Introduction: Achieving adequate follow-up for surgical patients is challenging in resource-poor environments, especially for short-term surgical missions (STSM). The aim of this study was to evaluate late postoperative complications (POC) and quality of life (QOL) of surgical patients using mobile phones to facilitate patient follow-up.
Methods: Since 2008, an organization sponsored by a US academic institution has conducted surgical trips in partnership with a public hospital in Haiti. During the 2016 trip, mobile phones were used to facilitate follow-up for 2014-2015 operative patients. Late POC and QOL were then evaluated among follow-up patients.
Results: Follow-up was achieved in 34 (31%) of 110 operative patients with a mean length of follow-up of 17.8 months (range: 3-60). Of 110 patients, 96 (87%) had phone numbers recorded; phone contact was achieved in 25 (23%) of these patients. Out of a total of 34 follow-up patients, twenty (59%) returned to clinic and 14 (41%) were interviewed solely over the phone. Follow-up patients reported a 41% improvement in ability to complete ADLs (p=0.001) and a 71% reduction in pain (p<0.001). One year after surgery, all seven prostatectomy patients who were previously catheter-dependent no longer required indwelling catheters (p=0.001).
Conclusions: To our knowledge, this study is one of the first to utilize mobile phones to acquire long-term follow-up for patients following a STSM. Our results demonstrate that it is possible to measure postoperative outcomes not otherwise obtainable in the perioperative period. Such long-term follow-up is useful and essential for determining the effectiveness and safety of STSMs.
short-term surgical trips, mission trips, follow-up, quality of life, global surgery, global health, mobile phones, Haiti
The unmet need for surgical services worldwide, particularly in low- and middle-income countries (LMICs), is profound, with an estimated 5 billion people without adequate access [1,2]. “Global surgery” encompasses a variety of interventions that have attempted to address that need, including short-term surgical missions (STSM) [1]. Methods can vary greatly between STSMs, but most share the goal of delivering quality care in the context of limited resources and time with the hope of long-lasting impact for patients [2-5]. However, obtaining long-term follow-up of patients is challenging for STSMs—and there are few descriptions of the methods used to achieve such follow-up and even fewer reports of clinical outcomes—making determination of their success challenging [3,6]. Achieving patient follow-up is challenging even for established hospital systems in rural, resource-poor settings where STSMs often function, but there is evidence that mobile phones may enhance patient follow-up in such settings, including rural Haiti [7-12]. The aim of this study was two-fold: 1) to evaluate the efficacy of mobile phones to facilitate long-term patient follow-up (> one year) among a cohort of STSM patients in rural Haiti and 2) to measure long-term surgical outcomes, particularly late postoperative complications (POC) and the impact of operations upon patient quality of life (QOL), not measurable in the perioperative period.
Surgical trip logistics, surgical techniques, and perioperative protocols
Since 2008, a U.S. school of medicine, department of surgery, urology and anesthesiology have partnered with a non-profit organization to provide surgical care at L’Hôpital St. Thérèse in Hinche, Haiti. The annual trip and surgical operations performed are entirely funded by members of the organization through private charitable donations with occasional grant support. All necessary medications and supplies are transported in-country by the team. The trip consists of two operative weeks flanked by one week of pre- and post-operative clinic. Patients are primarily referred by the hospital, but many patients come to clinic after hearing about the trip through radio announcements made by the non-profit partner or by word of mouth.
All inguinal hernia repairs were Bassini tissue repairs without mesh, and patients received antibiotics for one day postoperatively per Haitian medical system requirements. All simple prostatectomies were performed solely for the indication of benign prostatic hyperplasia (patients with presumed prostate cancer were excluded although pathologic analysis was not available to confirm diagnosis) using an open suprapubic approach, and patients received antibiotics until all catheters were removed (six weeks postoperatively). All patient interviews were conducted and recorded on paper charts by participating medical student team members. Trained interpreters were employed to communicate with patients, who predominantly spoke Creole. Diagnostic testing was limited by the environment to a few basic laboratory tests including hemoglobin and hematocrit, BUN/creatinine, x-ray, and ultrasound. All patients received necessary medications, education and supplies for proper wound care and discharge instructions to return to clinic one week after surgery for post-operative evaluation.
