Posterior Reversible Encephalopathy (PRES) syndrome is a very rare clinical and neuroradiological condition which is seen in certain patient groups and creates awareness. In the case series, the predominance of female patients is 2/1.Risk factors are hypertension, preeclampsia or eclampsia, renal disease, immunosuppressive therapies and endothelial dysfunction. The true pathophysiological mechanisms have not yet been fully elucidated. It is also controversial that PRES has preferred the posterior brain region. The classic findings of PRES are acute mental state changes, headache, visual disturbances and seizures.
In this case report, we aimed to show the importance of early diagnosis and treatment in the patient who was diagnosed with postpartum psychosis according to the clinical and radiological findings but was found to be PRES at the end of the period until coma.
A 19-year-old female patient had mental status changes within 10 (ten) days following a normal pregnancy and normal vaginal delivery, and she had unrest and agitation in the form of somnolans, confusion, and attacks. Psychiatric treatment was started with the diagnosis of postpartum psychosis, followed by a nervous breakdown, and was placed in the intensive care unit 20 (twenty) days postpartum upon the development of encephalopathy, lethargy and coma.
The patient had hypotonic tetraplegia, severe dyskinesia and central vomiting after intensive care. She was feeding on the PEG. Neuroradiological investigations at the time of the onset of clinical findings were evaluated as normal, and two weeks later, the cranial MRI showed widespread lesions in the gray matter areas of the cerebellum, basal ganglia and cerebral cortex. In intensive care unit, parenteral antiepileptic treatment was applied with non-convulsive status clinic.
brain MRI, encephalopathy, PRES syndrome
Posterior Reversible Encephalopathy (PRES) syndrome is a very rare clinical and neuroradiological case, which is distinctive, raises awareness and is seen in specific patient groups. In the case series, the superiority of female patients at the ratio of 2/1 draws attention. However, all the age groups are potentially affected [1]. Risk factors are hypertension, preeclampsia or eclampsia, renal disease, infections, cytotoxic and/or immunosuppressive treatments, and the situations accompanied by endothelial dysfunction. Actual pathophysiological mechanisms have not been fully elucidated yet. It is also controversial that PRES apparently prefers the posterior brain region. The classical findings of PRES are acute mental state changes, headache, visual disturbances and seizures. Mental state changes can vary from mild somnolence to stupor, and disturbances and agitations occurring as attacks can also be seen. Reduced wakefulness, confusion and concentration difficulties are common. Essentially four types of brain magnetic resonance imaging (MRI) are defined. There is no single diagnosis indicator. Together with appropriate clinical findings, MRI can less likely verify brain tomography (BT) diagnosis and exclude alternative causes. Strength of clinical findings varies. Slight confusion or agitation can be seen in the cases; however, they may also go into a coma. Seizures and status epilepticus are common, and non-convulsive status epilepticus may be more common than generalized status epilepticus. When PRES and non-convulsive status are combined, it may be confused with psychosis, drug intoxication or psychogenic conditions [1-4].
In the current study, it is aimed to submit a PRES case who had normal blood pressure during pregnancy and in the early postpartum period but diagnosed as postpartum psychosis due to hypertension, mental status changes, visual hallucinations, wakefulness defect, agitation and seizure clinics and treated at the intensive care unit after status of coma developed.
In a nineteen-year-old female patient, mental changes started to occur within 10 (ten) days following a normal pregnancy and normal vaginal delivery, and she had somnolence, confusion and discomfort and agitations occurring as attacks. Psychiatric treatment was started with the diagnosis of postpartum psychosis, it was followed by a seizure that was interpreted as a nervous breakdown and the patient was hospitalized in the intensive care unit after postpartum 20 (twenty) days upon the development of encephalopathy, lethargy and coma. Throughout the intensive care treatment, hypotonic tetraplegia and severe dyskinesia developed in the case receiving antihypertensive therapy, after the intensive care and she became bed-dependent and central vomiting occurred. The patient was fed with formula via Percutaneous Endoscopic Gastronomy (PEG). Neuroradiological examinations at the time of onset of the clinical findings were evaluated as normal, and in the cranial MRI taken two weeks later, widespread lesions in the gray matter areas of the cerebellum, basal ganglia and cerebral cortex were shown and the case was diagnosed as severe PRES and parenteral antiepileptic treatment was applied with non-convulsive status. Cerebrospinal fluid (CSF) analysis was normal. There was no abnormality in the vasculitis indicators and blood values. In electroencephalography (EEG), generalized surface rhythm irregularity and epileptiform activities had occurred.
