Introduction: Minimal paravalvular leaks (PVLs) through microdefects around the annulus have been demonstrated immediately after valvular replacement surgery and usually disappear after regional tissue healing. It has been recognized that endothelium takes place in some pathological process during wound healing. In this study we aimed to investigate the role of endothelial functions in patients with persistent PVLs detected in the early postoperative period.
Methods: This study enrolled a total of 33 patients (14 female, mean age: 47.9±10.4 years) who had PVL detected by means of transesophageal echocardiography (TEE) within 3 months after prosthetic valve replacements, and 40 control subjects (19 female, mean age: 49.9±13.0 years) without PVL in the early postoperative period. Endothelial functions were evaluated by measurement of endothelium-dependent flow- mediated dilation (FMD) secondary to reactive hyperemia.
Results: The demographic, echocardiographic and laboratory parameters did not differ between the groups except for lactate dehydrogenase levels which were higher in PVL group. Calculated FMD values were found to be significantly lower in PVL group than the control group (12.9±1.8 vs 13.8±1.6 %; p=0.022). In the receiver operating characteristic curve analysis, FMD values below 12.8% predicted PVL formation with a sensitivity of 55%, and a specificity of 31% (area under curve= 0.355, p=0.034). There was a weak and negative correlation between FMD values and the number of paravalvular defects (r= -0.246 ; p=0.036).
Conclusion: Endothelial dysfunction in patients with prosthetic heart valves may play an important role in the development of PVLs during the early postoperative period.
Echocardiography, Cardiac imaging, Cardiac surgery, Transesophageal echocardiography
Paravalvular leaks (PVLs) are potential complications of mitral valve replacement. Most are asymptomatic and benign, but some may cause symptoms due to heart failure, arrhythmia, endocarditis or hemolysis. Although surgical procedures have been well established, and recent technological advances have led to more hemodynamically efficient prosthetic heart valves, PVL is still an unavoidable complication of prosthetic valve implantation [1,2]. PVLs occur with an incidence of 2–10% in the aortic position and 7–17% in the mitral position [3,4]. The PVL incidence is much higher with mechanical than with bioprosthetic valves [5,6]. PVLs may be seen either immediately after valve replacement in the operating room or during the follow-up period. The immediate PVLs are usually associated with technical difficulties related to calcification of the native annulus. Late PVLs are commonly a consequence of suture dehiscence [7] caused by prosthetic valvular endocarditis or gradual reabsorption of incompletely debrided annular calcifications [8].
Minimal paravalvular leaks through microdefects around the annulus and the insertion points of the sutures have been demonstrated immediately after valvular replacement surgery and they usually disappear after regional tissue healing during the early postoperative period [9]. The vascular endothelium secretes numerous factors which regulate cell growth, vascular tone, platelet and leukocyte interactions and thrombogenicity. It has been recognized that endothelium takes place in some pathological process during wound healing including mitogenesis, fibrosis, vascular hypertrophy, and inflammation [10]. Endothelial dysfunction has been associated with various cardiovascular disorders. Persistence of small paravalvular leaks described in the early postoperative period may be secondary to endothelial dysfunction.
In this study, we aimed to investigate the endothelial functions by using a noninvasive method evaluating endothelium-dependent flow mediated dilation (FMD) in the brachial artery, in patients with prosthetic heart valves who had paravalvular leak detected in the early postoperative period.
Study Population
Between January 2012 and December 2013, 33 patients (14 female, mean age: 47.9±10.4 years) who had persistent PVL detected by transesophageal echocardiograpy (TEE) within 3 months after prosthetic valve replacements, and 40 control subjects (19 female, mean age: 49.9±13.0 years) without PVL in the early postoperative period as confirmed by TEE were enrolled in this single-center case-control study. Patients with left ventricular systolic dysfunction (ejection fraction < 40%), end-stage liver disorders, renal insufficiency, chronic inflammatory diseases, connective tissue diseases, infective endocarditis, coronary artery disease, diabetes mellitus, smoking and malignancies were excluded from the study. Early postoperative period was defined as the 3 months after the heart valve replacement surgery. Complete blood count and blood chemistry panel were carried out in all patients at the time of admission. All patients provided a written informed consent and the study protocol was approved by the local ethics committee of the hospital in accordance with the Declaration of Helsinki and Good Clinical Practice guidelines.