Collection and review of patient medical records
Patient records prior to 2014 were unavailable for review. Since 2014, medical records have been standardized and patient data has been consistently collected to include patient contact information (telephone numbers when available). Patient records from 2014-2015 were reviewed for demographic, clinicopathologic information and immediate POC (seven days postoperatively). A postoperative complication was defined as any deviation from the normal postoperative course using the Clavien-Dindo classification system [13].
Use of mobile phone to enhance patient long-term follow-up (> one year postoperatively)
During the 2016 trip, prior patient records from 2014-2015 were reviewed and available telephone numbers were called to request that patients return to clinic during the four-week period when the team was in-country. A translator was employed to help make all necessary phone calls and to conduct interviews both in clinic and over the phone. In addition, radio announcements were made prior to and during the four-week trip by the non-profit partner to encourage patients who previously received surgery by the group to return to clinic. Three patients were also reached by other means: one patient who preceded the standardization of the medical records has worked as a team translator for several years and was thus already present, and two additional patients were able to be reached through a family member who has volunteered with the surgical trip for several years.
Measurement of long-term postoperative outcomes (> one year postoperatively)
A tool to measure post-surgical QOL was developed by the operative team (Figure 1) based upon the 36-item Short-Form Health Survey (SF-36) and previous experience [14]. The tool also incorporated the International Prostate Symptom Score (IPSS) for prostatectomy patients [15].
Patients who returned for follow-up clinic were examined, and early and late POC as well as QOL (using the previously mentioned QOL assessment tool) were assessed using a standardized questionnaire (Figure 1). Patients who did not return to clinic were called during the last week of the STSM to assess POC and QOL over the phone. Length of follow-up was calculated as the time from surgery to follow-up or to estimated date of death based on family report. Institutional Review Board approval from the U.S. institution and equivalent approval from our partner hospital were obtained as well as patient consent to participate in this study.

Figure 1. Quality of Life Survey
All statistical analyses were performed using SPSS statistics 23.0 (Armonk, NY: IBM Corp). Chi-square tests were used to compare demographics and clinical outcomes of 2014-2015 operative patients and the follow-up cohort as well as changes to QOL among the follow-up cohort; p-values were calculated using Fisher’s exact test. A p-value <0.05 was considered statistically significant.
A total of 110 patients received 113 operations from 2014-2015. The median age was 45 years (range: 2 months–86 years). The majority were male (90%), manual laborers (50%), unemployed (11%) and/or students (15%) with limited income. Average time travelled to the hospital was 76 minutes (range: 0–300 minutes), with the majority traveling via motorcycle. The majority of operations performed were inguinal hernia repair (39%) followed by open prostatectomy (15%) and hydrocelectomy (12%) (Table 1).
Table 1: Demographics and Clinicopathologic Features
Variable |
All 2014-15 patients
n (%) |
Follow-up cohort
n (%) |
p-value |
Operative patients |
110 |
34 |
-- |
Age, median (range) |
45yo (2 mo-80 yo) |
45 yo (6-76 yo) |
0.88 |
Gender
Male
Female |
99 (90)
11 (10) |
31 (91)
3 (9) |
1.00 |
Occupation
Manual laborers
Student
Unemployed
Other |
55 (50)
16 (15)
12 (11)
3 (3) |
19 (56)
5 (15)
9 (26)
1 (3) |
0.65 |
Distance travelled (minutes), average (range) |
76 (0-300) |
65 (5-300) |
0.51 |
Operations performed
Inguinal hernia repair
Prostatectomy
Hydrocelectomy
Other |
113
43 (39)
16 (15)
13 (12)
38 (34) |
34
14 (41)
8 (24)
2 (6)
10 (29) |
0.27 |
Eighty-five of these operative patients (77%) returned to follow-up clinic one week post-operatively. Seven patients developed POC (< seven days postoperatively) (8%) (Table 2) with most (72%) being Clavien-Dindo grade I or II. There were two surgical site infections (SSI) (2%), and four wound dehiscences (4%). There were three unplanned readmissions (3%): one patient was admitted for treatment of a deep venous thrombosis, one patient with a SSI/wound dehiscence was admitted for local wound care, and one patient with significant scrotal edema was admitted for pain control and intravenous antibiotics. Another patient required a reoperation (< 1%) for debridement of a Pseudomonas infection of her skin graft following a mastectomy for a necrotic breast mass. Finally, one patient suffered a neurologic event during surgery and was transferred to rehab following his recovery.
