Introduction: Children with hemiplegia have a deficit in the motor behaviour that interferes with their spontaneous use and quality of movement in the affected upper limb due learn not to use of their affected arm, which is known as "Disregard of development" and the presence of incorrect movements and increased tone, as well as associated reactions or mirror movements.
Aim: To assess the spontaneous use and quality of movement in the affected upper limb in a girl with hemiplegia applying a modified constraint-induced movement therapy (mCIMT) protocol.
Clinical case and intervention: The protocol was applied for five weeks, two hours per day in a girl who is 5-year-old with right infantile hemiplegia, a level II in the manual ability classification system, MACS. Four measurements are used in the time. Spontaneous use is assessed by the Shriners Hospital Upper Extremity Evaluation, SHUEE and the quality of movement is also assessed by the Quality of Upper Extremity Skills Test, QUEST.
Results: The spontaneous use obtained an increase of 20% from first assessment to last assessment during 5 weeks of treatment, and the quality of life obtained an increase of 9.65% from the first measurement the highest increase was produced by the improvements in grip.
Conclusion: An increase in the spontaneous use and quality of movement of the paretic upper limb could possibly be obtained in the child when applying constraint-induced movement therapy in the usual environment.
infantile hemiplegia, neuroplasticity, physiotherapy specialty, exercise therapy, movement disorder.
Infantile cerebral palsy (ICP) is defined as a series of permanent disorders that affect the child's motor and postural development. Functional limitations occur in their motor activity, triggered by the brain injury produced during the maturation of the central nervous system of the fetus or infant. ICP is characterized as a non-progressive encephalopathy. It is a chronic sensorimotor disorder that leads to the alteration of sensitivity, perception, cognition, communication and behaviour, in addition causing changes in posture, muscle tone and production of inappropriate movements. These alterations are usually caused by secondary problems of cerebral palsy, such as epilepsy and musculoskeletal disorders, which is the same as those of the brain. The prevalence of ICP in developed countries is 2 to 2.5 cases per 1,000 live births [1].
Children with hemiplegia (subtype of ICP) are characterized by deficits in motor behaviour accompanied by stereotyped movements and poor postural adjustments that interfere with the balance, reaction time and speed of reaching an object. The movements are slower and with awkwardness in the coordination, longer during the execution, with associated and mirror movements. The presence of mirror movements hinders the coordination of the affected upper limb. In children with hemiplegia they are increased and prolonged in time by the lack of selective control and presence of spasticity altering the bimanual coordination, which leads to a decrease in the use of the affected hand that usually interferes with the hand ability of the healthy upper limb [2].
From the first stage of childhood, children with hemiplegia, even those with the least affectation, tend to use their healthy hand as dominant in all tasks. Therefore, they learn not to use their affected arm, which is known as "Disregard of development" [3] This "non-use" of their affected upper limb produces an increase in muscle tone in this body segment, poor motor control, decreased muscle range of active and passive movement, generalized weakness and delay of musculoskeletal maturation, altering the quality of movement due to the presence of incorrect movements and increased tone, as well as associated reactions or mirror movements. This deterioration of non-use is caused by a neural dysfunction during brain injury [4]. This neuronal alteration has the ability to improve by activating certain brain areas that remained inactive after the injury through activity and through experience and learning (trial-error) [3].
Constraint Induced movement therapy (CIMT) is an intervention technique to improve the use and functionality of the affected upper limb in patients with brain injury. It was described by Taub et al. [5]in 1980 and is based on "learning not to use the affected upper limb".
The therapy began to be applied in primates later transferring to adults and consisted in the restriction of the non-paretic upper limb through a means of containment (sling, splint...) thus promoting the use of the affected upper limb in the activities of daily life. The restraint was maintained during 90% of the waking hours. 6 consecutive hours of intensive treatment were performed in a clinic with exercises of manipulative skill during a period of 10 to 12 days. The tasks integrated the repetition of the motor action with a variety of exercises. This repetition allowed the acquisition of motor learning in the paretic hand [5,6].
