Abstract
Background: Compared to women’s health providers, primary care physicians are less likely to provide contraceptive counseling and are more likely to provide preventive counseling. We evaluated clinical visits with both preventive and contraceptive counseling, to identify the potential of integrated health services.
Methods: Procedure and diagnosis codes were used to identify annual or family planning visits of women aged 13-49. Five managed care plans identified providers with at least fifteen of these visits in 2013. We abstracted 1,054 visits and performed a multilevel logistic regression analysis, with clinic site as the level-2 random effect, controlling for age, visit reason, clinic specialty, and non-contraceptive service.
Results: In 134 visits, both contraceptive and preventive counseling occurred. Women were more likely to receive both types of counseling when they had family planning (OR=5.9, 95% CI=2.7-12.7) or reproductive health (OR=3.1, 95% CI=1.6-6.0) visit reasons; received non-contraceptive services (OR=2.6, 95% CI=1.3-5.3) or visited multispecialty clinics (OR=38, 95% CI=4.9-273.9) and less likely if women were referred for primary care services (OR=0.1, 95% CI=0.1-0.9).
Conclusion: Combined counseling occurs mainly in family planning visits and when preventive health is included in the visit rather than referred out. Clinicians at multispecialty sites are more likely to integrate contraceptive and preventive counseling than those at family planning or primary care clinics. Annual visits represent a valuable opportunity to provide both types of counseling.
Key words
family planning, contraception, prevention, counseling, health care delivery, managed care, primary care, quality of care
Introduction
The 2010 Affordable Care Act (ACA) elevated disease prevention as a national priority, requiring that health plans cover a variety of preventive screening and counseling services without co-payment [1,2]. According to ACA guidelines, preventive services comprise screening and counseling for obesity, substance use, sexually transmitted infections (STIs), and cervical cancer. Contraceptive counseling and service provision are also included under the umbrella of “preventive services” [3]. Yet, provision of preventive health and contraceptive counseling tend to occur in separate contexts.
Primary care physicians, including family medicine, internal medicine, and adolescent medicine clinicians, represent the first point of contact for persons with a wide range of health concerns, providing health promotion, disease prevention, and counseling services in a variety of settings. They often collaborate with other health professionals and obtain appropriate consultations or referrals [1,4]. Despite this broad definition, only a low percentage of primary care providers administer contraceptive counseling during clinical visits. Numerous barriers may result in this gap in care, including competing preventive and acute health needs in the primary care setting [5-7]. Providers have inadequate time to address patients’ numerous family planning needs, they may be unprepared for detailed conversations regarding contraceptive methods, or they may believe that these responsibilities belong to specialists [8-10].
For women of reproductive age, well-woman visits or annual check-ups may represent appropriate occasions to provide counseling on contraceptive options in conjunction with other preventive health behaviors. Furthermore, visits that address treatment of chronic diseases should include conversations about contraception as part of preconception care, because hormonal contraceptive methods may interact with drugs used to treat certain chronic conditions, and because taking teratogenic medications may require avoidance of pregnancy [11].
Clinical guidelines for family planning providers recommend incorporating preventive health care topics into preconception care [7]. During family planning visits, physicians should address aspects of general well-being, including management of mental health, weight, and chronic illnesses. Preconception health services include counseling on topics such as domestic violence, STI prevention, and effective usage of contraceptive methods [12,13]. A 2013 survey of publicly funded clinics found differences in the self-reported delivery of preconception care services by clinic type [12].
By integratingffairsion Disease Control and Preventionttingian/gynecologists are more likely to provide these ing impairments, older adults0or preventive and contraceptive services, providers can promote comprehensive, coordinated care and facilitate the improvement of maternal and infant health outcomes, focusing on individuals who have difficulty accessing care outside of family planning visits [8]. Women with medical conditions may not go to a family planning provider in addition to their specialist. However, the extent and context in which this integration occurs is not known.
As part of a larger medical record review assessing the quality of family planning services in primary care clinics, we identified characteristics of Medi-Cal (California’s Medicaid program) managed care visits that provided both contraceptive and preventive health counseling during the same encounter. Specifically, we wanted to determine whether visits offering both contraceptive and preventive health counseling differ by provider specialty or by the reason for the visit.
Methods
Patient involvement
Our research questions were designed in response to community members’ [14] concerns that women who enrolled in Medicaid due to the Affordable Care Act implementation receive sufficient family planning services and counseling when they interact with their primary care providers.
