Abstract
For two reasons, communication is one of the major tools in the fight against any Ebola epidemics, with early case detection. Firstly, because Ebola is one of the most easily preventable of all infectious diseases and the thorough application of health- protection measures by the community of the sick persons is the best tool to fight any Ebola epidemic. Secondly, because during the two dozens of known Ebola epidemics health care workers have often met with people’s skepticism, or even hostility.
However, our review of Ebola communication, as outlined by WHO since 2013, shows that it has been marked by a series of errors, as well from a strategic perspective as in its concrete deployment. The same communication messages and tools have been used in non-epidemic and epidemic countries. A general ban on hunting has been promoted, while only 2% of sub-Saharan Africans live in areas inhabited by the bats that are the reservoir of the Ebola virus and while it is not proven that hunting is a major risk of infection. Erroneous or inappropriate messages have contributed to doubts and created anxiety.
To be effective, Ebola communication should be based on education about the disease, meaning explanation of its cause, its transmission and its prevention. We propose a communication strategy based on the notion of “microbe” as the causes of many diseases and on the fact that microbe transmission can often be prevented.
Introduction
An Ebola virus disease (EVD) epidemic begins with the spillover of the virus from a bat to an index human case, followed by human to human transmission, through contact with body fluids form a sick or a diseased person. In an ideal world, where early detection of EVD cases would be combined with a total respect of prevention measures, any EVD outbreak would stop after a few cases. In real world, during all the EVD epidemics communities have mistrust or rejected the prevention recommendations. In Liberia, Guinea, and Sierra Leone, abundant rumors and misunderstandings have hampered medical intervention, caused affected individuals to hide from medical staff, and have even resulted in the murder of healthcare workers. Unfortunately, it appears as though some aspects of the communication around Ebola from governmental and international organizations in these and other African countries have contributed to the spread of misinformation.
Misleading bushmeat messages
In March 2015, with Dr Atiyihwè Awesso, from the University of Lomé, we conducted an anthropological study on the perceptions of Ebola and the communication messages in Togo, a country free from Ebola [1]. We conducted 52 focus groups, 75 one-on-one interviews, and observed at-risk behaviors, in various locations all over the country. As far as we know, this is the only large study of Ebola perceptions in an Ebola-free country, and the only study to evaluate Ebola-related communication. Widespread knowledge of the Ebola hotline number (111) demonstrated that the messages disseminated by national media, posters, and local radio, have reached a large part of the population. This makes the nature of these messages all the more important.
The first lesson from our study was that the most remembered Ebola-prevention message was ‘avoid eating bushmeat’, which was emphasized as equally or even more important than washing one's hands or avoiding contact with people sick with Ebola. Studies conducted in other countries ranked the bushmeat message, which has been widely promoted all over Africa, as among the most well-known [2].
In a WHO Ebola Strategy document published in August 2014, ‘wild animal-to-human transmission’ is listed first among the information to be ‘used at the community level’, before ‘human-to-human transmission’ [3]. This document was designed to serve as the basis for all African Ebola communication programs. The WHO experts recommended that people ‘wear gloves and other appropriate protective clothing when handling wild animals’. In countries where hunters often go bare-footed and whose languages do not have a word for ‘glove’, these recommendations were translated into a prohibition on hunting and eating bushmeat. Anybody who traveled to Africa during in these years saw posters or eared radio messages instructing to avoid bush meat.
For example, an Ebola information picture book published by the Ivory Coast government, with the support of WHO, UNICEF, and the United Nations Operation in Côte d'Ivoire (UNOCI), and available on the UNICEF web site, contains four images demonstrating zoonotic transmission (from bats, monkeys, antelopes, and agoutis), versus only three for intra-human routes [4]. A UNICEF poster, also distributed by the Centers for Disease Control and Prevention (CDC), lists six ‘do nots’, including three relating to wild animals [5]. A Guinean Ebola picture book published by USAID, the Guinean Ministry of Health, and the NGO Plan, dedicates as much space to animal transmission as to human transmission (adding pigs, rodents and rabbits to the previous list) [6].
