According to The Seventh Report published in 2003 by the Joint National Committee (JNC 7), patients with systolic blood pressure of 120-139 mmHg or diastolic blood pressure of 80-89 mmHg are diagnosed with prehypertension. Prehypertension defined in different terms in different guidelines. Prehypertension often coexists with comorbidities such as ischemic heart disease, stroke and diabetes Early detection of hypertension, which is an important public health problem, is very important in both economically developing and developed countries. That's why we wrote this article to draw attention to prehypertension.
Prehypertension, comorbidity, health problem
According to The Seventh Report published in 2003 by the Joint National Committee (JNC 7), patients with systolic blood pressure of 120-139 mmHg or diastolic blood pressure of 80-89 mmHg are diagnosed with prehypertension [1]. According to the 2017 American hypertension guideline, the definition of elevated blood pressure is used in patients with systolic blood pressure of 120-129 mmHg and diastolic blood pressure <80mmHg [2]. According to the 2018 European guideline, the definition of high normal blood pressure is used in patients with systolic blood pressure of 130-139 mmHg and / or diastolic blood pressure of 85-89mmHg [3].
In a study by Vasan, et al. 30% of patients progressed from prehypertension to hypertension over a 4-year period [4]. Prehypertension often coexists with comorbidities such as ischemic heart disease, stroke and diabetes [5]. Therefore, early detection of hypertension, which is an important public health problem, is very important in both economically developing and developed countries. That's why we wrote this article to draw attention to prehypertension.
Prehypertension has been associated with increased body mass index, increased waist circumference, dyslipidemia, high fasting plasma glucose, smoking, insulin resistance, alcohol consumption and advanced age [5]. Certain factors have been associated with the progression of prehypertension to hypertension. Advanced age, male gender, increased C reactive protein, high salt intake, mongolian race, obesity, family history and increased waist circumference are among these factors [6-8].
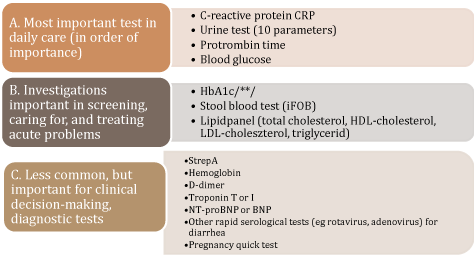
Figure 1. POCT categorization by frequency of use of the primary care
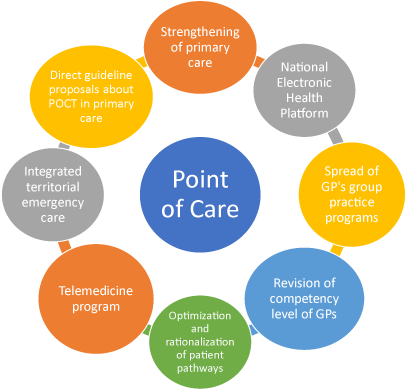
Figure 2. Connecting health policy priorities, and enabling factors for POCT dissemination in primary care
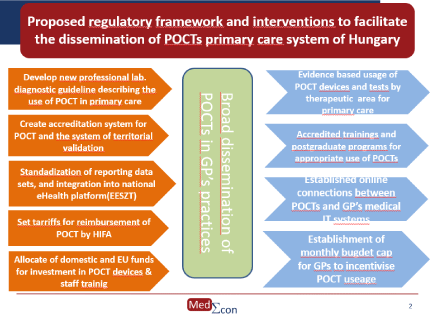
Figure 3. Favorable regulatory environment and necessary interventions in the primary care in order to support the dissemination of POCT
Masked hypertension should be evaluated by ambulatory blood pressure monitoring in patients with high normal blood pressure, according to the European guideline [3].
