Abstract
Peripheral ossifying fibroma (POF) represents a rare separate entity of reactive benign lesion of connective tissue origin, not being the soft tissue counterpart of central ossifying fibroma. The present article is a case report related to peripheral ossifying fibroma in a 13-year male who reported with a painless growth in the mandibular anterior region of jaw, its diagnosis, satisfactory clinical management along with brief review of literature.
key words
reactive benign lesion, Peripheral ossifying fibroma
Introduction
Gingival enlargement, particularly those belonging to the reactive group are frequently encountered in the oral cavity in the daily practice. Reactive lesions such as pyogenic granuloma, peripheral giant cell granuloma, irritational/traumatic fibroma and peripheral ossifying fibroma are innocuous in nature, rarely presenting with aggressive clinical features [1]. Amongst these lesions peripheral ossifying fibroma [POF] is an infrequently occurring focal, reactive, non-neoplastic tumor-like growth of the soft tissue that primarily arises from the interdental papilla [2]. It may be sessile or pedunculated, the color varying from pale pink to cherry with smooth surface accounting for 9% of all gingival growths. The present article highlights a case report related to peripheral ossifying fibroma in a 13-year male patient, its diagnosis, satisfactory clinical management along with reviewing its the current literature.
Case report
A 13-year-old male patient reported to the Department of Pediatric & Preventive Dentistry of Swargiya Dadasaheb Kalmegh Smruti Dental College and Hospital, Nagpur with a chief complaint of a painless growth in lower front region of jaw for one year. The patient’s history revealed the reoccurrence of soft tissue growth in lower anterior region of jaw for which he had underwent surgical excision one and half year back. Intraoral examination revealed a single pedunclated 15 mm × 15 mm irregular pale pink growth extending mesiodistally from distal surface of 31 up to the mesial surface of 42 and cervico-incisally from attached gingival up to the middle third of crowns of #23,24,25,26 (Figure 1). On palpation, the growth was non-tender with absence of discharge of pus or blood. Radiographic examination revealed erosive bone changes in the interdental area in relation with #24,25 (Figure 2). After obtaining the written consent from the patient’s parents, an excisional biopsy of the growth was performed under local anesthesia. The growth was enucleated and was sent for histopathological examination (Figures 3 and 4). The histopathology report revealed mass of connective tissue covered partly by parakeratinized stratified squamous epithelium with abundant of fibroblasts, thin collagen fibers, blood capillaries and few inflammatory cells. Also, few irregular calcified masses were appreciated (Figure 5). Correlating the clinical and radiological findings with the histopathological features a final diagnosis of peripherial ossifying fibroma was made.
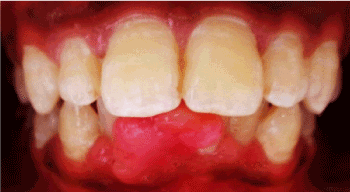
Figure 1. Irregular pale pink growth extending mesiodistally from distal surface of 24 up to the mesial surface of 42 and cervico-incisally from attached gingival up to the middle third of crowns of # 23,24,25,26.
