Abstract
Background
Temporary or permanent central venous catheter (CVC) insertion has been performed frequently for hemodialysis treatment. The loss of a broken CVC into the circulation is a rare and preventable complication. Here, we report a peculiarly case of a missed temporary CVC after using Moxifloxacin.
Case presentation
We report a 53-year-old uremia woman who was treated with moxifloxacin, fractured her CVC which migrated from right internal jugular vein to right atrium. After the discontinuation of moxifloxacin, her abnormal behavior disappeared.
Conclusions
CVC loss was rarely reported in hemodialysis patients, especially after using moxifloxacin. We report this
case to emphasize the side effect of a commonly used drug and make the clinicians to be cautious when they use
moxifloxacin in uremia patients with CVC who have a risk to be more susceptible to have drug adverse effect. In
systemically reviewing the literature, this is the first case report of moxifloxacin inducing abnormal behavior in a
patient on hemodialysis to fracture CVC.
Keywords
Case report, Central venous catheter (CVC), Uremia, Moxifloxacin
Abbreviation
CVC: central venous catheter; CNS: central nerve system; HCl: hydrochloride; CT: computed tomography; PIP-TAZ: piperacillin sodium-tazobactam sodium
Background
Moxifloxacin is of great use for tuberculosis treatment, which also has rare central nerve system (CNS) adverse effects like hallucinations, tremor, and suicidal thoughts or behaviors [1]. Rcently, Zubicoa et al. reported a 53-year-old male who underwent uneventful cataract extraction with intracameral injection of moxifloxacin and suffered from unilateral acute iris transillumination and distorted pupil [2]. Additionally, the application of moxifloxacin on patients with no underlying risk factors also developed hallucinations or severe acute uveitis, and the patients' symptoms completely resolved after discontinuation of the moxifloxacin [3-5].
Temporary central venous catheter (CVC) insertion is a technique commonly used in uremia hemodialysis patients, regarded as a routine tool in critical patients for measuring hemodynamic variations, delivery of medication and nutritional support. It also comes along with complications including malposition, arterial puncture and infections [6].
Most of those complications occur during the procedure of CVC. We report here a unique case of a 53-year-old uremia woman who was treated with moxifloxacin, fractured her CVC which migrated from right internal jugular vein to right atrium. After the discontinuation of moxifloxacin, her abnormal behavior disappeared soon.
Case presentation
A 53-year-old female presented to the outpatient department with a history of eight-year-chronic kidney disease caused by kidney stone and fever for 3 days. At admission, her vital sign was within normal limit. Clinical examination was remarkable for pain in right renal area, and bilateral lower extremity edema (+). The ultrasound revealed diffuse left kidney pathological changed, pyknosis kidneys, and hydronephrosis and stones in both kidneys. Initial laboratory examination showed white blood cell count 18.79^109/L, hemoglobin 74 g/L, and serum creatine 881.00 μmol/L.
According to her past medication history, we chose piperacillin sodium-tazobactam sodium (PIP-TAZ) for her fever. After a 3-day therapy with PIP-TAZ, the patient still kept at fever. Therefore, we added moxifloxacin hydrochloride (HCl) injection into her treatment. During the combined therapy of PIP-TAZ and moxifloxacin HCl, her temperature flowed at lower numbers than before. Two days later, her temperature was within normal limit.
After a 8-day supportive treatment, the serum creatine increased to 990 μmmol/L and urine volume remained less than 400 ml/d. Meanwhile, the urologist surgeons suggested that the surgery to destroy those stones was meaningless after estimating the patient. According to her past history, clinical presentation, laboratory examination and imaging, we made the diagnosis of uremia and recommended the patient to receive the treatment of dialysis. After discussion with her family, the patient chose hemodialysis. Under local anesthesia, a right central veins catheter was inserted to prepare for hemodialysis. The catheter was fixed at 13 cm at the skin level, after free aspiration of blood. Later in the day, the patient did well during the process of her first hemodialysis without complications. Her second hemodialysis was uneventful, and we withdrew PIP-TAZ at the same day from her therapy and continued the using of moxifloxacin HCl considering the possibility of mycobacterium tuberculosis infection. Three days after CVC insertion, we made it successful to construct the arteriovenous fistula at her left arm.