Table 2: Postoperative Complications
Variable |
All 2014-2015 patients
(7-day post-op)
(n = 110)
n (%) |
Follow-up Cohort
(> 1-year post-op)
(n = 34)
n (%) |
p-value |
Length of Hospital Stay (days),
average (range) |
2 (0-13) |
2 (0-8) |
0.74 |
Patients who developed POC
Clavien-Dindo I
Clavien-Dindo II
Clavien-Dindo III
Clavien-Dindo IV |
7 (6)
2 (29)
3 (43)
1 (14)
1 (14) |
2 (6)
0
2 (6)
0
0 |
0.65 |
Surgical site infections (SSI) |
2 (2) |
2 (6) |
1.00 |
Wound dehiscence |
4 (4) |
1 (3) |
1.00 |
Sepsis |
0 |
0 |
-- |
Readmission |
3 (3) |
0 |
-- |
Reoperation |
1 (<1) |
0 |
-- |
Inguinal Hernia Repair Complications
Chronic groin pain
Hernia recurrence |
--
-- |
0
1 (3) |
-- |
Open Prostatectomy Complications
Urethral Stricture
Impotence
Incontinence |
--
--
-- |
0
2 (25)
0 |
-- |
Of 110 patients, 96 (87%) had phone numbers recorded. Phone contact was achieved in 25 (23%) of these patients and 13 (12%) of the patients reached by phone subsequently returned to clinic. Long-term follow-up was obtained in a total of 34 (31%) patients. Twenty (59%) of these follow-up patients returned to clinic and 14 (42%) follow-up patients who could not return to clinic were solely interviewed over the phone. Seven patients (21%) who were not contacted via mobile phone returned to clinic (Figure 2). Prior to using mobile phones to facilitate follow-up (i.e., during 2014 and 2015 post-operative clinics), a total of only four operative patients followed-up in clinic.
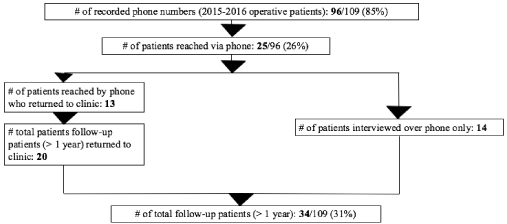
Figure 2. Follow-up Methods (> 1 year postoperative)
Among follow-up patients, mean length of follow-up was 17.8 months (range: 3–60). Mean age was 45 years (range: 6–76) and the majority of patients were male (91%). Mean travel time for patients was 65 minutes (range: 5–300 minutes), and the majority of patients used a motorcycle to travel to clinic. Half were manual laborers, mostly farmers, and the rest were either unemployed, students or other various professions such as tailors or craftsmen. Operations received were primarily inguinal hernia repair (41%) and open prostatectomy (24%) although 29% of patients received a variety of different operations including: cystoscopy and dilation (1), celiotomy for bilateral kidney stone obstruction (1), meatoplasty (1) and I&D of a neck mass (1). In this cohort, there were two (6%) reported SSIs and one (3%) reported wound dehiscence; both patients had received prostatectomies. One SSI was not diagnosed in a patient during the previous perioperative clinic because he had chosen to follow-up at another distant hospital. There were no reported episodes of sepsis, no readmissions or reoperations (Table 2).