Different studies [7–9] confirm that the merits acquired during the rehabilitation period were maintained between six months and one year after the intervention. After the application of Constraint Induced movement therapy following the use of the forgotten part, the stimulation of areas of the brain that had previously been inactivated by the use of the forgotten part was observed by means of magnetic resonance. An adaptation of the protocol is needed because most of the children did not complete the treatment because they did not exceed the full time of restriction, known as modified Constraint Induced movement therapy (mCIMT) [10,11].
Clinical case definition
The study is conducted on a 5-year-old girl who suffered brain damage during birth (perinatal injury) due to fetal distress. She was diagnosed with right spastic hemiplegia at 15 months of age when she attended day care, since inactivity was detected in the right upper extremity when performing bimanual tasks. Magnetic resonance diagnosis was confirmed, showing a cortico-subcortical lesion adjacent to the left central groove with gliosis foci and malacia. In addition, the ectatic Trolard vein is observed and, however, the lateral ventricles and third ventricle appear in a normal situation, size and morphology.
The girl has motor difficulties that show changes in the gait, of static and dynamic balance, obtaining an assessment on the scale of the case of Berg [12] independence (total score = 43) to be able to walk without limitations and not require a wheelchair. After an assessment of their motor skills, the girl is placed in level I of gross motor classification System in children with cerebral palsy, GMFCS [13].
There is a limitation of the manual functionality of the right upper extremity being found in a level II within the classification system of manual skill in children with cerebral palsy, MACS [14]. Its most pronounced deficit is manifested in fine motor skills, in the execution of manual motor skills with dexterity, and in the visual-motor coordination of the hand, since it requires a longer time to perform any activity.
In order to be able to apply the therapy, certain criteria of inclusion are considered [15].
- Lack of activity of the affected upper limb.
- Overcoming the 10º extension in the metacarpophalangeal and interphalangeal joints.
- Having more than 20º of extension of the wrist of the affected upper extremity.
- Adequate cognitive development to understand the verbal orders given for the execution of tasks.
- Cooperation in the execution of them.
The following were established as exclusion criteria:
- Have associated pathologies
- Have uncontrolled epilepsy
- Severe spasticity that prevents functional movement of the affected upper limb.
Method of intervention
The study is carried out in a period of 5 weeks of treatment, using a time of restriction of the healthy upper extremity of 2 hours per day (one hour in the morning and one hour in the afternoon) from Monday to Friday. An informed consent is given to the family for the execution of the therapy. The intervention protocol and informed consent were approved by the ethics committee of the San Pablo CEU University of Madrid.
The restriction used, is a partial, which consists of keeping the healthy hand closed and the thumb inside the fist by means of a transparent film that reaches the wrist joint, and that mimics the restriction of a glove [16] but it is more comfortable for the development of activities. Handling is prevented with the unaffected hand leaving the wrist and elbow joint free so that the girl can react to an external disturbance.
Both spontaneous use and the quality of movement of the affected upper limb were measured in four times as shown in figure 1.
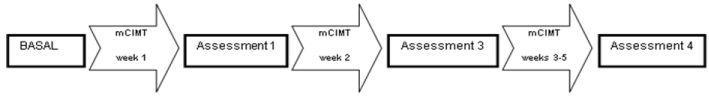
Figure 1.Description of the four measurements of both variables over time
Primary measures
Spontaneous use was assessed with the Shriners Hospital Upper Extremity Evaluation, Shuee Evaluation [17,18], which was used to record the values in the four measurements. This evaluation is based on the recording of videos of the girl performing a series of tasks to observe the hand functionality and the alignment of the joint segments of the affected upper limb in hemiplegic children in an age between 3 and 18 years. Spontaneous use is valued depending on the non-participation or active participation in the execution of 9 tasks:
- Remove bills from a wallet.
- Fold a paper.
- Tear a paper.
- Thread beads of a necklace.
- Unscrew a cap from a bottle.
- Separate plasticine with your hands.
- Cut plasticine with a knife.
- Put on your socks.
- Tying the laces.
The modified House scale is used for scoring tasks with a scale from 1 to 5, corresponding to 1 to 0% understood as the non-use of the affected limb in the task and the value 5 takes the value of 100% for the existence of spontaneous use from partial to complete.
