Background: Hypotension is one of the most common problems in the postoperative term after coronary artery bypass graft surgery. There is a link between catecholamines (dopamine, epinephrine, and norepinephrine) and blood pressure. Catecholamines were metabolized by renalase, which is primarily synthesized by kidneys. Therefore, purpose of this study was to find out whether there was a relationship between renalase amount and hypotension developed in the postoperative term by measuring renalase amounts and catecholamine levels of healthy and volunteered patients with normal tension and with patients who underwent coronary artery bypass graft surgery.
Method: Participants were 19 postoperative term patients who underwent coronary artery bypass graft showing hypotension (systolic lower than 90 mmHg), 22 patients who underwent coronary artery bypass graft surgery showing normal tension and 23 normotensive subjects. Patients who developed hypotension were treated with dopamine (2.5-15 µg/kg/min.) infusion. Patients’ blood samples were taken in the 6-8th, 24th, 48th and 72nd hours of the postoperative term. Catecholamine and renalase levels were determined by using ELISA.
Result: Low Catecholamine and high renalase levels were detected in the comparison of patients who developed hypotension in the 6-8th hours of the postoperative term as compared with patients who did not develop hypotension after coronary artery bypass graft surgery and healthy subjects. Blood pressure and catecholamines increased while renalase decreased after treatment.
Conclusion: The high renalase would show lower levels of catecholamines and blood pressure (hypotension) compared to the controls after coronary artery bypass graft surgery. So that measurement of renalase may have practical utility for the monitoring of catecholamines in order to better control dopamine infusion amount and hypotension and also may give an idea to the operators about whether hypotension develops in the postoperative term or not.
catecholamines, coronary artery bypass graft surgery, hypotension, renalase
Hypotension, or decreased blood pressure, is a common complication seen during and after open heart surgery [1,2]. After open heart surgery, possible reasons that can cause low blood pressure include, hypovolemia (intravasal, venous pooling, active bleeding), wrong modulation of the transport respirator, reduction of catecholamines, bolus of sedation, coughing, light sedation low cardiac output due to new ischemia or rhythm disturbances, loss of pacer stimulation, septicemia, faulty brain signals, medications and endocrinal problems [3]. Also, Reichert et al. reported that cardiac tamponade was responsible for 10% of all cases of persistent hypotension after cardiac surgery [3]. However, the other mechanism for causing hypotension after cardiac surgery is not entirely known. Decrease in blood pressure (hypotension) causes a decrease of blood flow to the kidneys [1]. Low kidney blood flow is a cause of acute renal failure and is one of the most common causes of kidney failure after open heart surgery [4]. One of the most commonly used drugs to control hypotension is dopamine [5,6,7], which is controlled by renalase [8].
Renalase (RNLS), FAD-dependent amine oxidase is an enzyme that in humans was first time identified by Xu in 2005[8]. RNLS gene encoded this enzyme is a flavin adenine dinucleotide-dependent amine oxidase that is secreted into the blood from mainly the kidney [7] as well as small amount of other biological tissues such as oocytes, granulosa, interstitial and luteal cells of ovary, spermatogenic cells of testis, cortex of adrenal gland, liver, skeletal muscle, the small intestine and heart [9,10,11]. This enzyme destroys catecholamines [epinephrine (catabolite, metanephrine), norepinephrine (catabolite, normetanephrine), dopamine (precursor of epinephrine and norepinephrine)] and mediates the regulation of blood pressure and cardiac function [8,11]. It has been also shown that renalase infusion in rats caused a decrease in cardiac contractility, blood pressure, heart rate, and prevented a compensatory increase in peripheral vascular tone [12]. Therefore, here it has been hypothesized that there might be link between renalase and catecholamines amounts in the postoperative term hypotension occured after coronary artery bypass graft surgery.
Based on the foregoing information, this clinical study aims to reveal how renalase and catecholamines are affected in randomly and prospectively selected cases who are administered dopamine for the treatment of blood pressure decreased within 6 to 8 hours after Coronary Artery By-Pass (CABG) surgery.