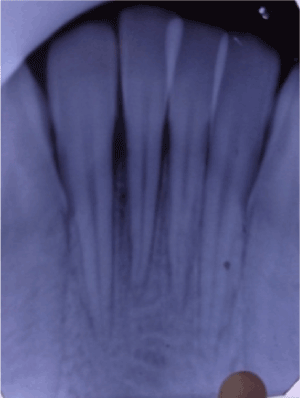
Figure 2. IOPA with mandibular anterior region demonstrating marginal bone loss in relation with 24,25
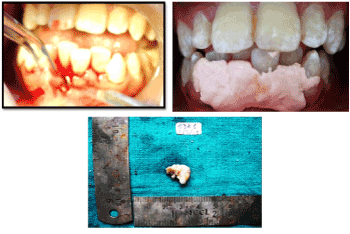
Figure 3. Surgical excision of the growth followed by covering of the surgical site with periodontal pack
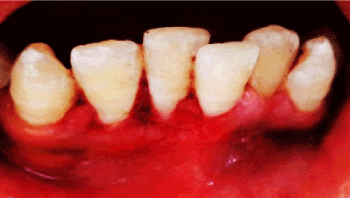
Figure 4. Follow up after 7 days

Figure 5. H&E staining of the excised growth demonstrating abundant fibroblast, thin collagen fibers, blood capillaries, inflammatory cells along with few irregular calcified masses suggestive of peripheral ossifying fibroma
Discussion
Fibromas of the gingiva arise mainly from the connective tissue or the periodontal ligament. Ossifying fibroma is a benign neoplasm which arises mainly in the craniofacial bones, the lesion being well demarcated from the adjacent bone and histologically composed of proliferating fibroblasts along with interspersed bone or calcified masses. Ossifying fibromas can be broadly divided into two types: central and peripheral. The nidus of origin for the central type lies in the endosteum or the periodontal ligament adjacent to the apex of the root which over a period causes the expansion of the medullary space producing the associate extra oral swelling whereas the peripheral type arises in relation to the soft tissues in the tooth-bearing areas of the jaws [3,4].
There exists tremendous controversy related to the nomenclature of POF. Various terms have been used including ossifying fibro-epithelial polyp, peripheral fibroma with calcification, peripheral cemento-ossifying fibroma, peripheral cementifying fibroma, peripheral fibroma with cement genesis, calcifying or ossifying fibrous epulis, peripheral fibroma with osteogenesis and calcifying fibroblastic granuloma to describe POF contributing to extreme confusion. Shepherd (1844) reported POF as “alveolar exostosis”. In 1972, Eversole et al. [5] coined the term POF which is widely used minimizing the problem of misnomer.
Till date the precise etiology of POF is unknown. Various factors have been addressed in literature which are believed to predisposing factors for the development of POF including trauma to gingiva, plaque accumulation, calculus, masticatory forces, ill- fitting appliances, mutilated teeth, poor quality or broken-down restorations and ill-fitting crowns [6].
Likewise, the pathogenesis of POF is not clear. Kumar et al. [7] suggested that POF arises from the periodontal ligament cells as it arises frequently in interdental papilla, its proximity to the gingiva and the periodontal ligament along with the presence of oxytalan fibers within the mineralized matrix of some lesions. It has been postulated that POF develops from the secondary fibrosis of long-standing pyogenic granuloma to which it resembles clinically as well as histopathologically. It may arise following chronic irritation of the periosteal and periodontal membrane causing metaplasia of the connective tissue along with formation of bone or dystrophic calcified masses [8]. Hormonal influences may play an important role, as it has predilection for females particularly in the second decade of life [9]. The rare manifestation of multicentric occurrence points to a role of genetics in the pathogenesis of POF [7].
POF had an incidence in the range of 9–10% [10]. It is more commonly seen in the first and second decade of life and has a female preponderance. The most common location for this lesion is the anterior maxilla (about 60% of cases) with 55–60% presenting in the incisor-cuspid region [11]. However, Kohli et al. [12] have reported a POF associated with an anterior mandibular neonate tooth in a 2-hour-old female, Buchner and Hansen reported a POF in a 7- month-old infant whereas Singh et al. [14] had reported a case of POF in the anterior maxilla in 70-year-old female [13]. In the present case also, it was reported in the mandibular anterior region. Clinically, the POF presented as an exophytic, smooth-surfaced, pink or red nodular mass that was sessile or on occasion on a pedicle. The size of the peripheral ossifying fibroma ranges from: 0.2-3.0 cm [13,15] to 9 cm in diameter [16].
The radiographic features of POF may range from no change to destructive changes depending on the duration of the lesion. In certain cases, superficial erosion of underlying bone, cupping defect and focal areas of radiopaque calcifications at the center of the lesion can be seen [8]. In the present case erosive changes were encountered in relation with tooth no 31, 41.