Secondary measures
Quality of movement and bimanual dexterity were measured through the quality of upper extremity test, Quest scale [17,19,20]. It gives us a numerical value that is obtained from the average of the percentages in 36 items distributed in four categories: dissociated movements, grip, support and postural reactions of both upper limbs. It takes a value from 0 to 100 expressed in percentages. 100% being the maximum quality value of both upper extremities, measuring each upper limb separately but without making a distinction between healthy and affected upper limb in the final percentage of each category.
It was designed for children with neuromotor dysfunction with spasticity, in order to assess the quality of manual function in children with cerebral palsy. It is validated for children between 18 months and 8 years of age.
Data analysis
A descriptive analysis is made of all the dependent variables for each of the measurements, highlighting the most important differences during the measurement time.
Primary outcomes
It is the variable that suffers the most variation in the results, with a notable increase in its percentage from the first to the last measurement by 20% (Table 1 and Figure 2).
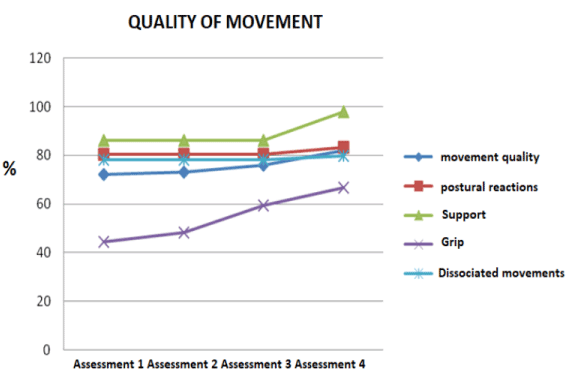
Figure 2.Progress the spontaneous use in affected upper limb for 4 measurements
Secondary outcomes
An increase in its value is obtained in each measurement executed. The difference between the values of the first measurement and the last one is accentuated, achieving an increase of 9.65% at the end of the intervention with mCIMT. This increase is determined to a greater extent by the changes originated in the grip that achieves an improvement of 22.26% from the first measurement. The dissociated movements, the supports and postural reactions also intervene in the increase of the percentage in the quality of movement and bimanual dexterity maintaining the values of the first to the third measurement and it is in the fourth measurement where the changes in the obtained results are appreciated obtaining an increase of 1.56% in the dissociated movements, 12% in the supports and 2.78% in the postural reactions (Table 2 and Figure 3).
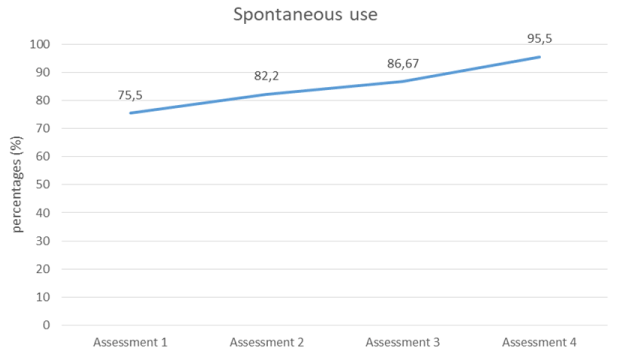
Figure 3.Progress the quality of movement in affected upper limb for 4 measurements
The deterioration of the functionality of the hand causes a weakness present in the execution of activities of daily life in infantile hemiplegia. There is an alteration compared to the healthy upper limb that manifests itself in the general slowness of movement, discontinuous movements, variability in the trajectory of movement and lack of spontaneous use and lack of quality of movement in the affected upper limb [21].
Benefits are obtained in each measurement produced by the acquisition of a more corrected posture of the trunk, head and shoulders in the execution of the grasping activities. These benefits are present from the second measurement (after one week of treatment with mCIMT). It increases the maintenance time of the supports of both upper limbs (greater than 2 seconds), observable in the last measurement after 5 weeks of intervention. It is produced by joint positioning in the wrist and elbow extension, which allows greater control and support of body structures.
The dissociated movements and the postural reactions do not show a remarkable percentage increase until the end of the intervention in the execution of the items in active elbow extension 0º, unlike the previous measurements where the dynamic articulation position of the elbow to carry out the task was 6º of active flexion.
