reproduction Update 22: 48-69. [Crossref]
- Kriplani A, Mahey R, Agarwal N, Bhatla N, Yadav R, et al. (2011) Laparoscopic management of juvenile cystic adenomyoma: four cases. J Minim Invasive Gynecol 18: 343-348. [Crossref]
- Bedaiwy MA, Henry DN, Elguero S, Pickett S, Greenfield M (2013) Accessory and cavitated uterine mass with functional endometrium in an adolescent: diagnosis and laparoscopic excision technique. J Pediatr Adolesc Gynecol 26: e89-e91. [Crossref]
- Jain N, Verma R (2014) Imaging diagnosis of accessory and cavitated uterine mass, a rare mullerian anomaly. Indian J Radiol Imaging 24: 178-181. [Crossref]
- ACOG Committee Opinion. Number 310, April 2005 (2005) Endometriosis in adolescents. Obstet Gynecol 105: 921-927.
- Akar ME, Leezer KH, Yalcinkaya TM (2010) Robot-assisted laparoscopic management of a case with juvenile cystic adenomyoma. Fertil Steril 94: e55-e56. [Crossref]