That have no scientific basis
These bushmeat messages had no scientific ground. In the chapter ‘What should be done once the epidemic is confirmed?’ the already-mentioned OMS strategy document places ‘wild animal-to-human transmission’ as the first risk requiring explanation at the ‘community level’ and lists ‘hunter’ as first among the ‘high-risk occupations’, before ‘health care workers, nursing staff’, while the EBV risk is 21 to 32 higher for health care workers than for the general population [7]. Even though the onset of an Ebola outbreak is due to viral transmission from an animal to a human, this form of transmission does not play any further role in the continuing spread of the epidemic, as the virus is then exclusively transmitted from person to person [8]. Therefore, messages about wildlife transmission not only have no utility during an epidemic but they distract from the vital messages, i.e. those that aim to prevent inter-human transmission.
What about the prevention of an epidemic in Ebola-free countries ? Firstly, let’s examine the case for mammals other then bats. As far as wild animals go, the Ebola virus has only been detected in gorillas, chimpanzees, and duikers [9]. The human index cases from several Congo and DRC outbreaks had been infected by one of these species [10]. Yet these infected animals were always dead when found by villagers [11]. Only half-a-dozen African countries have significant numbers of chimpanzees or small populations of gorillas. Therefore, in terms of non-flying mammals, bushmeat messages should only be used in a handful of countries and should not mention hunting, but scavenging. They could read, for example: ‘do not eat or touch any dead gorillas, chimpanzees, or duikers, that you might find...ʼ.
The suspected Ebola virus reservoir consists of several different bat species who inhabit an area spanning 22 Central and West African countries, populated by 22 million people (Figure 1) [12]. Over the last 14 years, one outbreak per year has occurred, indicating that the chance of contracting Ebola in the at-risk area is one out of 22 million, per year. For comparison, the estimated risk of contracting HIV from a blood transfusion in an industrialized country is more than ten times higher (about 1 in 2 million in the USA, 1 in 2.35 million in France) [13].
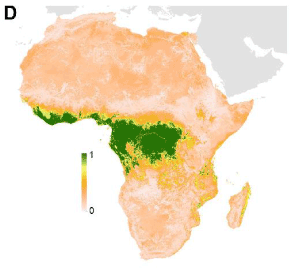
Figure 1. Predicted geographic distribution of reservoir bats.
Of course, for Ebola the infection of one index case subsequently causes an outbreak. However this doesn’t change the risk level for one individual. Large fruit bats are considered game in Africa and are heavily hunted in some regions, yet the route of Ebola transmission from bats to man has not been clearly established. Even though some outbreaks have been traced to the handling of hunted bats [14], alternative evidence points to other transmission routes. A serological survey in Gabon showed no association between hunting and Ebola infection and suggested ʻfruit contaminated by bat salivaʼ as a potential source of human exposure [15]. According to a study, the index case of the epidemic in West Africa occurred in December 2013 when a two-year-old boy played in a hollow tree housing a bat colony [16].
Firstly, people living outside the at-risk-area inhabited by the reservoir bats are not exposed to any risk and there is no ground to prohibit them from hunting bats. This concerns all the countries outside the 22 where those bats live and 96.6% of the 639 millions habitants of those 22 countries [17]. For example, there is no reason to ban any kind of hunting in Senegal, Mali, Burkina Faso, or Niger.
Secondly, given that the individual risk level of contracting Ebola from bats is 1 in 22 million per year (22 million people live in the infected bats area and there is in average one spillover per year), and that hunting only represents one exposure pathway, what is the real risk level from bat hunting? In comparison, the risk to get infected by HIV through blood transfusion is 1 in 2 million transfusions in the US, 1 in 2.35 million in France [18]. Even in the 22 countries where the reservoir bats are found, does this risk level, to which only part of their population is exposed, justify depriving hundreds of millions of people an important food source, which accounts for between 20% to 90% of the animal protein eaten in many regions? [19]. People living in the Congo River basin eat 4.9 million of tons of bush meat per year, around two thirds of the annual bovine production of the European Union [20].
And that are not followed
Our anthropological study showed that even though people knew that hunting was inadvisable or prohibited, they continued to hunt almost as usual. Although tallying hunting episodes was not a primary focus of this study, three out of our six investigator teams noticed bushmeat selling or encountered groups of hunters. During face-to-face interviews, the deputy head of a hospital said that ‘people have doubts about the disease and, despite awareness campaigns some people continue to eat bushmeatʼ. During different focus groups people stated that they felt the only reason to prohibit hunting was to protect wildlife, even adding on some occasions that Ebola was invented to prohibit hunting. During a filming of an awareness-raising video in the village of Barkouassi (central Togo) in July 2015, a man insisted on being filmed stating that he continued to hunt, and was not the only one... Press reports indicate that the practice of hunting and selling bushmeat still continues in various countries whether they are affected by Ebola or not, and papers have published pictures of hunters proudly handling game [21]. What kinds of impressions will people form when they hunt, butcher, and eat bushmeat, pigs, agoutis, or rabbits, and don't get Ebola? Wilkinson and Leach pointed out that ‘the inaccurate sensitization, which jarred with people's experiences, met with suspicion’ [22].
