Key words
Pelvic inflammatory disease, Wait time, Length of stay, Patient satisfaction
Abbreviations
PID: Pelvic Inflammatory Disease; CT: Chlamydia trachomatis; GC: Neisseria gonorrhoeae; STI: Sexually Transmitted Infection; ED: Emergency Department; PED: Pediatric Emergency Department; AED: Adult Emergency Department; WT: Wait time; LOS: Length of stay; SES: Socio-economic Status; TECH-N: Technology Enhanced Community Health Nursing
Introduction
Pelvic inflammatory disease (PID) is a common and serious upper reproductive tract disorder that disproportionately affects young and minority women. PID is associated with considerable longitudinal morbidity including ectopic pregnancy, tubal infertility, and chronic pelvic pain [1-3]. The disease is caused by sexually transmitted infections (STIs) including Chlamydia trachomatis (CT) and/or Neisseria gonorrhoeae (GC), and each episode increases the risk of long-term sequelae, therefore the public health impacts for optimal treatment and patient adherence are significant [4].
The emergency department (ED) commonly serves as the safety net for medical care for patients from low socioeconomic status backgrounds. Urban, minority adolescents and young adults often assume great responsibility for health care decision-making and self-management and the ED provides an immediate response to a perceived health threat or when patients have difficulty accessing other systems of care [5]. Local and national data show widespread ED use among adolescent and young women who require treatment for PID [6]. Several studies have demonstrated poor adherence to the CDC guidance on treatment of PID by ED providers, which may influence both patient satisfaction and longitudinal reproductive health outcomes [6,7].
Minority youth have low rates of medication adherence for a range of major health care problems, including asthma and PID [7-10]. Factors associated with non-adherence include health-care system/team factors, patient-related factors, therapy-related factors, condition related factors, social and economic factors [11]. Poor medication adherence, low socioeconomic status (SES) and low environmental supports among individuals transitioning towards autonomy may coalesce in the ED setting and compound problems with self-management resulting in adverse health outcomes making the experience of the ED visit extremely important.
One of the most significant issues impacting the experience of patients seeking care in ED settings is time, both wait time (WT) to see a provider and total length of stay (LOS) [12,13]. Patients using large academic centers are often seen by individuals in training; the process of trainee supervision may create further delays or otherwise influence the patient experience. Patient satisfaction is an important indicator of quality of medical care, and low satisfaction has been hypothesized to lead to adverse health behaviors and medication adherence [14,15]. This concern is particularly relevant to groups of patients that may mistrust the medical establishment, such as adolescents or disadvantaged minority populations. While there are a handful of studies assessing patient satisfaction and outcomes related to psychiatric care, no studies to date have addressed the potential relationship between patient satisfaction with care of acute medical conditions, such as PID [16,17]. The purpose of this study is to examine the relationship between WT, LOS and primary provider level of training on patient satisfaction and medication adherence among urban adolescents and young adults with PID.
Materials and methods
Study design
We evaluated data from the Technology Enhanced Community Health Nursing (TECH-N) study, a large randomized controlled trial of an intervention designed to improve self-management and prevent recurrent sexually transmitted infections in the outpatient setting (NCT01640379). The Johns Hopkins Medicine Institutional Review Board (IRB) approved this study. No ethical committee approval was necessary. Written informed consent was obtained from all participants.
Study setting and population
Eligible patients for enrollment in TECH-N trial were females ages 13-25 years old seen in one of three clinical and ambulatory settings of a large urban tertiary care medical center including (1) the pediatric and adolescent ambulatory care clinic, (2) the Pediatric Emergency Department (PED) and (3) Adult Emergency Department (AED). The inclusion criteria for the parent study include mild-moderate PID, disposition to outpatient treatment, living in the Baltimore metropolitan area and willingness to be randomized. Subjects were excluded from the trial if PID was diagnosed in the setting of pregnancy or concurrent diagnosis of sexual assault. Study recruitment occurred between August 2012 and November 2016.
All participants completed a baseline audio computerized assisted self-interview (ACASI) at the time of the ED visit and. also completed a face-to-face interview and ACASI at 30 and 90 days. Prior to leaving the enrolment site at baseline, all participants were provided a 14-day course of oral antibiotics dispensed by the health provider. All participants underwent a 2-week follow-up visit from an outreach worker, which included measures of medication adherence and patient satisfaction. Intervention participants received text-messaging reminders to promote medication adherence and a 3-5 day follow-up visit by a community health nurse. Participants randomized to the control group received standard care and were expected to self-manage PID and arrange follow-up care per the CDC guidelines. Participants received $10 remuneration for each interview and for each biological sample provided during the study. No remuneration was provided during the nurse intervention visit as visit completion was a study outcome.
