Background: Studies find that while there is an increase in general awareness of HPV, many misconceptions about HPV and the vaccine remain. An individual’s adoption of HPV vaccination should be influenced, in part, by the behaviour of others in their network. Understanding differences between HPV vaccine adopters and nonadopters when it comes to trust in sources, knowledge of HPV and HPV vaccines, and individual networks are critical as vaccine decisions are rarely made without consultation with others in the individual’s social network.
Methods: An online survey of students attending a Northern California university (N=346) assessed HPV vaccination sources of information, knowledge, and adoption among young adults.
Results: Seventy-seven percent of respondents reported relying on the internet when initially seeking health or medical information. Respondents who received the HPV vaccine were more likely than unvaccinated respondents to know that HPV causes cancer (70% vs. 43%) and that it is sexually transmitted (80% vs. 62%). Vaccinated individuals are more knowledgeable about HPV and the HPV vaccine than non-vaccinated young adults. Social network differences are visible between vaccinated and unvaccinated respondents.
Conclusion: The likelihood that a young adult will be vaccinated against HPV was positively related to whether the individual was part of the decision to vaccinate, whether the individual’s parent(s) were a part of the decision to vaccinate, whether or not they believed their family members to also have been vaccinated, and the density of their social network.
social network factors, HPV information sources, HPV vaccine
The Centres for Disease Control and Prevention (CDC) estimates that 20 million Americans are infected with the human papillomavirus (HPV), with six million new cases a year [1]. While HPV vaccines are highly effective, vaccine adoption among young men and women in the United States remains low [2]. Studies find that while there is an increase in general awareness of HPV, many misconceptions about HPV and the vaccine remain [3].
Misconceptions about HPV are likely to vary depending on an individual’s social network. There is evidence that trusted sources in women’s social networks encouraged them to be vaccinated [4]. Researchers have posited that social networks affect health through five basic mechanisms: social support, social influence, access to resources (e.g., information), social involvement, and person-to-person contagion. Because people’s social networks shape the information, they are likely to possess, network analytic methods can advance our understanding of the social influence processes involved in the adoption of behaviours [5].
Threshold models of collective behaviour work to explain the social influence process. The models suggest that an individual engages in behaviour based on the proportion of people in the social systems that are already engaged in that behaviour [5]. According to threshold models of collective behaviour, an individual’s adoption of HPV vaccination should be influenced, in part, by the behaviour, or perceived behaviour, of others in their network. The collective behaviour threshold is the proportion of adopters in a system before an individual’s adoption. However, individuals may not correctly discern the adoption behaviour of everyone in their system. This is especially true for unobservable innovations such as HPV vaccination adoption (i.e. we cannot “see” if someone has had the HPV vaccine or not unlike being able to “see” if someone, for example, taken up smoking). Therefore, questions about the individual’s behaviour(s) are reduced to perceptions of the individual’s social network.
The purpose of this study is to look at differences between HPV vaccine adopters and nonadopters when it comes to trust in sources, knowledge of HPV and HPV vaccines, and individual networks. In addition to demographic factors, HPV source information and social network factors were assessed.
Participants and procedures
This cross-sectional study recruited students by convenience sampling from a Northern California university (N = 346). Students involved in undergraduate social clubs or enrolled in undergraduate communication courses that offered extra credit for research participation were invited to complete a web-based survey during February and March 2015. The majority of respondents were female (66%) Asian (46%, followed by White, non-Hispanic, 34%), sexually active (66%), and heterosexual (92%).
After providing informed consent, participants completed a questionnaire assessing demographic characteristics, initial health-seeking behavior, HPV vaccine adoption status, HPV vaccine decision making, HPV and HPV vaccine information source trust, HPV and HPV vaccine knowledge, network perceptions of HPV adoption, and social network homophily and density.
Measures
Although social networks are naturally complex, they tend to exhibit fundamental patterns [6]. Two fundamental dimensions of network structure are density and homophily [7]. Social network density is a common measure of how well connected a network is, or how closely knit it is. Density is often used to compare networks against each other. Homophily is the tendency to relate to people with similar characteristics and often leads to the formation of homogenous groups. Extreme homogenization can negatively impact access to information that is novel to the group. Both density and homophily are supposed to influence the viral spread of beliefs and behaviours [8].