1.5 Tesla MRIı study was applied for the case. Cranial MRI examination was performed according to the cranial MRT1W, axial (section thickness 5.5 mm; TR 560;TE:9.5 Matrix 288*182) and T2W sagittal (section thickness: 5 mm, TR: 5300, TE:82, matrix: 384*192) and T2 flair axial (section thickness 5.5 mm,TR:8000, TE: 98,TI: 2000, matrix:320*224); T2 axial (section thickness 5.5 mm,TR:3700,TE:88 matrix: 320*256) techniques (Figures 1-4).
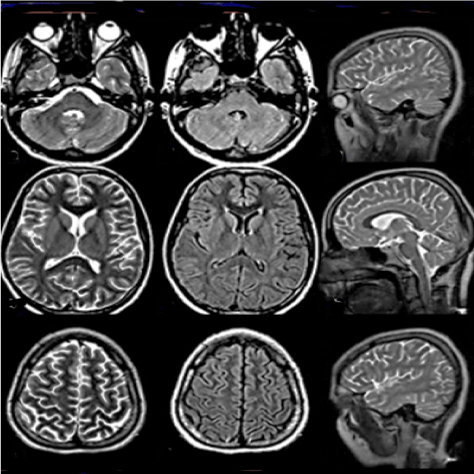
Figure 1. Patient’s first film. T2W,T2flair, T2 sagittal normal MRI
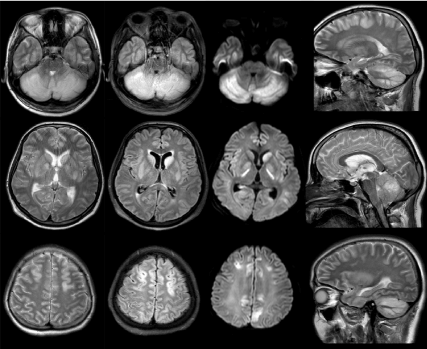
Figure 2. T2w,T2 sagittal, T2 flair brain imaging; Edema and thickening due to involvement in cortical gray matter areas of cerebellum,basal ganglia,frontal and parietal lobe.Diffusion images in the same regions of diffusion restriction
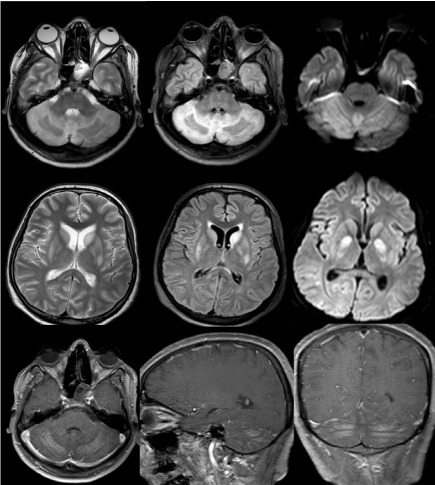
Figure 3. Control MRI of the patient after 10 days.T2W,T2 flair axial imaging. Lesions in the
cerebellum and basal ganglia persist but regression exists. Contrast enhancement in the areas of gray matter in the rebellum ,especially in the T1W contrast section
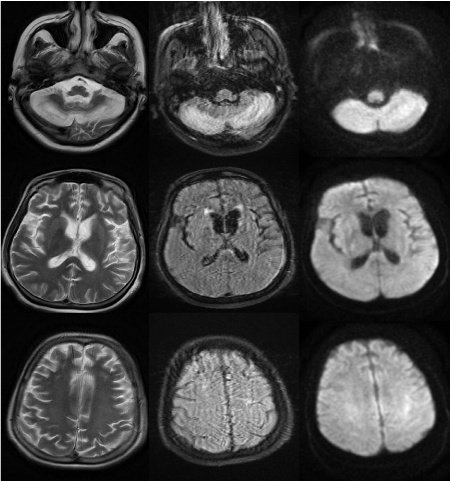
Figure 4. Control MRI of the patient after two and a half months:T2W and T2flair axial sections, Cerebral and basal ganglia lesions disappeared .However, there is still a cerebellum lesion. Diffuse cerebral atrophy has developed
PRES is an acute neurotoxic syndrome. Although it is typically reversible, it may also cause a long-term disability. Impaired consciousness can be serious from confusion to somnolence, from lethargy to encephalopathy or coma. Impaired consciousness is reported as 13-90%. Seizure activity occurs in 92% of the cases. Focal neurological symptoms are not mentioned at all or specified in 3-17%. 20-30% of the cases have normal blood pressure, and neurological findings are often difficult to resolve, and high evidence causing suspicion are required in clinical context.