Among inguinal hernia repair patients, none reported chronic groin pain. There was one (3%) small asymptomatic recurrent hernia in a patient who underwent a bilateral hernia repair in 2014. Among prostatectomy patients, there were no reported urethral strictures, or incontinence. There were two patients (25%) who reported difficulty with ejaculation and/or maintaining an erection following surgery (Table 2).
There were two deaths three months following surgery due to non-surgical disease. One 68-year-old male appears to have died of a stroke or cardiac arrest and one 9-year-old male died of presumed lymphoma.
Between the preoperative and postoperative period among all follow-up patients, there was a 71% reduction in reported pain (p <0.001), a 41% improvement in ability to complete activities of daily living (ADLs) (p = 0.001), and a 26% improvement in ability to complete work (p = 0.049) (Figure 1). Among the nine prostatectomy patients, all seven (100%) who were catheter-dependent prior to surgery no longer had indwelling catheters (p = 0.001). In addition, one year following surgery, obstructive urinary symptoms decreased by 25% (p = 0.015), hematuria decreased by 67% (p = 0.24), dysuria decreased by 100% (p < 0.001) and frequency of urination increased by 133% (p = 0.33) (Figure 3).
Our study represents one of the first to successfully achieve long-term follow-up (> one year) for STSM patients using mobile phones to facilitate patient follow-up. Follow-up obtained was then utilized to measure the long-term outcomes of the operations performed, with a focus on late POC and the impact of operations upon patient QOL, both not measurable in the perioperative period. Our results demonstrate that mobile phones can be successfully utilized by STSMs to obtain long-term follow-up for patients in rural Haiti. STSMs should strive to obtain such follow-up data as the information obtained is essential in measuring the success of STSMs.
Much has been written about the challenges of global surgery, and of STSMs in particular [1-4]. One of the major challenges for STSMs is obtaining adequate patient follow-up, which is necessary to measure patient outcomes and quantify impact. The cost-effectiveness of STSMs has frequently been questioned; however, limited reported methods and outcomes data make such analysis incomplete [2]. One study conducted by Torchia et al. [6] successfully achieved interval patient follow-up one year postoperatively utilizing an in-country physician to conduct follow-up at a mean cost of $20,000 per year. In our own experience, patient follow-up is limited by several factors that were similarly identified by Torchia et al. Communication with in-country partners can be challenging, which may limit the amount of follow-up information that can be transmitted remotely. Utilizing in-country physician partners can be cost-prohibitive and the reproducibility of such results obtained remotely has been questioned [6]. But even established hospital systems in LMICs, especially in rural areas, struggle to obtain patient follow-up for a variety of reasons, including poor patient health literacy as well as the far distances that patients must travel in order to obtain surgery and subsequent care.6,7 Community health workers (CHW) have been utilized to conduct postoperative visits at patients’ homes in order to address these challenges; however, relying upon such a network is also imperfect and expensive with the reproducibility of such results obtained remotely also questioned [8]. Despite their demonstrated utility, a partner physician or CHW network were not easily or reliably available for us to utilize to conduct interval follow-up.
