Abstract
Objective:Many studies have extensively explored gait initiation (GI) among older population; however, there seems to be a need for further investigating the reliability of this method, particularly during obstacle crossing or dual tasking.
Aim:In this study we evaluated the reliability of the two-timing phases of GI, reaction phase (RP) and the anticipatory postural adjustment phase (APAP), regarding obstacle negotiation.
Method:11 healthy older adults participated in this study (mean ±SD age: 66.27± 3.58 year). The tests were performed in 4 conditions: a smooth walkway; a smooth walkway with concurrent cognitive task; an obstructed walkway; and an obstructed walkway with a concurrent cognitive task. In all 4 conditions the assessment was performed by the same rater in 2 sessions which were 15 minutes apart. Time in RP and APAP of GI were calculated from the center of pressure (COP) trajectory. Furthermore, intra class correlation coefficients (ICC) and standard errors of measurement (SEM) were calculated for all conditions.
Results:The RP showed excellent reliability in all conditions; single task condition on both smooth (ICC=0.81, SEM=0.04) and obstructed walkways (ICC=0.84, SEM=0.03), dual task condition on smooth (ICC=0.76, SEM=0.04) and obstructed (ICC=0.86, SEM=0.04) walkways. The APAP showed good to excellent reliability in related conditions; single task condition on the smooth (ICC=0.79, SEM=0.04) walkway and obstructed walkway (ICC=0.65, SEM=0.04) and when dual tasking on the smooth and obstructed walkways [(ICC=0.73, SEM=0.04) and (ICC=0.81, SEM=0.03), respectively.
Conclusions :We found good to excellent reliability for reaction and anticipatory postural adjustment phases. However, no clear pattern was found regarding to the effect of obstacle negotiation, or dual-tasking. This reliable method can be used as a tool of assessment in fall preventive rehabilitation programs, before and after training.
Key-words
Gait initiation; Reliability; Obstacle negotiation; Aging
Abbreviations
COP: Center of Pressure, RTP: Reaction time phase, APAPT: Anticipatory postural adjustment phase, GI: Gait initiation, COM: Center of mass
Introduction
Gait initiation (GI) is a voluntary destabilizing behavior that is a sensitive indicator of dynamic postural stability [1,2]. GI provides insight into postural control and biomechanical changes related to aging and identifies fall risk in older adults [2-5]. The central nervous system interacts with the environmental instability and prepares the individual for body movement with both compensatory and anticipatory postural adjustments (APAs). APAs are affected by aging; for example, posterior shifts of the center of pressure decreases with aging, leading to the forward and lateral acceleration of the center of mass (COM)toward the stance limb in order to enable the swing leg to raise [6-9]. Previous research has shown that the reduced posterior shift of COP is related to the risk of falling [2].
Study of the successful obstacle negotiation in older adults is very important as many falls in this population are caused by tripping over objects [10]. During obstacle negotiation, from the pre-crossing phase, foot placement requires more cognitive involvement compared to walking on an unobstructed walkway [10]. Dual-task paradigms are used to evaluate interactions between cognition, gait, and fall risk. Since GI requires higher cognitive resources compared to steady walking, it has been shown that the increased duration of APAs in GI while dual-tasking is associated with increased risk of falling in older adults [11,12]. Hence, the duration of APAs under dual-task conditions is specifically a sensitive indicator of dynamic balance efficiency in GI [1,13].
Generally, in order to consider a method as a valid and reliable one, its consistency and precision must be examined in repeated measures. Reliability methods are used to measure this precision and consistency related to repeatability of a variable. Few studies of reliability of GI have been undertaken [1,14] while the importance of the correlation between the length of APA in voluntary step execution and fall risk in older adults [10,15] rise the necessity of investigate the reliability of the reaction time and anticipatory postural adjustment phases of GI during obstacle negotiation in respect to dual tasking, as a cognitive overload, in older adults If found reliable, this assessment could be used before and after preventive interventions in clinical environments to evaluate interventions in healthy older adults. Therefore, the purpose of the present study was to determine test-retest reliability of quantitative measures of GI timing parameters during voluntary step initiation under different cognitive demands. Our hypothesis is high reliability of this method and therefore, it is an applicable method for future studies in fall risk studies. This study is reliability part of registered work in Iranian Registry of Clinical Trials (N= IRCT2017022513146N5).
