Abstract
Surgical treatment of proximal patellar tendinopathy/Jumper´s knee is known to be difficult, and occasionally partial tendon ruptures complicates the treatment.
Objectives: To prospectively in a case series of patients operated for chronic painful patellar tendinopathy evaluate the incidence of partial ruptures, and the occurrence of patellar bone pathology in relation to the rupture site.
Material and Methods: Fifty-seven consecutive patients (53 males and 4 females) with a mean age of 24 years (range 17-47), and a long duration (> 5 months) of pain symptoms from proximal patellar tendinopathy, were included. All had failed conservative management, including loading regimens. For pre-operative evaluation: clinical examination, US+DP examination, and the VISA-P score (function) was used. Per-operative evaluation: findings during arthroscopic treatment. In all patient ultrasound (US)+Doppler (DP) examination verified the diagnosis. All were treated with the US-guided arthroscopic shaving method, followed by a specific rehabilitation program.
Results: Before surgery, the mean VISA-P functional score was 32 (range 15-77). In 23/57 tendons (40%) there was a partial rupture, and in all these 23 tendons there was prominent bone (spur, sharp edge) in close relation to the partial rupture. In 16/23 tendons with a partial rupture the pre-op US examination showed signs of a partial rupture together with prominent bone in the patellar tip, and in 7/23 only prominent bone was noticed. The preoperative VISA-P score for the 23 tendons with a partial rupture did not significantly differ from the VISA-P score in the tendons without a partial rupture.
Conclusions: In consecutive patients operated for patellar tendinopathy with the US-guided arthroscopic shaving procedure, partial ruptures were found in 40% of the tendons, and prominent bone was found in close relation to the rupture site. Prominent bone in the patellar tip found during the pre-operative US examination indicates a partial rupture in the tendon.
Introduction
Patellar tendinopathy is a relatively common overuse condition especially among athletes involved in leg explosive sports, and it is a condition known to be difficult to treat [1-3]. Conservative management focusing on different types of loading regimens is first line treatment [4,5]. In a sub-group of patients loading regimens are not enough to lower or cure the pain to allow for full training and sports activity, and these cases are treated surgically. The golden standard method for surgical treatment has been tenotomy and intra-tendinous revision of tendinopathic tissue, however, the results have been shown to be varying and the method is questioned [5]. A new surgical treatment method guided by ultrasound, ultrasound (US)+Doppler (DP)-guided arthroscopic shaving [6,7], has been shown to give good and stable clinical results in mid-term follow-ups [8].
In a sub-group of patients operated with the US+DP-guided arthroscopic shaving method, partial ruptures have been identified. This study aimed to evaluate the number of partial ruptures and their possible relationship with prominent bone (spurs, sharp edges) in the patellar tip, in consecutive operations performed by the same surgeon.
Material and Methods
Consecutive patients seeking help for chronic painful patellar tendinopathy between 2016 and 2018, were included. There were 57 patients, 53 males and 4 females (mean age 24 years, range 17-47) with a long duration (mean 16 months, range 5-48) of pain symptoms. All had failed traditional conservative management, including specific loading regimens. The patients were high level athletes, many were professionals, in different sports such as; Soccer (n=22), Gaelic football and Hurling (n=8), Rugby (n=5), Handboll (n=5), Alpine and Free Skiing (n=5), Ice hockey (n=4), Fitness (n=2), Gymnastics (n=1), Triatlon (n=1), Floorball (n=1), Basketball (n=1), Taekwondo (n=1), and Long distance running (n=1).
Previous conservative management included loading regimens (n=57), cortisone injection (n=10), PRP injection (n=11), high volume injection of local anaesthesia alone (n=3), sclerosing polidocanol injection (n=3).
All patients were clinically and with US+DP diagnosed to have patellar tendinopathy in the proximal part of the patellar tendon. US+DP showed a thickened proximal patellar tendon with irregular structure mainly dorsal and central in the tendon, including hypo-echoic regions and high blood flow coming from the dorsal soft tissues and going into the tendon.
Surgical treatment
The surgical treatment [6,7] was performed in local anaesthesia.
The patients were in a supine position with straight knee and relaxed quadriceps. We used standard antero-medial and antero-lateral portals, and a pressure-controlled pump. No tourniquet was used. US was used per-operatively. A standard arthroscopical evaluation of the whole knee joint was performed. Then the patellar tendon insertion into the patella was identified, and a 4.5 mm full radius blade shaver was introduced. Simultaneous ultrasound examination (longitudinal and transversal views) guided the procedure. Careful shaving, aiming to destroy only the region with high blood flow and nerves adjacent to the tendinosis changes on the dorsal side of the tendon (separating the Hoffa fat pad from the patellar tendon), was done. In cases with a bone spur or sharp edge on the patellar tip (Figure 1 and 2), careful removal with the shaver was performed. In such cases it was necessary to also remove some tendinosis tissue to reach the sharp bone, but emphasis was put on preserving tendon tissue. In cases with a partial tendon rupture (Figure 2) the rupture was debrided until fresh borders, using the shaver. The portals were sutured, and 20 ml of Chirocain was injected into the joint.
