A study of wholistic practices outcomes among people with disabilities was conducted. The evaluative question was whether the participants were “better off” after beginning Wholistic Practices sessions. The participants were people with intellectual and mental disabilities in community living situations who had experienced challenges in behavior, mood, and/or quality of life that had resisted other interventions for many years.
The utilization of wholistic or alternative therapies has burgeoned in the past decade among people of advanced age, people with physical and medical conditions, and people with mental illnesses. It is no longer unusual to find alternative and massage techniques available in major hospitals and addiction centers. However, the application of these approaches among people with intellectual and developmental disabilities has been documented in only one prior study. The present study was an attempt to replicate the first.
This study should be considered a pilot or “case study” because the participants were purposefully selected, the sample was small, surrogate respondents were required for many participants who were non-verbal, and the design lacked a control group. Nonetheless, the results of this pilot study were positive. The quantitative data showed statistically significant improvements in 5 out of 15 major life quality areas – and an increase in an overall quality of life scale computed from the 15 areas. The qualitative data indicated strong approval of Wholistic Practices coupled with desire for continuation.
The present study revealed strong reasons to continue and expand the implementation of wholistic practices, and equally important, to include rigorous scientific outcome evaluation to provide the evidence necessary for advocates and skeptics alike. The system should vigorously pursue the possibility that there is a useful and economical innovation available to assist ‘difficult to support’ people in their everyday lives.
Intellectual disability, mental disability, massage, Wholistic, touch, behavior
The Independent Outcome Evaluation of the Pennsylvania Wholistic Practices[1] Initiative was intended to test whether the participants were “better off” after they begin. To do this, we measured qualities of life before or near the beginning of their involvement, relying on the reports of the participants and the people closest to them. Then, after the “sessions”[2] have begun, we measured qualities of life again. Comparing the before to the after measurements will show whether people are better off – as well as in what ways, and how much.[3]In scientific jargon, this is a variant of the Pre-Post No-Control Outcome design.
The nonprofit agency Networks for Training and Development[4] began its second Demonstration effort to explore the use of Wholistic Practices among people with the labels of intellectual and developmental disabilities in early 2016. [5]The Center for Outcome Analysis scientific group visited with and interviewed each of the participants at least twice to detect evidence of the outcomes, including quality of life changes.
This report is intended to contribute to the scientific body of knowledge about the utility of the nontraditional Wholistic Practices among people with intellectual and developmental disabilities, particularly those who are experiencing difficulty with emotions or behaviors. In the Networks demonstrations in two Pennsylvania counties, small numbers of people having difficulty were referred or self-referred to the Wholistic interventions because other approaches (behavioral, medical, chemical) were not successful.
System stakeholders, including administrators, managers, workers, families, and the people receiving supports, saw an attractive chance that a new and innovative intervention might have positive outcomes. The Wholistic practices were seen to have the potential to be helpful, but at much lower cost – and much less fraught with restrictiveness, risk, and side effects – than the traditional behavioral, medical, or chemical approaches. But evidence of the hoped-for success of the alternative intervention would be needed to be sure that the Wholistic approaches ‘work.’ Hence the outcome studies described here were initiated along with the demonstration.
Western medicine has traditionally been based on the notion that the body can be “repaired” via physical means, and has tended strongly toward a mechanistic view of the world. Western medicine has been strongly skeptical of treatments and methods that are outside its current empirical base. It has often attacked alternatives as unproven, and more strongly as quackery, snake oil, and unscientific.
More recently, alternatives have gained somewhat grudging recognition. This has taken place in view of a burgeoning scientific literature that shows widespread use, and positive results, from non-traditional approaches. For example, the National Center for Complementary and Integrative Health (NCCIH) was founded in 1998 as part of the National Institutes for Health.
The current research with Networks for Training is intended to review the scientific literature on Wholistic Practices as applied with innovative populations, and to conduct new research on the outcomes of applying such practices with people who have intellectual and developmental disabilities.
In Western societies, the application of therapeutic and health-promoting techniques that involve touch and energy are considered non-traditional, and have been met with considerable skepticism and resistance from Western professional health practitioners [1]. They are generally considered to need much more solid evidence of their efficacy before being applied – or even permitted.
The most widely known example is acupuncture. Acupuncture has been used for thousands of years – medical historians differ in their estimates from 2,000 to 6,000 years – and it has survived in the mainstream of health work in China and other Asian locales for a long time. In the Western world, there are roughly 50 years of scientific attention and study, with slowly accumulating evidence of utility [2] reported moderate NIH acceptance; Vickers et al. [3] performed a meta-analysis of 29 published studies and found the evidence compelling). Nevertheless, it is rare in the Western world for a mainstream physician to refer a patient to an acupuncturist for pain, even when nothing else has worked [4].
Beyond acupuncture, the Western scientific literature on holistic treatments for pain, mobility, sleep, anxiety, and other problems has burgeoned in the past two decades. The impact of holistic and therapeutic massage techniques on metastatic bone pain was studied longitudinally by Jane et al. Field [5] reported physiological evidence of massage therapy impacts via decreases in cortisol and serotonin, coupled with dopamine increases.
Field et al. summarized a decade of studies on massage therapy for a variety of purposes including growth of infants, pain reduction, enhancing immune function, alleviating motor problems, and – significantly for the present studies – decreasing depression and aggression. Listing et al. [6] reported finding reductions in perceived stress and also physiological cortisol with massage among women after primary treatment of breast cancer. Mooventhan et al. [7] reported positive effects of both acupuncture and massage on pain, sleep, and health – all contributing to enhanced quality of life.