Methodology
Participants
Eleven older adults, 10 females and 1male, aged 65-80 years, were recruited from a facility offering activities for older adults in Tehran (Table1). Inclusion criteria were as follows: age> 65 years old, being able to initiate gait and walk independently, living independently in the community, having the ability to understand an auditory cue to initiate gait, score >24 in Mini-Mental State Examination [16]. Potential participants were excluded if they had depression and anxiety according to Hospital Anxiety and Depression Scale (HADS) scores, neurological or musculoskeletal disorders or significant auditory or visual impairments [17,18]. All participants gave written informed consent form approved by the ethics committee at Tehran University of Medical Sciences (Grant number: IR.TUMS.REC.1396.2936).
Table 1. Participants Demographical Characteristics.
Variable |
Mean |
SD |
Range |
Height, cm |
161 |
6.0 |
151-175 |
Weight, kg |
66.2 |
3.5 |
56-93 |
Age, y |
70.8 |
8.5 |
65-74 |
Berg balance scale |
54.3 |
3.3 |
42-56 |
Body mass index, Kg/m2 |
26.2 |
3.3 |
20.7-32.9 |
HADS-D |
4.8 |
3.0 |
1-10 |
HADS-D: Hospital Anxiety and Depression Scale- depression Subscale; SD:Standard deviation
Procedure
Tests were performed in 4 conditions: GI on unobstructed walkway; GI on unobstructed walkway with a concurrent cognitive task; GI on obstructed walkway; and GI on obstructed walkway with a concurrent cognitive task. Test order was randomized. Before data collection, the participants performed only one trial for each condition to minimize learning.
All tests were assessed by the same rater in the same laboratory environment in 2 sessions 15 minutes apart. The participants initially stood upright on the force platform. The initial foot position was 10° abduction in both feet, with heels separated mediolaterally by about 6 cm, equidistant from the midline of the platform’s recording surface [10]. To ensure that position of the feet was identical in all conditions, we used an outline of each foot drawn on a sheet of paper. We installed them on the surface of force platform in all conditions. Participants were instructed to distribute their weight equally between their right and left legs [17].
Participants were instructed to look straight ahead at an eye level target, a black dot at the center of a white 2.5 cm radius circle on a red background. The target was at the cross point between the perpendicular line to the line between two eyes and the opposite wall [19]. Participants were instructed to look down at the floor and obstacle after the auditory cue. The auditory cue occurred 2000 ms after onset of the force plate recording. This time was used to calculate initial COP position identified as the mean amplitude in the 1500 ms period, prior to the onset of the auditory cue [10]. The participants initiated the gait with their self-selected leg immediately after auditory cue. We focused on first step to study gait initiation.
In the obstacle crossing condition, an obstacle was placed on the walkway and participants were instructed to step over the obstacle after the gait initiation step. The obstacle was white, and its dimension was 91.0 cm width × 2.4 cm height × 1.0 cm depth. We located the obstacle 1m from the initial position on the brown walkway. The reason for this placement was that in healthy older adults, the average for the first-step length during GI is 52.5 cm [20]; therefore, our participants were not able to step over the block on the first step and they initiated anticipatory motor planning for correct foot placement on the first step [10,21]. Therefore, if the obstacle was closer, anticipatory motor planning during GI would demand little attention because participants would know that they were able to cross the obstacle in the first step. The participants were requested to check the location of the obstacle before the trial and instructed to step over the obstacle.
