A 35-year-old G3P2002 at 39 weeks’ gestation presents to labor and delivery (L&D) with uterine contractions, and is found to be in active labor with the fetus in head presentation. She has had a complicated antepartum course with a non-good prenatal care including lack of one anatomy scan in the second trimester. Her prior infants, each weighing approximately 3200 g, were delivered vaginally without complications. Ultrasound evaluation upon presentation to L&D confirms that the infant is in head presentation; the estimated fetal weight (EFW) is 3400 g. Clinical assessment of the maternal pelvis are determined to be adequate for a fetus of this estimated weight. The cervix is 5 cm dilated, 100% effaced and the fetal head is at zero station. After five hours, the patient with vaginal delivery gave birth to a male baby with body weight 3450 g and Apgar score 7/8. The infant had a bilateral cleft lip and palate (figure 1), became a karyotype that resulted with an extra copy of chromosome 13. The patient was informed in detail, as well as receiving appropriate advice and recommendation.
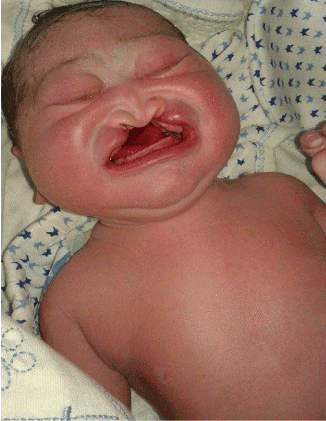
Figure 1. Patau syndrome. Bilateral cleft lip and palate
Trisomy 13 or Patau syndrome in 1960, was described as one genetic disorder in which a person has an extra copy of chromosome 13 (or 3 copies of genetic material from chromosome 13, instead of the usual 2 copies). Trisomy 13 occurs in about 1 out of every 12,500 newborns [1,2,3,4,5]. Patau syndrome can be caused by free trisomy of chromosome 13 (75% of cases), and trisomy from Robertsonian translocations (25% of cases). Prenatal diagnosis is feasible by G-banding of chromosomes from chorionic villi, amniocytes, and peripheral leukocytes, while ultrasound screening can reveal an enlarged nuchal translucency at 12–14 weeks of gestation, and a wide spectrum of major anomalies that can be associated with trisomy 13 such as; CNS anomalies (45%–55%): holoprosencephaly, agenesis of the corpus callosum, and cerebellar malformations., Craniofacial anomalies (80%): bilateral cleft lip and palate, micro and anophthalmia, and micrognathia., Congenital heart disease (40%–50%):septation defects and absent pulmonary venous return., Urinary tract anomalies (30%–35%): cystic renal dysplasia., Skeletal anomalies (20%–30%): postaxial polydactyly and clenched hands [6]., Abdominal wall anomalies (30%): exomphalos etc. Trisomy 13 or Patau syndrome is a lethal condition in most cases, and 95% of the survivors die within 6 months. Very rare cases without severe malformations have survived for several years. With epilepsy, severe psychomotor delay and blindness can also be associated.
- Irving C, Richmond S, Wren C, Longster C, Embleton ND (2011) Changes in fetal prevalence and outcome for trisomies 13 and 18: a population-based study over 23 years. J Matern Fetal Neonatal Med 24: 137-141. [Crossref]
- Parker SE, Mai CT, Canfield MA, Rickard R, Wang Y, et al. (2010). Updated national birth prevalence estimates for selected birth defects in the United States, 2004–2006. Birth Defects Res A Clin Mol Teratol 88: 1008-1016. [Crossref]
- Savva GM, Walker K, Morris JK. (2010). The maternal age‐specific live birth prevalence of trisomies 13 and 18 compared to trisomy 21 (Down syndrome). Prenat Diagn 30: 5764. [Crossref]
- Vendola C, Canfield M, Daiger SP, Gambello M, Hashmi SS, et al. (2010). Survival of Texas infants born with trisomies 21, 18, and 13. Am J Med Genet A 152: 360-366. [Crossref]
- Crider KS, Olney RS, Cragan JD (2008). Trisomies 13 and 18: population prevalences, characteristics, and prenatal diagnosis, metropolitan Atlanta, 1994–2003. Am J Med Genet A 146: 820-826. [Crossref]
- Paladini D, Greco E, Sglavo G, D'Armiento MR, Penner I, et al. (2010). Congenital anomalies of upper extremities: prenatal ultrasound diagnosis, significance, and outcome. Am J Obstet Gynecol 202: 596-e1. [Crossref]
Article Type
Case Report
2021 Copyright OAT. All rights reserv
Publication history
Received date: October 16, 2017
Accepted date: October 31, 2017
Published date: November 03, 2017
Copyright
©2017 Gashi AM. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Citation
Gashi AM (2017) Patau Syndrome - A case later diagnosed. J Pregnancy Reprod 1: DOI: 10.15761/JPR.1000120
Corresponding author
Astrit M. Gashi, MD
University Clinical Centre of Kosovo, Pristine, Tel;+37744266902;
E-mail : bhuvaneswari.bibleraaj@uhsm.nhs.uk

