Posttraumatic aneurysm (pseudoaneurysm) although are described extensively, occur infrequently in clinical practice, being them found with most frequently after surgical procedure such as osteotomies and TMJ surgery; this vascular disease also occurs regularly in wounds caused by projectile of firearm, and be originate weeks or months after the trauma. In the following case report of early onset pseudoaneurysm of the internal maxillary artery, which is quickly diagnosed by a high clinical suspicion of vascular injury and performing selective carotid angiography confirmed the diagnosis of pseudoaneurysm of almost immediate appearance. This patient is successfully treated with embolization coiling and had no complications after the procedure.
An aneurysm is an irreversible dilation of an artery. This may involve all layers of the arterial wall (true aneurysm) or only a portion of the underlying wall and tissue (false aneurysm or pseudoaneurysm) [1]. Traumatic extracranial aneurysms are infrequent injuries caused by dissection or direct damage to the arterial wall as a result of traumatic brain injury, either from a closed or penetrating trauma [2,3]. Because the transmural or circumferential damage of the vessel causes an extravasation of the blood within the surrounding tissue, thus producing a contained and throbbing hematoma, it is currently termed a false aneurysm, or better known as a pseudoaneurysm [1,3,4].
Post-traumatic aneurysms are unusual lesions in clinical practice and although they correspond to <1% of all aneurysms that develop in the cephalic region, their rupture is a catastrophic event that can lead to severe life-threatening hemorrhage or thromboembolism [1,4-6].
Consequently, the development of pseudoaneurysms in the internal maxillary artery secondary to blunt or penetrating trauma in the maxillofacial region as the main etiology, supports the extended study with additional images and adequate endovascular management to provide the best outcome to this clinical entity [1,4,5,7,8].
However, within the literature it has been stated that the development of a pseudoaneurysm may require 1 to 8 weeks, after the initial trauma, and therefore its diagnosis is made weeks to months later to the insult of the glass; thus, the following case report presents an early-onset pseudoaneurysm [5,7,9,10].
A 40-year-old male patient presented with a gunshot wound, which enters the left zygomatic region, with a superior anterior to inferior posterior trajectory without crossing the midline, lodging in the cervical region. patient who enters oriented person space time, with Glasgow coma scale 15/15, with Mark Gunn pupil left eye and limitation for abduction of the same eye, presents ipsilateral facial paralysis, without any other associated neurological deficit, with tendency to desaturation due to obstruction of the airway. Valued by the peripheral vascular surgery service, who do Doppler of neck vessels and do not show pathology at this level.
In the imaging studies performed in the emergency department, there is no evidence of intracranial injury, I draw considerable attention to the commitment of the lateral mass of C1 (Figure 1 and Figure 2); Due to the high suspicion of lesion of the left vertebral artery, cerebral angiography was decided (Figure 3).
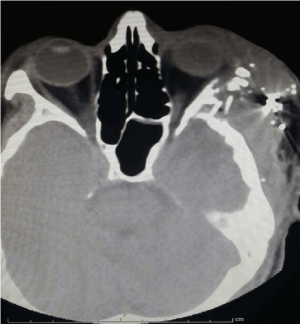
Figure 1. Simple cerebral scanography showing fracture of the lateral wall, left orbit with metallic and bone splinters in soft tissues
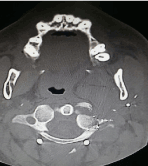
Figure 2. Commitment of the left lateral mass of C1
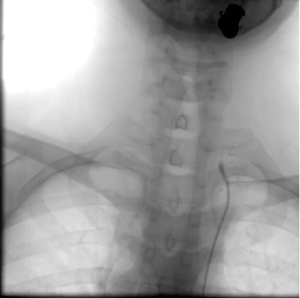
Figure 3. Absence of flow of the left vertebral artery
In cerebral angiography, Pseudoaneurysm dependent on the left maxillary artery is evidenced, as well as ipsilateral vertebral artery thrombosis, it was decided to carry out pseudoaneurysm embolization immediately, with satisfactory evolution with improvement in oxygenation which allowed extubation.
The posttraumatic pseudoaneurysm of the internal maxillary artery is an established complication with rare incidence in maxillofacial trauma, which usually occurs 1 to 8 weeks after vessel injury and depends on the arterial defect caused [1,5,10].
The majority of documented pseudoaneurysms of the internal maxillary artery are sequelae of closed or penetrating trauma, with the highest risk factor being trauma that causes injury directly to the head followed by a spinal fracture; and in a smaller proportion it can also occur as a complication of infections, orthognathic or temporomandibular joint surgery, after fractures of the mandibular condyle or by puncture of the arterial wall by medical procedures [5,6,10]. More rarely, pseudoaneurysms of the internal maxillary artery may be a consequence of post-radiation vasculopathy or tumor invasion [1].