Study protocol
For this analysis, we focused on ED care and only included patients who were enrolled from the PED and AED. We also only included the standard of care control group patients, given the potential relationship between study procedures and the outcomes of interest. We collected data from the electronic medical record including WT (time between registration and start of visit with a clinician), LOS (start of visit with clinician to disposition), provider level of training (faculty/mid-level provider versus trainee), location of service (AED or PED) and demographic data (age, insurance type) and matched to data from the 2-week outreach interview during which participants were queried about satisfaction with care and medication adherence.
Measurements
Self-reported medication adherence during the two-week antibiotic treatment period was measured using the item, “Did you take all of the medications given to you at the hospital?” The measurement was yes or no and dichotomously coded (1 or 0). Only a few participants presented a prescription bottle for pill counts by the outreach worker. Patient satisfaction was measured by the patient report at the 2-week outreach study visit, using the item, “Are you satisfied with the care you received?” This measurement was yes or no and dichotomously coded (1 or 0).
Data analysis
Descriptive statistics for demographic and health information were examined for the entire cohort, including patient age, type of insurance, location of service (PED or AED), WT, LOS, provider level of training. We separated the cohort into dichotomous groups based on location of service (AED or PED) and compared means for WT and LOS by t-test statistic. We further divided the cohort into those with above mean wait time or below mean wait time, and above mean LOS or below mean LOS, for their respective locations. Similarly, we divided the cohort into dichotomous groups based on provider type and compared means for WT and LOS by t-test statistic. Chi-square testing was used to evaluate the relationship between LOS, WT, satisfaction, and medication adherence. Logistic regression was then used to analyze the relationship between WT, LOS and medication adherence, making adjustments for age, provider type, and insurance status. Logistic regression was also used to analyze the relationship between provider type and adherence, adjusted for age and insurance. IBM SPSS Statistics 23 (IBM Corp. Released 2015. IBM SPSS Statistics for Windows, Version 23.0. Armonk, NY: IBM Corp) was used for all statistical analyses.
Results
Sample description
During the period of 08/06/2012 – 12/7/2016, 127 women diagnosed with PID were enrolled in the control arm of the TECH-N study. 83 patients were treated in the ED setting and completed the two-week questionnaire. (Figure 1) The majority of patients (71%) were enrolled in the Pediatric ED, while the remainder was enrolled in the Adult ED. Most study participants were low-income African American patients (92%) with a mean age of 19 years (SD = 2.6 years). A trainee physician was the main provider for 42% of participants.
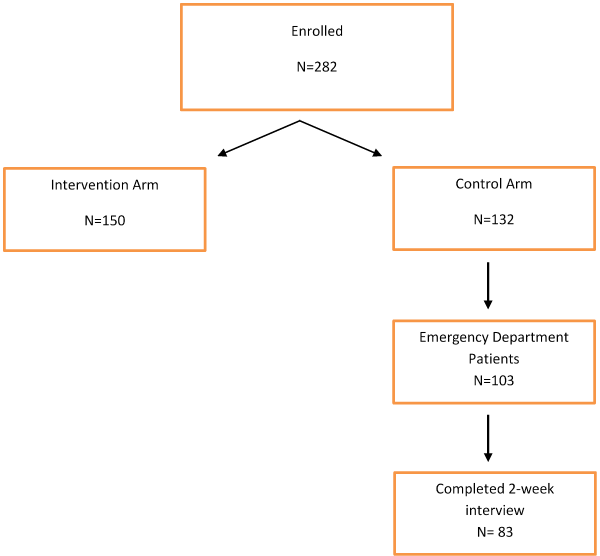
Figure 1. TECH-N Study enrollment flow diagram
The associations between wait time and length of stay, medication adherence and patient satisfaction
Overall, 96% of this cohort reported satisfaction with care, but only 46% reported yes to medication adherence. Mean WT was 55 minutes and mean LOS was 320 minutes (5 hours). LOS differed significantly between the adult ED (AED) and the pediatric ED (PED) sites, so all analyses were repeated with WT and LOS adjusted by site. Mean WT in the PED was 59 minutes while mean WT in the AED was 52 minutes (p=0.1). Mean LOS in the PED was 198 minutes while mean LOS in the AED was 341 minutes (p<0.01). When adjusted by site of care, there was no difference in satisfaction for patients with longer than mean WT (96% for both groups) or LOS (100% vs 93%, chi-square 2.9, p=0.09). Patients with above mean wait time had statistically similar medication adherence to those with shorter than mean wait time (55% vs. 41%, chi-square 0.10, p=0.9). When controlling for age, insurance and provider type, patients with above mean WT did not have significantly lower medication adherence rates than those with shorter than mean WT. (OR 1.47, 95% CI 0.52-4.15, p=0.47). Patients with above mean LOS were initially appeared less adherent with medication than those with below mean LOS, but this was not statistically significant (51% vs. 40%, chi-square 0.97, p =0.3). When controlling for age, insurance and provider type, patients with longer than mean LOS were not less likely to report medication adherence (OR 0.49, 95% CI 0.17-1.45, p=0.19).