It is the day after the surgery of arteriovenous fistula when the catheter was fractured, and the patient presented no symptoms of discomfort. It’s said that the patient woke up early in that morning, took off her dirty cloths and then washed it in the bathroom by herself. As soon as her daughter woke up and founded no catheter on the patient’s neck, the on-call resident found the outside part of catheter on the bedside table (Figure 1A and B). Neither results of the clinical examination and ECG were positive. Her X-ray and computed tomography of chest showed no evidence of the missing catheter (Figure 1C and D). Her family denied the psychotic history and genetic disease. The attending doctor realized that it might be the side effect of moxifloxacin and discontinued the drug right away. To confirm the position of catheter, the patient took her ultrasound immediately. It showed that the inside catheter was truly existed with the length of 10 cm and moved to the crossroads of right atrium and inferior caval vein. Fortunately, the catheter didn’t make it way into the right ventricle.
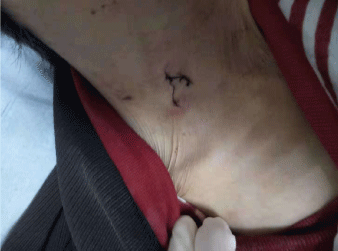
Figure 1A. There was no catheter at the place where it was placed, but red and swollen wound could be seen (arrow)
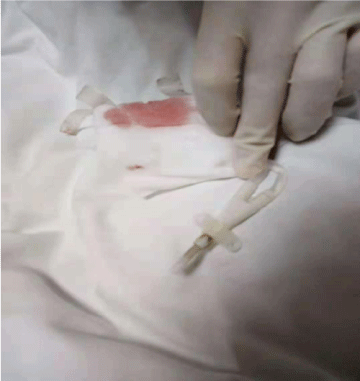
Figure 1B. The outside of the catheter (arrow) found on the patient's bedside table
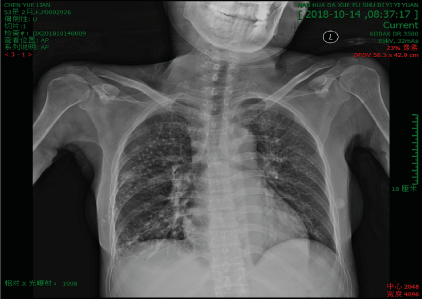
Figure 1C. Chest X-ray showing no imaging of the missing catheter
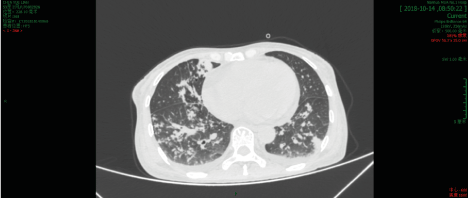
Figure 1D. Computed Tomography demonstrating negative result of the missing catheter’s position
After informed consent, the pre-operative radiography confirmed the migration of the catheter in the inferior caval vein (Figure 2A). Under the local anesthesia, the intravascular foreign body was percutaneous removed under the guidance of inferior vena cavography via lasso technique by the chief of thoracic and cardiovascular surgeon (Figures 2B and C). The procedure was uneventful. Three days after the removal surgery, the patient received her second CVC to continue hemodialysis, and her subsequent hemodialysis was successful too. The patient was doing well without vascular complication.