Massage and other holistic approaches have begun to be used among people with specific conditions. Several have involved children with cerebral palsy [8-11]. Multiple sclerosis has been targeted as well [12,13].
The extension of nontraditional practices into the field of aging, including Alzheimer’s and the other dementias, has also expanded rapidly. There are hundreds of articles in this realm already. Gleeson et al. [14] emphasized the role of touch in the caring process among elders with cognitive impairments:
The practice of nursing the elderly involves a lot of personal contact, during the delivery of fundamental physical care. While physiological and safety needs are crucial to clients in long-term settings, higher-order needs need also to be addressed. From the clients’ perspective, nurses’ use of touch provides comfort, warmth and security, although there is a dearth of empirical evidence of these benefits. This paper explores the nurse’s use of touch, the impact of touch and the experiences of touch on the older person in long-term settings. Because of the dearth of research in the use of touch with elderly clients in long-term care mental health facilities, a review of the literature was performed on the topic. This revealed that touch by nurses is frequently associated with routine tasks within nursing, and is less likely to be a caring touch intervention. Recommendations include further research on the topic and caution with widespread adoption of caring touch as an intervention.
As of the time of this writing, many hundreds of United States hospitals and senior care centers offer several forms of holistic therapies [15] – partially because they have gained credibility over the past decades, and partially because caregivers have observed that “they work.” As Gleeson & Timmons suggested, perhaps “they work” largely because they introduce simple safe and caring touch into the lives of people often ill, frightened, and lonely. The literature continues to grow.
Suggestions that massage and other alternative therapeutic interventions (including aroma therapy and acupressure, among others) might be useful among people with intellectual and developmental disabilities (under the outmoded terminology ‘mental retardation’) began to appear in the literature just before the turn of the century. One article described a positive impact on severe self-injurious behavior that responded to no other treatment over a period of years [16].
The demonstration effort conducted by Networks for Training & Development in Pennsylvania was more inclusive than anything we found in the scientific literature. It was intended to address emotional and behavioral challenges across a wide range of settings and kinds of participants.
The only study yet done that was close to the Networks initiative was done among people with intellectual and developmental disabilities in Queensland, Australia [17]. This study provided 5 weeks of twice-weekly massage sessions to 25 participants who lived in three residential group homes. The participants were people with severe disabilities ranging in age from 18 to 65. Their hypothesis was stated as:
…massage therapy may improve mood state, including anxiety and stress, reduce pain and improve sleep/wake behavior and fatigue. These benefits are of importance as they have substantial impact on quality of life.
A battery of measures was applied before and after the 5 weeks to detect changes in several aspects of life quality. The results were encouraging but not spectacular:
Mood of participants improved markedly immediately following massage session … and pre-massage mood was observed to increase over the study period. However, pre- and post-intervention measures indicated massage did not improve pain, sleepiness, depression, or stress levels or sustain positive mood three days post-intervention. Participants’ satisfaction with their current health significantly improved …, as did their satisfaction with their current happiness …, suggesting that massage therapy offered some improvement in quality of life.
The authors modestly concluded that:
The results of this pilot indicate that massage may be of benefit to people living with high care needs and represents a practical innovation providing tactile stimulation that may be integrated into care.
The Cooke study group emphasized touch as the nature of the intervention. We note that Networks’ Wholistic Practices may be conceptualized and studied in two very general ways that are distinct but overlapping:
- Touch – Tactile Stimulation, a primary need of primates, without which a variety of negative consequences are predictable [18];
- Energy – Processes that enhance health, healing, and well-being in ways that Western science cannot yet model or quantify – basically the manipulation of internal and external energy fields of which the Universe is, including us, constructed [19].
Many of the techniques offered in the Networks “menu” of Wholistic practices are energy practices in their essence, e.g., acupressure, Reiki, craniosacral therapy, and reflexology. But they also involve touch.
At least temporarily, it is possible to study the Networks Wholistic Practices interventions “menu” as something that centrally involves touch. This has the advantage of following the scientific rule called Occam’s Razor: Among competing hypotheses, the one with the fewest assumptions should be selected. Thinking primarily of touch and tactile stimulation as the “causal” intervention is sensible at the exploratory stages of research, as did Cooke et al., because it is observable and measurable – whereas at our stage of understanding about how the Universe really works, which is very primitive,[6] and therefore we cannot describe or monitor the theorized fields of life energy in ways that are valid and reliable.
If we adopt this approach just for the time being, we do not have to include models and measures of things not yet understood at all in Western science, e.g., life energy flow, acupuncture points, chi, chakras, meridians, or the atman.
There is an advantage to temporarily limiting our theoretical approach to studying Wholistic Practices in terms of touch, and that is the known central and indispensable role of touch among human beings. Anthropologists and primatologists have perceived our need for touch as arising and evolving from the social and ‘grooming’ patterns among the pre-human primates. As the leading expert on the subject [18] wrote recently,
Grooming is a widespread activity throughout the animal kingdom, but in primates (including humans) social grooming, or allo-grooming (the grooming of others), plays a particularly important role in social bonding which, in turn, has a major impact on an individual’s lifetime reproductive fitness. New evidence from comparative brain analyses suggests that primates have social relationships of a qualitatively different kind to those found in other animal species, and I suggest that, in primates, social grooming has acquired a new function of supporting these.
Dunbar showed that grooming behaviors, which take many forms, are crucial to social cohesion and individual well-being including health. In the past two decades, mainstream health science literature has busily produced compelling evidence that relationships and human connectedness are more important for physical health and longevity than blood pressure or even quitting smoking [20,21].