This retrospective/prospective study was started after the approval of the local ethics committee and the informed consents of the patients were obtained (meeting number: 14, issue no: 05 dated 10.26.2017). It registered 19 coronary artery bypass cases (13 males, 6 females) who developed hypotension (systolic lower than 90 mmHg) in the early postoperative period, 22 coronary artery bypass cases (14 males, 8 females) whose blood pressure was normal, and 23 healthy individuals (15 males, 7 females) who presented at the hospital for their routine annual checkup and were found to be healthy. All patients underwent the CABG operation through standard premedication, anesthesia, aortic cannulation. Patients who developed hypotension after coronary artery bypass operation were started dopamine at a dose of 2.5µg/kg/min) [13,14]. However, if initial doses failed to achieve adequate tension, the dose was increased up to 5-15µg/kg/min [15].
From coronary artery bypass cases, samples of 5 ml. were taken in the post-operative 6-8-hour period, as well as at 24th, 48th and 72nd postoperative hours and put into plain biochemistry tubes, and tubes containing 3 ml heparin (green-capped) to study catecholamines (dopamine, epinephrine, norepinephrine) for the routine monitoring of patients. The samples were centrifuged at 4000 rpm and the sera and plasma were stored at -80oC until the time of analysis as described earlier [16].
Catecholamines and renalase analysis
Serum renalase (cat no: 201-12-5371), dopamine (Cat no: 201-12-1302) and epinephrine (MN), (Cat no: 201-12-0980; SunRed Biological Technology Co. Ltd, Shanghai; China), and norepinephrine (OPH1F2001) and levels were established using the ELISA method, as instructed in the producer company’s catalogue. It was noted in the company’s catalogue that the kit’s renalase detection range was 3–700 ng/ml, intra-assay value was <10% and inter-assay value was <12%. Also, as stated by the kits’ producers, assay range was 8-2000 nmol/L for dopamine, and 0.3–60 ng/mL for epinephrine), and 18 pg/mL -1000 pg/mL for norepinephrine. As for intra- and inter-assay values of the kits as reported by the producers, intra-assay values were 10% for dopamine, 10% for norepinephrine and 12% for norepinephrine, while the inter-assay values were 12% for dopamine, 12% for metanephrine and 11% for norepinephrine.
Statistical analyses
SPSS 21.0 for Windows (SPSS Inc., Chicago, IL, USA) software was used in all statistical analyses. Data obtained in the study were expressed as mean±standard deviation. Values for which p<0.05 were considered statistically significant. Kruskal Wallis one-way variance analysis was employed in the comparison of parameters between groups. Dual comparisons between groups were conducted using Mann Whitney U test. The correlations between group parameters were examined with Spearman correlation test.
When the patients were compared in terms of number of grafts used (2.7±0.3), perfusion time (97.4±9.8 min.) and aortic cross clamp duration (56.9±4.9 min.), there was not any difference between the patients who did and did not develop hypotension. Mean hemodynamic parameters CABG patients with and without hypotension developed after CABG was seen in Table 1. Heart rate was significantly higher in patient whom developed hypotension after coronary artery bypass graft surgery. However, CVP (mmHg) and MPAP (mmHg) values were similar in groups (Table 1).
Table 1. Hemodynamic parameters CABG patients with and without hypotension developed after CABG
Parameters |
**Normal tension |
***Hypotension |
CVP (mmHg) |
8.1 ± 1.2 |
8.2 ± 1.4 |
MAP (mmHg) |
88 ± 6.9 |
76 ± 5.4 |
MPAP (mmHg) |
24 ± 1.8 |
22 ± 1.1 |
HR (time/min; beats per minute) |
79 ± 1.3 |
118 a ± 3.6 |
CVP, central venous pressure; MAP, mean arterial pressure; MPAP, mean pulmonary arterial pressure and HR, heart rate. ap < 0.05 compared with and without hypotension developed after coronary artery bypass grafting.