Changing people’s behavior in order to avoid exposure to the virus is the first weapon in the fight against an Ebola epidemic. Avoiding any contact with the persons sick or dead from Ebola is sufficient to avoid infection. However, during the West African and previous epidemics these prevention messages have systematically been met with skepticism. Many families have hidden their sick or dead members. Two years after the beginning of the epidemic, some families continued to practice unsafe burials in Guinea [23]. In light of these continuing difficulties, does it make sense to continue promoting, in both epidemic and pre-epidemic countries, bushmeat messages that have no efficacy and are not believed? This can only contribute to increasing doubts about all Ebola communications and opening the door to a host of misconceptions. As is frequently observed when dealing with public health, suspicion can lead to distrust, and distrust can turn to hostility [24].
Inaccurate prevention recommendations
The widely-used UNICEF previously mentioned poster lists five ‘dos’ to protect ‘yourself, your family, your community’, including ‘cook your food properly’. Another UNICEF poster recommends ‘avoiding undercooked food and bushmeat’ [25]. The aforementioned USAID picture book shows women sweeping their courtyard and disposing of trash into dustbins with the following recommendations: ‘Clean drinking water sources (wells, drillings, pumps), clean and sweep toilets, collect and place garbage in dustbins, bury or burn garbage’. Another page states ‘Clean out pits to avoid stagnant water’. In actual fact, these practices have nothing to do with Ebola prevention and dilute, once again, any factually correct messages, those that can actually prevent human-to-human transmission. Whether the messages related to either transmission (do nots) or prevention (dos), misinformation can only augment levels of suspicion, since no rational explanation can be given to support such unfounded messages.
In addition to incorrect information, negative messages are also being disseminated. The USAID picture book encourages communities to report any newcomers to the authorities. The WHO, UNICEF and ONUCI picture book includes a series of images showing a man denouncing a hunter to the police, with the caption ‘I should report all preventive measure violations to the authorities’ (Figure 2). Even though both health workers and anthropologists have documented that stigmatization and coercion undermine efforts to control the disease, these books encourage a repressive management of the epidemic.

Figure 2. Example of advice on Ebola from a WHO/UNICEF/ONUCI picture book [26].
Contributing to anxiety
Another major failure in Ebola communication strategies is that there is no clear discrimination between areas or countries where people are at immediate risk of infection and those areas in which no Ebola cases have been recorded.
In ‘pre-epidemic countries’, WHO recommends the dissemination of ‘standard case definition (…) for community-based surveillance [26]’. The definition includes ‘Illness with onset of fever (...) OR at least one of the following signs: bleeding, bloody diarrhoea, bleeding into urine, OR any sudden death’. Strangely enough, this definition is much wider than the one for “routine surveillance” by health workers, which replaces “OR” by “AND”. Following these guidelines, posters and radio spots detailing so-called Ebola symptoms have been broadcast throughout sub-Saharan Africa. According to the available data, no Ebola case was reported thanks to these messages in Western Africa, outside Guinea, Sierra Leone, and Liberia. In Mali, the index case was a little girl who had traveled for two days from Guinea while displaying symptoms. She was admitted to hospital after her grandmother had already consulted with two traditional healers. In Senegal, the patient was diagnosed thirteen days after hospitalization, and in Nigeria, the first patient collapsed on arrival at an airport [27].
While the use of these types of posters and radio spots is justified in areas where an outbreak is on-going, in other non-affected areas and countries it only contributes to raising anxiety levels, with doubtful utility. Our study in Togo emphasized the strong undercurrents of fear and uncertainty about the reality of Ebola. During the above-mentioned filming, in the town of Langabou, in central Togo, a nurse related to us how a group of people visiting his dispensary vehemently told him that ʻEbola is in the community but the government prohibits him to tell themʼ. Communities are simultaneously being told how to identify Ebola symptoms, but are also informed that the country is free from infection, resulting in mixed – and confusing – messages.