Given these challenges, the utilization of mobile phones to coordinate patient follow-up has been investigated in various rural, resource-poor settings, including Haiti [7,8,10-12]. Haiti has an estimated 62% mobile phone ownership rate, and 86% of our operative patients had mobile phone numbers recorded. Thus, we became interested in investigating the success of mobile phones to facilitate patient follow-up among our surgical population. Using mobile phones, we were able to facilitate follow-up of at least one year postoperatively in 34/110 (31%) operative patients. During the four-week period that we conducted phone calls, only 26% of patients with phone numbers recorded could be reached by phone. There are likely many reasons for the unreliability of mobile phone communication within our patient population. We conducted these phone calls for a limited time period (four weeks while in country) and at least one year following patients’ surgeries. In Haiti, when a mobile phone is lost, a new phone with a new SIM card and phone number must be purchased. Therefore, the long interval of elapsed time between surgery and our follow-up (one year) would likely increase the probability of a lost phone and a non-working number. Furthermore, the majority of our patients live in rural areas with limited income and restricted access to electricity thereby limiting their ability to add minutes to their phones or have access to adequate cell phone signal and/or charged phones. Despite these challenges, mobile phones did successfully enhance long-term patient follow-up among our patient population. Prior to the use of mobile phones to facilitate patient follow-up during the 2014 and 2015 trips, a total of four patients from previous years had returned to clinic for follow-up. Our trip is conducted during the same month every year, and our in-country partners facilitate patient referral and follow-up utilizing radio announcements to the region surrounding Hinche. As a result, seven patients who were not reached via phone did return to clinic. Our results suggest that patient follow-up may be best facilitated through a variety of means, and that sustainable interventions—coordinated with in-country partners with predictable patterns—are important contexts within which to provide patient care and conduct follow-up.
Our objective in obtaining long-term patient follow-up (> one year postoperatively) was to measure patient outcomes that could not be measured in the perioperative period such as the impact of operations upon patient QOL, and which would help guide future recommendations for performing surgery in Haiti. The demographics of the follow-up cohort reflect those of operative patients (Table 1). The objective of the perioperative clinic conducted one week following surgery is to perform SSI surveillance; however, it is unknown whether additional patients develop an SSI and whether they are treated following our departure. We did not find a dramatic difference in the type or rate of early POC measured among the follow-up cohort (Tables 2). Among the follow-up cohort, two patients reported SSI, one of which was also a wound dehiscence. Only one of these patients with a reported SSI was not previously identified during our perioperative clinic because he had followed up at an outside hospital. There were no reported episodes of sepsis, readmissions or reoperations.
Late POC particular to inguinal hernia repair and open prostatectomy were also evaluated. There is limited data on long-term outcomes for both inguinal hernia repair and open prostatectomy patients in resource-poor settings; however, there is some data to suggest that such operations can safely be performed with acceptable mortality and morbidity [16-19]. Among the follow-up inguinal hernia repair patients, no patients reported chronic groin pain. One patient who had a bilateral inguinal hernia repair two year prior reported a small asymptomatic inguinal hernia. Among prostatectomy patients, we had particular concerns about catheter adherence post-operatively as patients are encouraged to keep indwelling penile catheters four weeks postoperatively and premature removal could result in urethral stricture; however, among our follow-up prostatectomy patients there were no reported urethral strictures. There were two patients above 50 years of age who reported having trouble either maintaining erections and/or ejaculating, but given that both were catheter-dependent prior to surgery, it is unclear whether impotence was present prior to surgery.
In order to measure QOL, we created a survey that incorporated components of the SF-36—which has been validated among inguinal hernia patients—and reflected our previous experience working with this population in which patients tended to present to our clinic with advanced surgical disease that caused significant pain and therefore significantly limited their activities of daily living (ADLs), including work (Figure 3) [14,20]. For prostatectomy patients, we also surveyed urinary symptoms, incorporating the IPSS, which has been well validated among urologic, and in particular prostatectomy, patients [15]. Among all follow-up patients, there was a 71% reduction in reported pain from the preoperative to the postoperative period, a 41% improvement in their ability to complete ADLs, and a 26% improvement in their ability to work (all p < 0.005) (Figure 3). Among the prostatectomy patients, obstructive urinary symptoms, haematuria and dysuria all decreased post-operatively, and most notably, all seven of nine prostatectomy patients who previously had indwelling catheters prior to surgery were no longer catheter-dependent (Figure 4). There was an increase in reported nocturia; however, this is not entirely unexpected following an open suprapubic prostatectomy and could still be considered an improvement in QOL for the majority of patients who previously were catheter-dependent (Figure 4).