Table 2 shows that demographic and pre-operative laboratory measurements (except for creatinine) were similar in groups. However, as expected, diastolic and systolic blood pressure were lower in hypotension as compared with control subject’s values.
Table 2. Certain demographic and pre-operative laboratory variables of the patients before CABG and control
Parameters |
*Control
(n:23) |
**Normal tension
(n:22) |
***Hypotension
(n:19) |
Gender [n/n, (female/male)] |
13/10 |
8/14 |
6/13 |
Group Age (years) |
69 ± 11.8 |
74 ± 13.9 |
71 ± 18.1 |
Body mass index [kg/m2] |
27.6 ± 4.5 |
26.9 ± 6.9 |
28.1 ± 6.7 |
Systolic blood pressure [mmHg) |
118 ± 8.5 |
127 ± 8.1 |
85 a ± 3.4 |
Diastolic blood pressure [mmHg) |
86 ± 7.7 |
79 ± 2.4 |
56 a ± 3.1 |
Blood glucose (mg/dL) |
92 ± 6.8 |
104 ± 7.4 |
106 ± 6.2 |
Sodium [mEq/L, (mean ± SD)] |
142 ± 3.4 |
138 ± 2.4 |
141 ± 3.2 |
Potassium [mEq/L, (mean ± SD)] |
4.57 ± 0.2 |
4.71 ± 0.3 |
4.77 ± 0.4 |
Uric acid [mg/dL, (mean ± SD)] |
4.4 ± 1.3 |
4.6 ± 1.8 |
4.4 ± 1.3 |
Creatinine (mg/dL) |
0.6 ± 0.1 |
0.9 ± 0.1 |
1.1a ± 0.2 |
SD, standard deviation; *Healthy control; **Normal tension after coronary artery bypass grafting; ***Hypotension developed after coronary artery bypass grafting. ap < 0.05 compared with and without hypotension developed after coronary artery bypass grafting.
Certain time-depended post-operative laboratory variables in the coronary bypass patients who did and did not develop hypotension with and without dopamine treatment after coronary bypass surgery are presented in Table 3.
Table 3. Comparison of certain time-depended post-operative laboratory variables in the coronary bypass patients who did and did not develop hypotension with and without Dopamine treatment
Parameters |
** Normal tension |
*** Hypotension |
Times (hours) |
Times (hours) |
(6-8)th |
24th |
48th |
72nd |
(6-8)th |
24th |
48th |
72nd |
Systolic blood pressure (mmHg) |
114 |
122 |
117 |
128 |
88 a |
99 |
116 |
109 |
Diastolic blood pressure (mmHg) |
79 |
82 |
88 |
85 |
59 a |
67 |
76 |
82 |
Blood glucose (mg/dL) |
96 |
77 |
108 |
79 |
104 |
108 |
112 |
109 |
Sodium (mEq/L) |
142 |
138 |
139 |
142 |
131 |
142 |
141 |
139 |
Potassium (mEq/L) |
4.3 |
4.4 |
4.3 |
4.6 |
4.4 |
4.5 |
4.7 |
4.5 |
Uric acid (mg/dL) |
4.1 |
4.2 |
4.3 |
4.4 |
4.3 |
4.1 |
4.1 |
4.2 |
Creatinine (mg/dL) |
0.7 |
0.9 |
1.1 |
0.9 |
0.9 a |
1.1 |
1.1 |
0.9 |
**Normal tension after coronary artery bypass grafting without treatment dopamine; ***Hypotension developed after coronary artery bypass grafting and treated with dopamine; ap < 0.05 compared with and without hypotension developed after coronary artery bypass grafting.
Low catecholamine and high renalase levels were detected in the comparison of patients who developed hypotension in the 6-8th hours of the postoperative term as compared with patients who did not develop hypotension after coronary artery bypass graft surgery and healthy subjects. Blood pressure and catecholamines increased while renalase decreased after dopamine administered Figure 1A-D.