If touch is such a central primate need, a belief that is supported by ethologists and primatologists from Lorenz to Goodall, then providing safe and healthy means of human contact to people who have been utterly deprived of it should be a very good thing for quality of life, happiness, and very likely for health as well.
For many years, the principal author of this report has noticed that America’s community services system – the residential supports part particularly – has evolved into a “touch desert.” Hundreds of thousands of people left large public institutions over the past 50 years, and many more avoiding ever entering them, but in the “group home” structures that were created to replace them, there has been no safe place for people to experience touch with other human beings. This is, we think, primarily due to the justified fear of sexual exploitation and abuse.
However, the fact remains that we now have more than half a million Americans with intellectual and developmental disabilities living in “community homes” who never touch other humans. This is not normal, not conducive to quality of life, and not healthy. We primates are social creatures by design, and touch is particularly crucial for those among us who do not use verbal interaction as a substitute. In 40 years of study of the community services system in all 57 states and territories, this author has found that approximately half of people living in residential settings use verbal language very little or not at all.
For these reasons, we adopt a temporary and clearly incomplete model to understand what the Networks Wholistic Practices interventions are doing, and what might be the principal causal factor in producing positive outcomes: touch.
When people “in the system” experience challenges with depression or aggression, it is now generally understood to be viewed best as communication. Some people have been unable to benefit from other kinds of intervention – applied behavior analysis, medical, or chemical. It is possible that some of the underlying ‘problem’ faced by these people is a kind of isolation – a loneliness of never being touched or held.
With that as a temporary but possibly useful theoretical posture, we proceed next to describe the evaluation of the Networks Wholistic Practices demonstrations during 2016, followed by the results obtained.
The methods used in this study were both quantitative and qualitative. We collected data for ten participants via in-person interviews, both before the sessions began (or immediately after the first sessions) and later, after several sessions over a period of six months. The participants were in two counties – five in Philadelphia, and three in Northumberland. The interviews included both numeric ratings about states of mind and qualities of life, and open ended comments about reasons for participation and perceived impacts.
The quantitative aspect of the study is reflected in the interview instrument shown in Figure 1 below. The entire instrument package is available at:
http://eoutcome.org/Uploads/COAUploads/PdfUpload/NetworksWP-QOL-WholisticPracticesInventoryInstrument-V21-Final.pdf. (Figure 1)

Figure 1. Wholistic Practices Inventory: HOW DO YOU FEEL?
(To Be Answered by the Person and/or Whoever Knows the Person Best)
|
Life Quality Area |
THEN
(Before the First Session) |
NOW |
1 |
The thing(s) that led you to Wholistic Practices or Body Work |
1 2 3 4 5 |
1 2 3 4 5 |
2 |
Feeling calm |
1 2 3 4 5 |
1 2 3 4 5 |
3 |
Feeling happy |
1 2 3 4 5 |
1 2 3 4 5 |
4 |
Feeling in control |
1 2 3 4 5 |
1 2 3 4 5 |
5 |
Feeling confident |
1 2 3 4 5 |
1 2 3 4 5 |
6 |
Feeling safe |
1 2 3 4 5 |
1 2 3 4 5 |
7 |
Feelings about friends, family, neighbors |
1 2 3 4 5 |
1 2 3 4 5 |
8 |
Feelings about people you live with |
1 2 3 4 5 |
1 2 3 4 5 |
9 |
Feelings about people you work with |
1 2 3 4 5 |
1 2 3 4 5 |
10 |
Health |
1 2 3 4 5 |
1 2 3 4 5 |
11 |
Moving around |
1 2 3 4 5 |
1 2 3 4 5 |
12 |
Pain |
1 2 3 4 5 |
1 2 3 4 5 |
13 |
Sleep |
1 2 3 4 5 |
1 2 3 4 5 |
14 |
Socializing |
1 2 3 4 5 |
1 2 3 4 5 |
15 |
Life in general |
1 2 3 4 5 |
1 2 3 4 5 |
How many of these 15 questions were answered by you, even if with assistance or interpretation? ______
This instrument was derived from more than thirty years of scientific quality of life research beginning with the Pennhurst Longitudinal Study [22]. It has been used with tens of thousands of people with intellectual disability in many large and longitudinal studies and has shown good psychometrics properties including several forms of reliability and validity [23,24,25].
The method by which this scale is administered is important. It is well known that ‘Yes-No’ questions in surveys and interviews with people who have intellectual disabilities (or dementia, or of very young age) are very susceptible to the “Acquiescence Bias” problem. That is, the tendency to say ‘Yes’ to every question. This was first reported by Sigelman et al. [26] in the classic article “When In Doubt, Say Yes: Acquiescence in Interviews with Mentally Retarded [sic] Persons.” That study reported that as many as 40% of people in a series of studies would say ‘Yes’ to most questions – such as “Is the food here good?” – “Yes” – and “Is the food here bad?” – “Yes.”
The Sigelman group advanced survey methods in the disability field immensely by showing that “Either-Or” questions could be answered just as easily as “Yes-No” questions, but were not subject to the Acquiescence Bias. The Center for Outcome Analysis extended this finding to using two Either-Or questions to derive reliable answers to five point scale items. Prior to this innovation, it was difficult or impossible to obtain valid answers on scale items from many people with intellectual disabilities. The instruction lines in the scale on the page above show the procedure. Now that it has been used in 20 states and 7 countries, it is established as an optimal way to get the best possible data in studies of the present kind.
The 15 items in the scale can be averaged to produce a single number indicating overall quality of life – before and after the sessions begin.