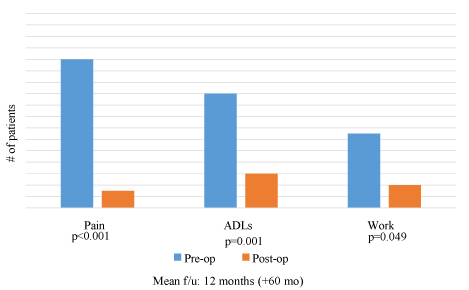
Figure 3. Postoperative Quality of Life—All Patients (n=34)
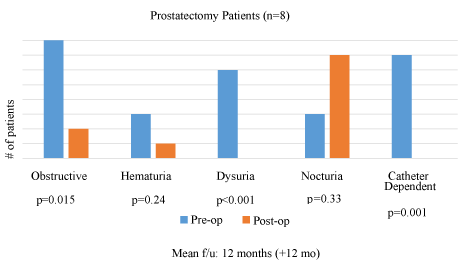
Figure 4. Postoperative Quality of Life—Prostatectomy Patients
Our study is limited both by the extent of follow-up obtained facilitated by the mobile phone as well as by the validity of results obtained. We are limited in the extent of follow-up obtained, particularly in clinic, by our limited time in country (four weeks), the far distances patients had to travel to reach clinic (on average 65 minutes primarily on motorcycle), and the unreliability of mobile phone communication among our patient cohort, as previously mentioned. In addition, the validity of the results obtained is limited. We relied heavily on self-report among patients given that we were not in-country to conduct interval follow-up closer to surgery and some patients were unable to return to clinic during our time present in Haiti. Such data obtained from patients is further limited by significant language barriers as well as poor health literacy of both the patients and translators we employ. For example, based on retrospective review, one patient did not report a previous SSI diagnosed and treated in our perioperative clinic a year prior. Finally, the limited power of our follow-up cohort with few reported adverse events as well as potential sample bias among follow-up patients limit our ability to generalize these results even amongst own entire patient cohort.
Future directions include 1) strengthening in-country partnerships in order to improve interval patient follow-up and therefore sustain quality patient care and 2) enhancing and standardizing our methods of evaluating patient outcomes in order to more uniformly and accurately quantify the impact of this STSM upon patient outcomes.
To our knowledge, this study is one of the first to report methods utilizing a mobile phone to facilitate long-term patient follow-up (> one year) for STSM patients. Our results demonstrate that obtaining such long-term follow-up is useful as it is possible to measure postoperative outcomes not measurable in the perioperative period that are essential to determining the effectiveness and safety of STSMs and which will help guide recommendations for practicing surgery, in particular prostatectomy, in Haiti.
We would like to acknowledge several people who supported our work and without whom these results would not be possible. Thank you to our translators Michelet Desire, Jean Gilles Mitial, and Rezanord Mercon (Zombie). We would also like to thank our partners at Project Medishare in particular Dr. Rony Destine and our partners at Hospital St. Therese in particular Dr. Prince Pierre. We would also like to acknowledge the other surgeons and anesthesiologists who performed operations and provided clinical care to study patients in particular Dr. Haack, Dr. Carney, Dr. Lynde, and Dr. Sullivan. Thank you to Meg Quinn for standardized our medical charts and initiating the collection of data for our trip starting in 2014. And, thank you to the rest of the students, residents and staff who have participated on these trips and contributed to the clinical care of these patients.