Compared with the results obtained in the quality of movement of affected upper limb in the presented study, we highlight a study about mCIMT, which publishes positive results in the assessment of the quality of movement of motor skills (measured through the Quest scale) using an intervention protocol of 3 weeks of treatment with an intensity of 6 hours per day of restriction and repetitive work [22]. In the study, the effectiveness of the intervention is demonstrated, since it is a larger sample and has a control group (18 hemiplegic children, 9 children experimental group and 9 children control group), unlike the case presented. In 2011, another investigation [23], this time made exclusively with a hemiplegic girl with characteristics similar to the girl's study, employs mCIMT for one hour per day for two weeks. At the end of the treatment, no important results are obtained, so it is extended to one more week of intervention. In this last assessment, an increase in the overall percentage of the total movement quality (also measured by the Quest scale) is recorded, which is appreciable in activities of the affected upper limb. The percentage increase in the variable studied from the first measurement to the last is greater than that obtained in the present study, since the girl started from a lower condition in the motor skills than the girl in this current study. If we make comparisons with the values of the study from the second measurement that resemble the initial motor condition of the case presented in this study, there is a greater increase in our study, which may be due to the use of a mCIMT protocol of greater intensity and duration. Thus, the protocol chosen for the intervention and the initial functionality of the patient are two important factors to be taken into account in the increase of the results obtained in the measurements.
The learning of the "non-use" of the affected upper limb through the intervention with mCIMT can provide an increase of spontaneous participation of the affected upper limb in the unimanual and bimanual tasks observed in all the measurements carried out through Shuee evaluation throughout the intervention time [24]. There is an increase of 20% in the performance of the affected upper limb from the first measurement to the last one. Before the intervention, the girl used her paretic limb in most actions for the active and stable grip of the object that was manipulated with the healthy hand. At the end of the intervention there is a spontaneous use of partial to full in most bimanual activities facilitating the activities into her family and school environment (data added by the parents and school teacher of the girl). In this way, the girl can use the affected hand spontaneously or without the reference of the other hand. The improvement in functional performance is reflected in the activities of daily life where She performs with independence, but higher quality the tasks of dressing and undressing, putting on socks and shoes with active participation of the affected upper limb. The parents provide information about the act of feeding, commenting that the girl uses her affected upper limb to give active support to the healthy limb, without the need for them to give a verbal order for its use, without any reference. Previously, the affected upper limb remained inactive under the table during the act of feeding, without any collaboration in it, performed exclusively by the healthy hand.
Being an uncontrolled trial with a single case and absence of a control group, it cannot be guaranteed that the response observed (changes produced throughout the intervention with respect to the baseline situation) is exclusively due to the mCIMT protocol [25].
For future research it would be necessary to expand the simple applying the same protocol and introducing a control group.
An increase in spontaneous use and quality of movement in the affected upper limb could possibly be obtained in the girl with right infantile hemiplegia when applying modified Constraint induced movement therapy into the usual environment.
Acknowledge the involvement of girl’s family in the study and the girl herself great interest and desire for improvement.
- Monge E, Molina F, Alguacil IM, Cano R, De Mauro A, et al. (2012) Use of virtual reality systems as proprioception method in cerebral palsy: clinical practice guideline. Neurologia 318: 1-10. [Crossref]
- Camacho-Salas A (2008) Infantile cerebral palsy: the importance of population registers. Rev Neurol 47: 15-20. [Crossref]
- Deluca SC, Echols K, Law CR, Ramey SL (2006) Intensive pediatric constraint-induced therapy for children with cerebral palsy: randomized, controlled, crossover trial. J Child Neurol 21: 931-938. [Crossref]
- Liepert J, Bauder H, Wolfgang HR, Miltner WH, Taub E, et al. (2000) Treatment-induced cortical reorganization after stroke in humans. Stroke 31: 1210-1216. [Crossref]
- Taub E, Harger M, Grier HC, Hodos W (1980) Some anatomical observations following chronic dorsal rhizotomy in monkeys. Neurosci 5: 389-401. [Crossref]
- Taub E, Miller NE, Novack TA, Cook EW 3rd, Fleming WC, et al. (1993) Technique to improve chronic motor deficit after stroke. Arch Phys Med Rehabil 74: 347-354. [Crossref]
- Naylor CE, Bower E (2005) Modified constraint-induced movement therapy for Young children with hemiplegic cerebral palsy: a pilot study. Dev Med Child Neurol 47: 365-369. [Crossref]
- Charles JR, Wolf SL, Schneider JA, Gordon AM (2006) Efficacy of a child-friendly form of constraint-induced movement therapy in hemiplegic cerebral palsy: a randomized control trial. Dev Med Child Neurol 48: 635-642. [Crossref]
- Sakzewski L, Provan K, Ziviani J, Boyd RN (2015) Comparison of dosage of intensive upper limb therapy for children with unilateral cerebral palsy: how big should the therapy pill be? Res Dev Disabil 37: 9-16. [Crossref]
- Wallen M, Ziviani J, Herbert R, Evans R, Novak I (2008) Modified constraint-induced therapy for children with hemiplegic cerebral palsy: a feasibility study. Dev Neurorehabil 11: 124-133.