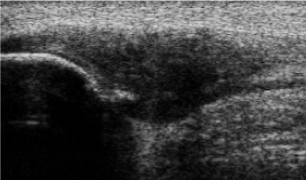
Figure 1. Grey scale ultrasound examination-longitudinal view. A sharp bone spur is seen in the patellar tip in a patient with a thickened proximal patellar tendon-proximal patellar tendinopathy
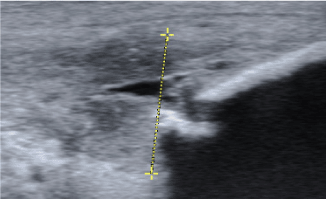
Figure 2. Grey scale ultrasound examination-longitudinal view. A sharp bone spur is seen in the patellar tip in a patient with a thickened proximal patellar tendon-proximal patellar tendinopathy
There was bandage from toes to above the knee.
After surgery the patients were resting overnight, allowed partial weight bearing, and seen for a follow-up visit the day after the operation. If the knee joint was swollen, evacuation was performed under strict sterile conditions. An ultrasound examination was done using sterile gel, and if everything looked fine rehabilitation according to a specific plan was started.
Below find the general guidelines for the rehabilitation program. There is sometimes need for an individual variation of the program.
Week 1-2: Full weight-bearing walking, ROM exercises and quadriceps contraction exercises. Light biking.
Week 3-4: Increased walking and biking. Introduction of closed chain strength training (low load and multiple repetitions).
Week 5-8: Heavier biking High resistance intervals) and strength training. No plyometric exercises until tolerate isometric, concentric and eccentric strength training.
Week 9-forward: Introduce more sport specific exercises.
If there is a partial tendon rupture the rehabilitation program is lengthened with 4 weeks. The program for week 1-2 is then used for 4 weeks.
Results
All patients had tenderness in the proximal patellar tendon and the mean VISA-P functional score was 32 (range 15-77) before surgery.
In 16/23 tendons with a partial rupture diagnosed during surgery the pre-op US examination showed signs of a partial tendon rupture together with prominent bone (spur, sharp edge) in the patellar tip.
In 7/23 tendons with a partial rupture diagnosed during surgery the pre-op US examination showed prominent bone in the patellar tip alone.
The pre-operative VISA-P score for the 23 tendons with a partial rupture did not significantly differ from the VISA-P score in the tendons without a partial rupture.
There were no complications in relation to the operations.
Discussion
In this observational study on consequtive patients operated for proximal patellar tendinopathy with the US-guided arthroscopic shaving procedure [6-9], we found partial ruptures in 23/57 (40%) tendons. In all cases with a partial rupture prominent bone from the patellar tip was found in close relation to the rupture site.
The number of partial tendon ruptures in patellar tendinopathy patients in this study is high compared to most other studies that have been reporting few, if any partial ruptures [5-8]. Karlsson, et al. [10] reported multiple partial patellar tendon ruptures, but in that study a partial rupture was defined based on ultrasound findings, where the findings of a hypo-echoic region in the tendon was interpreted as a partial tendon rupture. There was no verification during surgery. This is likely misleading because the ultrasound finding of a hypo-echoic region in a tendon represents only a fluid rich region, fluid not seldom covering under laying intact tendon tissue, such as in tendinopathy. Consequently, in that material [10], the diagnosis partial rupture was not macroscopically verified, and unfortunately, there is no information about bone pathology in the patellar tip.
The relatively high numbers of partial ruptures in our material is likely not representative for the traditional patient with patellar tendinopathy. The reason for this is that the patients in our study represent so called “difficult cases”, and second opinion cases, sent for evaluation by this surgeon that is specialised on treatment of tendinopathy. Anyhow, it seems of importance to provide more knowledge about this condition that is well known to be difficult to treat. There seem to be a wide span of patients, from having only tendinopathy to having tendinopathy plus partial rupture and bone pathology.
In this material, ultrasound examination was a good method to find bone spurs and sharp bone edges in the patellar tip, and such bone findings were related to partial tendon ruptures. Consequently, if there is bone pathology in the patellar tip on the pre-operative US examination, it seems that there is likely a partial tendon rupture. This is important information for the surgeon, that strengthens the indication to carefully explore the tendon especially in relation to the prominent bone. It can possibly be argued if it is of importance to find a partial rupture in a tendinopathic tendon? In our opinion, partial ruptures most often cause pain. We are performing these operations in local anaesthesia, and when we identify a partial rupture after having removed the fat tissue on the deep side [9], and occasionally some tendinopathic tissue on the deep side of the tendon, touching the tissue in the region for the partial rupture cause sharp pain. Then to continue, we need to add local anestesia in the region for the partial rupture. After adding local anaesthesia we can debride the partial rupture until fresh borders without causing pain. Altogether, this clearly indicate that the partial rupture is causing pain, and it seems appropriate to try to relief this pain by surgical revision using the shaver.