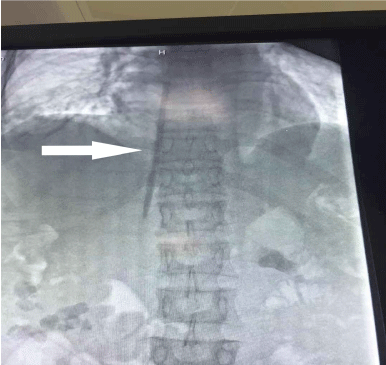
Figure 2A. Pre-operative radiography confirmed the migration of the intravascular catheter (arrow) in the inferior
caval vein
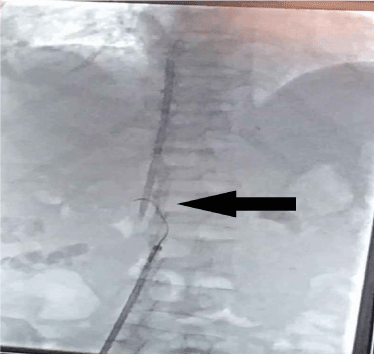
Figure 2B. The missing catheter was removed via lasso (arrow) technique
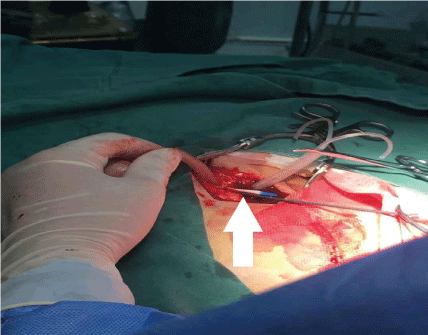
Figure 2C. The intravascular catheter (arrow) was about to be removed from the femoral vein
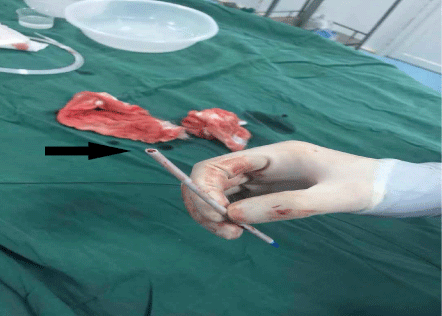
Figure 2D. The intravascular fractured catheter (arrow) was successfully taken out
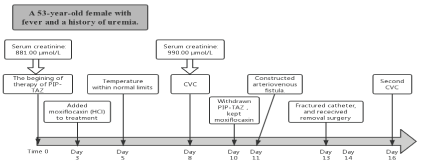
Figure 3. Timeline of the reported case
Discussion and conclusion
In this case, the patient presented good reaction to PIP-TAZ at her last in-patient period controlling her fever. As a result, we chose PIP-TAZ to deal with her fever again. It turned out that she didn’t react well this time. Her CT scan showed multiple patchy and striped hyperdense shadows in both lungs, and nodular calcification in some lesions (Figure 1D) [7]. The infectious diseases physician, considering of the result of CT, suggested that we should add moxifloxacin (HCl) to the anti- infection treatment at day 3 for the suspected diagnosis of lung tuberculosis. Then laboratory tests (day 10), detection of tuberculosis antibody and T-SPOT, conformed the possibility of mycobacterium tuberculosis infection [8,9]. Therefore, we discontinued PIP-TAZ and kept moxifloxacin HCl along as the anti-infection treatment until day 13.
As to the fractured catheter, we found the cut at the end of broken catheter (Figures 1B and Figure 2D). We deemed that the catheter was broken by external force such as scissors. Moxifloxacin is an ideal agent for tuberculosis treatment [1]. But this medicine, one subtype of Quinolones, can also cause CNS events, including hallucinations, tremor, and suicidal thoughts or behaviors. Not to mention that the uremic patient had the symptom of oliguria, this could lead to the inefficient excretion of toxin and drugs, and her age of 53 years old. Thus, we deduced it as a drug-induced hallucination. This may explain the abnormal behavior of the patient. Therefore, we should be cautious before making the decision to add moxifloxacin to treatment of uremia patients or CVC patients under other circumstances, like ICU or emergency department. We are supposed to inform patients or their family members of possible adverse effects in drug use in advance as well.