In addition, asking the community to identify infected cases has resulted in numerous community misdiagnoses. In Burkina Faso, for example, even though no actual cases of Ebola have been confirmed, general anxiety and panic is rife among the population [28]. In Togo, we heard of two sick people with an unknown disease who were left untreated and died, due to Ebola fears. Of course it has been necessary to widely communicate Ebola information across Africa. But in Ebola-free countries this should only take the form of providing information and should stop short of asking people to change their behavior. It should provide information about the causes of Ebola (a microbe) and methods to prevent infection, while clearly stating that Ebola is not present in the country. Describing the symptoms and asking people to identify cases must be limited to epidemic areas. Otherwise, these messages produce no benefits, generate anxiety and initiate negative attitudes.
A member of an African Ebola committee told us that scaring people is a way to make them follow the recommendations, expressing what might be a common belief among communication specialists, not only those from Africa. For example, the head of the French government’s information office stated that the first step during crisis communication was to ʻmaximize the crisisʼ in order to ‘generate room to maneuver;, in other words to scare people to make them obedient [29]. This communication strategy was applied during the massive 2009 French influenza vaccination campaign ... which was a total failure [30]. The recent Ebola crisis again demonstrates the inverse is true, communication should always strive to alleviate fear, not increase it.
Promoting unjustified behavior changes
Relatedly, another error in Ebola communication was requesting people change their behaviors when Ebola was not a direct threat. The WHO recommends that pre-Ebola countries ‘promote and strengthen standard infection prevention and control practices within the community; e.g. hand washing, food safety, etc’ [31]. Consequently, washing hands, avoiding crowds, not shaking hands, etc. (of course along with avoiding bushmeat) have been widely promoted in non-affected countries.
Our study in Togo indicates that even though during the fall of 2014 people followed these recommendations, practices have subsequently significantly waned. Here again, questions are raised about the credibility of these Ebola communications. As for hand washing, which is beneficial against various diseases, linking this practice solely to Ebola outbreaks does not encourage people to continue these habits on a permanent basis. Hand washing would be promoted more efficiently as a protection against various infectious diseases, including Ebola.
Conclusion and proposals
When reviewing Ebola communication tools, one of the most striking aspects were that they listed ʻdosʼ and ʻdo notsʼ but never mentioned the ʻwhysʼ. As such, communication messages recommended and ordered certain actions, without explaining the motivation for doing so. The goal of Ebola public health communication should be to improve health literacy. This would involve a complete reworking of the global Ebola communication strategy, replacing the top-down message delivery system with a strategy that emphasizes awareness-raising and education. Throughout every Ebola epidemic, the emergence of such a profusion of confused ideas relating to Ebola underlines the lack of general knowledge on infectious diseases. In addition to preparing for Ebola outbreaks, raising levels of infectious disease knowledge would foster greater adherence to major public health programs, such as vaccination or the use of mosquito nets. Disseminating knowledge about infectious diseases and their prevention would clarify the reasons supporting hand washing recommendations, which should not only be associated with Ebola prevention. Even often illiterate African people can understand both that Ebola is caused by a microbe and the routes this microbe uses to pass from one person to another.
We therefore propose the following:
- That the bushmeat messages be abandoned. In countries inhabited by these species, people should only be told not to touch dead chimpanzees and gorillas.
- That communication should be clearly different in pre-epidemic and epidemic countries.
- That in a pre-epidemic state, communication programs educate about Ebola and infectious diseases and should be centered on the notion of microbe and microbe transmission prevention, without promoting unjustified behavioral change or encouraging community-based Ebola disease identification.
- That in epidemic areas communication not only includes recommendations and orders, but also explains the causes of Ebola, the way the Ebola virus is transmitted, and refrains from denouncing certain behaviors or individuals.
Of course, rumors, incorrect ideas, and adverse reactions have many cultural, political, and social causes, and communication alone will never be sufficient to erase them all [32]. However, one would hope that we can design communication tools that do not fuel them.
References
- Seytre B, Awesso A, Gnassingbé A (2015) ‘L’anthropologie au service d’une stratégie de sensibilisation, d’éducation et de communication au Togo’, EBODAKAR 2015, 19-21 May 2015. This study was supported by a grant from the Togolese government.
- Omidian P, Tehoungue K, Monger J (2014) Medical Anthropology Study of the Ebola Virus Disease (EVD) Outbreak in Liberia/West Africa, WHO.