The Qualitative aspects of this study were captured with four open-ended questions:
Reason for Participating
(Probes: Please tell us a little about what led you to pursue a wholistic approach with Networks. Why did you first come to these sessions? What were you hoping to get from these treatments? Your original purpose.)
So far, do you think you are getting any results about that Reason for Participating?
Has anything changed about your behavior?
(Probes: What has been your experience so far with this work and with us? (What effects has this work had on you? Others may also comment on what they have seen or you may report anything others have told you they’ve noticed in you.)
How to make it better or easier to keep doing it
(Probes: If so, what could help make this continue and grow for you? What would you like changed? How could we improve Wholistic Practices Services? What would make it better for you?)
Other Comments
(Probes: Any other things you think are important for us or others to know about your experience to-date? Want to add anything?)
Interviewers wrote the responses to these questions verbatim so they could be examined and compared later in search of common themes and insights.
The nature of the wholistic practices intervention
The ultimate criterion of scientific evidence is that other researchers can do the same things (experiments or treatments) and get the same results. This is called “replication” or “replicability.”
But in this study, “doing the same things” is an unusually complex issue. The “intervention” in this demonstration and outcome study was not a single mode or type of session – the intervention was in fact a menu of sessions from which each person could freely choose. Moreover, each person could change sessions and sample different ones.
As an example, several people were witnessed by the researchers who were shy, timid, or even touch-averse in the beginning. For at least two of them, beginning with reflexology applied only to the hands was acceptable, and quickly led relaxation and requests to try other modalities.
Hence the intervention offered in this demonstration, and studied in this evaluation, was actually the offering of a menu of Wholistic techniques. This must be considered a “limitation” of the current study in scientific terms, because other researchers next year in another location could never precisely duplicate “what was done” with the participants. Therefore “replication” is necessarily difficult if not impossible, and that in turn restricts our ability to show that “what was done here will work anywhere.”
For reference, the following table was filled out for each participant in the study at the Post interview. The range of choices was broad, though most included Reflexology and Massage.
What kinds of Wholistic work did you choose in each session? Please list dates for each session.
Kind of Wholistic Practice
Reflexology
Reiki
Massage
Cranio Sacral Therapy
Aromatherapy
Acupressure
Meditation Assistance
Breathing Exercises
Counseling
Coaching
Self-Help Information
Lifestyle Suggestions
Others
The entire study design was submitted to an Institutional Review Board for the Protection of Human Subjects in Research under the “Common Rule regulations of 1991 (34 CFR 97.101). The design, instruments, and informed consent procedures were examined and approved.
The potential participants were contacted first by the agencies that provided their day program supports to find out if they were interested in the Wholistic Practices and also in telling researchers about their experience. Only if they indicated willingness, and signed the consent, were they contacted and then interviewed by the research team.
Three interviewers with long experience in the field were trained by the Principal Investigator on the instrument and on field procedures. They then made their own contacts and scheduled individually convenient appointments in many cases, and in others met people at monthly Wholistic Clinics or agency focus groups about the program.
Interviews began in June 2016, and the last Post interview was completed in January 2017.
Although more than 40 people received free sessions during the demonstration, there were just 8 who continued with multiple sessions, and for whom the Before and the later Now interviews were feasible. Ages ranged from 27 to 68 with an average of 37. Gender was distributed as 6 female and 2 male. Ethnicity broke down as 1 European American, 3 African American, 1 Mixed, and 3 who did not care to report that information.
The data were entered on a Microsoft™ Excel© spreadsheet, and converted to the Statistical Package for the Social Sciences™ for analysis. Statistics included the nonparametric Wilcoxon Signed Ranks Test and the standard parametric Paired T-Test. For this small sample exploratory study, a significance level of 0.10 or below was deemed worthy of calling “significant” (meaning that a difference this large as the one obtained would happen by chance only one time out of ten or less).
This outcome evaluation has several limitations that must be stated up front and clearly.
- The self-report method is limited in that it relies on the participants’ perceptions about their well-being, rather than objective measures.
- Moreover, some participants are not able to clearly express their feelings and self-perceptions, so researchers must rely on the perceptions of people closest to them on a day to day basis.[7]
- The small number of people in this study also means that it has to be considered a pilot study. We cannot claim that what we find for these ten participants can be generalized (i.e., claimed to represent) what will happen to all similar people if they get involved in Wholistic Practices.
- With some participants, our first contact had to take place after the sessions began, and for them we had to rely on the memory of the people and those closest to them. This is an imperfect compromise of the true “pre and post” method, hence this study must be viewed with caution. (However, removing all the memory data did not change the final results in any major way, so we deemed it best to keep the memory data in the analysis, and include a warning of caution.)
- The survey instrument has not been rigorously shown to be reliable with this specific population. However, it was derived from an instrument that has been tested and shown to be reliable and valid for several similar populations [27], and therefore offers a reasonable expectation of acceptable reliability [8]
For the eight participants, their “Before and Now” perceptions of well-being are shown in the Figure 2 graph below. If the size of the bar in the graph increases from the Before (gray) to the Now (black), it means the participants perceived an improvement in their well being during the Wholistic Practices sessions. The darker bars are bigger than the lighter bars for 13 of the 15 quality of life areas – indicating enhanced quality reported in most of the quality of life dimensions. (Figure 2)
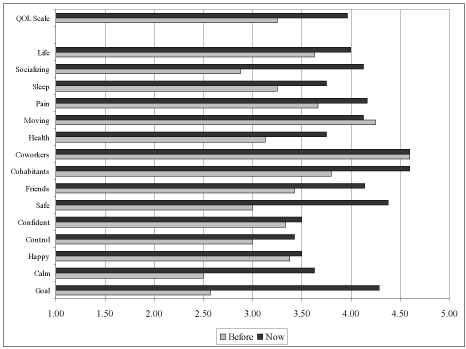
Figure 2. Qualities of Life in 15 Areas - Self-Reports “Before” and “Now”.