In general, we used to regard X-rays as the basic examination to get the position of intravascular guidewire [10]. But in this case, we failed to found the image of intravascular catheter via X-ray firstly, which mentioned to be effective in common views [11]. The image of CT also showed no evidence of the intravascular foreign body. Ultrasound, a convenient and economical non-invasive examination method, is widely used in clinical diagnosis. In recent years, the use of ultrasound has been proposed to reduce the number of complications and to increase the safety and quality of CVC placement [12]. In this case, it finally worked out well by ultrasound and the subsequent pre-operation radiography in diagnosis of intravascular catheter.
In conclusion, Moxifloxacin is not only effective, safe, but also harmful. It is better to sign an informed consent before using it on uremia patients who received CVC. When we need to confirm the position or migration of intravascular catheter, it’s advised to use ultrasound as the primary examination method. As a popular examination method in recent years, radiography is also recommendable.
Acknowledgement
We are grateful to Jianglong Li, Ph.D, M.D. for his constructive comments in improving the language, grammar, and readability of the paper
Funding
This study was not supported by any funding.
Availability of data and materials
The data supporting the conclusions of this article is included within the article.
Authors’ contributions
DYJ wrote the manuscript and contributed to acquisition of data. HZX was the treating physician of the patient and contributed to revising critically important intellectual content of the manuscript. WQS and HZX analyzed the clinical course and contributed to conception of conclusion. All authors read and approved the final manuscript.
Competing interests
The authors declare that they have no competing interests.
Consent for publication
Written informed consent was obtained from the patient for publication of this case report and any accompanying
images. The authors adhered to CARE guidelines/methodology.
Ethics approval and consent to participate
Not applicable.
References
- Xu P, Chen H, Xu J, Wu M, Zhu X, et al. (2017) Moxifloxacin is an effective and safe candidate agent for tuberculosis treatment: a meta-analysis. Int J Infect Dis 60: 35-41. [Crossref]
- Zubicoa A, Echeverria-Palacios M, Mozo Cuadrado M, Compains Silva E (2020) Unilateral Acute Iris Transillumination-like Syndrome following Intracameral Moxifloxacin Injection. Ocul Immunol Inflamm 2020:1-2. [Crossref]
- Mazhar F, Akram S, Haider N (2016) Moxifloxacin-induced acute psychosis: A case report with literature review. J Res Pharm Pract 5: 294-296. [Crossref]
- Higdon E, Twilla JD, Sands C (2017) Moxifloxacin-Induced Visual Hallucinations: A Case Report and Review of the Literature. J Pharm Pract 30: 375-377. [Crossref]
- Duncombe A, Gueudry J, Massy N, Chapuzet C, Gueit I, et al. (2013) Severe pseudouveitis associated with moxifloxacin therapy. J Fr Ophtalmol 36: 146-150. [Crossref]
- Endri M, Cartei G, Zustovich F, Serino FS, Fassina A (2010) Differential diagnosis of lung nodules: breast cancer metastases and lung tuberculosis. Infez Med 18: 39-42. [Crossref]
- Asri H, Zegmout A (2018) Historic sequelae of lung tuberculosis. Pan Afr Med J 30: 210. [Crossref]
- Sari NIP, Mertaniasih NM, Soedarsono, Maruyama F (2019) Application of serial tests for Mycobacterium tuberculosis detection to active lung tuberculosis cases in Indonesia. BMC Res Notes 12: 313. [Crossref]
- Zhao S, Wang Z, Zhao Y (2019) Loss of guidewire and its sequelae after central venous catheterization: A case report. Medicine (Baltimore) 98: e16513. [Crossref]
- Van Doninck J, Maleux G, Coppens S, Moke L (2015) Case report of a guide wire loss and migration after central venous access. J Clin Anesth 27: 406-410. [Crossref]
- Saugel B, Scheeren TWL, Teboul JL (2017) Ultrasound-guided central venous catheter placement: a structured review and recommendations for clinical practice. Crit Care 21: 225. [Crossref]
- Hoffman T, Du Plessis M, Prekupec MP, Gielecki J, Zurada A, et al. (2017) Ultrasound-guided central venous catheterization: A review of the relevant anatomy, technique, complications, and anatomical variations. Clin Anat 30: 237-250. [Crossref]