- Ebola Strategy (2014) Ebola and Marburg virus disease epidemics: preparedness, alert, control, and evaluation' (WHO) p. 40.
- Boite a images (2015) Prévention de la maladie à virus Ebola. Ivory Coast government.
- Ebola (Ebola Virus Disease) (2015) Centres for disease control and prevention, CDC.
- WHO (2015) Health worker Ebola infections in Guinea, Liberia and Sierra Leone. Ebola Strategy pp. 39-40.
- WHO (2015) Ebola virus disease.
- Pigott DM, Golding N, Mylne A, Huang Z, Henry AJ, et al. (2014) Mapping the zoonotic niche of Ebola virus disease in Africa. eLife 3: e04395.
2021 Copyright OAT. All rights reserv
- Judson SD, Fischer R, Judson A, Munster VJ (2016) Ecological Contexts of Index Cases and Spillover Events of Different Ebolaviruses. PLoS, Pathog 12: e1005780.
- Leroy EM, Rouquet P, Formenty P, Souquière S, Kilbourne A, et al. (2004) Multiple Ebola virus transmission events and rapid decline of Central African wildlife. Science 303: 387-390.
- Osterholm MT, Moore KA, Kelley NS, Brosseau LM, Wong G, et al. (2014) Mapping the zoonotic niche of Ebola virus disease in Afric. MBio 2: e00137-15.
- NIH (2012) What are the risks of a blood transfusion? National health lung and blood institute.
- EFS (2015) Surveillance épidémiologique des donneurs de sang', Invs.
- Leroy EM, Epelboin A, Mondonge V, Pourrut X, Gonzalez JP, (2009). Transmission of Ebola Viruses: What We Know and What We Do Not Know. mBio 8: 1-2.
- Becquart P, Wauquier N, Mahlakoiv T, Nkoghe D, Padilla C, et al. (2010) High prevalence of both humoraland cellular immunity to Zaire ebolavirus among rural populations in Gabon. PLoS ONE 5: e9126.
- Saéz am, Weiss S, Nowak K, Lapeyre V, Zimmermann F, et al. (2014) Investing the zoonotic origin of the West African Ebola epidemic. EMBO Molecular Medicine.
- West Africa Trends (2014) Bushmeat and the future of Protein in West Africa, African Center for Economic Transformation.
- Cooney D (2016) Ebola et la viande de brousse en Afrique.
- Fa JE, Peres CA, Meeuwig J (2002) Bushmeat Exploitation in Tropical Forests: An Intercontinental Comparison. Conservation Biology 16: 232-237.
- IRIN (2015) Bushmeat trade roaring again despite Ebola ban.
- Haby Niakate (2014) Ebola: viande de brousse, le goût du risqué. Jeune Afrique 30: 90.
- Annie Wilkinson, Melissa Leach (2015) Ebola–Myths, realities, and structural violence. African Affairs 454: 136–148.
- MVE (2015) de l’épidémie de maladie à virus Ebola. en Guinée published by Pr René Migliani.
- Bernard Seytre (2011) Vacciner, c’est convaincre. CAIRN pp. 89 – 104.
- UNICEF (2014) Five ways UNICEF is fighting Ebola. UNICEF connects.
- WHO (2015) Mali case, Ebola imported from Guinea. Ebola situation assessment, WHO.
- Badji D, Gautier AN, Khoudia NK, Desclaux A (2015) Premier cas d'Ebola à Dakar: les effets socioprofessionnels d'une mise en surveillance communautaire à domicile', EBODAKAR 19-21.
- Mark M (2015) First case of ebola reported in Africa’s most populous city Lagos. theguardian.
- Bila B, Gouo A (2015) La menace Ebola au Burkina Faso entre rumeurs et riposte nationale', EBODAKAR pp. 19-21.
- Lagarde MJC, Door MJP (2010) Une campagne de vaccination aux résultats décevants comme dans la plupart des autres pays. Les commissions d'enquête p. 7-155.
- Don Nutbeam (2000) Health literacy as a public health goal: a challenge for contemporary health education and communication strategies into the 21st century. Health Promotion International 15: 259-267.
- Chandler C, Fairhead J, Kelly A, Leach M, Martineau F, et al. (2015) Ebola: limitations of correcting misinformation. The Lancet 385: 1275–1277.