The most dramatic increase in the graph is the one at the bottom labeled “Goal” – which reflects answers about improvements in “The thing(s) that led you to Wholistic Practices or Body Work” – that is, the problem the participants hoped would be ameliorated by the Wholistic Practices sessions.
This could be considered the most important finding of the study. Whatever brought each participant to this demonstration, be it behavior or mood or another challenge, these problems had not been improved by other approaches – but Wholistic Practices are reported to have “worked” dramatically.
At the top of the graph labeled “QOL Scale” for “Quality of Life Scale.” This is the combined scores from all 15 quality of live dimensions.[9] On this overall scale, the dark bar is also much bigger than the light bar, meaning the combined scores on the 15 quality of life dimensions went up sharply. This means the participants’ responses indicated that their lives had improved overall.
The graph also show that there were increases from “Before” to “Now” in 13 of the 15 areas. The unchanged dimensions were in “Moving Around” and “Feelings about people you work with.” These two unchanged items suggested that the sessions did not change peoples’ ability to get around by themselves, nor did they change their relationships with co-workers.
Even with small samples, it is useful to apply statistics to see whether any of the changes visible in the graph are “significant.” Some differences over time could be due to random chance variation in measurement – but statistics can tell us the likelihood that the changes in the graph reflect “real” changes among the participants. The average scores for Before and Now, along with the appropriate statistical test of significance, are shown in Table 1.
The table shows the same information seen in the graph – average scores went up from Before to Now in 13 of the 15 areas of life quality. The column on the right shows statistical significance - the “odds” that such a large change could have happened just by chance. (Table 1)
Table 1. Average ratings of qualities of life, before and now – with significance
QOL Area |
Before |
Now |
Statistically Significant Change? |
Level of Significance (Parametric)[1] |
Life |
3.63 |
4.00 |
Yes |
0.020 |
Socializing |
2.88 |
4.13 |
|
0.142 |
Sleep |
3.25 |
3.75 |
Yes |
0.025 |
Pain |
3.67 |
4.17 |
|
0.138 |
Moving |
4.25 |
4.13 |
|
0.102 |
Health |
3.13 |
3.75 |
|
0.366 |
Coworkers |
4.60 |
4.60 |
|
0.164 |
Cohabitants |
3.80 |
4.60 |
|
0.187 |
Friends |
3.43 |
4.14 |
|
0.127 |
Safe |
3.00 |
4.38 |
Yes |
0.041 |
Confident |
3.33 |
3.50 |
|
0.305 |
Control |
3.00 |
3.43 |
|
0.224 |
Happy |
3.38 |
3.50 |
|
0.366 |
Calm |
2.50 |
3.63 |
Yes |
0.033 |
Goal |
2.57 |
4.29 |
Yes |
0.019 |
|
|
|
|
|
QOL Scale |
3.25 |
3.96 |
Yes* |
0.000 |
[1] When sample sizes are small, meaning roughly below 30, it has long been considered appropriate to use ‘nonparametric’ statistics for several reasons related to the assumptions and mathematics of using means and standard deviations. Nonparametric statistics, like the Wilcoxon that we used, make no assumptions about ‘normal distribution’ of the data or anything else required by statistics that rely on means and standard deviations. In Table 1, we report only the parametric significance tests because the results were the same by both statistics. For the present purpose, we can rely on the common T-Test, which is probably the most widely used and familiar statistic in use today.
To interpret the numbers in Table 1, first we have shaded the statistically significant areas of change. There were 5 out of the15: Life in General, Socializing, Feeling Safe, Feeling Calm, and The Thing That Led You to Wholistic Practices (Goal). These 5 areas tend to suggest a pattern of good relationships and peaceful feelings. It is also worth noting that 5 out of 15 significant results is high. It is surprising to get so many statistically significant results – 5 out of 15 – with such a small sample. It is more difficult to reach significance in small sample than it is in large samples. In turn this suggests that the changes we have seen in this small sample are “real” and relatively large.
In addition, the Overall Scale Score changed significantly. This means that we can say with confidence that, all in all, the people believe they are indeed “better off” than before they started Wholistic Practices. This finding is a good summary of the entire study.
It is useful as well to show which of the 15 items changed the most. Figure 3 shows the 15 items graphically, sorted by how much they increased from Before to Now. (Figure 3)
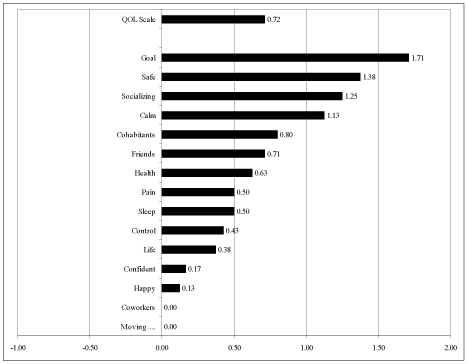
Figure 3. Increases in Quality of Life – From Largest to Smallest.
Figure 2 shows clearly that the largest change was in “Goal” – meaning “The thing(s) that led you to Wholistic Practices or Body Work.” That is an excellent result that strongly suggests that there was specific improvement. Whatever problem brought each person “in the door” was in fact addressed and “made better” by the Wholistic Practices sessions.
