Group G streptococci are a relatively less common cause of streptococcal infections. Here we report a bursitis case due to Group G streptococcus in a patient of orthopedics and traumatology department, with complaints of pain in the right knee without any underlying primary metabolic disease and trauma.
Group G streptococci, bursitis, infection
Septic bursitis (SB) is characterised by inflammation secondary to bursal infection. As they are superficially located, olecranon and prepatellar bursa are more prone to septic bursitis infection [1]. SB cases most commonly (approximately 85%of cases) occur in young to middle-aged men. They account for one third of acute bursitis cases presenting to the hospitals [1]. All four ‘cardinal’ signs of inflammation: calor (heat), dolor (pain), rubor (redness) and tumor (swelling) ususally present in prepatellar bursitis [2]. Although Lancefield group A (GAS) and group B streptococci are the most common streptococci in clinical presentations of streptococcal infections, several studies have reported that group G streptococci (GGS) may also share many microbiological characteristics with GAS and produce similar invasive infections such as; bacteremia and endocarditis, septic arthritis and osteomyelitis, puerperal infections, and meningitis [3].
A 62-year-old female patient without any chronic disease or trauma history applied to the orthopedics and traumatology outpatient clinic with complaints of pain in her right knee which began two days ago. In her physical examination, sensitivity in the right knee, swelling in prepatellar area and limitation of motion were detected. The patient was diagnosed as prepatellar bursitis without septic arthritis, and synovial fluid sample was collected from bursa. After ceftriaxone prophylaxis, the patient was undergone a bursectomy operation, and following the operation she was discharged with total cure and oral ciprofloxacin, and amoxicillin–clavulanate therapy.
Synovial fluid sent to the laboratory was inoculated on 5% sheep’s blood, chocolate and Eosin Methylene Blue (EMB) agars (Becton Dickinson, USA) according to the usual techniques for medical bacteriology, and incubated at 5% CO2 incubator for 18-24 hours. The microscopy of the fluid revealed; 57.600 WBC/µL (85% PMNLs), 6.700 RBC/µL. After 24 hours of incubation; β-haemolytic greyish colonies were detected on 5% sheep’s blood and chocolate agar plates. Catalase negative, non-motile gram positive cocci were identified as group G streptococcus both with Streptococcal latex test (Plasmatec, UK) and automated identification and susceptibility test system (PhoenixTM, BD, USA) (Figure 1). Antimicrobial susceptibility test of the isolate was performed by Kirby-Bauer disk diffusion method and detected as susceptible to penicillin, clindamycin, erythromycin, linezolid, teicoplanin and vancomycin according to European Committee on Antimicrobial Susceptibility Testing (EUCAST) rules.
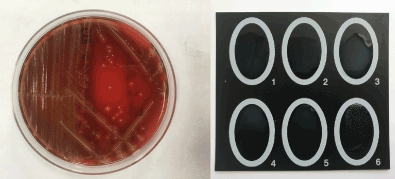
Figure 1. β-haemolytic greyish colonies on 5% sheep’s blood agar plate (on the left), streptococcal agglutination test (on the right).
GGS are asymptomatic colonizers of the skin, gastrointestinal tract, and female genital tract [2]. GGS has been widely accepted to cause opportunistic and nosocomial infections in patients with underlying; malignancy, immunocompromised state, cardiovascular disease, diabetes mellitus, cirrhosis, alcoholism, bone and joint disease. Usually it is uncommon to find GGS as a cause of bursa infection in patients who do not have primary metabolic disease, as in our patient [4].
2021 Copyright OAT. All rights reserv
Most of the GGS strains are sensitive to penicillins, vancomycin, erythromycin and cephalosporins [5]. The patient was treated with ceftriaxone, ciprofloxacin, and amoxicillin – clavulanate. Despite being penicillin sensitive, ceftriaxone, ciprofloxacin and amoxicillin – clavulanate were selected in antimicrobial therapy most probably due to antibiotic preference tendencies of clinicians.
Although detailed history of the patient is unknown, the prepatellar bursa which is located between the patella and the overlying skin, most probably might became inflamed due to repeated trauma, such as kneeling on hard surfaces in this case [6].
- Tuff T, Chrobak K (2016) Septic olecranon and prepatellar bursitis in hockey players: a report of three cases. J Can Chiropr Assoc 60: 305-310. [Crossref]
- Tracy RP (2006) The Five Cardinal Signs of Inflammation: Calor, Dolor, Rubor, Tumor and Penuria (Apologies to Aulus Cornelius Celsus, De medicina, c. A.D. J Gerontology 61: 1051-1052.
- Deng W, Farricielli L (2014) Group G streptococcal sepsis, septic arthritis and myositis in a patient with severe oral ulcerations. BMJ Case Rep.
- Skogberg K, Simonen H, Renkonen OV, Valtonen VV (1988) Beta-haemolytic group A, B, C and G streptococcal septicaemia: a clinical study. Scand J Infect Dis 20: 119–25. [Crossref]
- Zaoutis T, Schneider B, Steele Moore L, Klein JD (1999). Antibiotic susceptibilities of group C andgroup G streptococci isolated from patients with invasive infections: evidence of vancomycin tolerance among group G serotypes. J Clin Microbiol 37: 3380–3. [Crossref]
- Kratimenos P, Koutroulis I, Marconi D, Ding J, Plakas C, Fisher M (2014) Septic bursitis in an- 8-year-old boy. Case Rep Pediatr [Crossref].