According to the American guideline [2], after 3 months of lifestyle change, ambulatory or home blood pressure monitoring is performed if office systolic blood pressure is 120-129 mmHg and diastolic blood pressure <80 mmHg. If the blood pressure is 130/80 mmHg and above in this follow-up, masked hypertension is diagnosed. In this case, both lifestyle changes are made and drug treatment is started. If blood pressure is below these values, a lifestyle change is made due to increased blood pressure (high normal blood pressure). In addition, annual ambulatory blood pressure monitoring is performed to determine progression or masked hypertension.
Table 1. Advantages and Disadvantages of POCTs in primary care
Non-pharmacological approaches are recommended for all patients with prehypertension, as lifestyle changes such as weight loss, reduction of salt consumption and increased physical activity effectively reduce the risk of cardiovascular events. In patients with prehypertension, a reassessment is made 3-6 after lifestyle changes [3]. A meta-analysis of 10 randomized controlled trials showed that the risk of stroke and major cardiovascular events was reduced with antihypertensive therapy in patients with high normal blood pressure in high and very high risk patients [3].
Pharmacological therapy is recommended in patients with high normal blood pressure with diabetes mellitus, chronic kidney disease, or coronary artery disease with a class 2b indication according to the 2018 European guidelines [3]. In the TROPHY and PHARAO studies, pharmacological therapy has been shown to significantly reduce the development of hypertension in prehypertensive patients [9]. Drugs that inhibit the renin-angiotensin-aldosterone system in prehypertensive patients are the most promising group [10]. In addition, in a study conducted with prehypertensive patients, the use of low-dose diuretics provided optimal blood pressure.
- Chobanian AV, Bakris GL, Black HR, Cushman WC, Green LA, et al. (2003) Seventh report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure. Hypertension 42: 1206-1252. [Crossref]
- Carey RM, Calhoun DA, Bakris GL, Brook RD, Daugherty SL, et al. (2018) Resistant hypertension: detection, evaluation and management, A Scientific Statement from the American Heart Association. Hypertension 72: e53-e90. [Crossref]
- Williams B, Mancia G, Spiering W, Rosei EA, Azizi M, et al. (2018) 2018 ESC/ESH Guidelines for the management of arterial hypertension. Eur Heart J 1: 1–98. [Crossref]
- Vasan RS, Larson MG, Leip EP, Kannel WB, Levy D (2001) Assessment of frequency of progression to hypertension in nonhypertensive participants in the Framingham Heart Study: a cohort study. Lancet 358: 1682-1686. [Crossref]
- Erem C, Hacihasanoglu A, Kocak M, Deger O, Topbas M (2009) Prevalence of prehypertension and hypertension and associated risk factors among Turkish adults: Trabzon Hypertension Study. J Public Health (Oxf) 31: 47-58. [Crossref]
- Pitsavos C, Chrysohoou C, Panagiotakos DB, Lentzas Y, Stefanadis C (2008) Abdominal obesity and inflammation predicts hypertension among prehypertensive men and women: the ATTICA Study. Heart Vessels 23: 96-103. [Crossref]
- De Marco M, de Simone G, Roman MJ, Chinali M, Lee ET, et al. (2009) Cardiovascular and metabolic predictors of progression of prehypertension into hypertension: the Strong Heart Study. Hypertension 54: 974-980. [Crossref]
- Zheng L, Sun Z, Zhang X, Xu C, Li J, et al. (2010) Predictors of progression from prehypertension to hypertension among rural Chinese adults: results from Liaoning Province. Eur J Cardiovasc Prev Rehabil 17: 217-222. [Crossref]
- Pimenta E, Oparil S (2010) Prehypertension: epidemiology, consequences and treatment. Nat Rev Nephrol 6: 21-30. [Crossref]
- Fuchs FD, Fuchs SC, Poli-de-Figueiredo CE, Figueiredo Neto JA, Scala LCN, et al. (2018) Effectiveness of low-dose diuretics for blood pressure reduction to optimal values in prehypertension: a randomized clinical trial. J Hypertens 36: 933-938. [Crossref]