Echocardiography
Complete transthoracic echocardiography (TTE), two-dimensional (2D) and real-time three-dimensional (RT-3D) TEE studies (Philips iE33, Philips Medical System, Andover, MA, USA) were performed in all patients for the evaluation of prosthetic valves. Parasternal long axis and short axis views and apical five chamber view were used during TTE evaluation. Transmitral gradients and effective orifice area were measured with 2D TTE according to the current guidelines [11]. A TEE study was scheduled when there was an echocardiographic and/or clinical suspicion of PVL. During TEE study, PVL was assessed using several views including upper esophageal 5-chamber view, mid-oesophageal long and short-axis views, and the transgastric view as described in previous recommendations [12]. A high-velocity, eccentric turbulent jet with its origin beyond the edge of the sewing ring was considered as PVL (Figure 1A and 1B). A laminar, low-velocity regurgitant jet with its origin within the orifice of the sewing ring was considered transvalvular [13]. Color-flow Doppler was used to localize and determine the severity of PVL [11]. The longest diameter and the area of the paravalvular defects were measured on RT-3D TEE recordings (Figure 1C).
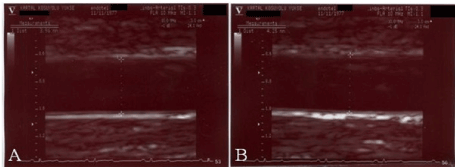
Figure 1. Two-dimensional transoesophageal echocardiography revealing a paravalvular leak as a high-velocity, eccentric turbulent jet with its origin beyond the edge of the sewing ring (A and B). Real time three dimensional transoesophageal echocardiography image with left atrial perspective illustrating the measurement of paravalvular defect sizes (C).
Vascular Assessment of FMD
All patients were studied at least 12 h after their last meal, according to a standard protocol previously described [14]. Patients were put in supine position for 10 min at rest before the measurement. The right arm was fixed in extended, relaxed position to provide correct analysis of the brachial artery 2–5 cm above the antecubital fossa. Then, brachial artery was monitorized longitudinally via a 17–5 MHz linear array ultrasound transducer (General Electric Vivid 5, Horten, Norway). The brachial artery was scanned in longitudinal section, the focus zone was set to optimize images of the lumen-arterial wall interface, and machine operating parameters were not changed during the rest of the study. Measurements were taken from the anterior to posterior “m” line at end diastole, incident with the R wave on the electrocardiography (Figure 2). Three cardiac cycles (in patients with atrial fibrillation seven cardiac cycles) were analyzed for each scan, and measurements were averaged. A baseline brachial artery diameter was evaluated, and a cuff placed around the forearm distal to the scanned artery segment was inflated to about 30 mmHg above the systemic systolic arterial pressure for five minutes. Maximal brachial artery diameter was established from six enrollments taken every minute after the cuff release. The percentage FMD was calculated via the formula: FMD (%) = (maximum diameter − baseline diameter)/baseline diameter × 100).
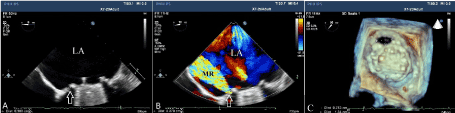
Figure 2. Measurement of brachial artery diameter at end diastole when maximum lumen diameter was visualized longitudinally using a linear array transducer before (A) and after (B) reactive hyperemia induced flow mediated dilatation.
Statistical Analysis
Statistical analyses were performed using IBM SPSS Statistics for Windows, Version 19.0. (IBM Corp. Armonk, NY). Descriptive statistics are reported as mean ± standard deviation for continuous variables with normal distribution or median (25th-75th percentiles) values for continuous variables without normal distribution and as frequency with percentages for the categorical variables. The Shapiro-Wilk test was used to test the normality of the distribution of continuous variables. Student t test or Mann- Whitney U test was used to compare continuous variables as appropriate. Categorical variables were compared using the Chi-square test. The significance level was accepted as p<0.05 in all statistical analyses. Correlational analyses were performed using Pearson or Spearmen’s correlation tests as appropriate. A logistic regression analysis was performed in order to identify any independent predictors of PVL development. A receiver operating characteristic (ROC) curve analysis was performed to assess the sensitivity, specificity, area under the curve (AUC) and confidence interval (CI) of best FMD cut-off values for predicting PVL development.