In dual-task conditions, subjects were required to perform the GI task concurrently with a cognitive task with, and without, stepping over the obstacle. The cognitive task was the auditory reaction time task recorded in an audio editor program. The words red, yellow, and blue were recorded in random order over 200 ms each with 500 ms time interval consisting of an overall time of 1600 ms. This time is in accordance with the preferred walking speed of older adults (range of 66-84 years old) which is about 100 cm/s [22,23]. Therefore, in dual tasking, cognitive task time (1600 ms) cover about 1.6 m. Because the obstacle was located in 1m distance, definitely, obstacle crossing, and cognitive task are congruent. It has been shown that adults over 70 years old show significant reduction in usual gait speed compared to those between 40 and 59 years old [24]. Because of the 1m distance of obstacle from the initial position, the cognitive task time was calculated to ensure that in the dual-task conditions the cognitive task coincided with the obstacle crossing. Participants were asked to say “yes” every time they heard the word “red”. Their responses were recorded with a sound recorder. Audio editing software was used to calculate the interval between the appearance of the word 'red' and the initiation of the response. This interval was recorded as the cognitive reaction time.
Data Collection and statistics
COP data were obtained using a Bertec Columbus (Ohio, USA) force platform (90 × 90 x 15.2cm) with a sampling rate of 1000 Hz, sensitivity of 10µv/div, and low-pass filter at 3 Hz. The analysis of GI data extracted specific temporal events, using a program written in SPSS [10]. Timing of the following events was calculated from the COP trajectory. First, step initiation was defined as the first mediolateral deviation of the COP toward the swing leg [COP excursion >3 SD away from the initial COP position defined as the mean amplitude in the 1,500ms period prior to the onset of the auditory cue]. Secondly, foot-off was defined as the end of the mediolateral shift of the COP toward the stance leg (absolute COP slope <100 mm/s, 2 samples in a row) [1]. The reaction phase was calculated as the time between the cue and step initiation. The APA phase was calculated as the time from step initiation to foot-off (Figure 1).
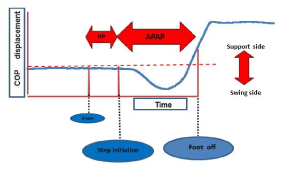
Figure 1. Mediolateral Center of pressure trajectory in gait initiation. The following timing events are marked in this figure: onset of the auditory cue (cue), the first mediolateral deviation of the center of pressure (COP) toward the swing side (step initiation), and the end of the mediolateral shift of the COP toward the stance leg (foot-off);RP: Reaction phase;APAP: Anticipatory postural adjustment phase.
A two-way random model (Model 2) of the intra class correlation coefficient was used to estimate the relative reliability. For each ICC, a 95% confidence interval (CI) was calculated. Paired t-tests on the difference of scores obtained at test and retest sessions were used to test for systematic bias [25]. ICC was from 0 to 1 and was interpreted as follows: 0.00–0.39 poor; 0.40–0.59 fair; 0.60–0.74 good; and 0.75–1.00 excellent [23]. The second root of mean square error (SEM), and 95% CI were calculated to provide an estimate of the absolute amount of error associated with the measurements in the same units as the measurement [26].
Results
Table 1 shows demographic characteristics of all participants in this study. Test and retest scores for the COP-derived GI measures in all conditions showed an absence of systematic bias (P>0.05, Table 2). The calculated ICC and SEM values are shown in Table 3. The COP-derived GI measures in older adults showed excellent reliability in reaction phase (ICC, 0.76 to 0.86) and good to excellent reliability in anticipatory adjustment phase (0.65 to 0.81). There was no trend related to the effect of obstacle negotiation, or dual tasking. ICC for RTP and APAP on the unobstructed walkway were 0.81 and 0.79, respectively. Also, in the second condition, on the unobstructed walkway with the concurrent cognitive task, ICC for RTP and APAP were 0.76 and 0.73, respectively. In obstacle crossing, ICC for RTP and APAP were 0.84 and 0.65, respectively and in the last condition, obstacle crossing when doing a cognitive task simultaneously, reliability scores for RTP and APAP were 0.86, 0.81, respectively.
Table 2. Descriptive Data for Test–retest COP Measures in Different Test Condition.