Clinic selection
Five Medi-Cal Managed Care plans participated in the study using sampling procedures designed to identify reproductive health visits in primary care clinics. With the plans’ medical directors, we identified outpatient primary care and OB/GYN clinics that were not enrolled in California’s Family Planning, Access, Care, and Treatment (Family PACT) program, as the quality of Family PACT providers had been assessed in the 2011 UCSF Family PACT evaluation [7,15].
Selection of visits
The study cohort consisted of all providers affiliated with one of the five plans and who served at least 15 female clients ages of 13 and 49 with a family planning service or annual/well-woman visit at outpatient office visits in 2013. Visits were identified using a list of CPT codes, ICD-9-CM diagnosis codes, and ICD-9-CM procedure codes.
Data collection
Medical directors from each plan sent letters introducing the study to eligible providers. Upon agreement to participate, providers were interviewed by telephone about main clinic characteristics and received client lists with visit dates of the first consecutive eligible women seen in 2013 for the abstraction.
Trained nurse abstractors collected data using iPads preloaded with survey questions that aimed to assess characteristics of clients and clinical visits. The custom iPad application used for the 2011 Family PACT MRR [7] was updated for the iPad 10.0 version. Completed surveys were transmitted to the UCSF Research Electronic Data Capture (RedCap) server. All data analyses were performed with SAS 9.4.
Outcome and predictor variables
The main outcome variable included visits where both contraceptive and prevention counseling were documented. Topics covered during contraceptive counseling included counseling on any reversible or permanent contraceptive methods, including natural family planning and emergency contraception. Prevention counseling topics included preconception care, folic acid use, STI and HIV prevention, cervical cytology, mammograms weight management, intimate partner violence, alcohol, tobacco, or substance use, and chronic disease management. A binary variable was created to highlight visits during which both prevention and contraceptive counseling were provided.
Visits were categorized based on four primary reasons for the visit: family planning, reproductive health, annual well-woman visits, and primary care. Reasons for the visit were grouped according to the chief complaint of the patient and the clinician’s documented reason for the visit. If there was more than one reason, each visit reason was counted separately. Visit reasons were not strongly correlated with each other, with correlation coefficients ranging from -0.32 to 0.03. We also assessed whether women had more than one reason of visit.
Clinic-reported provider specialties were assigned to three mutually exclusive categories: Primary care (i.e. family medicine, internal medicine, adolescent medicine), OB/GYN/women’s health, and multispecialty (two or more specialties at the clinic).
Patient age was categorized into women under 20 years, 20-29 years, and women 30 years and older. A binary variable was created to describe whether a non-contraceptive medical service was provided at the visit. Non-contraceptive medical services included the provision of immunizations and non-contraceptive drugs; treatment of an injury or acute or chronic illness; or pregnancy.
Referrals for preventive or reproductive health services included mammography, domestic violence services, substance abuse management or smoking cessation services, and other gynecological services.
SAS 9.4 Proc GLIMMIX was used for a multi-level logistic regression analysis with clinic site as the level-2 random effect. The study was approved by the University of California, San Francisco (UCSF) Institutional Review Board, the California Health and Human Services Agency (CHHS) Committee for the Protection of Human Subjects, and the California Department of Health Care Services (DHCS) Data Research Committee (DRC).
Results
Data abstraction
Overall, 1,244 charts from 63 clinics were abstracted, representing 18 counties in California. After excluding ineligible charts (women who had previously received a sterilization procedure or hysterectomy, or were in the sample due to coding errors), we kept 1,054 charts for the analysis.
Clinic specialties and client demographics
The majority (75%) of clinics described themselves as having a primary care specialty, whereas only 15% had multiple specialties, and 10% identified as having an OB/GYN or women’s health specialty. Women were on average 28 years old, with the largest proportion (42%) in the 20-29 age range. A fifth (21%) were adolescents and 37% were between 30-49 years.
Three plans could not provide information on race/ethnicity, which is kept in enrollment files that are not easily linked to the medical records. Of the 516 charts with race/ethnicity available, 42% were Hispanic. Parity was documented in only 522 of the charts. Where documented, most women had at least one child, and a third (34%) had three or more children (Table 1).
Table 1. Reported clinic specialties and documented patient demographics.