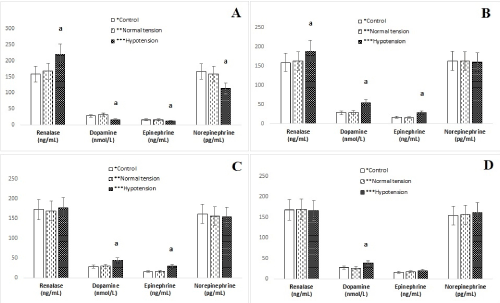
Figure 1. Comparison of renalase, dopamine, epinephrine and norepinephrine levels between the group who developed hypotension after coronary bypass surgery (A: within 6-8 hour; and B: 24 hours; C: 48 and D: 72 hours administered dopamine after hypotension developed), the group who did not develop hypertension (and did not receive any administration), and control group (was not subjected to any procedure). ap < 0.05 compared with and without hypotension developed after coronary artery bypass grafting.
After coronary artery bypass graft surgery seen low blood pressure can be life-threatening so that it must be treated on time [17,18]. Here we first-time report that the plasma concentration of renalase is markedly increased within first 6-8 hour in patients who developed hypotension after coronary artery bypass graft surgery as compared with patients who did not develop hypotension after coronary artery bypass graft surgery and healthy subjects. It was also found that plasma concentration of catecholamines were markedly decreased within first 6-8 hour in patients who developed hypotension after coronary artery bypass graft surgery as compared with patients who did not develop hypotension after coronary artery bypass graft surgery and healthy subjects. After dopamine administered [14,15] in patients who developed hypotension after coronary artery bypass graft surgery concentration of renalase is markedly decreased while concentration of catecholamines were increased in those patients. As mentioned before, renalase, a novel flavin adenine dinucleotide-dependent amine oxidase, is secreted into the blood by mainly kidney and metabolizes catecholamines in vitro (renalase metabolizes dopamine most efficiently, followed by epinephrine, and then norepinephrine) [10,11]. Here it was assumed that increased concentration of renalase (might be due to decreased blood flow to the kidneys) with 6-8 hours might cause hypotension after coronary artery bypass graft surgery. Because it has been previously shown that renalase infusion in rats caused a decrease in cardiac contractility, blood pressure, heart rate, and prevented a compensatory increase in peripheral vascular tone [12]. It was also previously reported that renalase administration to cases reduced plasma epinephrine levels by 82%, L-DOPA levels by 63%, and dopamine levels by 31%, and thus lowered blood pressure [19]. As circulating renalase levels decrease with dopamine administration, blood pressure is increased through increased catecholamine levels.
The data reported for the first time here let us think that if renalase blockers (monoamine oxidase inhibitors such as phenelzine, iproniazid, isocarboxazid, tranylcypromine, deprenyl, moclobemide, brofaromine) were given in addition to dopamine may prevent the destruction of catecholamines and mediate the elimination of hypotension [11] (or the opposite in case of hypertension) to manage persistent post-operative hypotension in the future.
Taken together, our results also suggest that renalase may play a critical role in cardiac function and systemic blood pressure and also provide a novel insight into understanding the function of renalase and hypotension seen after coronary artery bypass graft surgery. Also, measurement of renalase concentration in cases with low blood pressure resulting from decreased catecholamines after cardiopulmonary bypass might give an idea about catecholamine amounts.
This paper has been orally presented at the 14th International Update in Cardiology and Cardiovascular Surgery (UCCVS) Congress held at the Royal Seginus Convention Center in Antalya, Turkey on April 5-8, 2018.
There is no conflict of interest.
