Wound healing of chronic ulcers remains challenging, especially in regions of impaired perfusion, or in defects with bradytrophic tissue such as tendon exposure. This case impressively demonstrates a microvascular free flap coverage approach for complex Achilles tendon ulcers, outlining the limitations of conservative treatment attempts and the potentials of a surgical approach.
In an aging society, chronic leg ulcers are a dramatically increasing medical and health-economic problem. They account for significant patient morbidity, loss in quality of life and increasing healthcare expenditure [1]. Even with modern diagnostic tools and consequent therapy of the underlying disease in specialized centers, wound healing of chronic ulcers remains challenging. There is a great need for effective strategies, especially in order to accelerate the stages of granulation and epithelialization. In regions of impaired perfusion, or in defects with exposed bradytrophic tissue, conservative wound healing strategies often fail. These wounds usually require aggressive surgical debridement followed by microvascular free tissue transfer to achieve adequate defect coverage. The benefits of this approach include an enhanced blood supply at the recipient site and an immediate defect reconstruction [2].
A 53-year-old male patient with combined complex soft-tissue and Achilles tendon defect following surgical repair of a traumatic Achilles tendon rupture consulted our outpatient clinic for wound management. Written informed consent was provided by the patient to publish the following case details and associated images. He presented with an ulcer of 1.5 cm diameter with bacterial overgrowth within an externally grafted split skin. The wound had been resistant to conservative treatment for three months using antiseptic topicals and specialized wound dressings. The patient had a clinical history of type II diabetes. Venous insufficiency and peripheral arterial occlusive disease had been ruled out prior to our consultation. A punch biopsy taken from the center and margin of the ulcer showed capillary occlusion in the deeper dermis, compatible with livedoid vasculopathy. In order to promote angiogenesis and to optimize wound conditioning, cold atmospheric plasma (CAP) therapy three times a week for a duration of 90 seconds (PlasmaDerm® (Cinogy®)) was performed. Several in vitro and in vivo studies have demonstrated that CAP activates angiogenesis-promoting pathways and reduces the bacterial load in chronic wounds [3,4]. After four weeks of treatment, the defect reduced to 1.2 cm diameter, showing no further sign of infection (Figure 1). After achieving vital granulation tissue, defect coverage was attempted using another split skin graft. However, complete graft failure was observed.
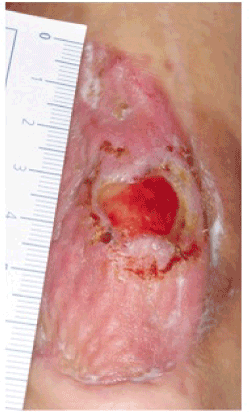
Figure 1. Therapy-resistant Achilles tendon ulcer in the center of a split skin graft after four weeks of CAP treatment three times a week for 90 seconds
Thereafter, complete surgical debridement was undertaken, followed by initiation of negative pressure therapy. Five days later, defect coverage was achieved using a free composite fasciocutaneous anterolateral thigh flap including fascia lata for Achilles tendon reconstruction [5,6] (Figures 2,3). The postoperative course was uneventful and led to an excellent clinical result in this complex anatomic localization. The patient was discharged from the hospital ten days after free flap reconstruction and returned to work eight weeks postoperatively (Figure 4).
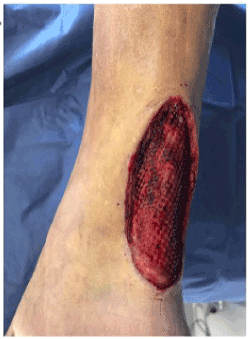
Figure 2. Tissue defect of the Achilles tendon side after surgical debridement
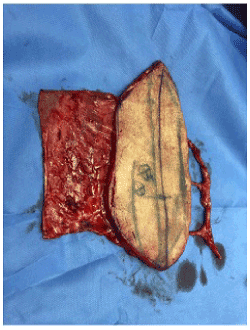
Figure 3. Free composite fasciocutaneous anterolateral thigh flap including fascia lata of the lateral vastus muscle
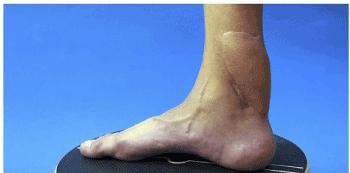
Figure 4. Postoperative result with a complete healing of the thigh flap
To conclude, wound healing of chronic ulcers remains challenging, especially in regions of impaired perfusion, or in defects with bradytrophic tissue such as tendon exposure. This case impressively demonstrates the need for localization-adapted special intervention strategies for defect coverage of complex wounds, outlining the limitations of conservative treatment attempts and the potentials of an interdisciplinary approach. Especially in demanding locations with tendon exposure, microvascular free flap coverage seems to be superior to free skin grafting.
none
none to declare
- Neumann HAM, Cornu‐Thénard A, Jünger M, Mosti G, Munte K (2016) Evidence-based (S3) guidelines for diagnostics and treatment of venous leg ulcers. J Eur Acad Dermatol Venereol 30: 1843-1875. [Crossref]
- Smith IM, Austin OM, Batchelor AG (2006) The treatment of chronic osteomyelitis: a 10-year audit. J Plast Reconstr Aesthet Surg 59: 11-15. [Crossref]
- Arndt S, Unger P, Berneburg M, Bosserhoff AK, Karrer S (2018) Cold atmospheric plasma (CAP) activates angiogenesis-related molecules in skin keratinocytes, fibroblasts and endothelial cells and improves wound angiogenesis in an autocrine and paracrine mode. J Dermatol Sci 89: 181-190. [Crossref]
- Isbary G, Heinlin J, Shimizu T, Zimmermann JL, Morfill G, et al. (2012) Successful and safe use of 2 min cold atmospheric argon plasma in chronic wounds: results of a randomized controlled trial. Br J Dermatol 167: 404-410. [Crossref]
- Ehrl D, Heidekrueger PI, Schmitt A, Liska F, Ninkovic M, et al. (2019) The Anterolateral Thigh Flap for Achilles Tendon Reconstruction: Functional Outcomes. Plast Reconstr Surg 143: 1772-1783. [Crossref]
- Houtmeyers P, Opsomer D, Van Landuyt K, Monstrey S (2012) Reconstruction of the Achilles tendon and overlying soft tissue by free composite anterolateral thigh flap with vascularized fascia lata. J Reconstr Microsurg 28: 205-209. [Crossref]