The second largest improvement was reported for “Feeling Safe.” That fits well with the discussions and conversations the researchers heard during the course of the interviews. As far as we could determine qualitatively, all participants became more social and less fearful during and after each session. For many, that calmness persisted for hours or even days.
Socializing (relationships with peers and support workers) and Feeling Calm were the next largest improvements. These are core values in the disability support system, and should be taken very seriously as outcomes. These outcomes are not usually expected from the other interventions commonly used for emotional and behavioral challenges – things like ABA, medical treatment, and chemical treatment.
Through months of meeting participants, direct support workers, family members, and practitioners, the researchers attempted to gain insight about the why and how of taking part in Wholistic Practices. In addition, in each interview, open-ended questions were asked, and the answers were written down on the interview form. To further supplement these qualitative methods, four focus group discussions were attended – two in Philadelphia County and two in Northumberland County.
Certain common themes have been observed by the three researchers, and these have appeared to cluster into three conceptual groups: initial reluctance versus eagerness, transition to positive acceptance, universal eager anticipation, and wanting more.
Below are the actual comments made during the interviews without filtering. Note that several of the participants do not use verbal language, and the quotes here may be from closely associated “surrogate respondents” who know the participants very well on a day to day basis. We have grouped the comments into common themes where possible.
Reason for participating
(Probes: Please tell us a little about what led you to pursue a wholistic approach with Networks. Why did you first come to these sessions? What were you hoping to get from these treatments? Your original purpose.)
Behavioral reasons
Had a lot of “behaviors”, other approaches haven’t been effective, difficulty managing emotions about food & men, can’t identify the triggers
She had “behavioral” issues that weren’t being adequately resolved-issues with trauma, boundaries
She had major “behavioral” issues for months that would end in extreme crisis situations; trauma history
Emotional reasons
Likes lotions and fragrances, stress problems, bad nerves, abuse/emotional problems, possible PTSD.
High anxiety, calming effect attended a conference on hypo/hypersensitivity. More natural, has autism/PDD.
Been unhappy - parents died. Staff approached her, she liked idea.
Enjoyment reasons
She was having hand massages and backrubs and was enjoying them.
Was told about it and said it would be fun and relaxing.
Physical reasons
Range of Motion (ROM), exercise.
Curiosity
Roommate was attending sessions, [Name] came with & liked the experience, and then continued to come.
Interpretation: the most common goal, or reason for participating, was to address behavioral and/or emotional difficulties. Other reasons included expectation of enjoyment, simple curiosity, and physical improvement.
So far, do you think you are getting any results about that Reason for Participating?
Enjoys hands but not feet. Has no desire to do Reiki.
Calmed me down when stressed.
Got upset when waiting for services at the Center. Seems calmer but no change in behavior data.
[Name] says it makes her feel “different”. She looks forward to it and feels good for the rest of the day.
Significant reduction in “acting out behaviors” - SIB, head-banging - in last few months.
Interpretation: Hard question, but those who answered were positive.
How to make it better or easier to keep doing it
(Probes: If so, what could help make this continue and grow for you? What would you like changed? How could we improve Wholistic Practices Services? What would make it better for you? Was there something about the service that you did not like?)
More
I wish I could come regularly and anytime I am interested.
Possibly increase the frequency, at least in the beginning.
Would like an increase in therapy sessions.
Deliver at home
Definitely better when therapist comes to the house.
It is much better at home! Having a variety of modalities is good for her.
Be sure staff support is available at the times of sessions
Continues to require staff assistance.
Needs assistance to coordinate appointments.
Handouts& training for all staff to understand and implement certain modalities.
Purely positive
No change and nothing I did not like.
Interpretation: Participants wanted more, and especially at their homes. But if it has to be at a Center, then staff availability was an absolute necessity to get people there and back at the precise times. One mention was made about staff learning to understand and provide some of the techniques.
The words of the participants themselves, and of the folks close to them, led to the general inference that the Wholistic Practices were enjoyed and resulted in tangible benefits. Some were reluctant at first, as we observed directly, but all who tried any of the techniques came back with more courage and requested more. All participants wanted to continue without hesitation.
The outcomes – particularly in terms of the challenges that brought some of the participants to the initiative – were universally believed to have been addressed. Some of the improvements were transitory, though, lasting only hours after each session. Others lasted until the next session, perhaps because those participants were eagerly anticipating the next one, and having something to look forward to may have been the primary factor in alleviating depressive or aggressive feelings within them.
The direct support workers and the family members closest to the participants were 100% in favor of continuing – and urged more, and more often. Finally, it was a common theme that the workers and families wanted to learn themselves how to apply some of the sessions so they would not have to wait weeks or a month for the next opportunity to see the participants enjoying themselves and feeling better.
The outcome evaluation of 2016’s Pennsylvania Wholistic Practices Initiative has revealed encouraging positive results. Although the evaluation’s research design was limited by small numbers, the lack of a “control group,” and variation in what the “intervention” was, it was quite clear that the 8 participants benefited from the sessions, reported no downsides or side effects, and strongly enjoyed the sessions. All concerned, including families and direct support workers, wanted to continue – and hoped for much more than once a month sessions.
In addition to positive results and desires to continue, we found that many or most of the workers and family members wanted to learn themselves how to apply what they saw as very soothing and helpful techniques. This could be a key to making the sessions more widely and frequently available.