The background to partial tendon ruptures in this material is not clear. All patients had a gradual onset of pain, indicating that the partial ruptures were not caused by a sudden overloading of the tendon. Because we have no information about the existence of bone spurs or sharp edges in the patellar tip before the evolution of tendon pain, we cannot state that the tendinopathy and partial ruptures were caused by the sharp bone in the patellar tip. Interestingly, a long patellar tip has been suggested to be involved in patellar tendinopathy [11]. Also, theoretically the sharp bone in the patellar tip might be bone formation as a result of different loadings on the bony tendon insertion caused by the thickened patellar tendon? It was interesting to notice that in this material in 16/23 patients with a partial rupture treatment with intra-tendinous injections had been used. Injection into a tendon might damage the tendon, from the injected volume that cause increased intra-tendinous pressure, and possibly also from the substances injected.
The surgical procedure is performed with US-guidance, and after the traditional careful shaving aiming to destroy only the region with high blood flow and nerves adjacent to the tendinosis changes on the dorsal side of the tendon (separating the Hoffa fat pad from the patellar tendon), the patellar tip is inspected. If there is sharp bone it is carefully shaved away until smooth underlaying bone surface. Then if there is a partial rupture it is shaved out to normal borders. We haven´t had any complications with this procedure. Occasionally there is some hemarthrosis after surgery, and evacuation at the day 1 follow-up is sometimes needed for the patient to be able to comfortable start to load with full weight bearing walking. For patients having a partial tendon rupture, we use a careful rehabilitation allowing only ROM exercises, walking, and light biking, the first 4 weeks after surgery. Apart from the 4 weeks longer rehabilitation period, there is no difference in the rehabilitation program compared to patients treated for tendinopathy alone. We have not seen any differences in the outcomes after surgery between patients having partial ruptures and bone prominences, and the patients having only tendinopathy changes.
It appears of importance to identify the patients that have a partial rupture and sharp bone in the patellar tip at an early stage, because there is likely a risk that a sharp bone spur in the patella can harm the tendon during certain loading situations. Even certain rehabilitation exercises might, potentially, harm the tendon. However, this needs to be evaluated in further studies.
In conclusion, partial tendon ruptures can be found together with tendinopathy in the proximal patellar tendon, and in this case series of consecutive patients operated for patellar tendinopathy with the US-guided arthroscopic shaving procedure, for all partial ruptures prominent bone was found in close relation to the rupture site. Prominent bone in the patellar tip found during the pre-operative US examination seem to indicate a partial rupture in the tendon.
References
- Khan KM, Maffulli N, Coleman BD, Cook JL, Taunton JE (1998) Patellar tendinopathy: some aspects of basic science and clinical management. Br J Sports Med 32: 346-355. [Crossref]
- Lian OB, Engebretsen L (2005) Bahr R. Prevalence of jumper's knee among elite athletes from different sports: A cross-sectional study. Am J Sports Med 33: 561–567.
- Kettunen JA, Kvist M, Alanen E, Kujala UM (2002) Long-term prognosis for jumper's knee in male athletes. A prospective follow-up study. Am J Sports Med 30: 689-692. [Crossref]
- Cook JL, Khan KM (2001) What is the most appropriate treatment for patellar tendinopathy? Br J Sports Med 35: 291-294. [Crossref]
- Bahr R, Fossan B, Løken S, Engebretsen L (2006) Surgical treatment compared with eccentric training for patellar tendinopathy (Jumper's Knee). A randomized, controlled trial. J Bone Joint Surg Am 88: 1689-1698. [Crossref]
- Willberg L, Sunding K, Ohberg L, Forssblad M, Alfredson H (2007) Treatment of Jumper's knee: promising short-term results in a pilot study using a new arthroscopic approach based on imaging findings. Knee Surg Sports Traumatol Arthrosc 15: 676-681. [Crossref]
- Lotta Willberg (2013) Patellar and Achilles Tendinopathy-sclerosing injections and ultrasound guided arthroscopic shaving. Thesis Umeå University.
- Sunding K, Willberg L, Werner S. Alfredson H. Forssblad M, Fahlstrom M (2015) Sclerosing injections and ultrasound-guided arthroscopic shaving for patellar tendinopathy - good clinical results and decreased tendon thickness after surgery - a medium term follow-up study. Knee Surg Sports Traumatol Arthrosc 23: 2259-2268.
- Danielson P, Andersson G, Alfredson H, Forsgren S (2008) Marked sympathetic component in the perivascular innervation of the dorsal paratendinous tissue of the patellar tendon in arthroscopically treated tendinosis patients. Knee Surg Sports Traumatol Arthrosc 16: 621-626. [Crossref]
- Karlsson J, Kälebo P, Goksör LA, Thomée R, Swärd L (1992) Partial rupture of the patellar ligament. Am J Sports Med 20: 390-395. [Crossref]
- Lorbach O, Diamantopoulos A, Kammerer KP, Paessler H.H (2008) The influence of the lower patellar pole in the pathogenesis of chronic patellar tendinopathy. Knee Surg Sports Traumatol Arthrosc16: 348–352.