The study population consisted of 33 PVL patients (14 female, mean age: 47.9±10.4 years) and 40 control patients (19 female, mean age: 49.9±13.0 years). The PVL group included 6 aortic, 24 mitral and 3 aortic+mitral valve patients, while, the control group included 7 aortic, 28 mitral and 5 aortic+mitral valve patients. There were 26 mitral and 7 aortic PVLs in the patient group and the severity of PVLs was mild in 6, moderate in 16 and severe in 11 patients. The 7 aortic PVL patient had only one paravalvular defect, whereas, among mitral PVL patients, 18 patients had only one paravalvular defect, 8 patients had 2 paravalvular defects and 1patient had 3 paravalvular defects. The mean paravalvular defect area was 0.15 (0.10-0.20) cm2 in aortic valves and 0.35 (0.20-0.80) cm2 in mitral valves.
The clinical and demographical characteristics of the two groups are presented in Table 1. The elapsed time since valve surgery was 47.5±18.9 days in the PVL group and 46.5±14.9 days in the control group. Left ventricular ejection fraction in patient and control groups were 57.5±7.6 % and 60±6.9 % respectively. There was no significant difference between groups in terms of age, gender, prosthetic valve type and position, cardiac rhythm, left ventricular ejection fraction, elapsed time since valve surgery, re-do valve surgery and surgical teams. The surgical technique and used pledgeted sutures were similar in all study population. The transaortic and transmitral gradients obtained by TTE were compared between the groups. Comparison of laboratory parameters between the groups were included in Table 2. There was no significant difference in terms of laboratory parameters between the groups except for lactate dehydrogenase which were significantly higher in the PVL group.
The percentage of FMD was significantly lower in PVL group as compared to controls (12.9±1.8 vs. 13.8±1.6 %; p=0.022) (Figure 3A). There was a weak and negative correlation between FMD values and the number of paravalvular defects (r= -0.246 ; p=0.036). The univariate parameters which were possible predictors of PVL development were taken into multiple logistic regression analysis (Table 3). Low percentage of FMD was the only independent predictor of PVL development (Odds ratio: 1.452 ; CI%95: 1.053-2.003; p=0.023). In the ROC curve analysis, FMD values below 12.8% predicted PVL formation with a sensitivity of 55%, and a specificity of 31% (AUC= 0.355, p=0.034) (Figure 3B).
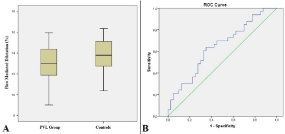
Figure 3. The box-plot graph comparing the percentages of flow mediated dilatation between paravalvular leak group and the controls (A) receiver operating characteristic curve revealing the area under the curve for FMD to predict PVL development.
Table 1. Comparison of the clinical and demographical characteristics between PVL group and controls.
|
PVL Group
(n:33) |
Controls
(n:40) |
P value |
Age, years |
47.9±10.4 |
49.9±13.0 |
0.235 |
Gender, n(%)
Male
Female |
19 (57.6)
14 (42.4) |
21 (52.5)
19 (47.5) |
0.665 |
Valve Position, n(%)
Mitral
Aort
Aort+Mitral |
24 (72.7)
6 (18.2)
3 (9.1) |
28 (70)
7 (17.5)
5 (12.5) |
0.895 |
Valve Type, n(%)
St.Jude Med.