The quantitative findings showed statistically significant improvements in overall quality of life, and in 5 out of 15 several specific areas. The comments and qualitative observations revealed compelling evidence of eagerness and anticipation by the end of the year – plus universal agreement that participants became more calm and/or happy before, during, and after the Wholistic sessions. For some, that positive impact faded after a few hours – for others, the sessions seemed to improve mood, behavior, and in some cases sleep for days or weeks.
This study represents a modest addition to the body of knowledge about Wholistic practices among people with the labels of intellectual and developmental disabilities. Even this small and limited evaluation provides ample grounds for expanded exploration in the intellectual disabilities service system. The study utilized the best known scientific instruments and the best possible research design in the circumstances. But the circumstances did not permit the kind of true Pre-Post With Control Group with Double Blind design that would be considered the gold standard. Our sample was small, the people were self-selected, the sessions were only once a month, surrogate perceptions and responses were needed for many participants who could not express their reactions in our formats, and in some cases we had to rely on memory rather than classical Pre-Post interviews.
The imperfections in this evaluation of a small pilot demonstration effort should not be taken to mean this study is useless – the proper interpretation is that the best science available in the circumstances yielded highly encouraging results. And naturally that this behooves the community of services and supports to proceed with larger groups, better controls and control groups, more frequent sessions, and wider geographic diversity.
To underline this conclusion, it worth quoting the humble conclusions of the most scientifically rigorous study prior to this one, by Cooke et al. (2016):
Despite encouraging preliminary results, the small sample size of this pilot and the range of complex disabilities experienced by participants meant that the impact of massage as a therapeutic treatment for particular disabilities could not be extrapolated.
Because Wholistic Practices have little or no risk of side effects, they may be a highly desirable alternative to behavioral, medical, or chemical treatment to control mood or behavior. Because they do not involve restrictive procedures or rewards based on contingencies, they are certainly less intrusive and more positive than behavior control approaches such as Applied Behavior Analysis.
One may adopt a narrow view of Wholistic Practices, and consider simple touch as the “observable” nature of the intervention. People in the service system, particularly group homes and supported living models, live in a “desert” of touch. Because of rules and restrictions that evolved to prevent inappropriate and exploitative sexual interactions, some people may live their lives almost never touching or being touched by other human beings with any kind of positive intent. According to modern understandings of the primates, including humans, this is an intolerable situation. High quality of life, mood, and even physical health are highly dependent on contact with others – from simple touch to complex relationships.
To the extent that quality of life is a goal of our support systems, interventions that safely promote calm and safe ways to experience human contact are absolutely essential. We are led to wonder how much of the depressive and aggressive challenges among people in the support system may be “caused by” their isolation, the lack of fulfilling a fundamental human need. This speculation seems simple, yet the evidence at hand suggests it is very much worth pursuing.
We believe that the Pennsylvania system should expand its exploration of Wholistic Practices, and continue to study its outcomes. The possibility of an effective way to address challenges that have resisted treatment by other means, at very low resource levels, should not be ignored or delayed.
The next step in studying the outcomes of Wholistic sessions scientifically is to work with larger numbers of participants. Eight is too few to generalize from, and may not be sufficient to publish in scientific journals.
Immediately, we need to look at another indicator of outcomes related to Wholistic participation – Incident Reports. If the participants really did become happier or more calm, then perhaps the number and severity of reported incidents decreased during their participation. That is easy to look into for these 8 participants using the HCSIS data system. We will be submitting a request for approval to do so to the Human Subjects Protection Board that oversees this study. In future studies, this should be a planned component from the beginning.
When larger evaluations are set up, it will be very helpful to include comparison groups in the design. This can be done via the “waiting list” approach. Once this option becomes known, it is virtually certain that more people will sign up for it than can be accommodated immediately. The first group can be chosen fairly, by lottery – and then their progress can be compared to the otherwise similar folks who are “waiting.”
At that stage, it will become worthwhile to track costs. In the community service system now, challenges arising from emotional and behavioral challenges are generally dealt with via costly professional, medical, and enhance staffing approaches. If Wholistic practices could even slightly reduce the need for those expensive interventions, we need to know that.
Finally, a new initiative focusing on victims of trauma has been proposed, and we believe this offers a high probability of measurable outcomes. Wholistic Practices can be highly targeted and directed toward inner feelings of fear and peacefulness. In many lives of many people in the system, nothing else has worked – and often nothing else has even been tried. If touch and/or energy work can alleviate some of that kind of suffering, we should try most diligently to find out.
[1] Terminology and spelling are discussed in Appendix A, B.
[2] For want of any better term, in this report we call each Wholistic Practices session a “session.”
[3] We will also be interested in costs in the long run, particularly if these techniques show promise as a alternative to the traditional intensive staffing approaches, which may achieve “control,” but are extremely expensive and do not appear to produce long term improvement.
[5] The first Demonstration in Philadelphia resulted in a descriptive report: Networks for Training and Development (2014). Finding Another Way through Alternative Practices: A Demonstration Project. Report submitted to the Philadelphia Office of Behavioral Health and Intellectual Disability Services.
[6] In support of this claim we need only mention the current chaos in physics – the apparent existence of Dark Energy and Dark Matter making up most of the Universe, and about which we have no theoretical consensus.
[7] This practice is called “use of surrogate respondents.” Although not ideal, it is the best method available, and was chosen and endorsed in the 1990 National Consumer Survey mandated by the U.S. Congress.
[8] populations (Fullerton, Dodder, & Douglass, & Dodder, 1999), and therefore offers a reasonable expectation of acceptable reliability
[9] A note about measurement: the 15 items that we combined into the Overall Scale Score do indeed meet the psychometric criterion for a “scale.” The common measure Cronbach’s Alpha is 0.837,which is quite high, and shows that the 15 items can justifiably be combined into a single overall indicator of life quality.