Variables |
Task |
With Obstacle |
Without Obstacle |
Mean, s |
P value |
Mean, s |
P value |
RP,s |
Single task |
0.14(-0.04,0.01) |
0.28 |
0.00(-0.04,0.02) |
0.53 |
RP,s |
Dual task |
0.00(-0.04,0.03) |
0.71 |
0.02(0.00,0.05) |
0.08 |
APAP,s |
Single task |
0.01(-0.02,0.04) |
0.45 |
0.02(-0.01,0.05) |
0.18 |
APAP,s |
Dual task |
-0.01(-0.04,0.01) |
0.22 |
0.01(-0.02,0.05) |
0.51 |
Values are mean (lower limit, upper limit),S refers to second, P refers to p-values of paired t-test on test–retest differences; COP: Center of pressure; RP: Reaction phase; APAP: Anticipatory postural adjustment phase.
Table 3. Test-retest Reliability Analysis of COP Measures for Single and Dual-task Conditions.
Condition |
Variable |
Obstacle Negotiation |
Without Obstacle Negotiation |
ICC(95% CI) |
SEM,s |
ICC (95% CI) |
SEM,s |
Single-task
|
RP, s |
0.84(0.54 ,0.95)
|
0.03 |
0.81(0.45 , 0.94) |
0.04 |
APAP, s |
0.65(0.13, 0.89)
|
0.04 |
0.79(0.41 , 0.93) |
0.04 |
Dual-task
|
RP, s |
0.86(0.57, 0.96) |
0.04 |
0.76(0.33, 0.93) |
0.04 |
APAP, s |
0.81(0.46, 0.94)
|
0.04
|
0.73(0.27 , 0.92) |
0.04 |
COP: Center of pressure; ICC: Intra class correlation coefficient; SEM: Standard error of measurement, RP: Reaction phase; APAP: Anticipatory postural adjustment phase, S: second
Discussion
This study showed the relative and absolute reliability of two-timing parameters derived from COP trajectory study in GI during obstacle crossing with a concurrent cognitive task in healthy older adults. We found excellent reliability in RTP and good to excellent reliability in APAP (our timing parameters of voluntary step execution) in all conditions. These values were similar during both dual tasking and obstacle negotiation without particular pattern in different conditions.
Our results confirmed Melzer’s report based on reported good to excellent reliability for similar parameters in voluntary step execution [1]. However, while they only considered single and dual tasking, we also considered obstacle negotiation in our conditions. The other difference was related to the schedule of trials in which they had 18 repetitions in three steps data collection (six trials in each data collection) while we used only one repetition before data collection in order to protect against the learning effect. It is possible that a well-learned postural challenge (obstacle crossing), its relevancy to daily activity with more automaticity, healthy status of our participants (decrease the aging effect) and less interferences with cognitive task, leaded to detecting similar values with only one repetition.
Halvarsson, et al. also reported good to excellent reliability in similar timing parameters during the voluntary step execution. They used two force plates in their method. Their definition for foot off, took into account the time points related to both lower limbs rather than only swing leg. This approach provides more generalizability to the real life in their method [27]; this might be the reason why the reliability scores were higher compared to Meltzer's. In our study, we had only one force plate to detect COP trajectory related to swing phase; nevertheless, our results were partially similar to results of Halvarsson, et al. [27]. Hartley, et al. [28], reported good to excellent reliability of these parameters in patient suffering from chronic ankle instability without considering dual tasking and learning effect reduction in method based on having 10 trial repetitions with one-week interval without concurrent cognitive task [28]. Our results are partially similar in single task conditions with less detrimental learning effect in healthy older adults. Based on previous studies [15], since most falls usually occur under attention demanding circumstances, it seems necessary to include a cognitive element in interventions programs for older adults (e.g. obstacle negotiation when doing a cognitive task). Step training programs have positive effect on obstacle negotiation improvements [29], and multi component exercise potentially prevent fall in older adults [30]. Therefore, we suggest using this reliable method before and after every dual tasking fall preventive intervention to measure its positive effects on RTP and APAP. The distinctive methodology for this outcome measures is that it may decrease the learning effect of repetition during assessments.