Carbomedics
ATS |
17 (47.3)
10 (27.7)
9 (25) |
18 (40)
14 (31.1)
13 (28.9) |
0.876 |
Cardiac rhythm, n(%)
NSR
AF |
14 (42.4)
19 (57.6) |
19 (47.5)
21 (52.5) |
0.665 |
ETSVS (days) |
47.5±18.9 |
46.5±14.9 |
0.920 |
LV EF (%) |
57.5±7.6 |
60±6.9 |
0.154 |
Surgical Teams, n(%)
1
2
3
4
5
6
7 |
3 (9.1)
7 (21.2)
4 (12.1)
6 (18.2)
7 (21.2)
5 (15.2)
1 (3) |
4 (10)
8 (20)
6 (15)
4 (10)
8 (20)
9 (22.5)
1 (2.5) |
0.955 |
Re-do Surgery, n(%) |
8(24.2) |
5(17.5) |
0.478 |
AF: Atrial fibrillation, ETSVS: Elapsed time since valve surgery, LV EF: Left vetricular ejection fraction, NSR: Normal sinus rhythm, PVL: Paravalvular leak
Table 2. Comparison of laboratory parameters between PVL group and controls.
|
PVL Group
(n:33) |
Controls
(n:40) |
P value |
White Blood Cell, (x103/dL) |
7.9 (6.1-9.5) |
8.2 (5.9-10.8) |
0.756 |
Hemoglobin (g/dL) |
11.7±1.8 |
11.9±2.3 |
0.630 |
Platelet, (x103/dL) |
277.8±112.8 |
235.9±70.1 |
0.210 |
Glucose, (mg/dL) |
108.3±25.7 |
122.9±44.1 |
0.267 |
BUN, (g/dL) |
27.6±9.6 |
33.4±12.3 |
0.224 |
Creatinine, (g/dL) |
0.8±0.2 |
1.4±1.5 |
0.065 |
Uric Acid (mg/dL) |
5.2±2.2 |
5.3±2.1 |
0.752 |
AST, (U/L) |
21 (17.75-26) |
20.5(18-23.75) |
0.501 |
ALT, (U/L) |
21 (13.75-29.25) |
21(16-29.5) |
0.997 |
LDH, (U/L) |
602 (486-1080) |
324 (244-383) |
<0.001 |
Albumin, (g/dL) |
4.1±0.5 |
4.1±0.7 |
0.705 |
INR |
2.5±0.5 |
2.4±0.6 |
0.573 |
Table 3. Multivariate regression analysis of possible predictors of paravalvular leak development.
| |
OR |
95% CI |
p value |
Age |
0.981 |
0.938 – 1.026 |
0.409 |
Gender |
0.750 |
0.260 - 2.163 |
0.594 |
LV EF (%) |
0.952 |
0.885 - 1.025 |
0.194 |
Valve position |
1.311 |
0.378 - 4.564 |
0.671 |
Valve type |
0.796 |
0.430 - 1.474 |
0.469 |
Surgical team |
0.971 |
0.722 - 1.308 |
0.849 |
Re-do surgery |
3.434 |
0.840 – 14.034 |
0.086 |
Low FMD (%) |
1.452 |
1.053 - 2.003 |
0.023 |
CI: Confidence Interval; FMD: Flow mediated dilatation, LV EF: Left ventricular ejection fraction, OR: Odds ratio
In this observational case-control study, we have focused on the role of endothelial dysfunction in the development of PVLs in the early postoperative period after mitral valve replacement surgery. Endothelium-dependent reactive hyperemia induced FMD in the brachial arteries of PVL patients were significantly lower than the controls. Endothelial dysfunction in patients with prosthetic heart valves may play an important role in the development of paravalvular leaks during the early postoperative period.
PVL is not a rare complication of valve replacement surgery. PVLs are twice as likely to occur with mitral than with aortic prosthesis [15]. The underlying causes for early PVLs are suture knot failure, inadequate suture placement, or separation of sutures from a pathologic annulus in endocarditis with ring abscess, myxomatous valvular degeneration and anomalous tissue retraction from the sewing ring [16]. PVLs may be clinically asymptomatic or may aggravate hemolysis or cause heart failure in case of moderate to severe regurgitation [17]. Small leaks without hemolysis may be left unrepaired without increased mortality and are managed with medical therapy, whereas repeat surgery, either resuturing or replacing the original prosthesis, remains the treatment of choice for symptomatic PVLs, particularly when associated with heart failure, hemolytic anemia or functional decline [15]. In the last decade percutaneous PVL closure has also provided promising results in the management of moderate to severe PVLs [18]. Echocardiographic guidance is crucial for success of interventional procedures including surgical repair and percutaneous closure [19].