The associations between impact of training level and wait time, length of stay and medication adherence
Patients seen by a trainee physician were far more likely to have a longer than average, site-adjusted LOS compared to those seen by an independent provider (OR 4.2, 95% CI: 1.6-10.6). WT did not differ (58 min vs. 52 min, p=0.7), but total LOS was significantly longer for those patients seen by a trainee physician (342 min vs. 249 min, p<0.01). There was a statistically significant difference in patient satisfaction by provider level of training, with patients seen by trainees being less satisfied (100% vs. 91%, p=0.04). Provider type was not associated with medication adherence in logistic regression, when adjusted for age and insurance status. (OR 2.14, 95% CI: 0.9-5.3).
Discussion
This study is the first to investigate the relationship between patient satisfaction and adherence to medication in the context of emergency department care. The urban, minority adolescent and young adult patients in this study are highly satisfied with PID treatment services delivered in emergency department settings despite long WT and LOS.
Adolescent and young adult patients often seek care for reproductive health in emergency department settings. The benefit of convenience appears to outweigh the downside of waiting time. The timing of care seeking is one potential reason for the choice of ED care [18]. Several innovative attempts have been made to change ED workflows to decrease WT and LOS. Such novel approaches include a priority admission triage (PAT) program, structured re-design process, improved communication with the medical department, “Emergency Journey Coordinators” and the use of laboratory testing to determine acuity [19,20]. With time, lean management techniques may improve patient flow and decrease LOS in the ED.
Wait time and efficiency of ED care (LOS) for STI may be negatively impacted if STI care is perceived as low-acuity or less desirable by the ED staff. Acuity based triage models lead to longer wait times for low acuity level patients. The widely used Emergency Severity Index triage model, which assigns triage level by number of resources required, does not count pelvic exam as an additional resource [21]. In the study institution, a majority of patients with suspected STI or PID will be triaged as level 4, or low acuity, and will wait for room availability after the higher acuity patients.
Strengths and limitations
The study has several strengths. We successfully enrolled patients from a vulnerable population and successfully followed them longitudinally over the two-week treatment period with an 80 % follow up rate. These adolescent and young adult low SES patients are historically less likely to complete satisfaction surveys [22-24].
The findings from this study must be considered in light of several general limitations. The study was conducted at a single academic center serving a largely low-income minority population; therefore, the results may not be generalizable. Even so, the youth in this community face significant health disparities associated with sexually transmitted infection so they are an important focus of study. The sample was limited to recruitment hours of the study; however, study team members were available from 11am to 11pm 7 days each week. We assessed the patients diagnosed with PID during non-enrolling hours and found the basic demographics (age, race, insurance status) were consistent with those recruited. Finally, control arm participants were incentivized to enroll in the trial and also interacted with TECH-N staff during their clinical visit. If control patients considered the TECH-N team an extension of the clinical care team, we must be careful in our interpretation of the satisfaction data. Finally, self-report was used to assess medication adherence due to low availability of pill counts at the 2-week outreach research visit and satisfaction was measured two weeks after the index visit. Our data suggest that patients were reflective about their treatment behaviors and two weeks is within the range of follow-up for other satisfaction and quality assessment questionnaires after receipt of care.
Conclusions
Patient satisfaction and the context of care may directly influence patient behaviors and longitudinal outcomes. Additional research exploring novel emergency department workflow strategies and triage systems for patients seeking care for PID may result in shorter visits of better or equal quality for improved clinical outcomes.
Funding acknowledgement
The TECH-N study, including support for all co-authors, is funded by the National Institutes of Health, National Institute of Nursing Research, Grant # R01NR013507.
Declaration of conflicting interests
The authors declare that there are no conflicts of interest.
References
- Westrom L (1995) Effect of pelvic inflammatory disease on fertility. Venereology 8: 219-222. [Crossref]
- Weström L (1987) Pelvic inflammatory disease: bacteriology and sequelae. Contraception 36: 111-128. [Crossref]
- Trent M, Haggerty CL, Jennings JM, Lee S, Bass DC, et al. (2011) Adverse adolescent reproductive health outcomes after pelvic inflammatory disease. Arch Pediatr Adolesc Med. 165: 49-54. [Crossref]
- Centers for Disease Control and Prevention (2010) Pelvic Inflammatory Disease. Sexually Transmitted Diseases Treatment Guidelines. Available at: http://www.cdc.gov/std/treatment/2010/pid.htm. Accessed April 17, 2015.