The survey contains 39 items with eight content domains. These domains include (1) demographics (five items), (2) initial health-seeking behavior (one item), (3) HPV vaccine adoption status (two items), (4) HPV vaccine decision-making (two items), (5) HPV and HPV vaccine source trust (ten items), (6) HPV and HPV vaccine knowledge (four items), (7) network perceptions of HPV adoption (six items), and (8) social network homophily and density (nine items). Of the 39 items, 30 were borrowed or modified from existing survey instruments, and nine were newly constructed.
Respondent characteristics
Respondents provided the usual demographic data and information about their health information-seeking behaviour based on HPV vaccine adoption status. Respondents were classified as HPV Vaccine Adopters if they gave “Yes” as a response to the question “Have you been vaccinated against HPV?” and nonadopters if they did not (1 = nonadopter; 2 = adopter). Respondents were classified as “involved in HPV vaccine decision making” if they gave “Yes” as a response to the question “Did you have any say in whether or not you were vaccinated against HPV?” Parent(s) were classified as “involved in HPV vaccine decision making” if “Yes” was selected for the answer to the question “Was the decision to get vaccinated or not get vaccinated for HPV made for you by your parent(s) or guardian(s)?”
Source trust
The question: “In general how much would you trust the following sources for information about health topics?” assessed source trust. To assess source trust about the HPV vaccine the following question was used: “Do you trust the following sources for information about the HPV vaccine?” Responses were “Yes” or “No” (1 = Yes; 2 = No) for both questions and assessed trust of the following sources: (a) Doctor, nurse or other health care professionals; (b) One or more family members; (c) Newspaper of magazine articles; (d) Television news stories; (e) Television entertainment programs; (f) Public service announcements; (g) The internet; and (h) Radio. “Yes/No” responses were used in favour of rating scales to better meet the assumptions of the number system, a problem that frequency counts and proportions avoid [9].
HPV and HPV vaccine knowledge
Two items assessed if respondents had heard of HPV and/or the HPV vaccine. For HPV, respondents answered “Yes” or “No” (1 = Yes; 2 = No) to the question: “Before today, had you ever heard of the human papillomavirus, or HPV?” For HPV vaccines, respondents answered “Yes” or “No” (1 = Yes; 2 = No) to the question: “Before today, had you ever heard of the HPV vaccine or shot?” Three items assessed HPV knowledge, each of which began with “Do you think” (a) HPV can cause cervical cancer; (b) you can get HPV through sexual contact; and (c) HPV can go away on its own without treatment. Responses were “Yes,” “No,” or “Unsure” (1 = Yes; 2 = No, 3= Unsure).
Network perceptions of HPV vaccine adoption
Six items assessed network perceptions of HPV vaccine adoption: (a) Most college students, in general, have had the HPV vaccine; (b) Most students at this university have had the HPV vaccine; (c) Most of my classmates have had the HPV vaccine; (d) Most people in my school club(s) or group(s) have had the HPV vaccine; (e) Most of my close friends have had the HPV vaccine; and (f) Most of my family members (siblings, cousins, etc.) have had the HPV vaccine. Responses were “Yes” or “No” (1 = Yes; 2 = No).
Social network density and homophily
Respondents identified three people in their social networks for the following three social networks: (a) people they discuss important matters with; (b) people they spend the most free time with; and (c) people who they turn to for health information. Six items assessed social network density, each of which began with “considering the people you identified, how close are they to each other?” Respondents selected “Total Strangers” and “Are very close” (1 = stranger; 2 = close) for each of the people they identified. Three items assessed social network homophily, each of which began with “considering the people you identified” and asked: (a) What is their sex?; (b) Are they in a club or group at your school?; and (c) Are they a family member or close friend? Responses were “Yes” and “No” (1 = Yes; 2 = No). While many homophily indexes are commonly used, based on this sample, we could not differentiate on some commonly used indexes such as age and neighbourhood because university student populations tend to have limited variability in these areas. Socioeconomic factors are also often used as indexes as homophily, but again, university student populations do not tend to have specific information on socioeconomic markers of their families.
Data analysis
Descriptive statistics characterized the study population and information-seeking behaviours. Z-tests determined source trust about HPV and HPV vaccine information, HPV and HPV vaccine information source trust differences between HPV vaccine adopters and nonadopters, and knowledge of HPV and HPV vaccine differences by HPV vaccine adoption status. Chi-square tests assessed the association between HPV vaccine adoption and perception of individual social network’s HPV adoption status. Binomial logistic regression examined the relationship between social network density and homophily on HPV vaccine adoption status. The multivariate model included all variables that were found in the bivariate analysis to be associated with the dependent variable with statistical significance (p < 0.05). Sensitivity analysis was performed by removing individual variables to assess their impact on the multivariate summary statistics.