The endothelium is a large paracrine organ that secretes a variety of factors for regulation of vascular tone, cell growth, platelet and leukocyte interactions and thrombogenicity [10]. The endothelium can sense and respond to numerous internal and external stimuli via cell membrane receptors and signal transduction mechanisms, leading to the synthesis and release of various vasoactive, thromboregulatory and growth factor substances. It has been recognized that endothelium takes place in some pathological process during wound healing including mitogenesis, fibrosis, vascular hypertrophy, and inflammation. A noninvasive technique has been widely used to evaluate flow-mediated vasodilation, an endothelium-dependent function, in the brachial artery [20]. In this technique, reactive hyperemia induced nitric oxide release is provoked, and subsequent vasodilation is imaged and quantitated as an index of endothelial function. Endothelial dysfunction plays an important role in the development of cardiovascular diseases such as atherosclerosis, hypertension, and heart failure [21,22]. In a previous study, it was reported that patients with prosthetic heart valve thrombosis had endothelial dysfunction which might contribute to the development of thrombosis [23]. However, endothelial functions have never been investigated in PVL patients up to date and to the best of our knowledge this is the first study in this field.
In the current study, endothelial functions assessed by the measurement of reactive hyperemia induced FMD were worse in the PVL patients than the controls. Furthermore, low FMD, or in other words, endothelial dysfunction was an independent predictor of early PVL development and also there was an association between FMD and the number of paravalvular defects. Since endothelium plays an important role during wound healing regulating mitogenesis and fibrosis, endothelial dysfunction may be associated with the persistance of paravalvular leaks during the early postoperative period.
The primary limitation was that our study was a nonrandomized, observational and single center study with a relatively small number of patients.
Endothelium-dependent reactive hyperemia induced FMD in the brachial arteries of PVL patients were significantly lower than the controls. Endothelial dysfunction in patients with prosthetic heart valves may play an important role in the development of paravalvular leaks during the early postoperative period
All of the authors have no conflict of interest.
The author(s) received no financial support for the research, authorship, and/or publication of this article.
- De Cicco G, Russo C, Moreo A, Beghi C, Fucci C, et al. (2006) Mitral valve periprosthetic leakage: Anatomical observations in 135 patients from a multicentre study. Eur J Cardiothorac Surg 30: 887-891. [Crossref]
- Kuwabara F, Usui A, Araki Y, Narita Y, Mizutani S, et al. (2011) Pathogenesis of paravalvular leakage as a complication occurring in the late phase after surgery. J Artif Organs 14: 201-208.
- Hammermeister K, Sethi GK, Henderson WG, Grover FL, Oprian C, et al. (2000) Outcomes 15 years after valve replacement with a mechanical versus a bioprosthetic valve: Final report of the veterans affairs randomized trial. J Am Coll Cardiol 36: 1152–1158. [Crossref]
- Ionescu A, Fraser AG, Butchart EG (2003) Prevalence and clinical significance of incidental paraprosthetic valvar regurgitation: a prospective study using transoesophageal echocardiography. Heart 89: 1316–1321. [Crossref]
- Khan SS, Trento A, DeRobertis M, Kass RM, Sandhu M, et al. (2001) Twenty-year comparison of tissue and mechanical valve replacement. J Thorac Cardiovasc Surg 122: 257-269. [Crossref]
- Wąsowicz M, Meineri M, Djaiani G, Mitsakakis N, Hegazi N, et al. (2011) Early complications and immediate postoperative outcomes of paravalvular leaks after valve replacement surgery. J Cardiothorac Vasc Anesth 25: 610-614. [Crossref]