Clinic Specialty (n = 1054) |
N |
% |
Primary Care |
791 |
75% |
Multi-Specialty |
158 |
15% |
OB/GYN &Women’s Health |
105 |
10% |
Age (n = 1049) |
|
|
13-19 |
220 |
21% |
20-29 |
438 |
42% |
30-39 |
248 |
24% |
40+ |
143 |
14% |
Ethnicity (n = 516) |
|
|
White |
140 |
27% |
Hispanic |
217 |
42% |
Black |
59 |
11% |
Asian/Pacific Islander |
60 |
12% |
Other |
40 |
8% |
Parity (n = 522) |
|
|
0 Children |
60 |
27% |
1 Child |
160 |
31% |
2 Children |
125 |
24% |
3 or More Children |
177 |
34% |
Visit reason by clinic specialty
Two thirds (65%) of the visits had one visit reason and 35% two or more reasons. Visit reasons were mainly family planning (46%), annual/new visits (44%) and primary care visit reasons (41%). A smaller percentage (15%) of visits had a reproductive health visit reason. Having more than one reason of visit was highly correlated with annual visit reason (r=.78). Women presented often with more than one reason of visit. While clinicians working at clinics with primary care specialty had mainly primary care and annual/new visit reasons (47% each), they also had a large proportion of visits (37%) with family planning reasons. Correspondingly, visits to clinics with OB/GYN or women’s health specialties primarily had family planning as the reason of visit (65%), but also included annual/new visits (25%), and primary care (17%) visit reasons. The distribution of visit reasons at multi-specialty clinics included family planning as the reason of visit (75%), annual/new visits (43%), reproductive health (29%), and primary care (25%) (Table 2).
Table 2. Reason for patient visit stratified by reported clinic specialty and number of visit reasons (n=1,054).
|
Visit Reasons |
|
Clinic Specialty |
Family Planning |
Reproductive Health |
Primary Care |
New/Annual |
More than one Visit Reason |
Family Planning/
Women’s Health |
65% |
26% |
17% |
25% |
36% |
Multi-Specialty |
75% |
29% |
25% |
2021 Copyright OAT. All rights reserv
43% |
57% |
Primary Care |
37% |
11% |
47% |
47% |
59% |
Provision of contraceptive and preventive services
Contraceptive counseling, method provision, and referrals tended to occur more often in visits that had a family planning visit reason. For instance, 43% of charts with a family planning visit reason included documentation of contraceptive counseling, compared to 5% in visits with an annual health visit or primary care visit reason. In contrast, charts that had a primary care visit reason or annual health visit reason had higher percentages of referrals for follow-up primary care visits, provision of non-contraceptive medical services, and preventive health counseling (Figure 1).
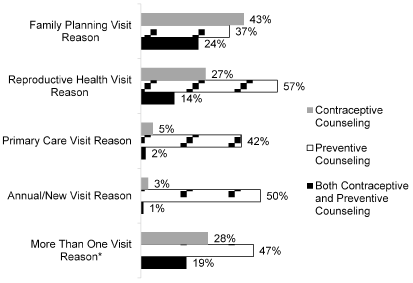
Figure 1. Provision of preventive and contraceptive counseling by visit reason (n = 1054).
*Not included in multivariable model due to a high correlation with annual visit reason.
Overall, 134 visits (13%) included both contraception and preventive health counseling during the same session. Provision of contraceptive and preventive counseling were not correlated (Phi = 0.14). Women who presented with more than one reason of visit were slightly more likely to receive contraceptive and preventive counseling (19%) than women with only one reason of visit (9%).
Multivariable analysis
A multilevel logistic regression model was constructed to assess the characteristics of client visits in which both preventive and contraceptive counseling occurred (Table 3).
Table 3. Associations between service, provider, and client characteristicsa and provision of both contraceptive and preventive counseling (n = 1054).
Characteristic |
Odds Ratio |
95% CI |
Visit Reason |
|
|
All Other |
Ref |
– |
Family Planning |
5.9 |
(2.7, 12.7) |
Reproductive Health |
3.1 |
(1.6, 6.0) |
Primary Care |
0.9 |
(0.4, 1.8) |
New/Annual |
1.4 |
(0.8, 2.4) |
Age |
|
|
20-29 years |
Ref |
– |
Under 20 years |
1.4 |
(0.7, 2.9) |
13-49 and 30-49 years |
0.5 |
(0.3, 1.1) |
Service at Visit |
|
|
No Non-Contraceptive Medical Service |
Ref |
– |
Non-Contraceptive Medical Service |
2.6 |
(1.3, 5.3) |
Referral Type |
|
|
No Referral |
Ref |
– |
Primary Care/Women's Health |
0.3 |
(0.1, 0.9) |
Provider Specialty |
|
|
Family Planning |
Ref |
– |
Multi-specialty |
36 |
(4.9, 273.9) |
Primary Care |
1.0 |
(0.2, 6.1) |
aIndependent variables: visit reason, referral for care, age, provider specialty.