The majority of respondents (77%) reported relying on the internet when they initially sought information about the HPV vaccine (Table 1). Regardless of vaccine adoption, 97% of respondents reported their doctor, nurse, or healthcare provider as their most trusted source of information about the HPV vaccine (Table 2). Significant differences were found between vaccinated and unvaccinated respondents in their trust of family members for health information. Vaccinated young adults (75%) were more likely to trust family members for information about HPV vaccines than non-vaccinated young adults (60%). Based on HPV vaccine adoption status, there were no significant differences for the other sources of HPV vaccine information.
Table 1. Sample demographic statistics and initial sources of health information
Considering social network characteristics, grouped by vaccine adoption status, showed significant differences in their network structure (Table 4, Figure 1). The unvaccinated had more densely connected networks with vaccine adopters noting a more open network. A chi-square test of independence examined the relation between HPV vaccine adoption and perceived network vaccine adoption. The relations between these variables was significant X2 (1, N = 346) = 52.55, p <0 .01. Young adults who adopted the HPV vaccine were more likely to perceive HPV vaccine adoption in their network. Nonadopters were more likely to report that those in their network are also unvaccinated.
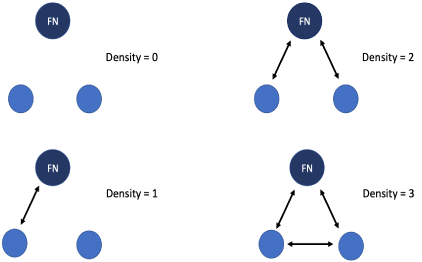
Figure 1. Levels of density based on self-identified connections. FN identifies the focal node in the network.
Table 4. Social network connections
Differences were also found in the individual’s perceptions of their network’s vaccination adoption status. Eighty-seven percent of vaccine adopters perceive their close friends to have been vaccinated, compared to 58% of nonadopters. Vaccinated individuals also perceived most of their family members to be vaccinated (87%), compared to 53% of nonadopters. Vaccine adopters described their close networks as being same-sex (82%) or comprised of equal amounts of men and women (18%). Nonadopters perceived their social network as comprising more of the opposite sex (58%). They were also more likely to discuss important matters with friends (94%) and family (81%) as compared to nonadopters (friends, 84%; family 73%). In terms of health topics, vaccine adopters relied on communication with family members (87%) more than nonadopters (74%), with nonadopters relying slightly more on friends (78%) than nonadopters (76%).
Looking more closely at adoption status, general factors related to young adult HPV vaccination status were: 1) an individual’s network structure (density and homophily), 2) the individual’s perceptions of their network’s vaccination adoption status, and 3) who was involved with vaccination decision-making. A test of the full model against the intercept-only model (null model) was statistically significant (predicting 83% and 51% respectively), indicating the predictors as a set reliably distinguished between those vaccinated and not vaccinated, χ2 (4) = 192.85. p < 0.001. Nagelkerke’s R2 of .58 indicates a moderate relationship between prediction and grouping (Table 5).
Table 5. Results from the logistic regression on HPV vaccine adoption status. Note: R2 = .79 (Hosmer & Lemeshow), .43 (Cox & Snell), .58 (Nagelkerke). Model X2(4) = 192.85, p < .01
The findings indicate that young adults who received the HPV vaccine were more knowledgeable about HPV and the HPV vaccine than nonadopters. It could be that individuals vaccinated at a young age attend to information about the HPV vaccine when it is incidentally present. While there was a significant relationship between vaccine adoption and HPV knowledge, it is not clear if adopters learned about the vaccine before or after vaccination.
Regardless of adoption status, the vast majority of respondents report their doctor, nurse, or health practitioner to be their most trusted source of information on HPV and HPV vaccines. Consistent with previous research, vaccine adopters were also more likely to trust family members for information on HPV and HPV vaccines [10]. This finding could indicate that the vaccinated individual’s network itself is made up of more knowledgeable individuals, therefore making the respondent more knowledgeable. It can also mean that the respondent, having been vaccinated, has educated the network on vaccine benefits.