- Kangovi S, Barg FK, Carter T, Long JA, Shannon R, et al. (2013) Understanding why patients of low socioeconomic status prefer hospitals over ambulatory care. Health Aff (Millwood) 32: 1196-1203. [Crossref]
- Goyal M, Hersh A, Luan X, Localio R, Trent M, et al. (2013) National trends in pelvic inflammatory disease among adolescents in the emergency department. J Adolesc Health. 53: 249-52. [Crossref]
- Trent M, Judy SL, Ellen JM, Walker A (2006) Use of an institutional intervention to improve quality of care for adolescents treated in pediatric ambulatory settings for pelvic inflammatory disease. J Adolesc Health. 39: 50-56. [Crossref]
- Mosnaim G, Li H, Martin M, Richardson D, Belice PJ, et al. (2014) Factors associated with levels of adherence to inhaled corticosteroids in minority adolescents with asthma. Ann Allergy Asthma Immunol. 112: 116-120. [Crossref]
- Lawson CC, Carroll K, Gonzalez R, Priolo C, Apter AJ, et al. (2014) "No other choice": reasons for emergency department utilization among urban adults with acute asthma. Acad Emerg Med. 21: 1-8. [Crossref]
- Dunbar-Jacob J, Sereika SM, Foley SM, Bass DC, Ness RB (2004) Adherence to oral therapies in pelvic inflammatory disease. J Womens Health (Larchmt) 13: 285-291. [Crossref]
- Medication Adherence. CDC’s Noon Conference. Available at: http://www.cdc.gov/primarycare/materials/medication/docs/medication-adherence-01ccd. Accessed April 16, 2015.
- Bleustein C, Rothschild DB, Valen A, Valatis E, Schweitzer L, et al. (2014) Wait times, patient satisfaction scores, and the perception of care. Am J Manag Care 20: 393-400. [Crossref]
- Sayah A, Rogers L, Devarajan K, Kingsley-rocker L, Lobon LF (2014) Minimizing ED Waiting Times and Improving Patient Flow and Experience of Care. Emerg Med Int. 2014: 981472.
- Mohamed B, Azizan NA (2015) Perceived service quality's effect on patient satisfaction and behavioural compliance. Int J Health Care Qual Assur 28: 300-314. [Crossref]
- Farley H, Enguidanos ER, Coletti CM, Honigman L, Mazzeo A, et al. (2014) Patient satisfaction surveys and quality of care: an information paper. Ann Emerg Med 64: 351-357. [Crossref]
- Biering P, Jensen VH (2010) The concept of patient satisfaction in adolescent psychiatric care: a qualitative study. J Child Adolesc Psychiatr Nurs. 23: 143-50. [Crossref]
- Biering P (2010) Child and adolescent experience of and satisfaction with psychiatric care: a critical review of the research literature. J Psychiatr Ment Health Nurs 17: 65-72. [Crossref]
- Jemmott LS, Jemmott JB, O'leary A (2007) Effects on sexual risk behavior and STD rate of brief HIV/STD prevention interventions for African American women in primary care settings. Am J Public Health. 97: 1034-1040. [Crossref]
- Webster F, Rice K, Dainty KN, Zwarenstein M, Durant S, et al. (2015) Failure to cope: the hidden curriculum of emergency department wait times and the implications for clinical training. Acad Med. 90: 56-62. [Crossref]
- Chan H, Lo S, Lee L, Lo W, Yu W, et al. (2014) Lean techniques for the improvement of patients' flow in emergency department. World J Emerg Med 5: 24-28. [Crossref]
- Asha SE, Ajami A (2014) Improvement in emergency department length of stay using a nurse-led 'emergency journey coordinator': a before/after study. Emerg Med Australas. 26: 158-163. [Crossref]
- Shefrin AE, Milner R, Goldman RD (2012) Adolescent satisfaction in an urban pediatric emergency department. Pediatr Emerg Care. 28: 63363-9. [Crossref]
- Rutherford KA, Pitetti RD, Zuckerbraun NS, Smola S, Gold MA (2010) Adolescents' perceptions of interpersonal communication, respect, and concern for privacy in an urban tertiary-care pediatric emergency department. Pediatr Emerg Care. 26: 257-273. [Crossref]
- Shreffler KM, McQui2021 Copyright OAT. All rights reserv (2009) Odds of having a regular physician and perceptions of care: ethnic patterns for women ages 25-45. Fam Med 41: 271-276. [Crossref]