- Maheshwari A, McCormick PJ, Sessler DI, et al. (2017) Prolonged concurrent hypotension and low bispectral index ('double low') are associated with mortality, serious complications, and prolonged hospitalization after cardiac surgery. Br J Anaesth 119: 40-49. [Crossref]
- Hori D, Ono M, Rappold TE, Conte JV, Shah AS, et al. (2015) Hypotension After Cardiac Operations Based on Autoregulation Monitoring Leads to Brain Cellular Injury. Ann Thorac Surg 100: 487-493. [Crossref]
- Reichert CL, Visser CA, Koolen JJ, vd Brink RB, van Wezel HB, et al. (1992) Transesophageal echocardiography in hypotensive patients after cardiac operations: Comparison with hemodynamic parameters. J Thorac Cardiovasc Surg 104: 321-326. [Crossref]
- Bove T, Monaco F, Covello RD, Zangrillo A (2009) Acute renal failure and cardiac surgery. HSR Proc Intensive Care Cardiovasc Anesth 1: 13-21. [Crossref]
- MacCannell KL, McNay JL, Meyer MB, Goldberg LI (1966) Dopamine in the treatment of hypotension and shock. N Engl J Med 275: 1389-1398. [Crossref]
- Kalish BT (2017) Management of Neonatal Hypotension. Neonatal Netw 36: 40-47. [Crossref]
- Bhayat SI, Gowda HM, Eisenhut M (2016) Should dopamine be the first line inotrope in the treatment of neonatal hypotension? Review of the evidence. World J Clin Pediatr 5: 212-222. [Crossref]
- Xu J, Li G, Wang P, Velazquez H, Yao X, et al. (2005) Renalase is a novel, soluble monoamine oxidase that regulates cardiac function and blood pressure. J Clin Invest 115: 1275-1280. [Crossref]
2021 Copyright OAT. All rights reserv
- Zhou M, Liang T, Wang Y, Jin D, Wang J, et al. (2013) Expression and tissue localization of renalase, a novel soluble FAD-dependent protein, in reproductive/steroidogenic systems. Mol Biol Rep 40: 3987-3994. [Crossref]
- Xu J, Li G, Wang P, Velazquez H, Yao X, et al. (2005) Renalase is a novel, soluble monoamine oxidase that regulates cardiac function and blood pressure. J Clin Invest 115: 1275-1280. [Crossref]
- Aydin S, Aydin S (2017) Can Strict Control of Renalase Present a New Treatment Alternative in Regulating Blood Pressure? J Cardiovasc Med Cardiol 4: 008-009.
- Desir GV (2007) Renalase is a novel renal hormone that regulates cardiovascular function. J Am Soc Hypertens 1: 99-103. [Crossref]
- Karthik S, Lisbon A (2006) Low-dose dopamine in the intensive care unit. Semin Dial 19: 465-471. [Crossref]
- Joannidis M, Druml W, Forni LG, Groeneveld ABJ, Honore PM, et al. (2017) Prevention of acute kidney injury and protection of renal function in the intensive care unit: update 2017: Expert opinion of the Working Group on Prevention, AKI section, European Society of Intensive Care Medicine. Intensive Care Med 43: 730-749. [Crossref]
- Bayram M, De Luca L, Massie MB, Gheorghiade M (2005) Reassessment of dobutamine, dopamine, and milrinone in the management of acute heart failure syndromes. Am J Cardiol 96: 47G-58G. [Crossref]
- Aydin S (2015) A short history, principles, and types of ELISA, and our laboratory experience with peptide/protein analyses using ELISA. Peptides 72: 4-15. [Crossref]
- Lin CY, Weng ZC, Loh SH, Hong GJ, Tsai CS (2007) Coronary artery spasm after off-pump coronary artery bypass grafting. ANZ J Surg 77: 126-129. [Crossref]
- Flack JM, Nolasco C2, Levy P3 (2017) The Case for Low Blood Pressure Targets. Am J Hypertens 30: 3-7. [Crossref]
- Desir GV, Peixoto AJ (2014) Renalase in hypertension and kidney disease. Nephrol Dial Transplant 29: 22-28. [Crossref]