View supplementary data
- Baer HA (2003) The Work of Andrew Weil and Deepak Chopra: Two Holistic Health/New Age Gurus: A Critique of the Holistic Health/New Age Movements. Med Anthropol Q 17: 233-250. [Crossref]
- Marwick C (1997) Acceptance of some acupuncture applications. JAMA 278: 1725-1727. [Crossref]
- Vickers AJ, Cronin AM, Maschino AC, Lewith G, MacPherson H (2012) Acupuncture for Chronic Pain: Individual Patient Data Meta-analysis. Arch Intern Med 172: 1444-1453. [Crossref]
- Sierpina VS, Frenkel MA (2005) Acupuncture: A Clinical Review. South Med J 98: 330-337. [Crossref]
- Field T, Hernandez-Reif M, Diego M, Schanberg S, Kuhn C (2005) Cortisol decreases and serotonin and dopamine increase following massage therapy. Int J Neurosci 115: 1397-1413. [Crossref]
- Listing M, Krohn M, Liezmann C, Kim I, Reisshauer A, et al. (2010) The efficacy of classical massage on stress perception and cortisol following primary treatment of breast cancer. Arch Womens Ment Health 13: 165-173. [Crossref]
- Mooventhan A, Nivethitha L (2014) Effects of acupuncture and massage on pain, quality of sleep and health related quality of life in patient with systemic lupus erythematosus. J Ayurveda Integr Med 5: 186. [Crossref]
- Whisler SL, Lang DM, Armstrong M, Vickers J, Qualls C, et al. (2012). Effects of myofascial release and other advanced myofascial therapies on children with cerebral palsy: six case reports. Explore (NY) 8: 199. [Crossref]
- Gallien P, Nicolas B, Dauvergne F (2007) Pain in adults with cerebral palsy. Ann Readapt de Med Phys 50: 558.
- Hirsh AT, Kratz AL, Engel JM, Jensen MP (2011) Survey results of pain treatments in adults with cerebral palsy. Am J Phys Med Rehabil 90: 207-216. [Crossref]
- Kim T, Nam MJ (2007) Effects of abdominal meridian massage with aroma oils on relief of constipation in institutionalized children with cerebral palsy. J Korean Acad Child Health Nurs 13: 90-101.
- Kes VB, Cengić L, Cesarik M, Tomas AJ, Zavoreo I, et al. (2013) Quality of life in patients with multiple sclerosis. Acta Clin Croat 52: 107-111. [Crossref]
- Motl RW, McAuley E, Snook EM, Gliottoni RC (2009) Physical activity and quality of life in multiple sclerosis: intermediary roles of disability, fatigue, mood, pain, self-efficacy and social support. Psychol Health Med 14: 111-124. [Crossref]
- Gleeson M, Timmins F (2004) The use of touch to enhance nursing care of older person in long-term mental health care facilities. J Psychiatr Ment Health Nurs 11: 541-545. [Crossref]
- Institute of Medicine (US) (2005) Committee on the Use of Complementary and Alternative Medicine by the American Public. Complementary and Alternative Medicine in the United States. [Crossref]
- Dossetor DR, Couryer S, Nicol AR (2008) Massage for very severe self-injurious behavior in a girl with Cornelia de Lange syndrome. Developmental Medicine & Child Neurology 33.
- Cooke M, Emery H, Brimelow R, Wollin J (2016) The impact of therapeutic massage on adult residents living with complex and high level disabilities: A brief report. Disabil Health J 9: 730-734. [Crossref]
- Dunbar RIM (2010) The social role of touch in humans and primates: Behavioural function and neurobiological mechanisms. Neurosci Biobehav Rev 34: 260-268. [Crossref]
- McTaggert, Lynne (2003) The Field: The Quest for the Secret Force of the Universe. HarperCollins (288p) ISBN 978-0-06-019300-3.
- Gladwell, Malcolm (2008) Outliers: The Story of Success. New York: Little, Brown and Company
- Ornish D (1999) Love & Survival: 8 Pathways to Intimacy and Health. New York: Harper & Collins
- Conroy JW, Bradley VJ (1985) The Pennhurst Longitudinal Study: A report of 5 years of research and analysis. Pennhurst Study Report PC-85-1. Philadelphia, PA: Temple University Developmental Disabilities Center/UAP. Boston: Human Services Research Institute.
- Conroy J (1995) Reliability of the Personal Life Quality Protocol. Report Number 7 of the 5 Year Coffelt Quality Tracking Project. Submitted to the California Department of Developmental Services and California Protection & Advocacy, Inc. Ardmore, PA: Center for Outcome Analysis
- Conroy J, Devlin S, Carver P, Meyer R, Adams A (2014) Review of Quality in the Specialized Residential Support System of Genesee Health Systems: Summary Report. Report submitted to Genesee Health System by Center for Outcome Analysis: Havertown, PA.
- Dodder R, Foster L, Bolin B (1999) Measures to monitor developmental disabilities quality assurance: A study of reliability. Education and Training in Mental Retardation and Developmental Disabilities 34: 66-76
- Sigelman CK, Budd EC, Spanhel CL, Schoenrock CJ (1981) When in doubt, say yes: Acquiescence in interviews with mentally retarded persons. Ment Retard 19: 53-58. [Crossref]
- Fullerton A, Douglass M, Dodder R (1999) A reliability study of measures assessing the impact of deinstitutionalization. Res Dev Disabil 20: 387-400. [Crossref]