- DeLuca SC, Case-Smith J, Stevenson R, Ramey SL (2012) Constraint-induced movement therapy (CIMT) for young children with cerebral palsy: effects of therapeutic dosage. J Pediatr Rehabil Med 5: 133-142. [Crossref]
- Kembhavi G, Darrah J, Magill J, Loomis J (2002) Using the berg balance scale to distinguish balance abilities in children with cerebral palsy. Pediatr Phys Ther 14: 92-99. [Crossref]
- Gray L, Ng H, Bartlett D (2010) The gross motor function classification system: an update on impact and clinical utility. Pediatr Phys Ther 22: 315-320. [Crossref]
- Eliasson AC, Krumlinde L, Rösblad B, Beckung E, Arner M, et al. (2006) The Manual Ability Classification System (MACS) for children with cerebral palsy: scale development and evidence of validity and reliability. Dev Med Child Neurol 48: 549-554. [Crossref]
- Ramachandran S, Thakur P (2011) Upper extremity constraint-induced movement therapy in infantile hemiplegia. J Pediatr Neurosci 6: 29-31. [Crossref]
- Eliasson AC, Krumlinde L, Shaw K, Wang C (2005) Effects of constraint-induced movement therapy in young children with hemiplegic cerebral palsy: an adapted model. Dev Med Child Neurol 47: 266-275. [Crossref]
- Gilmore R, Sakzewski L, Boyd R (2010) Upper limb activity measures for 5- to 16-year-old children with congenital hemiplegia: a systematic review. Dev Med Child Neurol 52: 14-21. [Corssref]
- Davids JR, Peace LC, Wagner LV, Gidewall MA, Blackhurst DW, et al. (2006) Validation of the Shriners Hospital for Children Upper Extremity Evaluation (SHUEE) for children with hemiplegic cerebral palsy. J Bone Joint Surg Am 88: 326-333. [Crossref]
- DeMatteo C, Law M, Russell D, Pollock N, Rosenbaum P, et al. (1983) The reliability and validity of Quality of Upper Extremity Skills Test. Phys Occup Ther Pediatr 13: 1-18.
- Thorley M, Lannin N, Cusick A, Novak I, Boyd R (2012) Reliability of the quality of upper extremity skills test for children with cerebral palsy aged 2 to 12 years. Phys Occup Ther Pediatr 32: 4-21. [Crossref]
- Steenbergen B, Charles J, Gordon AM (2008) Fingertip force control during bimanual object lifting in hemiplegic cerebral palsy. Exp Brain Res 186: 191-201. [Crossref]
- Pidcock FS, Garcia T, Trovato MK, Schultz S, Brady KD (2009) Pediatric constraint-induced movement therapy: a promising intervention for childhood hemiparesis. Top Stroke Rehabil 16: 339-345. [Crossref]
- Ramachandran S, Thakur P (2011) Upper extremity constraint-induced movement therapy in infantile hemiplegia. J Pediatr Neurosci 6: 29-31. [Crossref]
- Schweighofer N, Han CE, Wolf SL, Arbib MA, Winstein CJ (2009) A functional threshold for long-term use of hand and arm function can be determined: predictions from a computational model and supporting data from the Extremity Constraint-Induced Therapy Evaluation (EXCITE) Trial. Phys Ther 89: 1327-1336. [Crossref]
- Argimon JMª, Jiménez J. Methods of clinical and epidemiological research. Elsevier Third edition.



