We wish to describe a 22-year-old male with hepatotoxicity and fibrosis due to extensive ketamine abuse. During our workup there was no other significant cause for liver disease. Ketamine is an NMDA receptor antagonist used commonly as a procedural sedative. It is abused on “the street” and known as “Special K”. It is popular among users for its dissociative effects. Urological, biliary and liver abnormalities have been reported previously in the literature as a result of long-term Ketamine abuse-severe liver fibrosis/cirrhosis has rarely been reported in the US as a result of its abuse. This case offers important teaching points and may herald a new trend as Ketamine becomes increasingly popular.
long-term ketamine, liver disease, hepatotoxicity, ketamine abuse
We describe acute hepatopathy and fibrosis in a 22-year-old male regularly abusing ketamine. No other cause was identified. A liver biopsy was performed. The findings were consistent with F3 disease and sent to Weill Cornell for review-the pattern of hepatic injury was consistent with a ketamine-induced liver injury.
Ketamine is an NMDA receptor antagonist [1]. Its hallucinogenic and dissociative effects lend to abuse and make it popular at raves where it is known as “Special K”. The long-term effects of ketamine use are important to recognize as it is increasingly popular for treating chronic pain conditions [2,3]. As described elsewhere in the literature, ulcerative cystitis, hepatitis and biliary dilatation have been recognized as complications of chronic use.
Liver injury is known but cirrhosis directly resulting from ketamine alone is rarely reported [4].
A 22-year-old man with multiple prior admissions for management of erratic behaviour due to ketamine abuse was admitted to the ICU with AKI, HAGMA, lethargy and confusion. His parents at bedside provided valuable insight into his routine ketamine abuse-since age of 14 he has snorted 4 to 6mg of ketamine at least 3 times a week.
On presentation he was jaundiced without ascites and his urine was positive for ketamine metabolites. His INR was 2.5 and serum ammonia was 92 micromol/L. The albumin was 3.8 g/L, total bilirubin 6.7 mg/L (mostly direct), alk phos 818U/L, ALT 77U/L, AST 49U/L and serum creatinine of 10.6 mg/L.
His renal failure worsened, requiring temporary hemodialysis. ANA, ANCA, ceruloplasmin, ferritin, EBV, CMV-these were tested but did not contribute to aetiology. The anti-LKM level was elevated-our only serologic clue. Notably, this level can become elevated by drugs and toxins, especially when ketamine is involved [4]. An MRCP was negative for biliary sclerosis making PSC less likely. A liver biopsy was deemed necessary (Figure 1 and Figure 2).
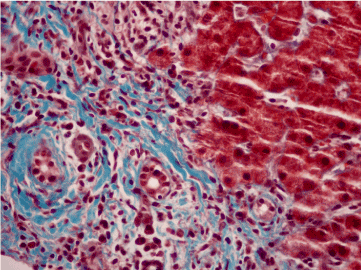
Figure 1. Liver biopsy 400x trichrome stain showing portal fibrosis
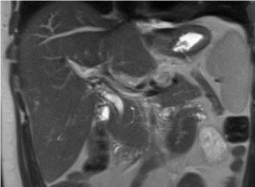
Figure 2. MRI with no evidence of biliary tree abnormality
He no longer required dialysis before hospital discharge. His jaundice and encephalopathy improved but did not completely normalize. He was scheduled for prompt follow up as an outpatient after discharge.
We report a case of chronic ketamine hepatopathy with acute liver injury/failure due to chronic illicit ketamine abuse. Liver biopsy findings, elevated anti-LKM levels and absence of PSC support this. There was no evidence for any viral, autoimmune or other toxic (Tylenol, alcohol) insult that could explain his pattern of injury. The pathologist noted specifically that the lymphocytic portal tract infiltration, ductular proliferation and atrophy as well as interface hepatitis and lack of iron deposition-in the absence of bile duct abnormalities on MRCP—was strongly suggestive of ketamine induced liver injury and our patient’s biopsy changes were nearly identical to prior pathological changes described in existing literature [6].
As ketamine is being used more frequently in the treatment of chronic pain (and being abused more by those seeking its dissociative properties) it follows that the clinician must learn to identify, understand and manage the potential hepatotoxicity of this anaesthetic agent. Every clinician should “mentally shelve” ketamine next to that old bottle of halothane [7].
- White JM, Ryan C (2009) Pharmacological properties of ketamine. Drug Alcohol Rev 15: 145-155. [Crossref]
- Noppers IM, Niesters M, Aarts LP, Bauer MC, Drewes AM, et al. (2012) Drug-induced liver injury following a reported course of ketamine treatment for chronic pain in CRPS type I patients. A report on 3 cases. Pain 152: 2173-2178. [Crossref]
- Sear JW (2011) Ketamine hepato-toxicity in chronic pain management: Another example of unexpected toxicity or a predicted result from previous clinical and preclinical data? Pain 152: 1946-1947. [Crossref]
- Wai MS, Chan WM, Zhang AQ, Wu Y, Yew DT (2012) Long-term ketamine and ketamine plus alcohol treatments produced damages in liver and kidney. Hum Exp Toxicol 31: 877-886. [Crossref]
- Wai MS (2009) Dilated common bile ducts mimicking choledochal cysts in ketamine. Hong Kong Med J 15: 53-56. [Crossref]
- Turkish A, Luo JJ, Lefkowitch JH (2013) Ketamine abuse, biliary tract disease, and secondary sclerosing cholangitis. Hepatology 58: 825-827. [Crossref]
- Neuberger J, Williams R (1984) Halothane anaesthesia and liver damage. Br Med J (Clin Res Ed) 289: 1136-1139.