Although they correspond to less than 1% of all aneurysms of the head, the incidence of pseudoaneurysms after a maxillofacial trauma has been reported in a range from 1 to 11% [7,11]. Nevertheless, and despite the fact that the incidence in the maxillary artery has not been determined; if it is not diagnosed or managed, there is a risk of thromboembolism or exsanguination after the rupture of the pseudoaneurysm that endangers the life of the patient.
The superficial temporal artery, the facial artery and the internal maxillary artery are the 3 most common branches of the external carotid system that potentially develop a pseudoaneurysm subsequent to a high-speed trauma [5,8].
The location of the maxillary artery usually isolates the vessel from the injury. As the external carotid artery branches out, it is protected by several structures belonging to the soft and hard tissues, within these the mass of the parotid gland and the bottom of the pterygopalatine fossa. It is in this surrounding tissue labyrinth that it is most susceptible to trauma due to the effect of maxillary fragments [8]. This is why the cause most related to the pseudoaneurysm of the maxillary artery is the penetrating trauma; since the artery is supported medially by soft tissues, but still relatively immobile, it is lacerated by the sharp edges of the bone fragments subsequent to the high-speed penetrating trauma in said region [9].
The classical clinical description of the pseudoaneurysm of the maxillary artery is a firm, painful and pulsatile mass, which is in synchrony with the heart rhythm, which is frequently confirmed by auscultation, since in some patients it is not possible to feel the pulsation more, however. they refer to the pulsating sensation in said area. The diagnostic suspicion is strongly based on a previous history of trauma and a clinical examination initially, but the correct diagnosis must be complemented with conventional arteriography, particularly when the clinical findings are insignificant, as in the present case due to its early appearance [7,8,10].
The appearance of post-traumatic aneurysms in the internal maxillary artery has been reported in a range of weeks and months after the traumatic event, with the earliest time being 7 days later [5,7,9,10-15]. Contrary to the majority of the case reports that can be reviewed in the literature, this patient with the appearance of a pseudoaneurysm in the maxillary artery almost immediately, which was diagnosed by performing a conventional angiography after a suspicion clinic by trauma mechanism and tomographic findings of high risk of vascular injury (Figure 4).
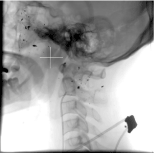
Figure 4. Aneurysmatic Dilatation Left maxillary artery 1.8 cm, width 2 cm
The clinical picture of this patient presented an indication for a neuroimaging evaluation; as indicated by the recommendations for head trauma of the NICE guidelines, which indicates the performance of an urgent image in the presence of focal neurological deficit; given in this patient by peripheral facial paralysis, the pupils of Marcus-Gunn that reflect damage in the optic nerve, and the injury in the abduction of the left eye [12-14]. Additionally, there are risk factors widely associated with the appearance of post-traumatic aneurysms at this level, such as projectile entry in the orbitopter area, the trajectory of the projectile is related to the great cerebral vessels, or in the presence of a subarachnoid hemorrhage or intracerebral hematoma. without another probable explanation [12,14].
The assessment of the patient with risk factors for developing a post-traumatic aneurysm should be evaluated early with radiological imaging. Taking into account that the time of onset of pseudoaneurysms is not known, arteriography is proposed by digital subtraction to all patients with gunshot wound having a vascular path or projectile entry in the orbito-pterional region [11,14]. This should be repeated in a prudent time, because a negative angiogram does not exclude the possibility of a traumatic pseudoaneurysm. The performance of the procedure again after 14 days is the time validated and recommended by the majority of authors, after a negative initial angiogram and patient with clinical, injury mechanism and risk factors for training of pseudoaneurysm [11,12,14,16].
Angiography is already widely considered in the literature as Gold Standard in the diagnosis of post-traumatic aneurysm, it is also preferred by specialists to perform an adequate non-surgical treatment of this entity, by endovascular embolization of the pseudoaneurysm [1,11,12,16-18]. The main advantages are the low risk of complication of the procedure, access to surgically difficult vessels, therapeutic intervention immediately after the diagnosis and verification of effectiveness by postembolization angiogram [1,9,12]. Although it is not a routine option to diagnose pseudoaneurysms but rather has better utility after using non-invasive imaging technique (contrast-enhanced CT, magnetic resonance imaging, or in some cases duplex ultrasound), when the lesion has been evaluated and endovascular treatment it is viable [1,8].
Most reports adhere strictly to the endovascular management of this type of lesions compared to surgical exploration, partly due to the difficulty of achieving adequate hemostasis because the internal maxillary artery has a large blood supply network from the side against the lateral and its connection with the internal carotid artery, without excluding that pseudoaneurysms that appear in distal areas of the maxillary artery have a difficult surgical approach and imply a greater risk of damage of adjacent structures and complications related to the surgical wound [1,7-10].