The differential diagnosis for a localized gingival overgrowth is shown in Table 1 [5,7,11,15,16]. Differential diagnoses should also include neoplastic growths due to the occurrence and similar presentations, though the incidence is rare. Some authors noted that cancer was included in the differential diagnosis in only 2% of cases [11] maintaining a high index of suspicion is important but at the same time discussion with the patient and his family members should prevent undue distress amongst them till a definitive histopathologic diagnosis is established.
Table 1. Differential diagnosis of a localized gingival overgrowth
Lesion |
Clinical features |
Histopathologic features |
Others |
Pyogenic granuloma |
Age-Not definitive
Site-gingiva (most common), lips, tongue, buccal mucosa
Features - usually an elevated pedunculated or sessile, asymptomatic fast growing soft red mass, bleeds easily |
Endothelium lined vascular channels engorged with red blood cells and chronic inflammatory cells |
More in young females, often associated with pregnancy |
Peripheral giant cell granuloma |
Age- 4th to 6th decade
Site - Exclusively on gingiva, mostly anterior to molars
Features- Purple or reddish purple in colour rapidly growing soft or firm mass which may be sessile or pedunculated. usually 0.5-1.5 cm in size and shows surface ulceration. |
Large number of multinucleated giant cells in vascularized fibro cellular stroma with inflammatory cell infiltration. |
‘Cupping’ resorption of the underlying alveolar bone seen in radiograph |
Peripheral ossifying fibroma |
Age-10-19 years
Site- Exclusively on gingiva
Features - Firm, pedunculated mass, colour same as surrounding mucosa |
Cellular fibrous connective tissue containing numerous calcified deposits Minimal vascular component. |
No bone involvement on radiograph, on rare occasions superficial erosion of bone seen |
Irritation fibroma |
Age – Not definitive
Site – mostly buccal mucosa, lips, gingiva
Features - Round to ovoid, asymptomatic, smooth, pink, firm, sessile or pedunculated mass |
Atrophic epithelium with dense collagenous matrix containing few fibroblasts and little or no inflammatory response. |
Most common |
Peripheral odontogenic fibroma |
Age-5-65 years
Site - gingiva
Features - Slow growing solid, firmly attached gingival mass sometimes arising between teeth and sometimes even displacing teeth. |
Islands of Odontogenic epithelium seen |
Soft tissue counterpart of central odontogenic fibroma
Uncommon |
Metastatic cancer |
Age -Not definitive
Site- gingiva (commonly)
Features- Swelling, destruction of underlying bone, loosening of teeth, paresthesia. Can be asymptomatic |
Will resemble tumor of origin |
Uncommon
Can mimic gingival reactive lesions |
Histopathology provides the confirmatory diagnosis with the identification of fibrous connective tissue and the focal presence of bone or other calcifications as was seen in this case. Three kinds of mineralized tissues can be seen in this lesion:
- Bone that may be woven or lamellar bone sometimes surrounded by osteoid, or in trabecular form;
- Cementum-like material that appears as spherical bodies resembling cementum or large acellular round-to-oval eosinophilic bodies;
- Dystrophic calcifications, which can range from small clusters of minute basophilic granules or tiny globules to large, solid irregular masses [15,16].
It is important to remove the lesion completely by including subjacent periosteum and periodontal ligament, besides the possible causes, to reduce recurrence. Thorough root scaling of adjacent teeth and/or removal of other sources of irritation should be accomplished. Tooth extraction is seldom necessary [7,15,16]. soft tissue lasers can also be used as the lasers have the advantage of providing a dry and bloodless surgery, reduced bacteremia at the surgical site, reduced mechanical trauma with resultant lessened psychological trauma for the patient, minimal scarring. Iyer et al. [17] recently reported a case of successful laser excision of POF with very little intraoperative bleeding, post‑operative pain, and suture less exercise, and excellent healing at the end of one week, suggesting that laser excision as one of the best options for management of POF.