In the multivariable analysis, women with a family planning visit reason had 5.9 times the odds of receiving both preventive and contraceptive counseling compared to those who did not have this visit reason, when controlling for age, clinic specialty, non-family planning service and referral (OR = 5.9, 95% CI = 2.7-12.7). Similarly, women with a reproductive health visit reason were about 3 times as likely to receive both counseling types compared to women with all other types of visit reasons. Yet, having a primary care or new/annual visit reason did not appear to significantly affect the likelihood of receiving both types of counseling. There were no differences by age in the odds of having integrated counseling.
Women who received a non-contraceptive medical service during their clinical visits had about three times the odds of receiving preventive and contraceptive counseling (OR = 2.6, 95% CI = 1.3-5.3). However, women who received primary care referrals were significantly less likely to receive both preventive and contraceptive care (0.3, 95% CI=0.1-0.9).
Women who were seen by a clinician at a multi-specialty clinic were significantly more likely than those seen at family planning specialty clinics to receive combined preventive and contraceptive counseling (OR = 36, 95% CI = 4.9-273.9). There was no significant difference in the likelihood of receiving both types of counseling between those seen at primary care and family planning specialty clinics.
Discussion
Clinical practice guidelines encourage coordinated care across specialties and the integration of preventive and family planning topics in primary and women’s health care [3,16]. Comprehensive counseling reduces the need for multiple medical visits and prevents fragmented health messages. The Affordable Care Act included access to contraception into the list of women’s preventive health services [17]. Preconception care topics that should be discussed with reproductive age women include preventive health topics such as weight management, smoking cessation, and management of chronic diseases [18]. In our medical record review, a third of the women presented to their managed care visits with more than one visit reason. Yet, only one in eight women (13%) received preventive health and contraceptive counseling at the same visit. This percentage was only slightly higher (19%) for women presenting with more than one visit reason.
Women with a family planning or reproductive health visit reason were more likely to also receive counseling on primary care topics, consistent with clinical practice standards for family planning visits [3]. Yet, visits with primary care visit reasons rarely combined contraceptive and preventive counseling topics. There were missed opportunities to address women’s contraceptive needs during annual well-woman visits where the discussion of preventive health behaviors is likely to occur and where women are likely to present with more than one visit reason. In addition, when prescribing medications with interactions or teratogenic side effects, clinicians need to address the effects of contraceptives, including potential drug interactions, on women’s fertility and chronic disease management. This is often not the case, and subspecialists may initiate medications important for women at risk of pregnancy (e.g. insulin, anti-infectives, or drugs that are teratogenic or affect fertility) without assessing contraceptive usage or providing contraceptive counseling [8,11,19].
The work setting may play a role in the provision of counseling. Clinicians tend to provide contraceptive counseling if they work alongside colleagues who have training in women’s health [8]. In this chart review, contraceptive and preventive counseling topics were more likely to be provided in an integrated form by clinicians at multi-specialty clinics than by those working at clinics with family planning or primary care specialties. Clinicians who can consult with colleagues of other specialties in the medical office may feel more comfortable discussing cross-specialty topics. As healthcare delivery moves toward coordinated care models such as the patient-centered medical home [20], it may become easier to address several topics during a clinic visit.
This analysis is limited to variables that can be retrieved from the abstracted medical records and may underestimate referral or counseling services if they were not recorded. Additionally, we could not include race/ethnicity or parity in the multivariable model due to high percentages of missing values. Furthermore, a chart review does not assess client preferences or concerns and whether these have been appropriately addressed in the patient-provider interaction. Chart review information on counseling needs to be complemented with patient feedback to determine counseling quality.
As managed care providers serve more women in need of reproductive health services, primary care visits provide the opportunity to counsel on contraception and preconception care in addition to preventive health counseling. Annual and well-woman visit, in particular, represent an underused opportunity to provide comprehensive client-centered counseling services and to facilitate prevention of unintended pregnancies and promotion of optimal women’s health.
Regardless of specialty, clinicians should address preventive and preconception counseling topics in women’s health visits and family planning counseling during annual well-woman and primary care visits.
Acknowledgements
We would like to thank Larry Suarez, software developer at 11Health Inc., for helping us modify the abstraction tool for the new iPad version.