- Dhasmana JP, Blackstone EH, Kirklin JW, Kouchoukos NT (1983) Factors associated with periprosthetic leakage following primary mitral valve replacement: with special consideration of the suture technique. Ann Thorac Surg 35: 170-178. [Crossref]
- Pate GE, Al Zubaidi A, Chandavimol M, Thompson CR, Munt BI, et al. (2006) Percutaneous closure of prosthetic paravalvular leaks: case series and review. Catheter Cardiovasc Interv 68: 528-533. [Crossref]
- Bonnefoy E, Perinetti M, Girard C, Robin J, Ninet J, et al. (1995) Systematic transesophageal echocardiography during the postoperative first 24 hours after mitral valve replacement. Arch Mal Coeur Vaiss 88: 315-319. [Crossref]
- Verma S, Anderson TJ (2002) Fundamentals of endothelial function for the clinical cardiologist. Circulation 105: 546-549. [Crossref]
- Zoghbi WA, Chambers JB, Dumesnil JG, Foster E, Gottdiener JS, et al. (2009) Recommendations for evaluation of prosthetic valves with echocardiography and Doppler ultrasound. J Am Soc Echocardiogr 22: 975-1014. [Crossref]
- Zamorano JL, Badano LP, Bruce C, Chan KL, Gonçalves A, et al. (2011) EAE/ASE recommendations for the use of echocardiography in new transcatheter interventions for valvular heart disease. Eur Heart J 32: 2189-2194. [Crossref]
- Cho IJ, Moon J, Shim CY, Jang Y, Chung N, et al. (2011) Different clinical outcome of paravalvular leakage after aortic or mitral valve replacement. Am J Cardiol 107: 280-284. [Crossref]
- Corretti MC, Anderson TJ, Benjamin EJ, Celermajer D, Charbonneau F, et al. (2002) Guidelines for the ultrasound assessment of endothelial-dependent flow-mediated vasodilation of the brachial artery: a report of the International Brachial Artery Reactivity Task Force. J Am Coll Cardiol 39: 257-265. [Crossref]
- Cappelli F, Del Bene MR, Santoro G, Meucci F, Attanà P, et al. (2011) The challenge of integrated echocardiographic approach in percutaneous closure of paravalvular leak. Echocardiography 28: E168-71. [Crossref]
- Kirali K, Mansuroglu D, Yaymaci B, Omeroglu SN, Basaran Y, et al. (2001) Paravalvular leakage after mitral valve replacement: is left atrial enlargement an additional indication for reoperation? J Heart Valve Dis 10: 418-425. [Crossref]
- Gürsoy OM, Astarcıoğlu MA, Gökdeniz T, Aykan AC, Bayram Z, et al. (2013) Severe mitral paravalvular leakage: echo-morphologic description of 47 patients from real-time three-dimensional transesophageal echocardiography perspective. Anadolu Kardiyol Derg 13: 633-640. [Crossref]
- Kliger C, Eiros R, Isasti G, Einhorn B, Jelnin V, et al. (2013) Review of surgical prosthetic paravalvular leaks: diagnosis and catheter-based closure. Eur Heart J 34: 638-649. [Crossref]
- Özkan M, Gürsoy OM, Astarcıoğlu MA, Wunderlich N, Sievert H (2012) Percutaneous closure of paravalvular mitral regurgitation with Vascular Plug III under the guidance of real time 3 dimensional transesophageal echocardiography. Turk Kardiyol Dern Ars 40: 632-641. [Crossref]
- Anderson EA, Mark AL (1989) Flow-mediated and reflex changes in large peripheral artery tone in humans. Circulation 79: 93-100. [Crossref]
- Laurent S, Lacolley P, Brunel P, Laloux B, Pannier B, et al. (1990) Flow-dependent vasodilation of brachial artery in essential hypertension. Am J Physiol 258: H1004-1011. [Crossref]
- Celermajer DS, Sorensen KE, Gooch VM, Spiegelhalter DJ, Miller OI, et al. (1992) Non-invasive detection of endothelial dysfunction in children and adults at risk of atherosclerosis. Lancet 340: 1111-1115. [Crossref]
- Kaya H, Ozkan M, Yildiz M (2013) Relationship between endothelial dysfunction and prosthetic heart valve thrombosis: a preliminary investigation. Eur Rev Med Pharmacol Sci 17: 1594-1598. [Crossref]