During embolization therapy, agents that occlude the lumen of the vessel are used, metal coils (coils) are preferred in the pseudoaneurysms of the maxillary artery and in this patient, because its effectiveness has been demonstrated when embolizing large vessels. useful in permanent embolization, and its double embolic capacity based on the mechanical action of bonina itself and its thrombogenic action by favoring the appearance of thrombi in its fibers, whether Dacron or Nylon [1,7,8]. This case reported a pseudoaneurysm formation of unusual early onset after a gunshot wound in the zygomatic region, its rapid diagnosis with arteriography and its successful management by endovascular technique.
The clinical suspicion of a pseudoaneurysm following a trauma with risk factors for the development of a traumatic aneurysm is decisive in the early diagnosis and adequate and immediate management. In this case, the clinical symptoms associated with the mechanism of injury and immediate radiological images contributed to the effective diagnosis of a pseudoaneurysm in the early-onset internal maxillary artery and elucidated a course of action in the approach of patients with gunshot wounds, with a history of the projectile in the orbitopter area and / or high suspicion of vascular injury. Endovascular treatment followed by diagnostic carotidography provides a satisfactory outcome.
- Chakrabarty S, Majumdar SK, Ghatak A, Bansal A (2012) Management of Pseudoaneurysm of Internal Maxillary Artery Resulting from Trauma. Journal of maxillofacial and oral surgery 14: 203-208. [Crossref]
- Zangbar B, Wynne J, Joseph B, Pandit V, Meyer D, et al. (2015) Traumatic intracranial aneurysm in blunt trauma. Brain injury 29: 601-606. [Crossref]
- Fulkerson DH, Voorhies JM, McCanna SP, Payner TD, Leipzig TJ, et al. (2010) Endovascular treatment and radiographic follow-up of proximal traumatic intracranial aneurysms in adolescents: case series and review of the literature. Child's Nervous System 26: 613-620.
- Greenberg MS (2010) Handbook of Neurosurgery. New York: Thieme Medical Publishers.
- Takeshita T, Hayashi K, Horie N, Morikawa M, Suyama K, et al. (2012) Endovascular treatment of intractable bleeding from a traumatic pseudoaneurysm of the internal maxillary artery. The neuroradiology journal 25: 469-474.
- Foreman PM, Griessenauer CJ, Falola M, Harrigan MR (2014) Extracranial traumatic aneurysms due to blunt cerebrovascular injury: Clinical article. J Neurosurg 120: 1437-1445. [Crossref]
- Soh HY, Muda AS, Jabar NA, Nordin R, Nabil S, et al. (2015). Non-pulsatile traumatic pseudoaneurysm of the internal maxillary artery following trauma to mandible. Oral and maxillofacial surgery 19: 423-425. [Crossref]
- Wang D, Su L, Han Y, Fan X (2015) Embolization treatment of pseudoaneurysms originating from the external carotid artery. Journal of vascular surgery 61: 920-926.
- Yeo MS, Goh TL, Nallathamby V, Cheong EC, Lim TC (2012) Maxillary artery injury associated with subcondylar mandible fractures: A novel treatment algorithm. Craniomaxillofac Trauma Reconstr 5: 83-88. [Crossref]
- Nardis AC, Boraks G, Torres AM, Gaigher ET, da Silva RA (2011) Uncommon complication of facial fractures. International journal of oral and maxillofacial surgery 40: 440-442.
- Ambrosi PB, Valenca MM, Azevedo-Filho H (2012) Prognostic factors in civilian gunshot wounds to the head: a series of 110 surgical patients and brief literature review. Neurosurg Rev 35: 429-436. [Crossref]
- Temple N, Donald C, Skora A, Reed W (2015) Neuroimaging in adult penetrating brain injury: a guide for radiographers. J Med Radiat Sci 36: 122-131. [Crossref]
- National Clinical Guideline Centre (2014) Triage, assessment,investigation and early management of head injury in children, young people and adults. [Crossref]
- Ecklund JM, Sioutos P (2013) Prognosis for gunshot wounds to the head. World neurosurgery 82: 27-29. [Crossref]
- Bonfield CM, Grandhi R, Jankowitz BT, Tyler-Kabara EC (2014) Traumatic intracranial aneurysm after penetrating brain trauma. BMJ case reports 2014: 206130.
- Quintana EM, Garcia AG, Valdes PV, Martinez AM, Fernandez MB, et al. (2012) Nuestra experiencia en el diagnóstico y tratamiento de los seudoaneurismas cerebrales. Radiologia 54: 65-72.
- Fankhauser GT, Stone WM, Fowl RJ, O'Donnell ME, Bower TC, et al. (2015) Surgical and medical management of extracranial carotid artery aneurysms. Journal of vascular surgery 61: 389-393.
- Dubel GJ, Ahn SH, Soares GM (2013) Transcatheter Embolization in the Management of Epistaxis. In Seminars in interventional radiology 30: 249.