Reliability of APAP (good to excellent), was somehow lower than RTP (excellent). This might be due to the fact that our subjects were free to select either right or left leg to initiate walking. Based on previous studies, GI may share an asymmetrical feature of motor control [31], since the S1 period (first part of APA) is partially under supraspinal control. Some studies [32], have reported that the lateral displacement of the COP to the initial swing leg before the initiation of gait is larger with the left leg in response to an external cue and it is also larger than gait initiation with the leg that has been spontaneously chosen. Furthermore, the weight shift to the initial swing side during gait initiation is asymmetrical when the leg is chosen in response to an external cue [32]. We had no external cue, but participants were free to select either leg which as a result, it may have an impact on the COP trajectory and therefore the reliability scores.
This study had some limitations. We had no physician examination to confirm the health status of our participants and therefore relied on their perceptions [10,27,32]. Another limitation was the innovative nature of this study; there were no previous studies on the reliability of GI with obstacle crossing which made it impossible for data comparison during obstacle negotiation. The methodological strength of this study was, nevertheless, that the testing environment and the time of the day were the same. Also, current results are obtained with only one repetition before the main data collection to reduce or eliminate the learning effect.
2021 Copyright OAT. All rights reserv
Conclusion
We found good to excellent reliability for reaction phase and anticipatory postural adjustment phases, but, no clear pattern was found regarding to the effect of obstacle negotiation and dual-tasking. Thus, these reliable outcome measures have a good potential to be a useful tool for evaluating central nervous system and dynamic balance for both diagnostic purposes and fall preventive clinical interventions. Future research is necessary to investigate the validity of this method for fall risk estimation.
Conflict of Interest
None
Acknowledgement
This study was supported by biomechanics laboratory of rehabilitation faculty, Tehran University of Medical Sci
References
- Melzer I, Kurz I, Shahar D, Levi M, Oddsson L (2007) Application of the voluntary step execution test to identify elderly fallers. Age Ageing 36: 532-537. [Crossref]
- Hass CJ, Waddell DE, Wolf SL, Juncos JL, Gregor RJ (2008) Gait initiation in older adults with postural instability. Clin Biomech (Bristol, Avon) 23: 743-753. [Crossref]
- Stins JF, van Gelder LM, Oudenhoven LM, Beek PJ (2015) Biomechanical organization of gait initiation depends on the timing of affective processing. Gait Posture 41: 159-163. [Crossref]
- Novak AC, Deshpande N (2014) Effects of aging on whole body and segmental control while obstacle crossing under impaired sensory conditions. Hum Mov Sci 35: 121-130. [Crossref]
- Lee J, Webb G, Shortland AP, Edwards R, Wilce C, et al. (2018) Reliability and feasibility of gait initiation centre-of-pressure excursions using a Wii® Balance Board in older adults at risk of falling. Aging Clin Exp Res 1-7. [Crossref]
- Palluel E, Ceyte H, Olivier I, Nougier V (2008) Anticipatory postural adjustments associated with a forward leg raising in children: effects of age, segmental acceleration and sensory context. Clin Neurophysiol 119: 2546-54. [Crossref]
- Bleuse S, Cassim F, Blatt JL, Labyt E, Derambure P, et al. (2006) Effect of age on anticipatory postural adjustments in unilateral arm movement. Gait Posture 24: 203-210. [Crossref]
- Uemura K, Yamada M, Nagai K, Shinya M, Ichihashi N (2012) Effect of dual-tasking on the center of pressure trajectory at gait initiation in elderly fallers and non-fallers. Aging Clin Exp Res 24: 152-6. [Crossref]
- Shik ML, Orlovsky GN (1976) Neurophysiology of locomotor automatism. Physiol Rev 56: 465-501. [Crossref]
- Uemura K, Yamada M, Nagai K, Ichihashi N (2011) Older adults at high risk of falling need more time for anticipatory postural adjustment in the precrossing phase of obstacle negotiation. J Gerontol A Biol Sci Med Sci 66: 904-909. [Crossref]
- Yamada M, Aoyama T, Arai H, Nagai K, Tanaka B, et al. (2011) Dual-task walk is a reliable predictor of falls in robust elderly adults. J Am Geriatr Soc 59: 163-164. [Crossref]
- Graveson J, Bauermeister S, McKeown D, Bunce D (2016) Intraindividual Reaction Time Variability, Falls, and Gait in Old Age: A Systematic Review. J Gerontol B Psychol Sci Soc Sci 71: 857-864. [Crossref]
- Wei TS, Huang CJ, Chen SK, Wu WL (2011) Effect of age on attentional demands and postural control of obstacle crossing:Evidence from a dual-task approach. J Med Bioeng 1: 36-41.