The rate of recurrence has been reported to vary from 8.9% to 20 [3,9]. It probably occurs due to incomplete initial removal, repeated injury or persistence of local irritants. The average time interval for the first recurrence is 12 months [15,18].
Conclusion
Peripheral ossifying fibroma is a slowly progressing reactive lesion requiring complete removal of the lesions down to the periosteum and periodontal ligament along with regular post excision follow-ups to minimize the possible chances of recurrence.
References
- Buduneli E, Buduneli N, Unal T (2001) Long-term follow-up of peripheral ossifying fibroma: report of three cases. Periodontal Clin Investig 23: 11-14. [Crossref]
- Neville BW, Damm DD, Allen CM, Bouquot JE (1995) Oral and Maxillofacial Pathology. Philadelphia: WB Saunders Co: 374-376.
- Bhaskar SN, Jacoway JR (1966) Peripheral fibroma and peripheral fibroma with calcification: report of 376 cases. J Am Dent Assoc 73: 1312-1320. [Crossref]
- Keluskar V, Byakodi R, Shah N (2008) Peripheral ossifying fibroma. J Indian Acad Oral Med Radiol 20: 54-56. [Crossref]
- Eversole LR, Leider AS, Nelson K (1985) Ossifying fibroma: a clinicopathologic study of sixty-four cases. Oral Surg Oral Med Oral Pathol 60: 505-511. [Crossref]
- Gardner DG (1982) T2021 Copyright OAT. All rights reserv attempt at clarification. Oral Surg Oral Med Oral Pathol 54: 40-48. [Crossref]
- Kumar SK, Ram S, Jorgensen MG, Shuler CF, Sedghizadeh PP (2006) Multicentric peripheral ossifying fibroma. J Oral Sci 48: 239-243. [Crossref]
- Kendrick F, Waggoner WF (1996) Managing a peripheral ossifying fibroma. ASDC J Dent Child 63: 135-138. [Crossref]
- Kenney JN, Kaugars GE, Abbey LM (1989) Comparison between the peripheral ossifying fibroma and peripheral odontogenic fibroma. J Oral Maxillofac Surg 47: 378-382. [Crossref]
- Layfield LL, Shopper TP, Weir JC (1995) A diagnostic survey of biopsied gingival lesions. J Dent Hyg 69: 175-179. [Crossref]
- Zhang W, Chen Y, An Z, Geng N, Bao D (2007) Reactive gingival lesions: a retrospective study of 2,439 cases. Quintessence Int 38: 103-110. [Crossref]
- Kohli K, Christian A, Howell R (1998) Peripheral ossifying fibroma associated with a neonate tooth: case report. Pediatr Dent 20: 428-429. [Crossref]
- Buchner A, Hansen LS (1987) The histomorphologic spectrum of peripheral ossifying fibroma. Oral Surg Oral Med Oral Pathol 63:452-461. [Crossref]
- Singh AP, Raju MS, Mittal M (2010) Peripheral ossifying Fibroma: A case report. J Nebr Dent Assoc 1: 70-72.
- Cuisia ZE, Brannon RB (2001) Peripheral ossifying fibroma- a clinical evaluation of 134 pediatric cases. Pediatr Dent 23: 245-248. [Crossref]
- Poon CK, Kwan PC, Chao SY (1995) Giant peripheral ossifying fibroma of the maxilla: report of a case. J Oral Maxillofac Surg 53: 695-698. [Crossref]
- Iyer V, Sarkar S, Kailasam S (2012) Use of the ER, CR; YSGG laser in the treatment of peripheral ossifying fibroma. Int J Laser Dent 2: 51-55.
- Das UM, Azher U (2009) Peripheral ossifying fibroma. J Indian Soc Pedod Prev Dent 27: 49-51.