Funding
This study was prepared by the University of California, San Francisco, Bixby Center for Global Reproductive Health and was supported by funding from an anonymous foundation. Additional support was provided by the National Center for Advancing Translational Sciences, National Institutes of Health, through UCSF-CTSI Grant Number UL1 TR001872. The publication’s contents are solely the responsibility of the authors and do not necessarily represent the official views of the NIH. All analyses, interpretations, or conclusions are those of UCSF.
References
- Sonfield A (2012) Beyond contraception: The overlooked reproductive health benefits of health reforms preventive services requirement. Guttmacher Policy Rev 15: 18-24.
- US Department of Health and Human Services. Preventive services covered under the Affordable Care Act, 2014. http://www.hhs.gov/healthcare/facts-and-features/fact-sheets/preventive-services-covered-under-aca (accessed 11 December 2016).
- Gavin L, Moskosky S, Carter M, Curtis K, Glass E, et al. (2014) Providing quality family planning services. MMWR Morbidity & Mortality Weekly Report 63:1-54.
- AAFP Policies Website, Primary Care. http://www.aafp.org.ucsf.idm.oclc.org/about/policies/all/primary-care.html (accessed 11 December 2016).
- Yarnall KS, Pollak KI, Østbye T, Krause KM, Michener JL (2003) Primary care: is there enough time for prevention? Am J Public Health 93: 635-641. [Crossref]
- Robinson R, Reiter J (2007) Behavioral consultation and primary care. Springer Science + Business Media, LLC.
- Thiel de Bocanegra H, Watts L, Menz M, Rao S, Darney P (2013) The 2011 Family PACT Medical Record Review: Assessing the Quality of Service. Sacramento, CA: Bixby Center for Global Reproductive Health. University of California, San Francisco, CA.
- Akers AY, Gold MA, Borrero S, Santucci A, Schwarz EB (2010) Providers’ Perspectives on Challenges to Contraceptive Counseling in Primary Care Settings. J Womens Health 19: 1163-1170. [Crossref]
- Lohr PA, Schwarz EB, Gladstein JE, Nelson AL (2009) Provision of contraceptive counseling by internal medicine residents. J Womens Health 18: 127-131. [Crossref]
- Pollak KI, Krause KM, Yarnall KS, Gradison M, Michener JL, et al. (2008) Estimated time spent on preventive services by primary care physicians. BMC Health Serv Res 8: 245. [Crossref]
- Schwarz EB, Maselli J, Norton M, Gonzales R (2005) Prescription of teratogenic medications in United States ambulatory practices. Am J Med 118: 1240-1249. [Crossref]
- Robbins CL, Gavin L, Zapata LB, Carter MW, Lachance C, et al. (2016) Preconception Care in Publicly Funded US Clinics That Provide Family Planning Services. Am J Prev Med 51: 336-343. [Crossref]
- Dunlop AL, Jack B, Frey K (2007) National recommendations for preconception care: the essential role of the family physician. J Am Board Fam Med 20: 81-84. [Crossref]
- Essential Access Health Women and Health Care Reform Coalition. Pathways to Coverage and Care: Fufilling the Promise of Health Care Reform for Women. Los Angeles, 2016. http://www.essentialaccess.org/sites/default/files/Essential-Health-WHCR-Focus-Group-Report-20160822.pdf Accessed: June 5, 2017.
- California Department of Health Care Services. Family PACT, 2016. http://www.familypact.org/Home/home-page (accessed 12 February 2016).
- March of Dimes, Implicit Interconception Care Toolkit, 2017. https://prematurityprevention.org/Toolkits-Reports/IMPLICIT-interconception-care-toolkit (accessed 15 April 2017).
- Health Resources and Services Administration. Women’s Preventive Services Guidelines, 2016. https://www.hrsa.gov/womensguidelines2016/index.html accessed 04/15/2017
- Centers for Disease Control and Prevention, Preconception Health and Health Care, Content of Care for Women: Every Woman, Every Time, 2014. https://www.cdc.gov/preconception/careforwomen/index.html (accessed 15 April 2017).
- Mody SK, Farala JP, Wu J, Felix R, Chambers C (2015) Using the electronic medical record to assess contraception usage among women taking category D or X medications. Birth Defects Res A Clin Mol Teratol 103: 887-891. [Crossref]
- Nielsen M, Olayiwola JN, Grundy P, Grumbach K, Shaljian M (2014) The Patient-Centered Medical Home's Impact on Cost & Quality: An Annual Update of the Evidence, 2012-2013. Patient-Centered Primary Care Collaborative.