- Lessmann V, Gottmann K, Malcangio M (2003) Neurotrophin secretion: current facts and future prospects. Prog Neurobiol 69: 341-374. [Crossref]
- Pichierri G, Coppe A, Lorenzetti S, Murer K, de Bruin ED (2012) The effect of a cognitive-motor intervention on voluntary step execution under single and dual task conditions in older adults: a randomized controlled pilot study. Clin Interv Aging 7: 175-184. [Crossref]
- Folstein MF, Folstein SE, McHugh PR (1975) "Mini-mental state". A practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res 12: 189-198. [Crossref]
- Khanmohammadi R, Talebian S, Hadian MR, Olyaei G, Bagheri H (2016) The relative and absolute reliability of center of pressure trajectory during gait initiation in older adults. Gait Posture 52: 194-201. [Crossref]
- Slijper H, Latash ML, Mordkoff JT (2002) Anticipatory postural adjustments under simple and choice reaction time conditions. Brain Res 924: 184-197. [Crossref]
- Aruin AS (2006) The effect of asymmetry of posture on anticipatory postural adjustments. Neurosci Lett 401: 150-153. [Crossref]
- Lu B, Pang PT, Woo NH (2005) The yin and yang of neurotrophin action. Nat Rev Neurosci 6: 603-614. [Crossref]
- Mbourou GA, Lajoie Y, Teasdale N (2003) Step length variability at gait initiation in elderly fallers and non-fallers, and young adults. Gerontology 49: 21-26. [Crossref]
- Smidt GL (1998) Gait and rehabilitation 68-71.
- Kimura K, Hozumi N (2012) Investigating the acute effect of an aerobic dance exercise program on neuro-cognitive function in the elderly. Psychol Sport Exerc 13: 623-629.
- Novaes RD, Miranda AS, Dourado VZ (2011) Usual gait speed assessment in middle-aged and elderly Brazilian subjects. Rev Bras Fisioter 15: 117-122. [Crossref]
- Moghadam M, Ashayeri H, Salavati M, Sarafzadeh J, Taghipoor KD, et al. (2011) Reliability of center of pressure measures of postural stability in healthy older adults:Effects of postural task difficulty and cognitive load. Gait Posture 33: 651-655. [Crossref]
- Atkinson G, Nevill AM (1998) Statistical methods for assessing measurement error (reliability) in variables relevant to sports medicine. Sports Med 26: 217-238. [Crossref]
- Halvarsson A, Franzén E, Olsson E, Ståhle A (2012) Relative and absolute reliability of the new "Step-Ex" step-execution test in elderly people with and without balance problems. Disabil Rehabil 34: 1986-1992. [Crossref]
- Hartley EM, Hoch MC, McKeon PO (2016) Reliability and responsiveness of gait initiation profiles in those with chronic ankle instability. Gait Posture 49: 86-89. [Crossref]
- Okubo Y, Schoene D, Lord SR (2016) Step training improves reaction time, gait and balance and reduces falls in older people: a systematic review and meta-analysis. Br J Sports Med 51: 586-593. [Crossref]
- Huang T, Larsen KT, Ried-Larsen M, Møller NC, Andersen LB (2014) The effects of physical activity and exercise on brain‐derived neurotrophic factor in healthy humans: A review. Scand J Med Sci Sports 24: 1-10. [Crossref]
- Crowe A, Schiereck P, de Boer RW, Keessen W (1993) Characterization of gait of young adult females by means of body centre of mass oscillations derived from ground reaction forces. IEEE Trans Biomed Eng 42: 293-303. [Crossref]
- Hiraoka K, Hatanaka R, Nikaido Y, Jono Y, Nomura Y, et al. (2014) Asymmetry of anticipatory postural adjustment during gait initiation. J Hum Kinet 42: 7-14. [Crossref]