Results also indicate differences in social network characteristics based on vaccine adoption. Although vaccine adoption is not easily known, people’s perceptions of others’ vaccine adoption within their social network come into effect and we can infer that the HPV vaccine is being discussed in the respondent’s social network. HPV vaccine adopters largely perceived those in their network to have also been vaccinated while nonadopters perceived less of their network to have been vaccinated against HPV.
Vaccine adopters also had a less dense, more open network than that of nonadopters. High local density suggests less support for “new” ideas and enhanced health due to less diffusion of information from sources outside of the network [7,11]. Denser networks make it less likely that individuals will be exposed to new resources or ideas and will then be less likely to be vaccinated [12]. Vaccine adopters also reported a more homophilous network than nonadopters. Dyadic similarities between individuals create correlated outcome patterns. In this case, perceived HPV vaccination adoption status among social network members.
Social network factors predicted vaccination adoption. This is in line with the framework that uses social relations and networks as influences on health outcomes [5,13]. Social networks influence health behaviours through social support, social influence, social engagement and attachment, and access to resources [14]. An individual’s health and health behaviours can be predicted by the larger social context in which the individual is embedded.
However, some limitations should be noted. This cross-sectional survey sampled young adult students at one university. As with any survey, results are from self-reported information. Future research should focus on identifying additional social network factors that may influence vaccine adoption, such as healthcare access and health insurance status. Understanding social network factors that impact vaccine adoption is critical, as vaccine decisions are rarely made without consultation with others in the individual’s social network.
Despite these limitations, results support previous research that finds individual’s social networks serve as trusted information sources when it comes to vaccination [15]. A young adult’s social network and their position within the network have shown to be contextual predictors of well-being [5,13,16,17]. Efforts to increase vaccination rates could benefit from a better understanding of the social aspects involved in vaccine decision-making so that public health officials can focus on programs and information to target individuals for better health outcomes.
- Prevention CfDCa (2009) Adult Vaccination Coverage: The National Health Interview Survey (NHIS). Avaliable from: http://www.cdc.gov/vaccines/stats-surv/nhis/2009-nhis.html
- Prevention CfDCa. Human Papillomavirus. Avaliable from: http://www.cdc.gov/vaccines/pubs/pinkbook/downloads/hpv.pdf
- Allen JD, Mohllajee AP, Shelton RC, Othus MKD, Fontenot HB, et al. (2009) Stage of adoption of the human papillomavirus vaccine among college women. Prev Med 48: 420-425. [Crossref]
- Cohen EL, Head KJ (2013) Identifying knowlede-attitude-practice gaps to enhance HPV vaccine diffusion. J Health Commun 18: 1221-1234. [Crossref]
- Valente TW (2010) Social Networks and Health. Oxford University Press, Oxford.
- Wellman B, Berkowitz SD (1988) Social structures: A network approach. Cambridge University Press, New York.
- Hall A, Wellman B (1985) Social networks and social support. Academic Press. San Diego, CA. pp: 23-41.
- Golub B, Jackson MO (2012) How homophily affects the speed of learning and best-response dynamics. Quarterly J Econom: 127.
- Barnett GA, Hamliln DM, Danowski JA (1981) The Use of Fractional Scales in Communication Audits. Communication Yearbook 5. New Brunswick, NJ: Transaction. pp: 455-471.
- Caskey R, Lindau ST, Alexander GC (2009) Knowledge and early adoption of the HPV vaccine among girls and young women: Results from a national survey. J Adolesc Health 45: 453-562. [Crossref]
- Rogers EM, Kincaid DL (1981) Communication Networks: Toward a New Paradigm for Research. Free Press. New York.
- Valente TW (1996) Social network thresholds in the diffusion of innovations. Social Networks 18: 69-89.
- Valente TW, Hoffman BR, Ritt-Olson A, Lichtman K, Johnson CA (2003) The effects of social-network method of group assignment strategies on peer-led tobacco prevention programs in schools. Am J Public Health 93: 1837-1843.
- Berkman LF, Glass T (2000) Social integration, social networks, social support, and health. Social Epidemiol 1: 137-173.
- Brunson EK (2013) The impact of social networks on parents' vaccination decisions. Pediatrics 131: e1397-e1404. [Crossref]
- Helliwell JF (2006) Well-being, social capital, and public policy: What's new? The Econom J 116: C34-C45.
- Kawachi I (2010) Social capital and health. Handbook of Medical Sociology. (6th edn), Vanderbilt University Press. Nashville, TN. pp: 18-32.