- Meara JG, Leather AJ, Hagander L, Alkire BC, Alonso N, et al. (2015) Global Surgery 2030: evidence and solutions for achieving health, welfare, and economic development. Lancet 386: 569-624. [Crossref]
- Shrime MG, Sleemi A, Ravilla TD (2015) Charitable platforms in global surgery: a systematic review of their effectiveness, cost-effectiveness, sustainability, and role training. World J Surg 39: 10-20. [Crossref]
- Wolfberg AJ (2006) Volunteering overseas--lessons from surgical brigades. N Engl J Med 354: 443-445. [Crossref]
- Schneider WJ, Migliori MR, Gosain AK, Gregory G, Flick R; Volunteers in Plastic Surgery Committee of the American Society of Plastic Surgeons; Plastic Surgery Foundation (2011) Volunteers in plastic surgery guidelines for providing surgical care for children in the less developed world: part II. Ethical considerations. Plast Reconstr Surg 128: 216e-222e. [Crossref]
- Sykes KJ (2014) Short-term medical service trips: a systematic review of the evidence. Am J Public Health 104: e38-48. [Crossref]
- Torchia MT, Schroder LK, Hill BW, Cole PA (2016) A Patient Follow-up Program for Short-Term Surgical Mission Trips to a Developing Country. J Bone Joint Surg Am 98: 226-232. [Crossref]
- Pathak A, Sharma S, Sharma M, et al. (2015) Feasibility of a Mobile Phone-Based Surveillance for Surgical Site Infections in Rural India. Telemed J E Health 21: 946-949. [Crossref]
- Matousek A, Paik K, Winkler E, Denike J, Addington SR, et al. (2015) Community health workers and smartphones for the detection of surgical site infections in rural Haiti: a pilot study. Lancet 385 Suppl 2: S47. [Crossref]
- House DR, Cheptinga P, Rusyniak DE (2015) Availability of mobile phones for discharge follow-up of pediatric Emergency Department patients in western Kenya. PeerJ 3: e790. [Crossref]
- Foong DY, Butler DP, Vanna K, Sok Leng T, Gollogly J (2012) A mobile phone initiative to increase return for speech therapy follow-up after cleft palate surgery in the developing world. J Plast Reconstr Aesthet Surg 65: e260-261. [Crossref]
- Odigie VI, Yusufu LM, Dawotola DA, Ejagwulu F, Abur P, et al. (2012) The mobile phone as a tool in improving cancer care in Nigeria. Psychooncology 21: 332-335. [Crossref]
- Lin H, Chen W, Luo L, Congdon N, Zhang X, et al. (2012) Effectiveness of a short message reminder in increasing compliance with paediatric cataract treatment: a randomized trial. Ophthalmology 119:2463-70. [Crossref]
- Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240: 205-213. [Crossref]
- Ware JE Jr., Sherbourne CD (1992) The MOS 36-item short-form health survey (SF-36). I. Conceptual framework and item selection. Med Care 30:473-83. [Crossref]
- Bosch JL, Hop WC, Kirkels WJ, Schröder FH (1995) The International Prostate Symptom Score in a community-based sample of men between 55 and 74 years of age: prevalence and correlation of symptoms with age, prostate volume, flow rate and residual urine volume. Br J Urol 75:622-30. [Crossref]
- Beard JH, Ohene-Yeboah M, devries CR, Schecter WP (2015) Hernia and Hydrocele. Debas HT, Donkor P, Gawande A, Jamison DT, Kruk ME, et al. (Edtr). Essential Surgery: Disease Control Priorities. (3rd edn) 1. Washington (DC).
- Condie JD Jr, Cutherell L, Mian A (1999) Suprapubic prostatectomy for benign prostatic hyperplasia in rural Asia: 200 consecutive cases. Urology 54: 1012-6. [Crossref]
- Meier DE, Tarpley JL, Imediegwu OO, Olaolorun DA, Nkor SK, et al. (1995) The outcome of suprapubic prostatectomy: a contemporary series in the developing world. Urology 46: 40-44. [Crossref]
- Kiptoon DK, Magoha GA, Owillah FA (2007) Early postoperative outcomes of patients undergoing prostatectomy for benign prostatic hyperplasia at Kenyatta National Hospital, Nairobi. East Afr Med J 84: S40-44. [Crossref]
- Brazier JE, Harper R, Jones NM, O'Cathain A, Thomas KJ, et al. (1992) Validating the SF-36 health survey questionnaire: new outcome measure for primary care. BMJ 305: 160-164. [Crossref]