Non-specific clinical findings and majority of the radiological models increase the difficulties in diagnosis. Differential diagnosis should be performed by the clinical findings such as ictal or post-ictal situations (whether accompanied by status epilepticus or not), progressive multifocal leukoencephalopathy (PML), severe leucoencephalomalacia, CADASIL (cerebral autosomal dominant arteriopathy with subcortical infarcts and leukoencephalopathy), infectious encephalitis, acute disseminated encephalomyelitis, MELAS (Mitochondrial myopathy, encephalopathy, lactic acidosis and episodes similar to stroke), cerebral venous thrombosis and ischemic stroke. MRI characteristics of these clinical findings were reported separately [2,5-7].
In PRES, four types of MR (Magnetic Resonance) imaging are defined. In the present case, central pattern was observed at which relatively lobar exposure was lower and basal ganglia and brain stem were more affected. There is no single diagnosis indicator. Together with appropriate clinical findings, MRI can less likely verify BT (Brain Tomography) diagnosis and exclude alternative causes. Seizures and status epilepticus are common and non-convulsive status epilepticus may be more common than generalized status epilepticus. In the present case, PRES and non-convulsive status occurred together. Therefore, it was thought as psychosis and it could not be diagnosed [8,9].
In this case report, it is aimed to review the characteristics of the disease according to the results of clinical and radiological examinations and to show that the importance of early diagnosis and treatment and that the disease may progress with a serious deterioration if not treated.
- Johnson EK, Lin MY (2011) Posterior reversible encephalopathy syndrome. Hosp Med Clin 4: 358-367.
- Legriel S, Pico F, Azoulay E (2011) Understanding posterior reversible encephalopathy syndrome. Annual Update in Intensive Care and Emergency Medicine 3: 631-653.
- Granata G, Greco A, Iannella G, Granata M, Manno A, et al. (2015) Posterior reversible encephalopathy syndrome-Insight into pathogenesis, clinical variants and treatment approaches. Autoimmunity Reviews 14: 830-836. [Crossref]
- Hobson EV, Craven I, Blank SC (2012) Posterior reversible encephalopathy syndrome:A truly treatable neurologic illness. Peritoneal Dialysis International 32: 590-594. [Crossref]
- Lang CR, Coeller N (2013) Posterior reversible encephalopathy syndrome:a unique presentation. American Journal of Emergency Medicine 31: 1423.e3-1423e4. [Crossref]
- Kuzu M, Tezcan S, Sorgun MH, Işıkay CT (2016) Postpartum normotansif PRES olgusu. Ankara Üniversitesi Tıp Fakültesi Mecmuası 69: 33-35.
- Türker M, Zeyneloğlu P, Pirat A, Araz C, Dönmez F et al. (2011) Yoğun bakım ünitesinde izlenen posterior reversible ensefalopati sendromu (PRES): Olgu sunumu. Journal of the Turkish Society of Intensive Care 9: 103-106.
- Sha Z, Moran BP, McKinney AM, Henry TR (2015) Seizure outcomes of posterior revesible encephalopathy syndrome and correlations with electroencephalographic changes. Epilepsy&Behavior 48: 70-74. [Crossref]
- Demirtaş G, Demirtaş Ö, Tursun İ, Şahin T, Şahin C (2016) Postpartum PRES (posterior reversible encephalopathy syndrome) olgusunun sunumu ve literatür taraması. Kocatepe Tıp Dergisi 17: 44-49.




